Understanding the Risks and Complications of Cataract Surgery
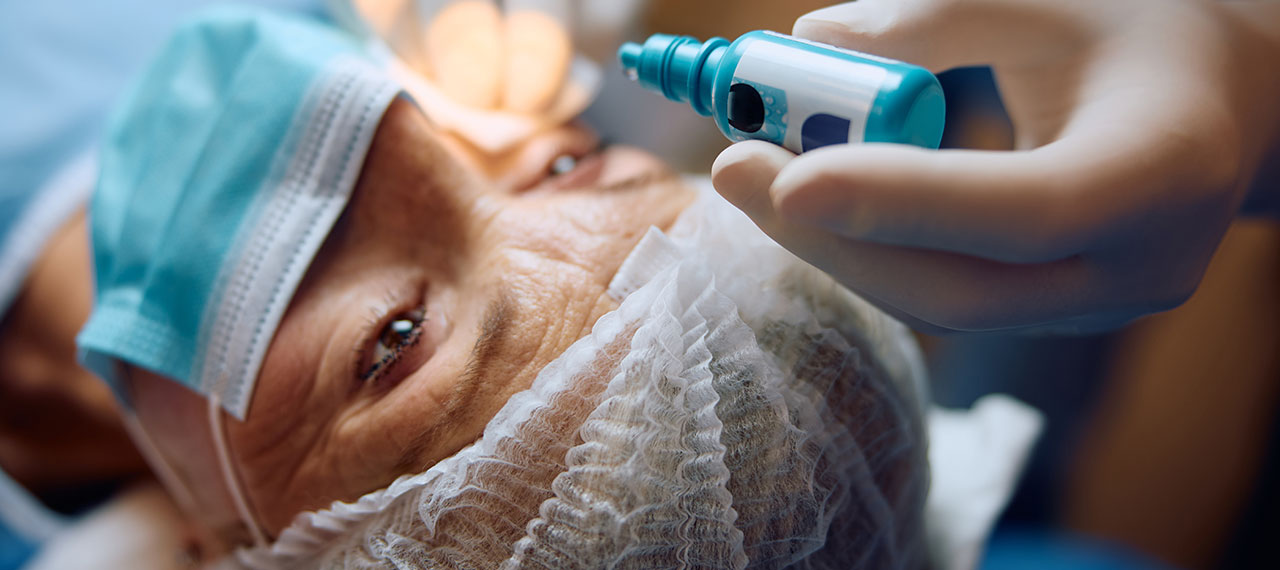
Cataract surgery is one of the most common and successful surgical procedures performed worldwide. It involves removing the cloudy lens of the eye and replacing it with an artificial intraocular lens (IOL) to restore clear vision. While it is generally considered safe and highly effective, like any surgical procedure, cataract surgery comes with potential risks and complications. Understanding these risks can help patients make informed decisions and be better prepared for their recovery.
Common Risks and Complications
- Infection (Endophthalmitis)
Endophthalmitis is a severe, albeit rare, complication that can occur following cataract surgery. It typically arises when bacteria or fungi enter the eye during or after the procedure, leading to significant inflammation and potential vision loss if not treated promptly. The risk is minimised through stringent sterilisation protocols, use of antibiotic eye drops, and careful post-operative care.Symptoms of endophthalmitis often develop within a few days after surgery and may include:\n- Intense eye pain\n- Redness and swelling of the eye\n- Blurred or decreased vision\n- Sensitivity to light (photophobia)\n- Pus or discharge from the eye
If these symptoms occur, immediate medical intervention is necessary. Treatment usually involves an intravitreal injection of antibiotics or antifungal agents directly into the eye to combat the infection. In severe cases, a vitrectomy (removal of the vitreous gel inside the eye) may be required to remove infected material and preserve vision.
While the risk of endophthalmitis is low—occurring in approximately 0.1% of cataract surgeries—patients with conditions such as diabetes, compromised immune systems, or prior eye infections may be at a slightly higher risk. Strict adherence to hygiene, avoiding water exposure to the eye in the early post-operative period, and taking prescribed antibiotic drops can significantly lower the chances of infection.
- Inflammation and Swelling
Post-operative inflammation and swelling are common and expected responses as the eye heals. Most cases are mild and resolve with the use of prescribed anti-inflammatory eye drops, but in some instances, the swelling can be more pronounced and require extended treatment.
Inflammation can affect different parts of the eye, leading to specific conditions such as:- Anterior uveitis (iritis): Inflammation of the iris and surrounding structures, leading to discomfort and light sensitivity.
- Cystoid macular oedema (CMO): Swelling in the central part of the retina (macula), causing blurred or distorted vision. This typically occurs a few weeks after surgery and may require prolonged use of steroid or nonsteroidal anti-inflammatory eye drops.
Risk Factors for Post-Operative Inflammation:
- A history of uveitis or other inflammatory eye conditions
- Diabetes or other systemic diseases affecting blood vessels
- Complicated cataract surgeries, such as those involving a posterior capsule rupture
- Excessive eye rubbing or non-compliance with post-operative medication
In most cases, inflammation and swelling subside within a few weeks, but persistent or severe cases may require additional treatments such as oral steroids or intravitreal injections. Regular follow-ups with an ophthalmologist ensure that any prolonged inflammation is addressed promptly to prevent long-term visual impairment.
- Wash your hands properly.
- Soak clean gauze or cotton wool in the cooled, boiled water.
- Wipe gently from the inner corner near your nose towards the outer corner.
- Avoid wiping inside the eye or rinsing it with water.
- Do not apply pressure to the eye.
Avoid Certain Medications
Your surgeon may advise against using blood-thinning medications such as aspirin unless medically necessary. - Posterior Capsule Opacification (PCO)
Posterior Capsule Opacification (PCO), often referred to as a “secondary cataract,” is a common post-operative complication that can occur weeks, months, or even years after cataract surgery. Although cataract surgery involves replacing the natural cloudy lens with an artificial intraocular lens (IOL), the thin membrane (posterior capsule) that holds the lens implant in place remains in the eye. Over time, this capsule may become cloudy due to the growth and proliferation of residual lens epithelial cells, leading to vision problems that resemble the original cataract.Symptoms of PCO
PCO symptoms can vary from mild to severe and typically include:- Blurred or hazy vision – Similar to looking through a fogged-up window
- Glare and halos around lights – More noticeable at night, making driving difficult
- Increased light sensitivity – The eye may struggle to adjust to bright or dim conditions
- Reduced contrast sensitivity – Difficulty distinguishing objects against backgrounds of similar colour
- Gradual decline in vision clarity – The visual impairment worsens over time, mimicking cataract symptoms
Causes and Risk Factors
PCO occurs when residual lens epithelial cells left behind during cataract surgery begin to multiply on the posterior capsule, forming a thin, cloudy membrane that obstructs light passing through to the retina. Several factors can increase the likelihood of developing PCO, including:- Younger age at the time of surgery – Younger patients are more likely to experience cell proliferation leading to PCO.
- Certain intraocular lens (IOL) types – Some materials and designs of IOLs are more prone to PCO than others.
- Pre-existing eye conditions – Patients with uveitis, diabetes, or high myopia may be at greater risk.
- Surgical technique – The way the surgeon removes the cataract and places the IOL can influence the likelihood of PCO.
Treatment: YAG Laser Capsulotomy
Fortunately, PCO is highly treatable with a YAG laser capsulotomy, a non-invasive and painless laser procedure that restores clear vision within minutes. The procedure involves:- Application of dilating eye drops – This enlarges the pupil for better access to the posterior capsule.
- Use of the YAG laser – A specialised laser creates a small opening in the cloudy posterior capsule, allowing light to pass freely to the retina.
- Immediate vision improvement – Most patients notice clearer vision almost instantly or within a few hours.
Recovery and Risks of YAG Laser Capsulotomy
The recovery from a YAG laser capsulotomy is usually quick, with minimal discomfort. However, as with any procedure, there are some potential risks, including:- Temporary eye floaters – Small dark spots may appear in vision but typically resolve within a few weeks.
- Increased intraocular pressure (IOP) – A temporary rise in eye pressure may occur, requiring monitoring.
- Retinal detachment (rare) – In very rare cases, the laser procedure can increase the risk of retinal detachment, particularly in highly myopic patients.
Prevention of PCO
While PCO cannot always be prevented, certain measures can reduce its likelihood:- Use of advanced IOL designs – Modern IOLs with sharp-edged designs help prevent cell migration onto the posterior capsule.
- Meticulous surgical techniques – Surgeons take steps to minimise leftover lens epithelial cells that could lead to PCO.
- Regular eye check-ups – Routine follow-ups with an ophthalmologist can detect early signs of PCO before it significantly impacts vision.
PCO is a relatively common but treatable condition following cataract surgery. While its symptoms can mimic those of the original cataract, a simple, quick, and effective YAG laser capsulotomy can restore vision almost instantly. Understanding the causes, symptoms, and treatment options for PCO allows patients to seek timely medical attention and maintain optimal eye health after cataract surgery.
- Retinal Detachment
Retinal detachment is a rare but serious complication that can occur after cataract surgery. It happens when the retina—a thin layer of light-sensitive tissue at the back of the eye—separates from its normal position. The retina plays a crucial role in vision by converting light into neural signals that are transmitted to the brain. When detachment occurs, it disrupts this process, potentially leading to permanent vision loss if not treated promptly.Types of Retinal Detachmentand Swelling
There are three main types of retinal detachment, each with different causes:1. Rhegmatogenous Retinal Detachment (RRD) – This is the most common form and occurs when a tear or hole in the retina allows fluid to pass through and accumulate underneath, causing the retina to pull away from the underlying tissue. It is often associated with aging and the natural shrinking of the vitreous gel inside the eye.
2. Tractional Retinal Detachment (TRD) – This occurs when scar tissue on the retina’s surface pulls it away from the back of the eye. It is more common in people with diabetes-related eye diseases (such as diabetic retinopathy) or those who have experienced previous eye injuries or inflammation.
3. Exudative Retinal Detachment (ERD) – This type results from fluid leaking underneath the retina without a tear or break. It can be caused by conditions such as inflammatory eye diseases, tumours, or vascular disorders.
Symptoms of Retinal Detachment
Early detection is crucial, as symptoms often develop suddenly. Key warning signs include:- Sudden appearance of floaters – Tiny dark specks or cobweb-like shapes that move across your vision.
- Flashes of light (photopsia) – Brief, flickering lights, especially in the peripheral vision.
- Blurred or reduced vision – A gradual or sudden decrease in visual clarity.
- A shadow or curtain effect – A dark area or veil that moves across part of the visual field, indicating progressive detachment.
- Distorted vision – Objects may appear warped or wavy.
If any of these symptoms occur, immediate medical attention is required. Delaying treatment increases the risk of permanent vision loss.
Causes and Risk Factors
While retinal detachment can occur spontaneously, certain factors can increase the risk, particularly after cataract surgery. These include:- High myopia (nearsightedness) – People with severe nearsightedness have elongated eyeballs, making the retina thinner and more prone to tears.
- Previous eye surgeries – A history of cataract surgery or other eye operations can increase susceptibility.
- Vitreous detachment – As part of the natural aging process, the vitreous gel inside the eye shrinks and pulls away from the retina, potentially causing tears.
- Family history – A genetic predisposition can elevate the risk of retinal issues.
- Eye trauma or injury – Blunt force trauma to the eye can lead to retinal detachment.
- Diabetes and eye diseases – Conditions like diabetic retinopathy can cause abnormal blood vessel growth, increasing the likelihood of tractional retinal detachment.
Diagnosis and Medical Evaluation
If retinal detachment is suspected, an ophthalmologist will perform several diagnostic tests, including:- Dilated eye exam – Using special eye drops to widen the pupils and examine the retina for tears, holes, or detachment.
- Optical coherence tomography (OCT) – A high-resolution imaging technique that provides cross-sectional views of the retina.
- Ultrasound imaging – Used when the retina is obscured by bleeding or dense cataracts, allowing doctors to assess the extent of detachment.
Treatment Options for Retinal Detachment
Retinal detachment requires urgent intervention to reattach the retina and prevent further vision loss. The treatment approach depends on the severity and type of detachment:- Laser Therapy (Photocoagulation) or Cryotherapy – If detected early, small retinal tears can be sealed using a laser or freezing treatment to prevent fluid from accumulating underneath.
- Pneumatic Retinopexy – A minimally invasive procedure where a gas bubble is injected into the eye to push the retina back into place. The patient must keep their head positioned a certain way to help the bubble press against the detachment.
- Scleral Buckle Surgery – A flexible band is placed around the eye to gently press the retina back into position, often used for larger detachments.
- Vitrectomy – In more complex cases, the vitreous gel inside the eye is removed and replaced with a gas or silicone oil to hold the retina in place while it heals.
Recovery and Prognosis
The success rate for retinal detachment surgery is high, but visual recovery depends on how quickly treatment is administered. In many cases, vision improves significantly, though some degree of permanent vision loss may occur if the detachment affected the central retina (macula).Post-surgery, patients must follow strict guidelines to aid healing, such as:
- Avoiding strenuous activities and sudden head movements.
- Maintaining specific head positions if a gas bubble was used.
- Using prescribed eye drops to reduce inflammation and prevent infection.
- Attending follow-up appointments to monitor healing.
Preventing Retinal Detachment After Cataract Surgery
Although not entirely preventable, steps can be taken to reduce the risk:- Regular eye exams – Routine check-ups help detect early signs of retinal weakness or tears.
- Avoiding excessive eye strain – Activities that involve heavy lifting or rapid eye movement should be done cautiously.
- Protecting the eyes from trauma – Wearing protective eyewear during sports or high-risk activities can prevent injury-related detachment.
- Managing underlying health conditions – Keeping diabetes and hypertension under control reduces the risk of retinal complications.
While retinal detachment after cataract surgery is uncommon, it remains one of the most serious complications due to its potential for permanent vision loss. Recognising early warning signs and seeking immediate medical attention can make a crucial difference in preserving vision. Advances in surgical techniques have significantly improved treatment outcomes, but prevention and early intervention remain the best strategies for protecting long-term eye health
- Intraocular Lens Dislocation
In rare cases, the artificial lens may become displaced, leading to blurred or doubleIntraocular lens (IOL) dislocation is a rare but potentially serious complication that can occur after cataract surgery. During the procedure, the cloudy natural lens of the eye is removed and replaced with an artificial intraocular lens. This new lens is typically secured within the eye’s capsular bag, the thin membrane that previously held the natural lens. However, in some cases, the IOL may shift from its original position, causing vision disturbances and discomfort.
While minor shifts in lens position may not always require treatment, significant dislocation can lead to visual impairment and may necessitate corrective surgery.
Symptoms of IOL Dislocation
The severity of symptoms depends on the extent of the lens shift. Common signs include:- Blurred or distorted vision – The lens is no longer properly aligned, disrupting normal focus.
- Double vision (diplopia) – If the lens moves significantly, it may cause a misalignment of images between the two eyes.
- Glare and halos around lights – The lens displacement can create irregular light refractions.
- A feeling that something is ‘off’ with vision – Patients often report that their eyesight feels unstable or changes when they move their head.
- Visible decentration of the lens – In extreme cases, an ophthalmologist may observe the lens displaced within the eye during an examination.
If any of these symptoms occur, especially after cataract surgery, it is essential to seek immediate medical attention to prevent further complications.
Causes and Risk Factors for IOL Dislocation
Several factors can contribute to the displacement of an intraocular lens:1. Weakness of the Capsular Bag
The capsular bag that holds the IOL in place can weaken over time, leading to gradual displacement. This is more common in:- Older patients, as natural eye structures degrade with age.
- Individuals with pre-existing eye diseases, such as pseudoexfoliation syndrome (PXF), which weakens the supporting fibres of the eye (zonules).
2. Trauma or Injury
A direct blow to the eye or head, such as in a fall or accident, can cause the IOL to shift from its original position. Even seemingly minor trauma can lead to dislocation, especially if the eye’s internal structures were already fragile.3. Post-Surgical Weakness or Complications
- If the zonules (the tiny fibres that hold the lens in place) were weak or damaged during surgery, the IOL may not be as stable.
- Complications during cataract removal, such as a posterior capsular rupture, can increase the risk of dislocation.
- An improperly positioned lens at the time of surgery may gradually shift post-operatively.
4. Pre-Existing Eye Conditions
Patients with certain conditions are at higher risk for IOL dislocation, including:- High myopia (severe nearsightedness): The longer eyeball structure can make the lens more prone to movement.
- Marfan syndrome, Ehlers-Danlos syndrome, or other connective tissue disorders: These conditions weaken the eye’s structural integrity.
- Glaucoma or previous glaucoma surgery: Certain procedures, such as a trabeculectomy, can disrupt the normal positioning of the IOL.
Treatment Options for IOL Dislocation
The treatment for IOL dislocation depends on the severity of the shift and its impact on vision.1. Observation and Monitoring
- If the dislocation is minimal and does not significantly affect vision, an ophthalmologist may choose to monitor the condition without immediate intervention.
- Some patients can adapt to slight lens movement without noticeable issues.
2. Glasses or Contact Lenses
In mild cases where the lens remains largely in place but causes minor visual disturbances, glasses or specialty contact lenses may improve vision without requiring surgery.3. Laser Capsulotomy (for Specific Cases)
In cases where posterior capsule contraction is a contributing factor, a YAG laser capsulotomy may be performed to improve visual alignment. However, this is only effective in select cases and is not a primary treatment for full dislocations.4. Surgical Correction
If the lens has significantly moved and is affecting vision, surgery is often required. There are different surgical approaches depending on the severity of the dislocation:- Lens Repositioning (Lens Refixation): If the IOL is still inside the eye but misaligned, an ophthalmologist can surgically reposition and secure it using sutures or other fixation techniques.
- Lens Exchange: If the IOL is severely dislocated or damaged, it may be removed and replaced with a new intraocular lens.
- Anterior Chamber IOL (ACIOL) Placement: If the capsular bag is too damaged to hold a new IOL, an alternative is to implant an anterior chamber lens in front of the iris instead.
- Scleral-Fixated IOL (SFIOL): A technique in which a new IOL is sutured or fixed to the sclera (the white of the eye), bypassing the need for capsular support.
Recovery and Prognosis
Most patients who undergo surgical correction for IOL dislocation experience significant improvement in vision. However, recovery depends on several factors:- The extent of the original displacement – More severe dislocations may require more complex procedures.
- Underlying eye health – Conditions such as glaucoma or diabetic retinopathy can affect healing.
- Surgical approach used – Some methods, such as scleral-fixated IOLs, require a longer recovery period.
Post-surgical care typically includes:
Use of prescribed anti-inflammatory and antibiotic eye drops to reduce swelling and prevent infection.Avoiding strenuous activities and sudden head movements for several weeks to allow the lens to stabilise.
Regular follow-up visits with the ophthalmologist to ensure the IOL remains securely in place.
Preventing IOL Dislocation
While IOL dislocation cannot always be prevented, certain steps can reduce the risk:- Choosing an experienced surgeon – A skilled ophthalmologist can ensure proper lens placement during cataract surgery.
- Avoiding trauma to the eye – Wearing protective eyewear during sports or high-risk activities can prevent accidental dislocation.
- Managing underlying conditions – Treating conditions like glaucoma or pseudoexfoliation syndrome can help maintain lens stability.
- Regular eye check-ups – Routine examinations allow early detection of any lens instability before it leads to significant vision problems.
Although intraocular lens dislocation is a rare complication of cataract surgery, it can significantly impact vision and quality of life. Recognising the early signs, seeking timely medical evaluation, and understanding available treatment options are crucial for maintaining long-term eye health. With advancements in surgical techniques, most cases can be successfully managed, restoring clear vision and preventing further complications.

- Increased Intraocular Pressure (Glaucoma)
Intraocular pressure (IOP) refers to the fluid pressure inside the eye, which is crucial for maintaining the eye’s shape and function. After cataract surgery, some patients experience a temporary or prolonged rise in IOP, which can lead to discomfort and, in rare cases, permanent damage to the optic nerve. If the pressure remains elevated for an extended period, it can lead to glaucoma, a progressive eye disease that can cause irreversible vision loss if left untreated.Most post-operative IOP elevations are transient, resolving within a few days or weeks with medication, but for some individuals, pressure spikes can become chronic and require long-term management.
Causes of Increased IOP After Cataract Surgery
Several factors can contribute to increased eye pressure following cataract surgery:1. Retained Viscoelastic Material
During cataract surgery, a viscoelastic gel is used to protect the delicate structures of the eye and maintain space during lens implantation. If this gel is not fully removed at the end of the procedure, it can temporarily block the eye’s drainage channels (trabecular meshwork), leading to a rise in intraocular pressure. This is one of the most common causes of short-term IOP elevation.2. Inflammatory Response
Surgical procedures trigger a natural inflammatory response as the body heals. Inflammation can cause swelling within the eye, leading to a temporary obstruction of the drainage system and subsequent fluid buildup. This often resolves with the use of steroid or non-steroidal anti-inflammatory eye drops prescribed after surgery.3. Pre-Existing Glaucoma
Patients with a history of glaucoma or ocular hypertension are at a higher risk of post-operative IOP spikes. Since their optic nerves may already be compromised, even a temporary rise in pressure can accelerate nerve damage, making careful monitoring essential.4. Corticosteroid Response
Steroid eye drops, often prescribed after cataract surgery to control inflammation, can increase IOP in steroid-sensitive individuals. This condition, known as steroid-induced ocular hypertension, can develop if the patient uses steroid medications for an extended period. If a patient exhibits an excessive IOP response, their doctor may switch them to non-steroidal anti-inflammatory drops.5. Pupillary Block
In some cases, the intraocular lens (IOL) placement or post-surgical swelling can lead to a pupillary block, where the normal flow of aqueous humor (fluid in the eye) is disrupted. This results in fluid accumulation and increased pressure. Specialised laser treatments or medications may be required to resolve this issue.6. Secondary Angle-Closure Glaucoma
If post-operative inflammation causes adhesions (synechiae) to form between the iris and the drainage angle, it can lead to angle-closure glaucoma, where fluid cannot exit the eye properly. This condition may require laser or surgical intervention to reopen the drainage pathways.Symptoms of Elevated IOP
Mild cases of increased intraocular pressure may not produce noticeable symptoms, which is why regular post-operative check-ups are essential. However, if pressure rises significantly, symptoms may include:- Eye pain or headache – Often described as a deep, aching discomfort in or around the eye.
- Blurred vision – Increased pressure can cause swelling of the cornea, leading to temporary visual disturbances.
- Seeing halos around lights – A common symptom of pressure-related corneal swelling.
- Redness in the eye – Indicates inflammation and possible drainage issues.
- Nausea or vomiting – Severe IOP spikes can lead to systemic symptoms, often seen in acute angle-closure glaucoma.
If these symptoms occur after cataract surgery, immediate medical attention is required to prevent damage to the optic nerve.
Diagnosing and Monitoring IOP
Ophthalmologists routinely measure intraocular pressure during post-operative visits using:- Tonometry – A standard test that determines eye pressure.
- Ophthalmoscopy – Examination of the optic nerve for signs of damage.
- Gonioscopy – A technique used to assess the drainage angle of the eye.
- Optical Coherence Tomography (OCT) – Provides detailed imaging of the optic nerve and retina.
Treatment Options for Increased IOP
The treatment approach depends on the severity and cause of the pressure elevation:1. Medications (First-Line Treatment)
- Topical eye drops: Beta-blockers, prostaglandin analogs, carbonic anhydrase inhibitors, or alpha agonists can lower eye pressure by reducing fluid production or improving drainage.
- Oral medications: In severe cases, acetazolamide (a carbonic anhydrase inhibitor) may be prescribed to rapidly lower IOP.
2. Laser Therapy
- Laser Peripheral Iridotomy (LPI) – Used to relieve pupillary block by creating a small opening in the iris to improve fluid flow.
- Selective Laser Trabeculoplasty (SLT) – Helps enhance drainage in patients with open-angle glaucoma.
3. Surgical Interventions
- Trabeculectomy – A surgical procedure that creates a new drainage pathway for excess fluid.
- Minimally Invasive Glaucoma Surgery (MIGS) – Less invasive techniques designed to improve fluid drainage with fewer complications.
- Glaucoma Drainage Implants – Small devices inserted into the eye to help maintain normal pressure levels.
Long-Term Management and Prevention
While temporary IOP spikes are common and often resolve without long-term damage, chronic elevation requires ongoing care. Patients at risk should:- Attend all post-operative follow-ups – Regular monitoring allows early detection and intervention.
- Adhere to prescribed eye drop regimens – Proper use of anti-inflammatory and pressure-lowering drops can prevent complications.
- Monitor symptoms at home – If vision disturbances or headaches occur, seek medical evaluation promptly.
- Limit prolonged steroid use – If steroids are necessary, doctors may prescribe the lowest effective dose or consider alternative treatments.
- Maintain a healthy lifestyle – Managing blood pressure, avoiding excessive caffeine, and staying hydrated can help regulate eye pressure.
Increased intraocular pressure after cataract surgery is a potential but manageable complication. While most cases are temporary, persistent pressure elevation can lead to glaucoma and optic nerve damage if untreated. Regular eye pressure monitoring, adherence to prescribed treatments, and early intervention are key to preserving long-term vision and ensuring a smooth recovery after cataract surgery.
- Corneal Oedema (Swelling)
The cornea may swell post-surgery, leading to temporary blurry vision. Most cases resolve with medication, but in severe cases, prolonged oedema may require additional treatment. - Droopy Eyelid (Ptosis)
Some patients develop ptosis, or drooping of the upper eyelid, after cataract surgery. This may be temporary but, in some cases, could require surgical correction. - Light Sensitivity and Glares
Many patients experience increased sensitivity to light, halos, or glares around lights, particularly at night. These symptoms usually improve over time but may persist in some individuals, especially if they have multifocal IOLs.
Factors Increasing the Risk of Complications
Certain factors can increase the likelihood of experiencing complications during or after cataract surgery:
- Pre-existing eye conditions (e.g., glaucoma, diabetic retinopathy, or uveitis)
- Previous eye surgeries
- Uncontrolled diabetes
- Severe myopia (nearsightedness)
- Use of blood thinners or anticoagulant medications
- Weak or damaged zonules (supporting fibres of the lens)
- Advanced age
Minimising Risks and Ensuring a Smooth Recovery
While complications cannot be entirely eliminated, they can be minimised by following these steps:
- Choosing an experienced surgeon: A skilled ophthalmologist significantly reduces the risk of surgical errors and complications.
- Following post-operative instructions: Proper use of prescribed medications, avoiding strenuous activities, and maintaining good hygiene reduce infection and promote healing.
- Attending follow-up appointments: Regular check-ups help detect and address any complications early.
- Managing underlying health conditions: Controlling diabetes, high blood pressure, and other medical conditions can improve healing and reduce risks.
- Protecting the eyes: Wearing sunglasses to reduce glare and avoiding eye rubbing can prevent unnecessary irritation or trauma.
Conclusion
Cataract surgery is a highly effective procedure that restores vision for millions of people each year. While it is generally safe, understanding the potential risks and complications allows patients to make informed decisions and take preventive measures. By selecting an experienced surgeon and following post-operative care instructions, the chances of a successful outcome with minimal complications are significantly increased.
