DIFFERENT TYPES OF CATARACTS
Cataracts form when protein builds up in the lens of your eye and makes it cloudy. 1
This keeps light from passing through clearly, leading to vision loss.
Initially, this will be a partial reduction in vision but advanced cataracts will cause blindness.
There are many different types of cataracts and numerous ways to classify them.2
The first four types listed below are purely descriptive:
- nuclear sclerotic;
- cortical;
- posterior subcapsular
- anterior subcapsular
They tell us about the location of the cataractous changes inside the lens, i.e. where the areas of opacity are to be found but do not tell us about the cause.3
Most of the other different types of cataracts are based on what caused the cataract, e.g. radiation cataract or traumatic cataract.
By far, the most common cause of cataracts is ageing.4
In fact, it is a normal part of the ageing process and, if you live long enough, you can expect to need cataract surgery at some point.
Fortunately, modern cataract operations are safe and highly effective; it is usually performed as a walk-in, walk-out day-case procedure.
The types of cataract seen with ageing are most commonly nuclear or cortical, though you may also see posterior subcapsular, or indeed a mixture of these different forms.
NUCLEAR CATARACTS
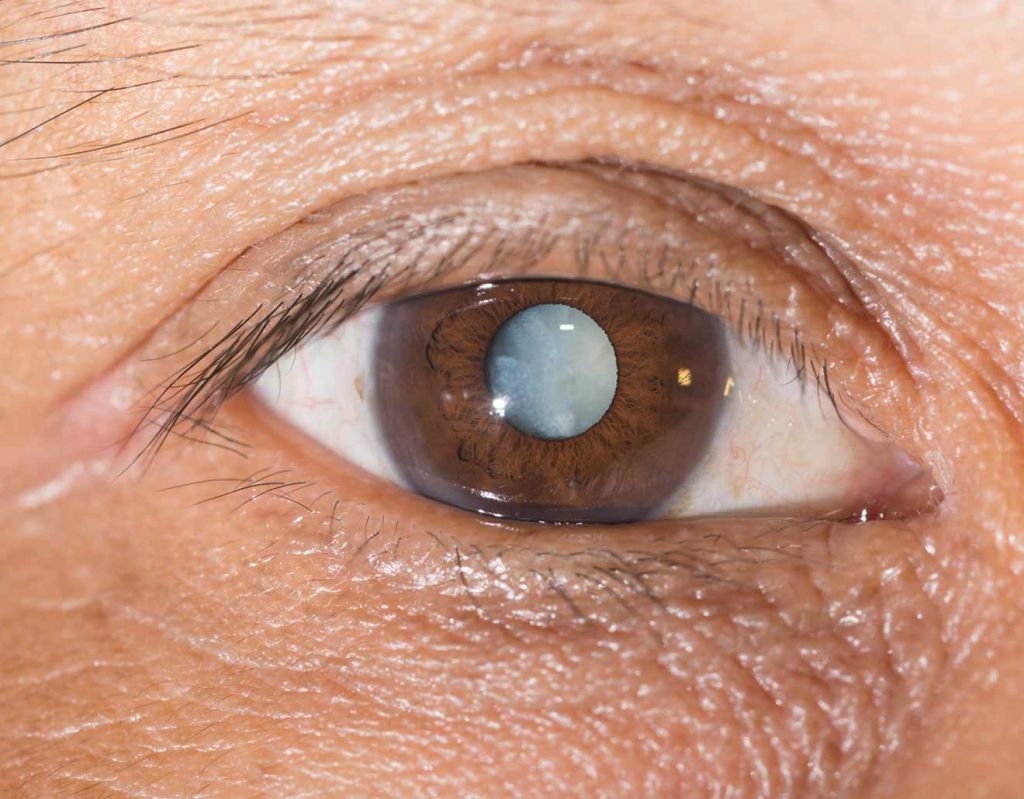
Also called a nuclear sclerotic cataract, this is the kind ophthalmologists see most often. Nuclear sclerotic cataracts are commonly associated with ageing.5
Anyone who lives long enough usually ends up with one.
They form in the central part of the eye’s lens, known as the nucleus.
As they get worse, the density and hence focusing power of the lens increases and your reading vision may actually improve.
It’s an effect known as second sight but unfortunately doesn’t last long.
Steadily over time, the lens continues to harden and becomes yellow or even brown (called lens brunescence).
You will have greater difficulty seeing small or fine details, colours get less saturated and objects may acquire a yellowish hue.
At night, you may notice halos around bright lights, such as car headlights.6
CORTICAL CATARACTS
These form within the outer shell of your lens known as the cortex.
They look like white wedges, usually triangular spokes that begin on the outer edge and progress and extend towards the centre.7
As they grow, they scatter light. If you suffer from diabetes, you are at higher risk of developing a cortical cataract.8
Cortical cataracts produce a range of symptoms and signs which include:
- Loss of vision
- Blurred vision with loss of details
- Glare from bright lights
- Difficulty with night driving
- Double vision affecting one eye (known as monocular diplopia)
The main initial symptom that patients notice is glare, a dazzling or disabling bright haze when a bright light source is present.
It becomes difficult to drive at night or in low light conditions.
Vision will become hazy, indistinct or fogged.
Colours become less clear and it can be hard to tell different shades apart.
Depth perception (estimating how far away objects are) becomes more difficult, adding to vision problems when driving.
Because cortical cataracts produce a range of symptoms that affect both distance and near vision, patients often will seek help early on and proceed without much delay to cataract surgery.
POSTERIOR SUBCAPSULAR CATARACTS
Your natural lens is surrounded and held in place by a clear bag known as the lens capsule.
Posterior subcapsular cataracts refer to opacities that appear just inside the back surface of the bag at the rearmost part of the lens.
The symptoms of posterior subcapsular cataracts can exceed what one might expect from the amount of opacification.
Most commonly patients suffer from the glare caused by bright lights, such as car headlights or the sun when low in the sky.
As the subcapsular cataract progresses it will lead to a steady loss of vision with blur or fogging. 9
Due to the severity of symptoms, particularly glare, patients often present early to have their cataracts removed.
People with diabetes or using oral steroids such as prednisolone, particularly in high doses, have an elevated chance of developing a posterior subcapsular cataract.10
ANTERIOR SUBCAPSULAR CATARACTS
Anterior subcapsular cataract (ASC) is similar to the posterior type above but instead, cataracts form at the front of the lens rather than the back. 11
ASC develops when the lens epithelial cells at the front of the lens become injured and die. This can happen with a range of causes including:
- Anterior uveitis (also known as iritis – inflammation of the iris)
- Injury to the eye
- Keratitis – Inflammation of the cornea
- Eczema (dermatitis) – inflammation linked with atopic dermatitis
- Radiation injury
- Electrical burns
- Implantable Collamer Lens or phakic intraocular lens (ICL)12
CONGENITAL CATARACT
A congenital cataract is a cataract that you’re born with or that presents in early life.
A congenital cataract is a common cause of lifelong loss of vision in children in the world today.
Congenital cataracts have a range of origins and may be genetic (dominant inheritance), arise from trauma or associated with intrauterine infection (e.g. rubella).
For many children, no cause can be identified.13
Early diagnosis is essential because early surgery to remove the cataract can result in good vision.
However, the visual result is very much dependent on when surgery is performed.
Good outcomes have been reported in children receiving an operation prior to six weeks of age where cataract affected one eye, and before ten weeks of age when both eyes present with cataracts.14
The management of congenital cataract has greatly improved over the past 40 years.
Insertion of an artificial lens implant after cataract extraction is now established practice, although there is still an ongoing debate on safety and predictability.
However, it is clear that children have benefited from advances in treatment in recent decades.
Congenital cataracts may be linked to certain conditions, such as galactosemia, myotonic dystrophy, or type two neurofibromatosis.
More than 200,000 children are legally blind from cataract and who have not had surgery, from complications of cataract surgery, or from abnormalities and eye problems linked to cataracts.15
The cumulative risk of having cataracts during the time while a child is growing is as high as one per 1000.16
TRAUMATIC CATARACTS
Many injuries can result in traumatic cataract formation.
It can occur when there is a direct penetration of the lens by a foreign object.
However, penetration is not required because blunt trauma to the eye or surrounding area can produce a “shock wave” within the eye.17
For example, you can get a traumatic cataract if you’re hit in the eye by a ball.
It could also occur from a thermal burn or chemical injury.
The cataract could develop quite quickly after the eye injury or even appear years later.18
SECONDARY CATARACTS
Secondary cataracts is the name used for cataracts caused by a medical condition or treatment, that is it arises due to something else.
Examples of secondary cataract would include diabetes, oral steroids (prednisolone) or short-sightedness which are all risk factors for developing lens opacities.
Another use of the term ‘secondary cataracts’ is when referring to a separate eye condition known as posterior capsular opacification (PCO). PCO is also known as “after-cataracts”.
This is all rather confusing.
First of all, PCO is not a true cataract, but rather a whitening of the capsular bag that was left behind after the lens was removed.
PCO is a normal occurrence after cataract surgery in about 20% of cases and treatable with a laser.
So the term secondary cataract complicates our understanding if used to refer to PCO; we should use it to mean a true cataract caused by another medical condition or treatment.
RADIATION CATARACTS
Many people now understand the importance of protecting themselves against the sun’s ultraviolet (UV) rays and the link between UV and skin cancer.
But UV can also cause damage to the eyes, too.
Ultraviolet-A (UV-A) and ultraviolet-B (UV-B) both can induce the development of cataracts.
As they are not in the visible spectrum for humans they are not necessary for sight.
UV is also a risk factor for damage to the retinas of children.19
The risk of getting cataracts increases if you spend too much time out in the sun without adequate eye protection.
People who regularly work outdoors in the sun, like farmers, gardeners, those in the fishing industry, are more likely to get radiation cataracts.
To help protect against it, you should wear sunglasses with 100% UV-A and UV-B protection.
Other sources of radiation can be linked to cataract formation, e.g. the treatment of cancer using radiation therapy.
LAMELLAR OR ZONULAR CATARACTS
This type of cataract usually presents in younger children and in both eyes.
The genes that cause them are passed from parent to child, so there is often a family history of Lamellar cataracts.
Familial lamellar cataracts are typically inherited as an autosomal dominant trait.
They usually have a good visual outcome after surgical removal.
They can be stable or over time, the whole central part of the lens may become white. In this case, eye surgery will be required.
POSTERIOR POLAR CATARACTS
Posterior polar cataracts occur on the central back part of the lens.
They are usually linked to genes that are inherited within the family.
Posterior polar cataracts typically do not cause visual symptoms..
ANTERIOR POLAR CATARACTS
Anterior polar cataracts appear as small white dots and are located on the front and centre of the lens.
Similar to posterior polar cataracts, this type usually does not affect vision.
POST-VITRECTOMY CATARACTS
A vitrectomy is a surgical procedure to remove the clear gel from the back part of the eye (known as the vitreous).
This is usually done if: you have had a retinal detachment; if there has been bleeding into the vitreous; or occasionally to facilitate access to the retina for the correction of another eye problem.
If you have undergone a vitrectomy, it is highly likely that the procedure will induce the formation of a cataract.20
The post-vitrectomy cataract can develop fairly rapidly after surgery.21
A second procedure to remove the cataract is required and will have been discussed prior to undergoing a vitrectomy.
CHRISTMAS TREE CATARACTS
Christmas tree cataracts are formed from highly refractile multicoloured crystalline ‘needles’ intersecting the fibres of the deep lens cortex.
They are also known as polychromatic cataracts.
This type of cataract is most common in people who have myotonic dystrophy, a genetic condition that impairs muscle function.22
BRUNESCENT CATARACTS
Brunescence is the term used for a nuclear cataract that has been left to progress.
A brunescent cataract turns very hard and brown.
Brunescence makes it more difficult to tell colours apart, notably purples and blues.
Surgery to extract it is more complicated and will take longer than operating on a less mature cataract.
Additionally, the risks of the procedure will be greater.23
DIABETIC SNOWFLAKE CATARACTS
This is a rare type of cataract that affects patients who have uncontrolled diabetes.
It presents rapidly forming greyish white subcapsular opacities that resemble a snowflake.
It is also known as a diabetic cataract.24
- https://pubmed.ncbi.nlm.nih.gov/26319346/
- https://pubmed.ncbi.nlm.nih.gov/7634995/
- https://pubmed.ncbi.nlm.nih.gov/9500153/
- https://pubmed.ncbi.nlm.nih.gov/15708105/
- https://pubmed.ncbi.nlm.nih.gov/20829639/
- https://pubmed.ncbi.nlm.nih.gov/27531294/
- https://pubmed.ncbi.nlm.nih.gov/19719805/
- https://pubmed.ncbi.nlm.nih.gov/20474067/
- https://pubmed.ncbi.nlm.nih.gov/26766561/
- https://pubmed.ncbi.nlm.nih.gov/31238690/
- https://pubmed.ncbi.nlm.nih.gov/3977225/
- https://pubmed.ncbi.nlm.nih.gov/21710954/
- https://pubmed.ncbi.nlm.nih.gov/22383071/
- https://pubmed.ncbi.nlm.nih.gov/22383071/
- Gilbert C. Worldwide causes of blindness in children. In: Wilson ME, Saunders RA, Trivedi RH, eds. Pediatric Ophthalmology: Current Thought and a Practical Guide. Heidelberg, Germany: Springer; 2009: 47-60
- Haargaard B, Wohlfahrt J, Fledelius HC, Rosenberg T, Melbye M. Incidence and cumulative risk of childhood cataract in a cohort of 2.6 million Danish children. Invest Ophthalmol Vis Sci. 2004;45(5):1316-1320.
- https://pubmed.ncbi.nlm.nih.gov/8268696/
- https://pubmed.ncbi.nlm.nih.gov/23931462/
- https://pubmed.ncbi.nlm.nih.gov/21617534/
- https://pubmed.ncbi.nlm.nih.gov/29373808/
- https://pubmed.ncbi.nlm.nih.gov/24357418/
- https://pubmed.ncbi.nlm.nih.gov/8258504/
- https://pubmed.ncbi.nlm.nih.gov/11709249/
- https://www.hindawi.com/journals/joph/2010/608751/