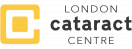Overview of cataracts and their symptoms
Cataracts are a very common eye condition and are in fact the leading cause of reduced vision in the world, accounting for roughly 40% of all cases of blindness.
Across England and Wales, there are thought to be approximately 2.5 million people who are aged 65 or above who have some level of reduced vision as a result of having cataracts.
The majority of cataracts are age-related. They first can be seen in the 40s or 50s, but may not affect the quality of your vision until after age 60.
There are multiple risk factors for developing cataract lens opacities at an earlier age than expected, including prolonged exposure to UV from the sun and inhaling tobacco smoke.
Other causes of cataracts include:
- eye injury
- chronic diabetes
- longer-term steroid medications
- radiotherapy treatments for cancer
The presence of a cataract is not restricted only to adults. Infants Can also be affected and cataracts can be present at birth (when they are known as congenital) or can result from infection during pregnancy.
Examples of infections leading to cataracts include toxoplasmosis, rubella (measles), cytomegalovirus (CMV), syphilis and herpes simplex.
Looking at various clinical studies, there is no definitive point at which we can say that the changes found in normal lens ageing end and a diagnosis of true cataract begins. 1 2 3
What is important is the symptoms created by the lens opacity and their effect on the lives of the individual.
If normal life is disrupted because of cataract symptoms, then cataract surgery is warranted. Please note that this point is not defined by a score on a letter test chart – some patients with 20/20 vision can be disabled by cataract and not able to function as they need.
Cataracts and your lens
The lens of your eye is normally clear and allows for a high level of vision by helping you to see things in focus. Your lens is towards the front of your eye and lies just behind your coloured iris.
The lens of your eye directs light (refracting light rays) onto the retina at the back of your eyeball to form a sharp image. The image is carried as information through your optic nerves and onwards to the brain.
However, the lens can become cloudy, in which case it is known as a cataract. For anyone who suffers from cataracts, their vision is akin to looking through a fogged window or frosted glass.
Cataracts are not painful and will not result in red eyes. The most common symptom is blurred, cloudy or misty vision.
When vision is cloudy because of cataracts, day-to-day activities become more difficult, including driving a car (driving is much worse at night or in low light), reading a book or seeing a phone display, or just seeing the details on someone’s face while having a conversation.
The majority of cataracts only develop gradually and so initially do not have a significant effect on your eyesight.
However, over time cataracts will inevitably reduce your ability to see.
Symptoms can take months or even years before you will notice them.
Cataracts will typically develop in both eyes, but on occasion will affect only one.
With both eyes impacted by cataracts, the loss of vision however can be quite different in each eye.
The rate of progression may be faster in one eye than the other, leading to a greater loss of vision on that side while maintaining reasonably clear vision in the other.
Cataract surgery
While the cataract is relatively early in its development, you can improve your vision by getting a different prescription or using brighter lighting.
However, as the cataract progresses, these remedies may not be sufficient and it may be time to have cataract surgery.
The only way to cure your cataract is to replace your cloudy lens with an artificial lens implant – this is cataract surgery.
Your choice to undergo cataract surgery will likely be based on how much cataracts affect your day-to-day activities.
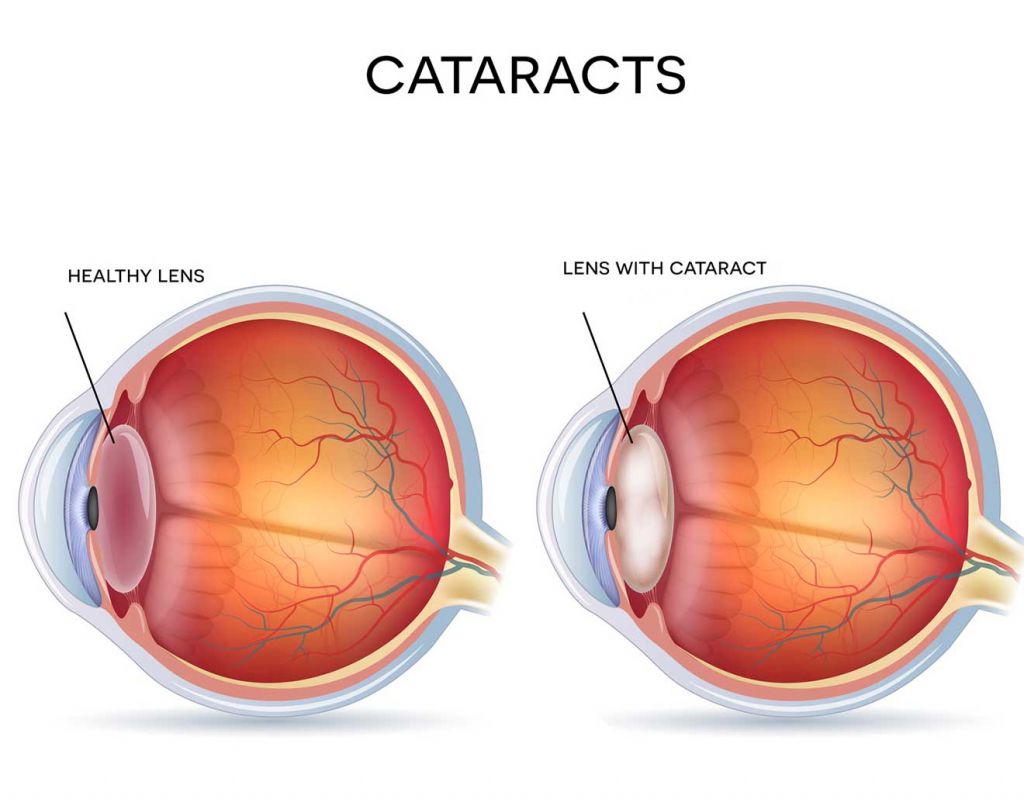
Modern phacoemulsification cataract surgery is a very well-established procedure with excellent results and a low complication rate.
Almost all cases are performed as day-case procedures using only local anaesthetic.
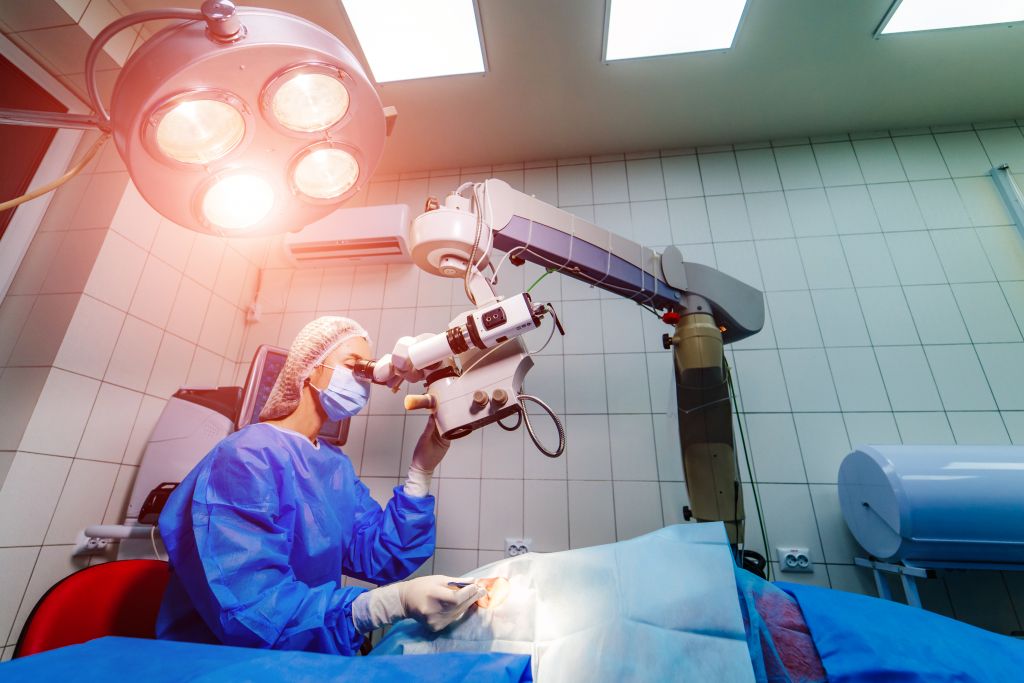
What are the symptoms of cataracts?
There are multiple reasons why someone can have cloudy vision, including a range of eye diseases.
This will include refractive errors (needing glasses or contacts) like myopia and astigmatism.
A frequent cause of blurred vision, particularly in the elderly, is cataracts. You will need an eye examination to be certain of a cataract diagnosis.
Multiple aspects of vision decline with age, unfortunately, falling away in a linear manner as time progresses. 4
Research showed that the following types of vision get worse as we get older:
- Visual acuity (seeing letters on a test chart)
- Contrast sensitivity (detecting and discriminating between various shades)
- Glare (reduced vision when faced with a bright light source)
- Visual field tests (how much we can see and be aware of across our field of vision)
- Stereoacuity (our 3D perception) remained fairly constant until we were in our mid-70s, and after which it declined at an accelerating rate.
If you have a cataract, at first you may not be aware of any symptoms. Cataracts don’t cause pain or redness of the eyes.
Your symptoms will depend on the severity of the cataract, the lighting conditions, the type of cataract and if you have a cataract present in one or both eyes.
Many cases of cataract in the early stages may not reduce eyesight significantly. Most patients are unaware of any visual symptoms.
Many cataracts are detected at a routine eye examination or while looking for new glasses. This is one reason that regular eye tests are so important.
A frequent early symptom of cataracts is that vision at night or in low light may not be as good as it once was.
However, as the cataract progresses, more of the lens becomes cloudy and opacified. More obvious symptoms appear at this stage of cataract development.
Only an ophthalmologist or optometrist can come to a formal diagnosis. However, the index of suspicion should be raised if one or more of the symptoms of cataracts below are present:5

Table 1: Symptoms of cataract – table format
| Symptoms of cataracts | |
| 1 | Blurred, misty or cloudy vision (like looking through fog) making it difficult to read, watch TV or recognise faces |
| 2 | Increasing difficulty seeing at night or in dim light |
| 3 | Problems with glare, particularly when driving at night |
| 4 | Sensitivity to glare and bright lights, including light from the sun – bright lights may be dazzling or uncomfortable to look at |
| 5 | Needing brighter lights for reading or other activities |
| 6 | The appearance of haloes (circles of light) around bright lights, e.g. car headlights or streetlights |
| 7 | Colours may look faded, washed-out or less clear – blues especially may appear desaturated and dull |
| 8 | You may notice a yellow or brown tinge to colours |
| 9 | Double vision in one eye |
| 10 | Frequently changing glasses or contact lens prescription |
If you have noticed a change in your vision, such as mistiness, your first step should be to make an appointment for an eye examination.
However, if you get symptoms that are not associated with cataracts, such as eye pain, flashes of light or sudden loss of vision, you will need an urgent assessment of your eyes.
Now let’s look at the common cataract symptoms in more detail.
Cloudy or blurred vision and cataracts
Blurred vision is the number one symptom caused by cataracts.
It is not possible to have significant cataracts without some level of clouding or blur; these are the most common symptoms mentioned by patients seeking help and who ultimately are diagnosed with cataracts.
Cloudy or blurry vision can be caused by all three main types of cataracts:
- Nuclear sclerotic cataracts
- Cortical cataracts
- Posterior subcapsular cataracts
Other cataract symptoms will usually be present as well and will vary according to the severity and location of the lens opacity.
For example, the blur will often be accompanied by glare, difficulty with night driving, or light sensitivity.6
In a healthy eye, the natural lens helps light to focus correctly onto the retina.
The youthful lens is very clear with optical properties that, when paired with the cornea, deliver a superb level of vision which is one of the best across the animal kingdom.
Any form of lens opacity (cataract) will obstruct or disturb how light rays journey through the eye and our naturally excellent quality of vision will be impaired, leading to clouding or blurring of your eyesight.
Location of the cataract
Cataracts can be small and restricted to one part of the lens, in which case they can impact just one area of vision, e.g. a single cortical cataract spoke towards the edge of the lens.
However, if that small opacified area is in the centre, e.g. a small but central posterior subcapsular cataract, the effect on vision can be severe with very significant blur.
Cataracts can also be more widespread, for example with nuclear cataracts.
Here they will cause very little blur initially but gradually more cloudy vision as the density of the cataract increases.
Vision may resemble looking through a frosted piece of glass.
Either way, blurry or cloudy vision can in many cases be the first thing you become aware of.
As your cataract continues to develop and progress, your eyesight will become more blurred over time.
Causes of blurred vision
It will be reasonably obvious that blur can be caused by many different eye conditions, not just cataracts, and an expert opinion will be needed to identify the cause of vision loss.
Blurred vision commonly can arise from dryness of the eyes, which affects a great many people, especially in the cataract age group.
Of course, it is usual to see patients who have both cataracts and dry eyes.
We also need to differentiate cataract from other eye problems, e.g. glaucoma, diabetic eye disease or macular degeneration – again, all common in the elderly where cataracts are most often found.
It is very important to be seen by an optometrist or ophthalmologist if you notice your vision becoming blurred or if there is some other change to your eyesight.
Blurred vision and needing cataract surgery
If cataracts are confirmed as the cause of the cloudy vision by your optometrist, you will likely be referred to an eye specialist who performs cataract extraction for further assessment and, most likely, scheduling for cataract surgery.
The timing for cataract surgery will depend on the degree to which you suffer from blur or cloudiness in your vision, as well as other symptoms of cataracts, such as glare, sensitivity to light, halos, etc.7
The main factor is the degree to which the cataract is affecting your day-to-day life and the activities you want to do.
If you drive in the dark each day, you would likely need surgery earlier than a non-driver, even if their vision on a letter (Snellen) test chart was worse than yours.8
Research showed that contrast sensitivity testing (a contrast sensitivity test that assesses your ability to distinguish between finer and finer degrees of light versus dark) had the best correlation with the degree of problems and visual disability as described by the patient.9
Contrast sensitivity testing can help your surgeon understand the impact on your life and expedite cataract surgery.
Cataracts, glare and sensitivity to light

Measuring visual acuity using a standard Snellen or similar letter chart is the most common, conventional test of the quality of our vision, both in normal eyes and those with cataracts.
However, some patients diagnosed with cataracts can see well using standard letter tests but report suffering from poor levels of vision sufficient to prevent normal life.10 11 12
Indeed, complaints of glare are very frequent for patients with cataracts yet they can read down to the small lines on the chart and so be said to have “good visual acuity.”13
Glare is most often caused by bright sunlight or car headlights – people may find that this glare disability is considerably more of a handicap than a small to medium reduction in letter test visual acuity.14
As cataracts develop, especially cortical cataracts and posterior subcapsular cataracts, you may become aware that glare and sensitivity to light are now too much of a handicap, whereas previously the same level of light was no problem.
Lamps or other spot sources of light, vehicle headlights, and the sun will become a source of great frustration.
You may notice that the light emitted will spread out – the single spot of light is now a diffuse sheet of glare.
But it can also lead to star-bursting (rays of light spreading out from the central bright spot), haloing (rings around lights) or doubling of images.
Often people wear sunglasses to try and mitigate the effects of glare, but cataract surgery is the only way to fix this problem effectively.
Cataracts and light scatter
But what causes this glare and light sensitivity? We need to talk about the scattering of light.
Cataracts are known to introduce what is known as light scatter. Here, some of the rays are not focused accurately or bounce off in different directions.
Some rays scatter forwards (forward light scatter) and spread out on the retina – other rays reverse course and bounce back towards the front of the eye (backward light scatter).
The effect is to reduce the sharpness and contrast of the image made on the retina.15 16
All eyes have some optical imperfections. In a young, healthy eye most of the rays of light coming from a single light source, e.g. an LED bulb, will enter through the cornea, pass through the pupil hole in the iris and then through the lens, being focused to one point on the retina.
Only around 10% of light in younger eyes is scattered.17
In this case, you would see the LED bulb as it actually is – a small, single point of light – without halos, glare, distortion or star-bursting of light.
However, after 50 years of age, light scatter within the eye begins to increase markedly.18
When we as optometrists or ophthalmologists diagnose your cataract by looking at it with a microscope, we are seeing backward light scatter – the rays of light bouncing back towards us during the examination.
We can hazard a guess as to the severity of the impact on your vision by the density of the cataract, but in reality, this doesn’t tell us accurately about forward light scatter – the spread of incorrectly focused light rays going forwards to hit your retina and be seen by you.
So we have to listen to the patients’ visual problems and not disregard them because what we examiners see at the microscope does not correlate with how well you actually see. Glare and light sensitivity are common complaints of cataract.
They will increase as the cataract progresses, blocking a clear path for light to travel through to the back of the eye, impairing your ability to see clearly.
Which cataract types cause glare and light sensitivity?
Multiple research studies have looked at which type of cataract leads to the greatest degree of glare disability.
The results have been mixed, although it is safe to say that all cataract types (nuclear, cortical and posterior subcapsular) can cause glare and light sensitivity.
On balance, though, cortical and posterior subcapsular cataracts create the greatest difficulty with glare, in the presence of an oncoming light source, including daylight.
Adamsons and team found in their research that glare test scores were significantly lower for almost all patients with cataracts than for patients with healthy, clear lenses.
They also found that glare was worse for patients with posterior subcapsular cataracts.19
Research by Stifter et al also showed that posterior subcapsular cataracts created the worst effect when testing for contrast sensitivity, i.e. distinguishing among shades mixed together.20
They also found that both posterior subcapsular and cortical cataracts, even when mild and early, could significantly reduce contrast sensitivity.
Research by Williamson highlighted that all types of cataract are associated with glare disability, although posterior subcapsular opacities created more severe glare than cortical cataracts.21
Other studies found no difference between cataract types and the severity of glare induced.22
Patients need more than just testing vision on a letter chart, as this is insufficient to assess the degree to which a patient with cataracts may be affected.
Testing using contrast sensitivity can really help to simulate the difficulties faced by a patient in the real world and reveal who may benefit most from early cataract surgery.23
Cataract types and their symptoms
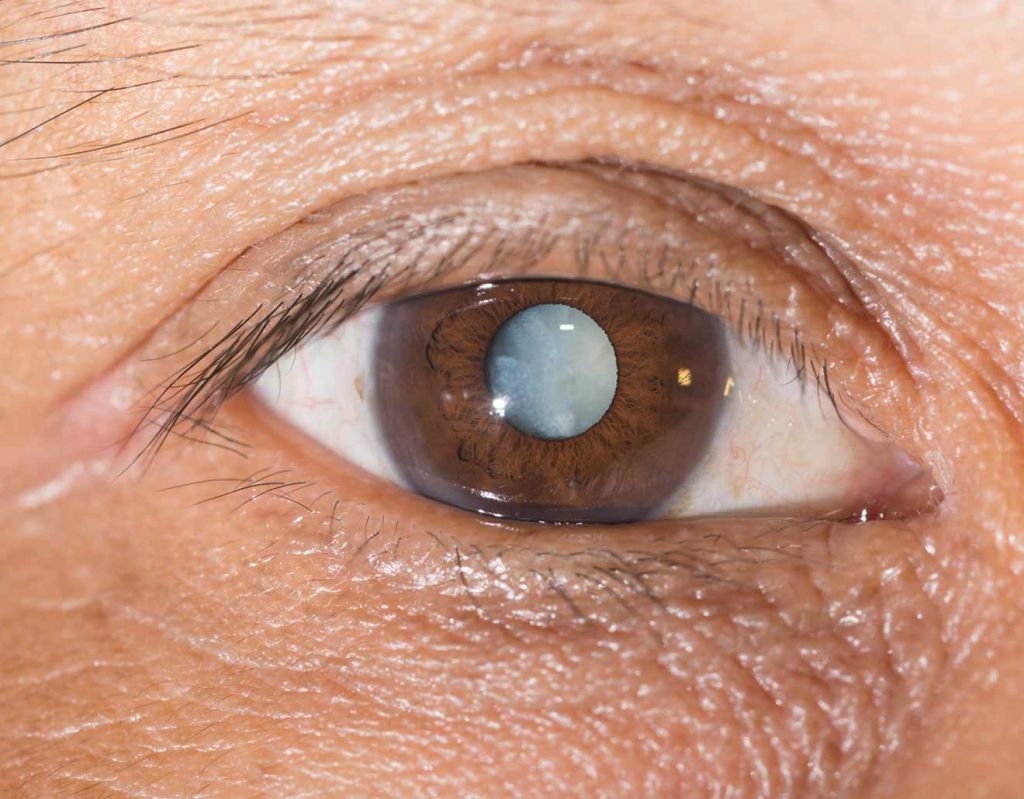
Different portions of the lens may be affected more than others and your eye doctor will classify your cataract according to the location of the opacity inside the lens.
This anatomical classification is the most frequently used by optometrist and ophthalmologists.24
It does not tell us about the cause of the cataract but does imply the kind of symptoms you can expect.
Cataracts are classified into three different types:
- Cataracts affecting the centre of the lens (nuclear cataracts)
A nuclear cataract may initially cause more shortsightedness as the centre of the lens becomes harder and denser.25 This hardening of the lens is known as “sclerosis”, and so this type may also be called nuclear sclerotic cataracts. This increased density makes the lens more powerful and creates short-sightedness, often resulting in a temporary boost in your reading vision called “second sight”. Changes in vision are usually gradual.
However, with time the lens will slowly become more yellow in colour which results in worsening cloudy vision. Many patients can delay having cataract surgery with the use of reading and/or distance glasses, or wear sunglasses with an anti-glare coating, and take simple helpful steps such as avoiding driving at night.
As the cataract steadily progresses, the lens can actually turn brown, known as brunescence. With advanced yellow or brown discolouration of the lens, it will become hard to distinguish between different shades of colours.
- Cataracts that affect the edges of the lens (cortical cataracts)
A cortical cataract starts off as small, white or cream, wedge-shaped opacities on the outer part of the lens cortex (also known as “cortical spokes”). They tend to progress slowly, extending towards the middle, and interfering with light as it passes through the body of the lens. These cataracts often resemble spokes of a wheel that point inward.
Light tends to scatter when it hits the spoke-like opacities.26 Cortical cataracts can cause glare, sensitivity to light, blurry vision, and difficulties with depth perception. Anti-glare glasses can help although cataract surgery will eventually be needed to fix this condition.
- Cataracts that affect the back of the lens (posterior subcapsular cataracts). A posterior subcapsular cataract often begins as a small, opacified area at the back of the lens, often central and right in the path of light rays on their way to your retina. A posterior subcapsular cataract can decrease your ability to see print or a phone screen, impairs your vision in bright light, and creates halos or glare around bright light sources at night.
Posterior subcapsular cataracts most commonly do not have a clear cause. However, they may be associated with an eye or systemic disease or other factors including: atopic disease (eczema, asthma, hay fever); short-sightedness; use of steroids; diabetes; iritis (inflammation of the iris and uvea); retinitis pigmentosa (RP); history of trauma; and glaucoma.27
Posterior subcapsular cataracts will tend to progress faster than other forms of cataract – you may go from clear vision to significant sight loss within months or even weeks.28
Without treatment, posterior subcapsular cataracts can reduce vision to the point of blindness.
Table 2: Types of cataracts and their symptoms
| Symptoms from different types of cataracts | ||
| Cataract type | Location of opacity in the lens | Most common symptoms |
| Nuclear (sclerotic) cataracts | The central part of the lens, akin to the core of a planet | Blurred, misty or cloudy vision (like looking through fog) making it difficult to read, watch TV or recognise facesGlare, especially at nightIncrease in short-sightedness, temporarily improving reading vision, but blurring distance visionDifficulty distinguishing shades of coloursYellow hue to the vision, and fading of colours |
| Cortical cataracts | Spoke-like wedge opacities coming in from the edge of the lens, usually towards the front | Cortical cataracts can cause glare problems, particularly when driving at nightSensitivity to lightBlurry visionDifficulties with depth perception |
| Posterior subcapsular cataracts | Diffuse whitening at the rear of the lens, which may be small and central or affect a wide area | Impairs reading visionGlare and light sensitivityDifficulty with vision in bright lightHalos or glare around light sources at nightBlurry vision |
How do different cataract types affect vision?
The most common method of measuring vision is very familiar to most patients – using a letter chart and reading down from the biggest letters at the top through lines of steadily smaller letters until one can go no further.
But this is not the only way of assessing how well we can see. Letter charts just test our central, highest-resolution vision and don’t take into account our peripheral vision.
You could have fantastic central vision, seeing better than 20/20, but if you have lost most of your peripheral vision (tunnel vision) you will be effectively blind.
Further, because the letter charts use black on white print, they are known as high contrast tests, whereas the real world is in varying shades of different colours.
Patients can have lost a great deal of functional vision if they can’t distinguish shades, even if they score well in black-on-white tests.
Standard letter tests also don’t take into account having a light shining in your eyes at the same time. Many cataract patients are disabled by glare from oncoming lights but would perform perfectly in an office setting.
So when we assess a patient’s vision to decide on the severity of their cataract, we include a range of vision test techniques: examination with a microscope, visual acuity (VA), contrast sensitivity (CS) and glare disability (GD).29
The significant differences between the morphological types of cataract should be taken into consideration when the benefit of cataract surgery is to be measured on the basis of functional improvement.
Patients with posterior subcapsular cataract (PSC) can have a more marked functional impairment, indicating that cataract surgical intervention is indicated at an earlier stage in these patients.
One study looked at patients who were waiting for cataract surgery on their first eye.
They were asked to describe their visual difficulties in everyday life with a specific questionnaire designed for this purpose.
Further, all the cataracts were graded using the Lens Opacities Classification System III (LOCS III).
Patients described their vision for day-to-day life as significantly worse with PSC compared to nuclear cataracts.
PSC patients had more impairment for both near and distance vision, even though their visual acuity using a standard letter chart was the same.30
There was a high degree of correlation between the contrast acuity measurements and functional vision as reported by patients.
This endorses the clinical relevance of recording contrast sensitivity in patients with cataract.
Particularly, the severity of posterior subcapsular cataract has a major effect on the impairment of contrast acuity.
Contrast acuity corresponded closely to the self-reported visual difficulties in everyday life.31
Short-sightedness and cataracts
Short-sightedness (the common name for myopia) and cataracts seem destined to be found together like hand and glove. Why is this so?
- Firstly, patients who are short-sighted are more likely to develop cataracts. The reasons aren’t clear but the correlation is without a doubt. Also, the greater the severity of myopia, the higher the chance of getting cataracts earlier than would be expected. For example, patients with high myopia (a prescription of -6.00 dioptres or worse) are twelve times more likely to get cataracts.32
- Secondly, those who develop nuclear cataracts (affecting the centre of the lens and very commonly found in age-related cataracts) will often become short-sighted. The greater density of the lens core increases its focusing power, pulling the image forwards inside the eye and resulting in myopia. Distance vision will become more blurry and reading vision can temporarily improve, reducing again as the cataract becomes more opaque.
What is short-sightedness?
Short-sightedness – myopia – is a very commonly occurring problem of focusing. It is what is known as a refractive error, which means that light is not focused correctly onto the retina, and the image you see is blurred.
Those with myopia have blurry distance vision, although near vision will be clear. The distance away at which things start to become blurry depends on how bad the myopia is.
If your prescription is very mild, say -1.00 dioptres, you will have clear vision out to about 1.2 to 1.5 metres away. Beyond that things get out of focus.
But if you have more severe myopia, let’s say -8.00 dioptres, things are much worse. Objects are clear only if within 12-14 cm away from your eyes; beyond that range blur becomes extreme.
With such a severe degree of short-sightedness, any object needs to be held so close to the face that the near vision “benefit” of myopia is not useful. Obviously, this is a very disabling level of refractive error.
How is short-sightedness corrected?
In places with established healthcare systems, myopia is most commonly treated with one of the following three options:
- Glasses
- Contact lenses
- Laser eye surgery
Another very effective option is now available for high and extreme myopia.
Implantable Contact Lenses (ICLs) are contact lenses that can be placed permanently inside the eye and need no maintenance.
They can provide decades of good vision with the benefit of being removable should the need ever arise.
Orthokeratology (Ortho-K) is another option for short-sighted patients.
With Ortho-K, contact lenses are worn throughout the night which has the effect of flattening the cornea and removing the need for glasses or a contact lens during the daytime.
A significant downside of orthokeratology is the increased risk of corneal infections, particularly with nasty organisms like Pseudomonas aeruginosa and Acanthamoeba, which can leave permanent corneal scarring and reduction of vision.33 34
One research paper on Ortho-K and infection showed that despite early intervention and treatment, the majority of corneal infections resulted in scars and nearly 10% of eyes required surgical treatment.
The risk of infectious keratitis should be strongly emphasised to those using this method of vision correction.35
In less-developed nations, one or more of these options may not be widely available.
It is an unfortunate fact that uncorrected refractive error is one of the world’s most common causes of treatable vision loss.
Eye problems linked with short-sightedness
Being short-sighted has more implications than just needing to wear glasses, use contact lenses or have laser eye surgery.
There are alterations in the anatomy of a myopic eye that place someone at a higher risk of a number of eye conditions.36
Many of these are serious problems that have the potential to cause blindness.37
The various eye conditions linked to being short-sighted include:38
- Cataract
- Retinal tears, holes and degenerations
- Retinal detachment
- Strabismus (more commonly called a squint where the eyes look in different directions)
- Glaucoma (a raised pressure in the eye leading to vision loss)39
- Disease of the macula (the vital high resolution central retinal area)
- Lazy eye (amblyopia)
Short-sight and the risk of getting cataracts
Those who are short-sighted carry a greater chance of developing cataracts. The increased risk varies according to the type of cataract: nuclear, cortical or posterior subcapsular cataract.
One research paper that pooled multiple studies highlighted that nuclear cataracts were found three times as often in short-sighted patients as normal eyes.
Also, these patients had twice the chance of developing posterior subcapsular cataracts. Interestingly, there was no association found with cortical cataract.40
A separate research study from Salisbury, United States, clearly demonstrated that the likelihood of developing a cataract correlated with the severity of myopia.
Even for mild myopia, the risk of getting nuclear cataracts was doubled when compared to people who did not need glasses.
For people with high myopia, the danger of developing nuclear cataracts was high at up to 4.5 times the risk.
For posterior subcapsular cataracts, the chance of being affected was even higher:41
Table 1: The risk of posterior subcapsular cataracts with short-sightedness
| Severity of Short-Sight | Elevated Risk of Cataracts |
| Mild myopia (up to -2.00D) | Risk raised 60% |
| Lower Moderate myopia (-2.00 to -5.00 dioptres) | Risk raised 220% |
| Higher moderate myopia (-5.00 to -6.00 dioptres) | Risk raised 440% |
| High myopia ( -6.00 or worse) | Risk raised 1,130% |
For high myopia where the patient had glasses of -6.00 dioptres or higher, the risk was elevated by a factor of 12 for posterior subcapsular cataracts.
As described by previous studies, no association was found between myopia and cortical cataracts.42
However, patients who wear no glasses or those who are long-sighted and hyperopes tend to develop more cortical cataract than myopes.
These cortical cataracts might be caused by shear stress inside the crystalline lens due to accommodation efforts at the time of onset of presbyopia.
Cataracts causing short-sightedness
The lens inside the eye, along with the cornea, focuses incoming light rays onto the retina at the back of the eye. It does this by a process called refraction.
Refraction is simply how light bends when passing across a junction of two substances when one is denser than the other.
For example, light passing through the air (very low density) will be diverted when it hits something denser such as glass.
Image of refraction a surface
If you shape the glass into a smooth curved surface, you can bring all the rays of light together at a single point – the focal point.
Image of lens refraction
In the eye, refraction happens in two locations – the cornea and the natural lens.
The cornea is the workhorse, delivering two-thirds of the eye’s focusing power; the lens adds the remaining one third but is able to change its shape and vary the amount of focus power applied (at least when we are younger than around 45 years old – after that, we lose this ability and will need reading glasses).
The amount of refraction (bending) of light, depends on the relative densities of the material that light is passing through.
Inside the eye, light is passing through essentially saltwater (lower density) and then through the body of the lens (higher density), and so rays are refracted and brought together.
When you develop an early nuclear cataract, the central part of the lens becomes denser but without becoming more opaque.
So light isn’t obstructed by the early cataract but IS focused to a greater degree.
Image cataract lens focusing light more.
The result is that the image is brought forwards inside the eye, now landing just in front of the retina.
This is exactly what occurs in patients who are short-sighted – the image is not focused at the right point on the retina but instead lands in front of it.
The rays of light then travelling on and arriving at the retina are not in focus, and the image you see is blurry.
Image of short-sighted focus
Hence, nuclear cataracts create short-sightedness.43
Patients will most often notice that their reading vision has improved, sometimes to the extent of no longer needing reading glasses!
This welcome change is known as “second sight”. The downside is that distance vision is somewhat blurred, as happens to all short-sighted people.44
The result of this is that people who previously needed glasses for reading may no longer have to use them anymore, or frequent increases in the power of your glasses prescription may be required.
This reading vision miracle doesn’t last, however.
The nuclear cataract continues to harden and begins to yellow and opacify.
More and more light is now being blocked from passing through the lens creating cloudy vision, desaturated colours and glare.
Nuclear cataract changes progress slowly so it may take years before cataract surgery is needed.
Summary
Cataracts and short-sightedness are intertwined. Being myopic makes you more likely to get cataracts, most often of the posterior subcapsular or nuclear types.
And getting nuclear cataracts will make you more short-sighted.
The treatment of cataract with surgical extraction in short-sighted patients is also more complicated with the added risk of complications.
You can learn more about cataract surgery in myopia in our published article.
Decreased colour perception
Due to the clouding of the eye, colours can become less vibrant and increasingly muddy over time. “Real” whites will appear much more yellow in comparison.
Because this occurs at such a slow and gradual pace, most patients won’t notice colour changes until after surgery is done to remove one or both cataracts.
“When people develop cataracts, there is a marked fading or yellowing of colours, which is sometimes noticed,” says Michael Nordlund, MD of Cincinnati Eye Institute.
“One of the most prominent improvements in vision after cataract surgery is a marked improvement in colour vision.
Patients often comment following surgery that they don’t ever remember seeing such vibrant colours. In fact, we are just restoring the colour vision of their youth.”
Difficulty driving at night
Because cataracts make it difficult to balance the contrast between the darkness and bright lights from oncoming traffic, most affected people will experience trouble driving at night.
If blaring headlights and luminous street lamps are giving you a headache, you may want to get checked out, notes Shoshana Ungerleider, MD, internal medicine physician at Sutter Health’s California Pacific Medical Center.
“Patients often complain of a problem with night driving and reading road signs.
If you notice these and/or frequent changes in your eyeglass or contact lens prescription, make an appointment to see your eye doctor for an exam.”
Trouble reading fine print
According to All About Vision, the lens inside the eye is comparable to a camera lens, focusing light onto the retina and letting us see things clearly both up close and far away.
This lens is mostly comprised of water and protein, and the protein is arranged in such a way that allows light to pass through it.
Because cataracts cause the protein to clump together, small print may become difficult to discern in the eye’s refractive mirror.
Scott MacRae, MD, ophthalmologist and chairman of the Public Health Committee with the American Academy of Ophthalmology, cites blurry or waxy reading and distance vision as one of the blaring signs of cataracts.
“Things start to look like there is a film in front of your eyes. The sharpness is gone.”
Double vision
Diplopia, more commonly known as double vision, can be another silent sign of cataracts. However, this is not to be mistaken as the diplopia that comes from improper alignment of the eyes.
Double vision, in this case, will occur even when looking through one eye.
“At first, the cataract may cause cloudiness in one’s vision that will affect only a small part of the eye’s lens and may not be so noticeable,” warns Dean Hart, OD, optometrist and professor at Columbia University’s School of Medicine.
“But as the cataract grows in size, it will cloud more of the lens and will also distort the light passing through it. As a result, you may get double vision in a single eye if only that eye has the cataract.”
If you have cataracts, you may notice that the prescription for your glasses or contact lenses changes more often than usual.
Some of these symptoms could be caused by problems other than cataracts, such as diabetes or glaucoma.
So if you notice any problems with your vision, make an appointment with your optometrist.
An optometrist is a registered healthcare professional who examines eyes, tests sight and dispenses glasses and contact lenses.
Is my cloudy vision a symptom of cataract development?
There are also other less common causes of cloudy vision, including corneal abrasions (where the cornea becomes scratched), dry eyes, opacification (were a cloudy layer of scar tissue forms beneath the lens), or scarring of the cornea (the clear part in front of the eye).
On top of this, other causes can include optic neuritis, macular degeneration, diabetic retinopathy, infections and inflammation.
If you are experiencing a sudden deterioration in vision, you should seek immediate medical attention.
Cloudy vision can take a toll on your lifestyle, often making it difficult to read, drive, or see faces clearly. A number of eye conditions can cause this, including: 2
- Myopia (short-sightedness): objects at a distance appear blurry
- Astigmatism: both near and far objects appear distorted and blurry
- Presbyopia: age-related change in the ability to focus on near objects
- Cataracts: cloudy vision due to changes in the lens of the eye affecting vision at all distances
How a cataract forms
The lens, where cataracts form, is positioned behind the coloured part of your eye (iris).
The lens focuses light that passes into your eye, producing clear, sharp images on the retina — the light-sensitive membrane in the eye that functions like the film in a camera.
As you age, the lenses in your eyes become less flexible, less transparent and thicker.
Age-related and other medical conditions cause tissues within the lens to break down and clump together, clouding small areas within the lens.
As the cataract continues to develop, the clouding becomes denser and involves a bigger part of the lens.
A cataract scatters and blocks the light as it passes through the lens, preventing a sharply defined image from reaching your retina.
As a result, your vision becomes blurred.
Cataracts generally develop in both eyes, but not evenly. The cataract in one eye may be more advanced than the other, causing a difference in vision between eyes.
How do we grade cataracts?
Ophthalmologists will grade your cataract according to its type and severity. A very common method is the Lens Opacities Classification System III (LOCS III) which uses photographic transparency images of the lens as standards to compare against.
Cataract grading schemes have provided eye specialists with a way to discuss and describe their clinical assessments.
They can also compare developments in diagnostic devices to correlate an objective measurement with a clinical one.45
Why do cataracts cause cloudy vision?
A cataract is a common eye condition in which the lens inside the eye loses its transparency.
The lens is the part of the eye that helps to focus light on the retina, the light-sensitive layer on which images are formed. In healthy eyes, the lens is transparent and allows light to pass through.
When the lens is cloudy from a cataract, the images formed are foggy.
The lens of the eye works like a camera to focus light on the retina and form images, adjusting to allow us to see objects at varying distances.
Cataracts are made up of clumps of protein that cloud the lens – it’s a bit like cooking an egg white where the transparency gradually gives way to milky cloudiness.
Usually, both eyes are affected, but vision may be better in one eye than the other.
Cataracts mainly occur in older people, often developing as part of the natural ageing process. In fact, in the UK, cataracts account for more than one-third of the cases of vision impairment in people above the age of 75.
How are cataracts diagnosed?
Cataracts are usually found during a routine eye exam — from determining the sharpness and clarity of your vision to examining your overall eye health.
Here, you’ll find out more about how these tests are conducted to detect cataracts, as well as a look at new technologies and insights into how cataract risk factors can be detected sooner and quicker
Cataracts can usually be picked up during a normal eye test, which is why it’s important to have one regularly (once every two years or more frequently if your optometrist recommends it).
During an eye exam, your optometrist will carry out a number of tests, like assessing how well you can see at varying distances, as well as having a good look at your overall eye health.
If they think you have cataracts, it’s likely that they will refer you to an eye doctor specialist (ophthalmologist) who can confirm the diagnosis and plan your treatment.
What is the treatment for cataracts?
If your cataracts are mild, stronger glasses and brighter reading lights may be helpful for some time.
However, most cataracts get worse over time (often many years) so it’s likely you will eventually need treatment.
The only treatment that is proven to be effective for cataracts is surgery.
This will usually be recommended if your loss of vision is affecting your daily activities, such as driving or reading.
It’s a very common and successful procedure and involves taking out the cloudy lens and replacing it with a clear, artificial one.
- https://pubmed.ncbi.nlm.nih.gov/12881335/
- https://pubmed.ncbi.nlm.nih.gov/17122131/
- https://pubmed.ncbi.nlm.nih.gov/10502578/
- https://pubmed.ncbi.nlm.nih.gov/9071208/
- https://www.mayoclinic.org/diseases-conditions/cataracts/symptoms-causes/syc-20353790
- Harding J. London: Chapman – Hall; 1991. Cataract: Biochemistry, Epidemiology and Pharmacology; pp. 83–124.
- https://pubmed.ncbi.nlm.nih.gov/15044934/
- https://pubmed.ncbi.nlm.nih.gov/1544787/
- https://pubmed.ncbi.nlm.nih.gov/2282946/
- https://pubmed.ncbi.nlm.nih.gov/17122131/
- https://pubmed.ncbi.nlm.nih.gov/2724116/
- https://pubmed.ncbi.nlm.nih.gov/2282946/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3306069
- https://pubmed.ncbi.nlm.nih.gov/10374152/
- https://pubmed.ncbi.nlm.nih.gov/14693761/
- https://pubmed.ncbi.nlm.nih.gov/11327677/
- https://pubmed.ncbi.nlm.nih.gov/7753528/
- https://pubmed.ncbi.nlm.nih.gov/7753528/
- https://pubmed.ncbi.nlm.nih.gov/1497520/
- https://pubmed.ncbi.nlm.nih.gov/15342050/
- https://pubmed.ncbi.nlm.nih.gov/1486072/
- https://pubmed.ncbi.nlm.nih.gov/15044934/
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3306069/
- Thompson J, Lakhani N. Cataracts. Prim Care. 2015;42(3):409-23. doi:10.1016/j.pop.2015.05.012
- https://jamanetwork.com/journals/jamaophthalmology/fullarticle/484355
- https://pubmed.ncbi.nlm.nih.gov/28917409/
- https://pubmed.ncbi.nlm.nih.gov/15474821/
- https://europepmc.org/article/PMC/1041793
- https://pubmed.ncbi.nlm.nih.gov/2282946/
- https://pubmed.ncbi.nlm.nih.gov/15342050/
- https://pubmed.ncbi.nlm.nih.gov/17122131/
- https://pubmed.ncbi.nlm.nih.gov/15953641/
- https://pubmed.ncbi.nlm.nih.gov/25158307/
- https://pubmed.ncbi.nlm.nih.gov/19123161/
- https://pubmed.ncbi.nlm.nih.gov/28534320/
- https://pubmed.ncbi.nlm.nih.gov/26649982/
- https://pubmed.ncbi.nlm.nih.gov/16101943/
- https://pubmed.ncbi.nlm.nih.gov/32347918/
- https://pubmed.ncbi.nlm.nih.gov/21684603/
- https://pubmed.ncbi.nlm.nih.gov/23938120/
- https://pubmed.ncbi.nlm.nih.gov/15953641/
- https://pubmed.ncbi.nlm.nih.gov/15953641/
- https://pubmed.ncbi.nlm.nih.gov/10549667/
- https://pubmed.ncbi.nlm.nih.gov/18222002/
- https://pubmed.ncbi.nlm.nih.gov/30489359/