If you are preparing for lens surgery, one of the first things you will notice is the number of tests performed before the procedure. Many patients are surprised by how detailed the pre-operative assessment can be. These tests are not unnecessary steps; they are an essential part of ensuring that surgery is safe and that the artificial lens implanted during the procedure provides the best possible visual outcome.
Lens surgery is not simply about removing the eye’s natural lens. The procedure also involves selecting and implanting a carefully calculated intraocular lens that must match the exact measurements of your eye. Because of this, surgeons rely on a series of specialised diagnostic tests to gather accurate information about the eye’s structure, vision, and overall health.
Every eye is unique, and even small differences in anatomy can influence which lens is most suitable. Pre-operative testing allows surgeons to evaluate corneal curvature, eye length, retinal health, and other critical factors before surgery takes place. These measurements guide lens power calculations and surgical planning.
If you are considering Lens Surgery in London, understanding these tests can help you feel more confident and prepared for the procedure. Knowing that each measurement contributes to a personalised surgical plan often reassures patients that their treatment has been carefully designed to achieve safe surgery and the best possible visual results.
The Importance of Pre-Operative Testing
Before lens surgery takes place, the surgeon needs a detailed understanding of your eye health and anatomy. Pre-operative testing provides essential information about structures such as the cornea, retina, and optic nerve, allowing the surgical team to plan the procedure safely and effectively. These evaluations ensure that the surgery is tailored to the specific characteristics of your eyes.
One of the key purposes of these tests is to identify any underlying conditions that may influence surgery, such as glaucoma, retinal disease, or corneal irregularities. Detecting these issues early allows the surgeon to adjust the surgical plan if necessary and reduce the risk of complications during or after the procedure.
Pre-operative testing also helps determine the most suitable intraocular lens to replace the natural lens. Precise measurements of the eye ensure the correct lens power is selected, which is essential for achieving clear vision after surgery. Modern diagnostic tools provide highly accurate data, allowing surgeons to create a personalised treatment plan for the best possible visual outcome.
Comprehensive Eye Examination
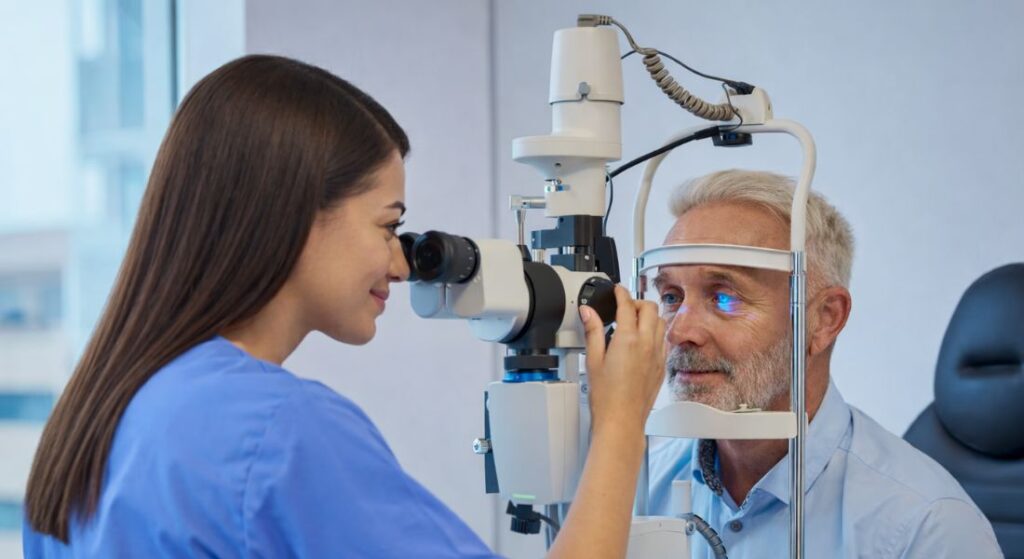
The evaluation process for lens surgery typically begins with a comprehensive eye examination. This detailed assessment allows the ophthalmologist to evaluate the overall health of your eyes and determine whether surgery is an appropriate option. By carefully examining both the front and back structures of the eye, the surgeon can identify any conditions that might influence the safety or outcome of the procedure. This step provides a complete understanding of your eye health before moving forward with surgical planning.
- Assessment of the Front of the Eye: The ophthalmologist carefully examines structures such as the cornea, iris, and natural lens. This evaluation helps detect issues like corneal irregularities, cataract severity, or other abnormalities that could affect surgical planning and visual outcomes.
- Evaluation of the Retina and Optic Nerve: A thorough examination of the back of the eye is performed to assess the retina and optic nerve. Identifying conditions such as macular problems or optic nerve damage is essential, as these may influence both the safety of surgery and the expected visual improvement.
- Confirming Suitability for Surgery: The findings from the examination help determine whether lens surgery is the best option for your vision needs. The surgeon uses this information to assess potential benefits, risks, and whether additional tests are required.
- Identifying Other Eye Conditions: If additional eye conditions are detected during the examination, they may need to be treated or closely monitored before surgery. Addressing these issues in advance helps ensure the procedure is as safe and effective as possible.
In conclusion, a comprehensive eye examination is a critical first step in the lens surgery process. By evaluating all major structures of the eye, the surgeon can confirm whether the procedure is appropriate and identify any factors that may influence the outcome. This careful preparation ensures that surgery is both safe and beneficial for improving vision.
Visual Acuity Testing
One of the most familiar tests performed before lens surgery is visual acuity testing. This is the standard eye chart examination used to measure how clearly you can see letters or symbols at different distances. It helps determine how much your current vision has been affected by cataracts or refractive errors such as nearsightedness, farsightedness, or astigmatism.
Visual acuity testing provides an important baseline measurement of your eyesight before surgery. By recording how well you see at different distances, the surgeon gains a clear understanding of the severity of your visual impairment and how significantly the natural lens is contributing to reduced vision. In some cases, additional tests may also be performed to measure how your vision performs under different lighting conditions or with corrective lenses.
After surgery, this baseline allows doctors to compare your new visual performance with your pre-operative results. It helps determine how much improvement has been achieved and whether the chosen intraocular lens is delivering the expected visual outcome. The test also assists the surgeon in identifying whether any remaining visual limitations are related to the lens or to other structures within the eye, such as the retina or optic nerve.
Refraction Assessment
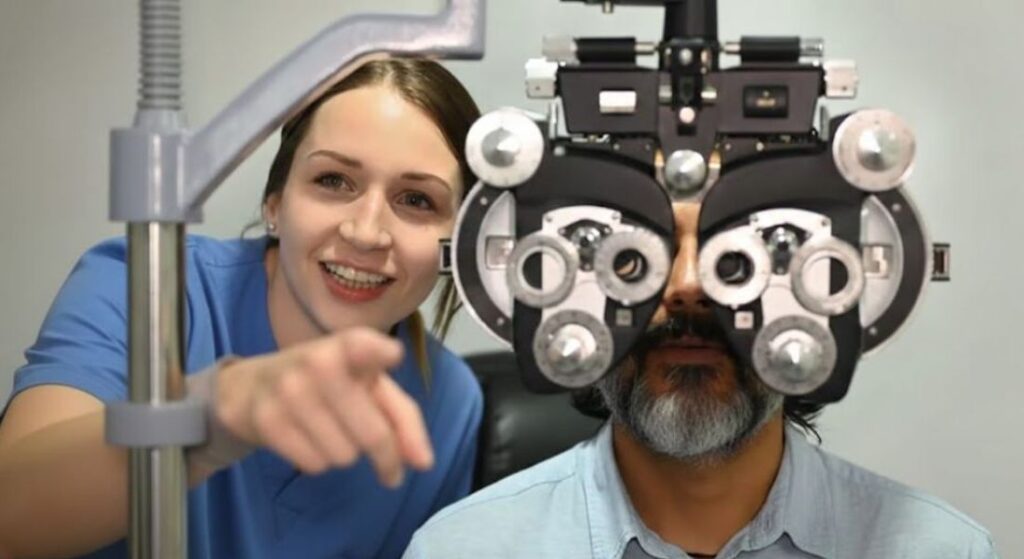
Refraction testing is carried out to determine your current glasses prescription and assess how clearly you see. During this examination, the optometrist measures how light focuses inside your eyes to identify any refractive error. This helps provide an accurate understanding of your present vision. It also forms an important part of the assessment before planning lens surgery.
During the test, different lenses are placed in front of your eyes and you are asked which ones provide the clearest vision. You will usually compare several lens options so the optometrist can refine the prescription step by step. This process helps identify the degree of short-sightedness, long-sightedness or astigmatism that may be affecting your vision. The test is simple, painless and usually completed within a few minutes.
Knowing your exact prescription helps guide the selection of the most suitable intraocular lens power. The measurements collected during refraction are used alongside other eye tests to plan your treatment accurately. This information also helps predict how your vision may change once the cloudy natural lens is replaced. As a result, your surgeon can better estimate the visual outcome after surgery.
Biometry: Measuring the Eye
Biometry is one of the most important diagnostic tests performed before lens surgery. This test measures the physical dimensions of the eye, which are essential for calculating the correct power of the intraocular lens (IOL). Accurate measurements help ensure that the new lens focuses light properly on the retina after surgery. Modern biometry technology provides highly precise data, allowing surgeons to plan the procedure with greater confidence and predictability.
- Measuring Axial Length: Biometry determines the axial length of the eye, which is the distance from the front surface of the cornea to the retina at the back. This measurement is critical because even small variations can affect how the implanted lens focuses light.
- Determining Lens Power: The axial length measurement is used in formulas that calculate the exact power of the intraocular lens required for each patient. Accurate calculations help achieve the desired visual outcome and reduce the likelihood of needing additional vision correction after surgery.
- Using Advanced Optical Technology: Modern optical biometry devices use light-based technology rather than ultrasound to measure the eye. These systems are highly precise and provide detailed data that supports better surgical planning and lens selection.
- Importance of Measurement Accuracy: Even tiny differences in the measurements can influence the clarity of vision after surgery. For this reason, surgeons rely on advanced instruments and repeat measurements when necessary to ensure the most accurate results possible.
In conclusion, biometry is a crucial step in preparing for lens surgery because it provides the precise measurements needed to select the correct intraocular lens. By accurately determining the eye’s axial length and other optical characteristics, surgeons can plan surgery with greater precision. This careful preparation helps maximise the likelihood of achieving clear, stable vision after the procedure.
Corneal Curvature Measurement
Another important part of the pre-operative assessment is measuring the curvature of your cornea. The cornea is the clear, transparent outer layer at the front of your eye that plays a key role in focusing light. Its shape affects how light enters the eye and how clearly images are formed on the retina. Even small variations in corneal curvature can influence your overall prescription and vision quality.
Keratometry is the test used to measure the curvature of the cornea. During this examination, a specialised instrument carefully measures the shape of the front surface of your eye. The test is quick, painless and does not involve touching the eye. It provides precise information about how your cornea bends light.
These measurements are essential when calculating the correct power of the replacement intraocular lens. Accurate corneal data helps your surgeon select a lens that will provide the best possible visual outcome. It can also show whether you have astigmatism that may need correction. In some cases, this information helps determine if a specialised lens, such as a toric lens, would be beneficial for your vision.
Corneal Topography
Corneal topography is a diagnostic test that creates a detailed map of the surface of your cornea. The cornea plays an important role in focusing light, and its shape can affect the clarity of your vision. During this test, advanced imaging technology scans the front of your eye to measure its exact contours. This produces a colour-coded map that shows how evenly the cornea is shaped.
The test can identify very subtle irregularities in the corneal surface that may not be visible during a routine examination. These small variations can influence how light enters your eye and may affect your overall vision. Detecting these details helps your surgeon plan the procedure more accurately. It can also influence the type of intraocular lens that may be most suitable for you.
Corneal topography is particularly useful if you have astigmatism, as it helps determine the precise orientation required for toric lenses. This ensures that the lens is positioned correctly to improve visual clarity. The test is also especially helpful for patients who have previously undergone laser vision correction. In these cases, it provides valuable information about the current shape of the cornea before surgery is planned.
Optical Coherence Tomography (OCT)
Optical coherence tomography, commonly known as OCT, is a high-resolution imaging test used to examine the retina at the back of your eye. The test uses light waves to create very detailed images of the eye’s internal structures. It is completely painless and usually takes only a few minutes to perform. OCT allows your surgeon to assess the health of the retina before planning lens surgery.
During the scan, the machine produces detailed cross-sectional images of the retina and the macula. These structures are responsible for your central vision and your ability to see fine details clearly. By examining these layers closely, your eye specialist can detect even small changes in retinal structure. This level of detail helps provide a clearer understanding of your overall eye health.
OCT is particularly useful for identifying conditions such as macular degeneration, diabetic eye disease and retinal swelling. Detecting these problems before surgery is important because they can influence visual outcomes. If any abnormalities are discovered, your surgeon may adjust the surgical plan or the type of intraocular lens used. This careful evaluation helps ensure that the treatment approach is safe and appropriate for your eyes.
Retinal Examination
A dilated retinal examination is an important part of the pre-operative assessment before lens surgery. This test allows the surgeon to examine the retina thoroughly and identify any conditions that might affect the safety or outcome of the procedure. By widening the pupil with special eye drops, the ophthalmologist gains a clearer and more complete view of the structures at the back of the eye. This careful evaluation helps ensure that the retina is healthy before surgery takes place.
- Pupil Dilation for Better Visibility: During the examination, eye drops are used to widen the pupil, allowing the surgeon to see deeper into the eye. This expanded view makes it easier to detect subtle changes or abnormalities in the retinal tissue that may not be visible through a normal pupil.
- Detection of Retinal Abnormalities: The examination helps identify conditions such as retinal tears, areas of degeneration, or early signs of retinal disease. Recognising these issues before surgery is essential, as they could increase the risk of complications if left untreated.
- Pre-Surgical Treatment if Needed: If retinal problems are discovered, treatment may be recommended before proceeding with lens surgery. For example, preventive laser therapy can sometimes stabilise weak areas of the retina and reduce the risk of future complications.
- Protecting Surgical Outcomes: Ensuring that the retina is healthy before surgery helps reduce the chances of unexpected problems during or after the procedure. A stable retina supports better visual outcomes and contributes to a safer surgical experience overall.
In conclusion, a dilated retinal examination is a vital step in preparing for lens surgery. By carefully examining the retina, surgeons can detect and manage potential problems before the procedure. This proactive approach helps minimise risks and supports the best possible visual results after surgery.
Intraocular Pressure Measurement
Intraocular pressure (IOP) testing measures the pressure inside your eye and forms an important part of the pre-operative eye examination. The pressure within the eye must remain within a healthy range to protect delicate structures such as the optic nerve. During this assessment, your eye care professional uses specialised equipment to measure the internal eye pressure. This information helps provide a clearer picture of your overall eye health before surgery.
The test also helps detect conditions such as glaucoma or ocular hypertension, both of which can damage the optic nerve if they are not properly managed. In most cases, the measurement is quick and painless and may involve a gentle puff of air or a small instrument placed near the eye. The procedure is safe and is routinely performed during eye examinations. Identifying abnormal pressure early allows your doctor to recommend appropriate monitoring or treatment.
Knowing your eye pressure before surgery provides a useful baseline for comparison after the procedure. This allows your surgeon to monitor any changes that may occur during the recovery period. The information can also help determine whether additional precautions are required during surgery. By understanding your eye pressure in advance, your surgical team can plan the procedure with greater safety and precision.
Tear Film and Dry Eye Assessment
A stable tear film is important for both accurate eye measurements and comfortable healing after surgery. The tear film covers the surface of your eye and helps keep it smooth, clear and well protected. When this layer is healthy, light can enter the eye properly and measurements of the cornea are more precise. For this reason, surgeons often evaluate the condition of your tear film during the pre-operative assessment.
Dry eye can sometimes distort the surface of the cornea, which may affect the accuracy of the measurements used for lens calculations. If the ocular surface is not stable, the results of certain tests may vary from one reading to another. This could potentially lead to less precise planning for the procedure. Identifying dry eye beforehand allows your surgeon to address the issue before surgery takes place.
If signs of dry eye are detected, treatment may be recommended before the operation. This may include lubricating eye drops or other therapies designed to improve tear quality. Treating the condition helps restore a smoother and healthier ocular surface. As a result, the measurements used for calculating your intraocular lens power become more reliable.
Pupil Size and Reaction Testing
Your pupil size and the way your pupils respond to light are also important factors in surgical planning. The pupil controls how much light enters your eye, which can influence how certain intraocular lenses perform. During the examination, your eye specialist measures the size of your pupils in different lighting conditions. This helps provide a clearer understanding of how your eyes function in everyday situations.
Some advanced intraocular lenses are designed to work best within specific pupil size ranges. By measuring this characteristic, your surgeon can assess whether particular lens designs are suitable for your eyes. These measurements help guide the selection of lenses that are most likely to provide clear and comfortable vision. Careful evaluation ensures that the chosen lens matches your individual eye characteristics.
For example, larger pupils may increase the risk of visual phenomena such as halos or glare with certain multifocal lenses. Understanding how your pupils behave allows the surgeon to consider these factors when planning your treatment. This helps reduce the likelihood of unwanted visual effects after surgery. As a result, the most appropriate lens type can be selected to suit your vision needs.
Intraocular Lens Power Calculation
After all the necessary eye measurements have been collected, your surgeon uses specialised formulas to calculate the power of the intraocular lens that will be implanted during surgery. These calculations are an essential part of the treatment planning process. The aim is to select a lens that will allow light to focus correctly on the retina after your natural lens has been replaced. Accurate planning helps improve the likelihood of clear vision following the procedure.
The formulas used for these calculations combine information gathered from several tests, including biometry, keratometry and other important measurements of the eye. By analysing this data together, the surgeon can predict how light will travel through your eye after surgery. This allows the lens power to be tailored to your individual eye structure. The process helps ensure that the replacement lens provides the most suitable visual correction.
Accurate calculations are essential for achieving the best possible visual outcome. Modern calculation formulas are highly advanced and take into account multiple anatomical factors, such as the length of the eye and the shape of the cornea. These sophisticated methods have significantly improved the precision of lens surgery planning. As a result, patients today often experience more predictable and reliable vision after surgery.
Lifestyle Discussion and Visual Goals
Testing alone does not determine the final treatment plan for lens surgery. Your lifestyle, hobbies and daily visual activities also play an important role in deciding which type of lens may be most suitable for you. During your consultation, your surgeon will ask questions to understand how you use your vision throughout the day. This discussion helps ensure that the treatment plan reflects your personal needs and expectations.
You may be asked about how often you use computers, read, drive at night or carry out tasks that require close focus. These everyday activities provide valuable information about the type of vision that matters most to you. For example, some people prioritise clear distance vision, while others need greater comfort when reading or using digital devices. Understanding these habits helps guide the decision-making process.
These conversations help determine whether a monofocal, multifocal or extended-depth-of-focus lens may be the most appropriate option. Each lens design offers different visual benefits depending on your lifestyle and preferences. By matching the lens choice to the way you use your eyes every day, surgeons can improve the overall outcome. This personalised approach often leads to greater satisfaction with the final result.
Why These Tests Matter for Surgical Success
Every test performed before lens surgery plays an important role in achieving the best possible visual outcome. Each examination provides specific information about the health and structure of your eyes. When these results are combined, they give your surgeon a complete understanding of your vision. This detailed assessment forms the foundation of effective surgical planning.
Accurate measurements allow surgeons to select the most appropriate intraocular lens and calculate the correct lens power. Precise data helps reduce the chance of unexpected vision changes after surgery. The tests can also identify any underlying eye conditions that may need attention beforehand. Detecting these issues early helps ensure that the procedure is carried out as safely as possible.
Many patients feel reassured knowing that their surgery is planned using careful measurements and detailed diagnostic information. This preparation allows the surgical team to tailor the treatment to your individual eye characteristics. As a result, the procedure can be performed with greater confidence and precision. Thorough pre-operative testing significantly improves both safety and patient satisfaction.
FAQs:
1. What tests are done before lens surgery?
Before lens surgery, several diagnostic tests are performed to assess eye health and measure the eye accurately. These typically include visual acuity testing, refraction assessment, biometry, corneal curvature measurements, retinal examination, intraocular pressure testing and imaging such as optical coherence tomography (OCT). These tests help surgeons plan the procedure and select the correct intraocular lens.
2. Why are so many tests needed before lens surgery?
Multiple tests are required because lens surgery must be tailored to each patient’s eyes. Every eye has unique anatomical features, and accurate measurements are essential to calculate the correct intraocular lens power. The tests also help identify any eye conditions that could affect surgical safety or visual outcomes.
3. What is biometry and why is it important?
Biometry is a diagnostic test that measures the length of the eye and other key dimensions. These measurements are used in formulas that calculate the power of the artificial intraocular lens implanted during surgery. Even very small measurement differences can affect the final visual result, which is why this test is so important.
4. Does the testing before lens surgery hurt?
Most pre-operative eye tests are completely painless and non-invasive. Many involve imaging technology that scans the eye without touching it. Some tests may involve eye drops to dilate the pupils, which can cause temporary blurred vision or light sensitivity for a few hours.
5. Why is corneal curvature measured before surgery?
The curvature of the cornea plays a major role in how light focuses inside the eye. Measuring the corneal shape helps surgeons calculate the correct lens power and determine whether astigmatism is present. This information may influence whether a specialised lens, such as a toric intraocular lens, is recommended.
6. What does OCT scan check before lens surgery?
Optical coherence tomography (OCT) scans the retina and macula at the back of the eye. It creates detailed cross-sectional images that help detect conditions such as macular degeneration, diabetic eye disease or retinal swelling. Identifying these issues before surgery helps surgeons plan treatment more safely.
7. Why is a retinal examination necessary before lens surgery?
A retinal examination allows the surgeon to assess the health of the retina and detect problems such as retinal tears, degeneration or other abnormalities. If any issues are found, they can often be treated before surgery to reduce the risk of complications and protect visual outcomes.
8. Is dry eye testing necessary before lens surgery?
Yes, assessing the tear film and checking for dry eye is important before surgery. Dry eye can affect the accuracy of corneal measurements used for lens calculations. Treating dry eye beforehand helps ensure more reliable measurements and supports smoother healing after the procedure.
9. How long do pre-operative eye tests take?
The full pre-operative assessment usually takes between 60 and 90 minutes. This includes several different tests and may involve pupil dilation. The exact time can vary depending on the clinic and whether additional imaging or specialised examinations are required.
10. Do these tests determine which lens I will receive?
Yes, the results of the pre-operative tests help your surgeon select the most appropriate intraocular lens for your eyes. Measurements such as eye length, corneal curvature and pupil size are combined with information about your lifestyle and visual goals to recommend the most suitable lens type.
Final Thoughts: Careful Testing Supports Safer Lens Surgery
The detailed tests performed before lens surgery are an essential part of ensuring safe treatment and accurate visual outcomes. Each examination provides important information about the structure and health of your eyes, allowing surgeons to measure the eye precisely and calculate the correct intraocular lens power. By combining results from multiple diagnostic tests, your surgeon can create a personalised surgical plan designed to deliver the best possible vision after the procedure.
Although the number of tests may seem extensive, they play a crucial role in improving the safety and predictability of modern eye surgery. Careful pre-operative assessment helps identify potential risks, select the most suitable lens, and plan the procedure with greater precision. If you’re considering Lens Surgery in London, you can get in touch with us at London Cataract Centre.
References:
- Stopyra, W. and Grzybowski, A. (2025) Innovations in intraocular lens power calculation A review, Journal of Clinical Medicine https://www.mdpi.com/2077-0383/14/18/6585
- Olsen, T. (2007) Calculation of intraocular lens power: a review, Acta Ophthalmologica Scandinavica, https://pubmed.ncbi.nlm.nih.gov/17403024/
- Kim, J.S., Lee, H., Kim, E.K. and Kim, T.I. (2021) Improved accuracy of intraocular lens power calculation by preoperative management of dry eye disease, BMC Ophthalmology https://pmc.ncbi.nlm.nih.gov/articles/PMC8515725/
- Saad, E., Shammas, H.J. and Shammas, M.C. (2013) Scheimpflug corneal power measurements for intraocular lens power calculation in cataract surgery, American Journal of Ophthalmology, https://www.sciencedirect.com/science/article/abs/pii/S0002939413003115
- Fata, A.F., Elebiary, H.H., Elewa, L.S. and Elbayomi, A.M. (2020) ‘The effect of short acting mydriatics on intraocular lens power measurement using IOLMaster biometry’, QJM: An International Journal of Medicine https://academic.oup.com/qjmed/article-abstract/113/Supplement_1/hcaa058.021/5829155

