If you are wondering whether cataracts can lead to vision loss in older adults, the simple answer is yes, they absolutely can. Cataracts are one of the most common causes of gradual vision loss in elderly people. However, it is important for you to understand that this usually develops slowly over time rather than happening suddenly.
What makes cataracts particularly challenging is that the changes in your vision often happen so gradually that you may not realise how much your sight has been affected. You might adapt without noticing at first, even as the condition progresses. Over time, everyday activities can begin to feel more difficult than they used to be.
Tasks such as reading, recognising familiar faces, or driving at night may start to become frustrating for you. This is because the natural lens inside your eye becomes increasingly cloudy, reducing the sharpness of what you see. As the clouding worsens, your vision can feel dimmer, blurrier, or less reliable in different lighting conditions.
The good news is that cataracts do not usually cause irreversible blindness. In most cases, the vision loss linked to cataracts can be treated effectively. With timely diagnosis and cataract surgery when needed, your vision can often be greatly improved, helping you see more clearly and regain confidence in your daily routine.
Understanding Why Your Vision Feels Different
If you have noticed your vision becoming less sharp, more inconsistent, or slightly “off” compared to how it used to be, you should know this is extremely common as you get older. These changes usually do not happen overnight, which is why many people ignore them for a long time. You might also assume it is just tiredness, lighting, or simply needing a new glasses prescription.
What often begins as small visual discomfort can slowly develop into something more noticeable in your daily life. At first, you may not think much of it because the changes feel minor and easy to adapt to. However, over time, these small difficulties can gradually build up and start to affect how clearly you see in different situations.
You may find yourself struggling more with reading, recognising faces at a distance, or adjusting between bright and dim lighting. These everyday challenges can feel frustrating because your vision does not feel as quick or clear as it once did. These early signs are often linked to age-related changes such as cataracts, even when they seem mild at first.
What Cataracts Actually Are
A cataract is a condition where the natural lens inside your eye gradually becomes cloudy instead of staying clear. This lens plays a vital role in focusing light properly onto the back of your eye so you can see sharp, detailed images. When it becomes cloudy, the light is scattered, which causes your vision to become blurred or hazy.
It helps you to think of it like looking through a slightly frosted or misted-up window. The world around you are still there and unchanged, but the clarity is reduced. This is why objects may not appear as sharp or bright as they once did, even if your surroundings have not changed.
Over time, this clouding can slowly increase and affect your vision more noticeably. As it progresses, everyday tasks such as reading, watching television, or moving around in bright or dim light can become more visually challenging for you.
How Cataracts Begin to Form
Cataracts usually begin forming as part of the natural ageing process, although the changes inside your eye happen very gradually. Over time, the proteins within your eye’s lens begin to break down and clump together. This slowly reduces the lens’s transparency, making your vision less clear.
This is not something that happens suddenly, which is why you may not notice it for a long time. The changes are often so gradual that your brain and eyes adapt without you consciously realising it. Because of this, early cataracts can easily go unnoticed in the beginning stages.
At first, these changes may be so mild that you simply adjust your daily habits without thinking much about it. You might find yourself using brighter lighting, changing how you read, or relying more on your glasses. You may not realise that these small adjustments are happening because a cataract is slowly developing in the background.
Why Age Is the Biggest Risk Factor
Age is the most significant risk factor for cataracts because the natural lens of your eye changes over time. Just like other parts of your body, your eyes experience gradual wear and tear as you get older. The proteins in the lens slowly lose their original structure, which makes clouding more likely to develop.
As you age, these changes build up little by little rather than happening all at once. This is why cataracts are strongly linked to the ageing process, even though you may not notice anything in the early stages. Your vision can still feel normal for quite some time before symptoms become clearer.
Most people begin to notice cataract-related changes after the age of 60, although the process often starts much earlier at a microscopic level. It is a natural part of ageing, even if it feels frustrating or unexpected when it begins to affect your sight. Understanding this can help you recognise why your vision is changing and when to seek advice.
Early Signs You Should Watch For
Early changes in vision can often develop so gradually that you may not immediately realise something is different. One of the first signs of cataracts is a mild blurring of vision that does not fully improve even when you use glasses. This can create a sense that your eyesight is not as sharp as it used to be, even if daily activities still feel manageable. Because the changes are subtle, they are often dismissed as normal ageing at first.
- Subtle Blurring of Vision: One of the earliest indicators is a gentle but persistent blur that does not fully clear with corrective lenses. You might feel like your vision is slightly out of focus, especially when reading or looking at fine detail. This blurring can come and go, making it easy to ignore initially.
- Feeling That Vision Is “Not Quite Right”: You may struggle to describe exactly what has changed, but something feels off with your eyesight. Objects may not appear as crisp or clear as before, even in good lighting. This vague sense of reduced clarity is often an early warning sign.
- Increased Need for Brighter Lighting: You might find that you need stronger lighting to read or perform close-up tasks comfortably. Activities that were once easy in normal lighting may now feel dim or less clear. This change often develops slowly over time.
- Difficulty Seeing Fine Details: Small print, intricate patterns, or detailed work may start to feel harder to distinguish. This happens as the eye’s lens becomes less transparent, reducing sharpness. Because the change is gradual, you may adapt without realising it is happening.
In conclusion, early signs like mild blurring, increased lighting needs, and reduced clarity are often the first hints of cataract development. These changes tend to progress slowly, making them easy to overlook in daily life. Paying attention to small differences in your vision can help you identify issues earlier. If you notice these signs persisting, an eye examination can provide clarity and reassurance.
Changes in Night Vision

Difficulty seeing clearly at night is one of the more noticeable early symptoms of cataracts. You may find that driving after dark becomes increasingly uncomfortable for you, especially when you are faced with bright oncoming headlights or strong street lighting. These situations can make it harder for your eyes to adjust quickly.
The lights may start to appear more glaring, scattered, or even slightly blurred compared to how you used to see them. This can reduce your confidence when moving around in low-light conditions. As a result, night-time activities may begin to feel less safe or more stressful than before.
This change in your night vision is often one of the key reasons people decide to seek an eye examination. It can be particularly noticeable because it directly affects everyday tasks such as driving or walking in the evening. Recognising this symptom early can help you take the right steps to protect your vision and safety.
Sensitivity to Light Becomes Noticeable
As cataracts progress, you may start to notice that you become more sensitive to bright light, both indoors and outdoors. Sunlight that once felt completely normal may now feel uncomfortably harsh for you. As a result, you may find yourself squinting more often or turning away from bright light without realising it.
This happens because the cloudy lens inside your eye scatters light instead of allowing it to focus clearly on the back of your eye. When light is not focused properly, it can feel more intense and less controlled. This is why bright environments may start to feel uncomfortable or overwhelming.
The result of this change is a sense of discomfort in well-lit spaces, which can slowly affect your daily routine. You may begin to avoid very bright outdoor areas or prefer dimmer indoor lighting where your eyes feel more relaxed. Over time, this can influence how confident you feel in different lighting conditions.
Colours Start to Look Dull
Another subtle but important change you may notice is the way colours appear to you. You might find that whites no longer look as bright as they used to and can start to appear slightly yellowed. In the same way, vibrant colours may begin to look faded or less striking than before.
This happens because the clouding in your eye’s lens affects how light is filtered and transmitted. Instead of allowing light to pass through clearly, the lens begins to distort and scatter it. As a result, your perception of colour can slowly change without you immediately realising it.
Over time, this can also impact how you see contrast and brightness in your surroundings. You may notice that images and objects appear less vivid or slightly muted compared to how they once looked. This gradual shift can make the world feel less sharp and colourful overall.
Difficulty Reading Small Print

Reading is often one of the first everyday tasks you notice being affected by cataracts. You may find it harder to read books, newspapers, restaurant menus, or even text on your mobile phone. You might also start holding reading material further away or increasing the font size more often than before.
These small adjustments can become a regular habit for you without you fully realising it at first. What once felt quick and effortless may now require more concentration and effort. Over time, this can make reading feel more tiring than it used to.
Even if you have updated your glasses, you may still feel that the clarity is not quite right. This is because the problem is not only related to your prescription. Instead, it is also linked to how light is being processed and scattered inside your eye due to the developing cataract.
Frequent Prescription Changes
You may notice that your glasses prescription needs to be updated more often than it used to. At first, it might feel like your eyesight is simply getting worse over time. However, cataracts can actually be the underlying reason for this frequent change and instability in your vision.
New glasses may give you a temporary improvement in clarity, which can feel reassuring at first. You might see slightly better for a short time after getting them. However, this improvement often does not last because the root cause is not being fully addressed.
This is because glasses can only correct how light enters your eyes, not the clouding inside the natural lens. As a result, your vision may continue to feel inconsistent even after prescription updates. Over time, this can become frustrating as your glasses seem less effective than expected.
Cloudy or Blurry Vision That Worsens Gradually
Cataracts often develop slowly, which means the changes in your vision can be easy to miss at first. Instead of a sudden loss of sight, you may notice a gentle clouding or blurring that becomes more noticeable over time. Because the progression is so gradual, your brain often adjusts, making the issue feel less obvious in the early stages. This is why many people only realise the extent of the problem much later.
- Slow and Progressive Vision Changes: Cataracts typically cause a steady decline in clarity rather than an immediate drop in vision. You may find that things look slightly hazy or less sharp from week to week or month to month. This slow change can make it difficult to recognise how much your eyesight has actually shifted.
- Brain Adaptation to Blurred Vision: Your brain has a way of adapting to gradual changes in sight, which can mask early symptoms. Over time, you may unconsciously adjust how you see things without realising your vision is declining. This adaptation often delays awareness of the problem.
- Changes Become Noticeable in Comparison: Many people only become aware of vision loss when they compare current sight to older experiences. This might happen during an eye test or when noticing difficulty with tasks that were once easy. The difference becomes clearer when looked at side by side with past vision.
- Worse Clarity in Certain Lighting Conditions: Blurriness caused by cataracts often stands out more in specific lighting, such as bright sunlight or dim indoor settings. In these situations, glare or haze can make vision noticeably more uncomfortable. Over time, these conditions may begin to affect everyday activities.
In conclusion, cloudy or blurry vision from cataracts tends to worsen gradually, making it easy to overlook in the beginning. The slow progression and brain’s ability to adapt often delay recognition of the issue. However, small changes in clarity and lighting sensitivity can be early warning signs. Regular eye checks can help identify these changes before they significantly affect your daily life.
How Cataracts Affect Daily Life
As cataracts progress, they begin to affect everyday tasks that you may have previously taken for granted. Simple activities such as cooking, reading labels, watching television, or recognising people at a distance can gradually become more difficult and take more time than they used to.
You may start to notice that these tasks require more effort and concentration from you. What once felt quick and easy can slowly become frustrating or tiring. This change often happens so gradually that you adjust without realising how much your vision has changed.
Over time, this can lead to frustration and a gradual reduction in your independence. You might find yourself relying more on other people for help or avoiding certain situations where clear vision is important. These changes can have a noticeable impact on your confidence in daily life.
Emotional Impact of Vision Loss
Vision changes do not only affect your eyes; they can also have an impact on how you feel emotionally. You may begin to feel less confident when moving around in unfamiliar places or feel hesitant about going out alone. These feelings can develop gradually as your vision becomes less reliable.
It is completely natural for you to feel this way when your vision starts to become unpredictable. Not being able to see clearly can make everyday situations feel more uncertain or uncomfortable than before. This can sometimes affect your sense of independence as well.
Many people experience feelings of frustration or worry before they fully understand what is causing the change in their vision. You might find yourself feeling unsure about why things have become more difficult. Once the cause is identified, it often becomes easier to manage both the condition and the emotions linked to it.
When Cataracts Become a Serious Problem
Cataracts become a more serious issue when they begin to interfere significantly with your quality of life. If you find that reading, driving, or recognising faces is consistently difficult, it may be a sign that you need to start considering treatment options. At this point, the changes in your vision are no longer just mild inconveniences.
Your vision can start to affect your safety and independence in everyday situations. You may feel less confident carrying out normal activities, especially those that require clear and reliable eyesight. This can make daily life more challenging than it used to be for you.
This stage is usually when people are advised to explore surgical treatment options. Cataract surgery is often recommended because it can effectively restore clearer vision. Seeking professional advice at this point can help you understand the best next steps for your eye health.
How Cataracts Are Diagnosed
Diagnosing cataracts is usually straightforward and completely painless for you. An eye specialist will carefully examine your eye using a slit lamp, which allows them to view the lens in detail. This helps them clearly see any clouding that may be affecting your vision.
During the examination, the specialist can assess how much the cataract has developed. You do not need to worry, as the process is quick and non-invasive. It is simply a detailed check to understand the condition of your eye health.
You may also be asked to complete a vision test to measure how much your sight has been affected. This helps the specialist understand how the cataract is impacting your daily vision. Based on these results, they can determine the severity of the cataract and suggest the most suitable next steps for treatment.
Treatment Options Available
Cataracts cannot be reversed with medication, but there are ways to manage symptoms in the early stages. These temporary measures can help improve your vision and make daily activities more comfortable. However, they do not stop the cataract from gradually progressing over time. Understanding your options can help you decide when further treatment may be needed.
- Stronger Lighting and Visual Aids: In the early stages, improving your environment can make a noticeable difference. Brighter lighting helps reduce strain and makes reading or close work easier. Magnifying tools and anti-glare lenses may also provide temporary relief.
- Updated Prescription Glasses: As cataracts develop, your vision may change frequently, requiring updates to your glasses. New prescriptions can improve clarity for a while, especially for reading or distance vision. However, this is usually only a short-term solution.
- Lifestyle Adjustments: Small changes such as reducing glare, using larger print, or avoiding low-light reading can help manage symptoms. These adjustments make daily tasks more comfortable but do not address the underlying condition. Over time, their effectiveness may decrease.
- Cataract Surgery as the Only Permanent Solution: The only definitive treatment is cataract surgery, where the cloudy natural lens is removed and replaced with a clear artificial lens. This procedure restores vision by allowing light to pass clearly through the eye again. It is one of the most commonly performed and highly successful eye surgeries worldwide.
In conclusion, early cataract management focuses on improving comfort rather than curing the condition. While glasses, lighting, and lifestyle changes can help temporarily, they do not stop progression. Surgery remains the only long-term and effective solution for restoring clear vision. If symptoms begin to affect your daily life, discussing surgical options with an eye specialist is an important step.
What Cataract Surgery Involves
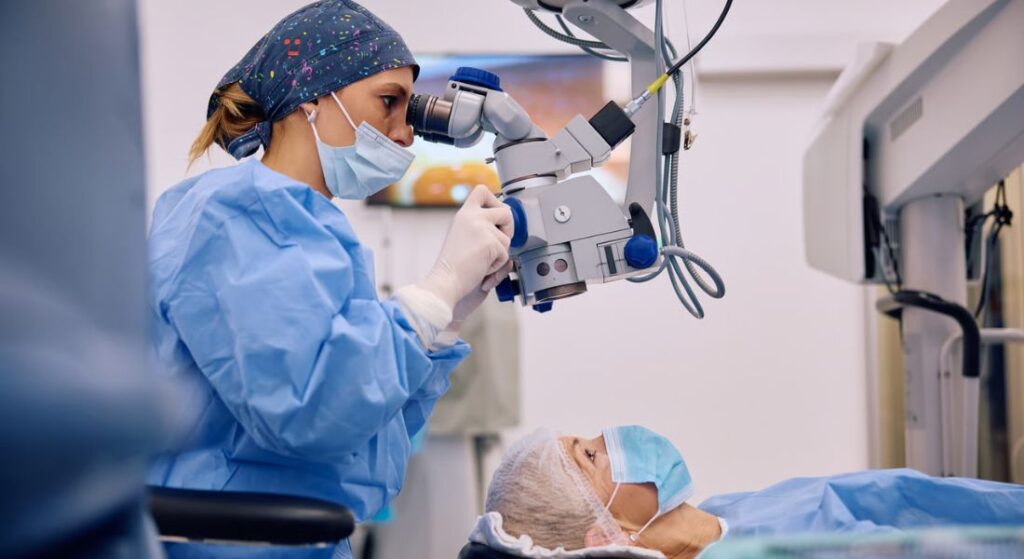
Cataract surgery is one of the most commonly performed and successful medical procedures worldwide. It is generally recommended when cataracts begin to significantly affect your vision and daily life. The procedure is usually carried out under local anaesthetic, which means you remain awake but your eye is numbed so you do not feel pain.
During the surgery, the cloudy natural lens inside your eye is carefully removed. It is then replaced with a clear artificial lens designed to restore clearer vision. This new lens helps light focus properly again, improving how you see.
The procedure is typically quick, and you will not need to stay in hospital overnight. Most people are able to go home the same day after a short recovery period. Many patients notice an improvement in their vision shortly after the operation.
Recovery and Life After Surgery
After cataract surgery, many people notice an improvement in their vision within just a few days. You may find that colours look brighter, sharper, and more natural than they have for years. This early improvement can feel very noticeable as your vision begins to clear.
Your recovery is usually smooth as long as you follow the aftercare instructions given to you. This typically includes using prescribed eye drops and avoiding heavy strain or rubbing your eye. These simple steps help support proper healing and reduce the risk of complications.
Over time, you can gradually return to your normal daily activities with much clearer vision. Most people experience a significant improvement in their overall quality of life. Tasks that once felt difficult often become easier and more comfortable again.
FAQs:
1. Can cataracts cause complete blindness in older adults?
Cataracts can cause severe vision impairment if left untreated, but they rarely lead to permanent blindness. In most cases, vision can be restored effectively with surgery.
2. How quickly do cataracts worsen?
Cataracts usually progress slowly over months or years. The rate varies from person to person, but changes in vision are typically gradual rather than sudden.
3. What are the first signs of cataracts?
Early signs include slightly blurred vision, increased sensitivity to light, difficulty reading small print, and needing brighter lighting for daily tasks.
4. Are cataracts painful?
No, cataracts are not painful. They affect the clarity of your vision but do not usually cause physical discomfort in the eye.
5. Can glasses fix cataracts?
Glasses may temporarily improve vision in the early stages, but they cannot treat or stop cataracts from progressing.
6. At what age do cataracts usually start?
Cataracts most commonly begin to develop after the age of 60, although early changes in the lens can start much earlier without noticeable symptoms.
7. When should I consider cataract surgery?
Surgery is usually recommended when cataracts begin to interfere with daily life, such as driving, reading, or recognising faces.
8. Is cataract surgery safe for elderly patients?
Yes, cataract surgery is one of the safest and most commonly performed procedures worldwide, with a high success rate even in older adults.
9. How long does recovery from cataract surgery take?
Most people notice improved vision within a few days, with full recovery typically occurring over a few weeks.
10. Can cataracts come back after surgery?
Cataracts themselves do not return after surgery. However, some people may develop a condition called posterior capsule opacification, which can be treated easily with a quick laser procedure.
Final Thoughts: Cataracts, Vision Loss, and Taking the Right Next Step
Cataracts are a common age-related condition that can gradually lead to vision loss in older adults. The changes often develop slowly, meaning you may not immediately notice how much your sight has been affected until everyday tasks such as reading, driving, or recognising faces become more difficult. Although this progression can feel concerning, it is important to remember that cataracts are a well-understood condition with effective treatment options available.
With regular eye examinations and early diagnosis, cataracts can be monitored and managed before they significantly impact your daily life. When the condition begins to interfere with independence or quality of vision, cataract surgery offers a safe and highly successful solution to restore clarity. Most people experience a noticeable improvement in their sight and overall confidence after treatment.
If you notice persistent changes in your vision, seeking professional advice is the best next step. Early action can make a meaningful difference in protecting your eyesight and maintaining your quality of life. If you’re looking to enhance your vision or need personalised guidance, our specialist team at the London Cataract Centre is here to help.
Reference:
- Quillen, D.A. (1999) Common causes of vision loss in elderly patients, American Family Physician, 60(1), pp. 99-108. Available at: https://pubmed.ncbi.nlm.nih.gov/10414631/
- Driscoll, R., Scantling‑Brown, H., Margrain, T. and others. (2021) A systematic review of the accessibility, acceptability, safety, efficiency, clinical effectiveness, and cost‑effectiveness of private surgical facilities. BMC Health Services Research. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11570012/
- Harvey, P.T. (2003) Common eye diseases of elderly people: identifying and treating causes of vision loss, Gerontology, 49(1), pp. 1-11. Available at: https://pubmed.ncbi.nlm.nih.gov/12457044/
- Ouyang, S. et al. (2023) Cataract, glaucoma, and diabetic retinopathy as risk factors in older adults, Geriatric Nursing, 53, pp. 170-174. Available at: https://pubmed.ncbi.nlm.nih.gov/37540912/
- Dinarvand, D., Panthakey, J., Hassan, A. and Ahmed, M.H. (2024) Frailty and visual impairment in elderly individuals: Improving outcomes and modulating cognitive decline through collaborative care, Diseases, 12(11), p. 273. Available at: https://www.mdpi.com/2079-9721/12/11/273

