Choosing the right lens for lens replacement surgery is one of the most important factors in achieving the best possible visual outcome. When surgeons discuss this topic with patients, one of the most common questions is how the appropriate intraocular lens (IOL) is selected. The decision is not based on a single measurement but rather on a detailed evaluation of your eyes, vision needs, and lifestyle preferences.
Lens replacement surgery involves removing the eye’s natural lens and replacing it with a clear artificial lens. Although the surgical procedure itself is highly refined and widely performed, the success of the operation depends heavily on selecting the correct lens. The chosen lens will determine how light is focused within the eye and how well you see at different distances after surgery.
To make the best recommendation, surgeons consider several factors, including your current prescription, corneal shape, eye health, and daily visual tasks such as reading, driving, or computer work. These factors help determine whether a lens designed for distance vision, multiple focal points, or astigmatism correction is most appropriate.
The goal of this personalised approach is to align the technical measurements of the eye with the patient’s visual priorities. By carefully balancing these elements, surgeons can recommend a lens that provides clear, comfortable vision while supporting the level of independence from glasses that each patient hopes to achieve.
Understanding Intraocular Lenses
Intraocular lenses are artificial lenses designed to replace the natural lens inside the eye during lens replacement surgery. These lenses are made from highly advanced, biocompatible materials that remain safely inside the eye for life. Modern intraocular lenses are carefully engineered to provide clear vision while maintaining comfort and stability within the eye.
There are several types of intraocular lenses available, each designed to address different visual needs. Monofocal lenses focus light at a single distance, usually for clear distance vision. Multifocal and extended depth-of-focus lenses are designed to provide vision at multiple distances, helping some patients reduce their reliance on glasses. Toric lenses are specifically developed to correct astigmatism by compensating for irregular corneal curvature.
Selecting the right lens involves more than simply choosing a design. Surgeons carefully match the lens type and power to the measurements of your eye, as well as your lifestyle requirements and visual goals. This personalised approach ensures that the chosen lens provides the best possible balance of clarity, comfort, and functional vision after surgery.
Assessing Visual Priorities

Before selecting an intraocular lens for surgery, it is important to understand a patient’s visual priorities and daily lifestyle needs. Different lens types provide different visual benefits, so the choice should reflect how you use your vision throughout the day. Some patients prioritise clear distance vision, while others prefer stronger near vision for reading or close-up tasks. By discussing these preferences in detail, the surgeon can recommend a lens that aligns with both your visual goals and everyday activities.
- Distance Vision for Daily Activities: Many patients prioritise clear distance vision for tasks such as driving, watching television, or recognising faces at a distance. In these cases, lenses designed to optimise distance clarity may be recommended. This approach can significantly improve confidence and safety in everyday activities.
- Near Vision for Reading and Hobbies: Patients who spend a lot of time reading, sewing, or performing other close-up tasks may place greater importance on near vision. Selecting a lens that supports these activities can make daily routines more comfortable and reduce reliance on reading glasses.
- Balancing Multiple Visual Needs: Some individuals prefer a balance between near and distance vision rather than focusing on one specific range. In these situations, certain lens designs may provide functional vision at several distances, supporting a variety of everyday tasks.
- Choosing the Appropriate Lens Type: Once visual priorities are clearly understood, the surgeon can recommend the most suitable lens option. This might involve selecting a monofocal lens for a single focal point or considering multifocal or extended depth-of-focus lenses to address multiple visual ranges.
In conclusion, assessing visual priorities is a key step in choosing the right intraocular lens for surgery. By understanding how patients use their vision in daily life, surgeons can tailor the lens selection to match individual needs. This personalised approach helps maximise satisfaction and ensures the best possible visual outcome after surgery.
Evaluating Prescription and Eye Measurements
Surgeons begin the lens selection process by carefully evaluating your current prescription along with detailed measurements of the eye. These measurements include factors such as corneal curvature, axial length, and the presence of any refractive errors like myopia, hyperopia, or astigmatism. Together, these values provide a comprehensive picture of how light is currently focused within your eye.
Advanced biometric testing is used to calculate the precise lens power required for the artificial intraocular lens. Modern diagnostic devices can measure the eye with remarkable accuracy, allowing surgeons to predict post-operative visual outcomes more reliably. Accurate calculations help minimise the chance of residual refractive errors and reduce the need for glasses after surgery.
Because every eye has unique characteristics, these measurements are essential for personalising the procedure. By analysing your eye’s specific anatomy and refractive profile, surgeons can recommend a lens that best supports clear, comfortable vision and aligns with your visual goals.
Considering Lifestyle Factors
Lifestyle plays an important role in determining the most suitable intraocular lens. Surgeons often ask detailed questions about your daily activities, hobbies, and visual priorities because different lenses perform better in different situations. For example, someone who frequently drives at night may benefit from a lens designed to minimise glare and halo effects around lights.
Patients who spend long hours working on computers, reading, or performing tasks that require focus at intermediate distances may prefer lenses that provide stable vision at arm’s length. Similarly, individuals involved in sports or active outdoor lifestyles may prioritise strong contrast sensitivity and crisp distance vision to support movement, depth perception, and quick visual response.
By understanding how you use your vision throughout the day, surgeons can recommend a lens that aligns with your lifestyle and personal expectations. This personalised approach helps ensure that the visual outcome supports everyday activities, improves comfort, and enhances long-term independence from glasses wherever possible.
Monofocal Lenses
Monofocal lenses are the most commonly used type of intraocular lens in lens replacement surgery. These lenses are designed to focus vision at a single distance, most often for clear distance vision. As a result, patients who choose monofocal lenses may still need reading glasses for near tasks such as reading books, using smartphones, or performing detailed work.
One of the main advantages of monofocal lenses is their reliability and predictability. Because they focus light at a single point, they tend to provide sharp, stable vision with fewer visual disturbances. Patients who receive monofocal lenses generally experience lower rates of glare, halos, or contrast sensitivity issues compared with some premium lens designs.
For this reason, monofocal lenses are often recommended for patients who prefer a straightforward solution or who have underlying eye conditions such as macular degeneration or glaucoma. In these cases, maintaining clear, high-quality vision with minimal visual side effects is often more important than achieving complete independence from glasses.
Multifocal Lenses
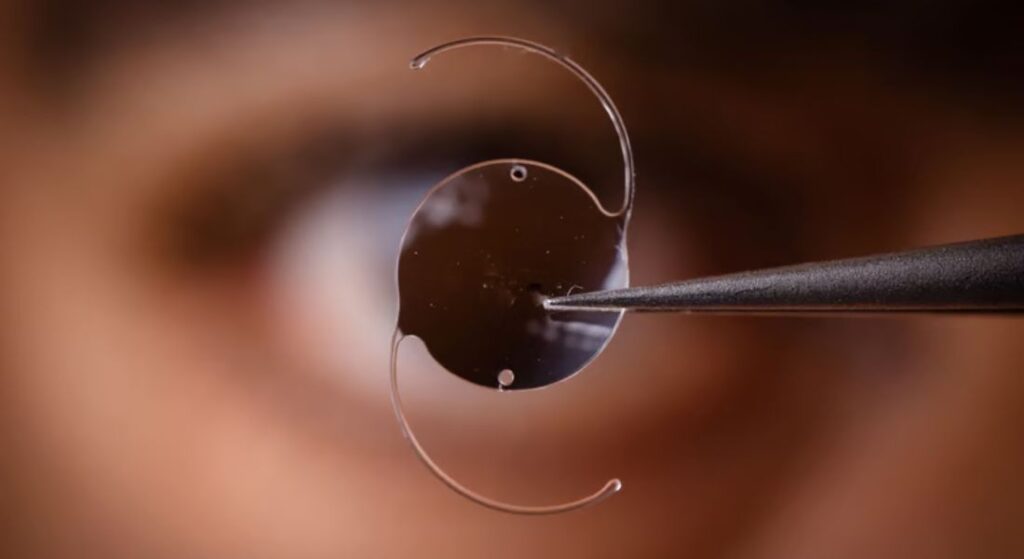
Multifocal lenses are designed to provide vision at more than one distance by creating multiple focal points within the same lens. This allows patients to see clearly at both near and distance ranges, and in some cases at intermediate distances as well. As a result, many people who choose multifocal lenses experience reduced dependence on glasses for everyday activities such as reading, using a phone, or driving.
These lenses use advanced optical designs to distribute light across different focal zones. While this technology can provide greater visual flexibility, it may also introduce certain visual phenomena. Some patients notice halos or glare around lights, particularly at night or in low-light environments, although many adapt to these effects over time.
Because of these characteristics, multifocal lenses are best suited for patients who prioritise independence from glasses and are comfortable with the potential trade-offs. A thorough discussion with the surgeon helps ensure that expectations are realistic and that the lens choice aligns well with the patient’s lifestyle, visual habits, and tolerance for possible visual effects.
Extended Depth-of-Focus (EDOF) Lenses
Extended Depth-of-Focus (EDOF) lenses are designed to provide a smooth and continuous range of vision, particularly between distance and intermediate ranges. Unlike traditional lenses that focus on a single point, EDOF lenses extend the depth of focus to allow clearer vision across multiple distances. This design helps many patients perform everyday tasks with less reliance on glasses. They are especially useful for people who frequently use computers or engage in activities that require clear intermediate vision.
- Continuous Range of Vision: EDOF lenses work by stretching the eye’s focus rather than creating multiple distinct focal points. This allows patients to experience clear distance and intermediate vision without abrupt transitions between viewing ranges. As a result, many daily activities such as walking, driving, and using digital devices become more comfortable.
- Ideal for Intermediate Tasks: Patients who spend significant time on computers, tablets, or other digital screens often benefit from EDOF lenses. The intermediate vision provided by these lenses supports tasks like office work, cooking, or viewing dashboards while driving.
- Reduced Night-Time Visual Disturbances: Compared with multifocal lenses, EDOF lenses often produce fewer visual side effects such as halos or glare around lights at night. This can make them a more comfortable option for patients who frequently drive in low-light conditions.
- Individual Suitability Assessment: Not every patient is an ideal candidate for EDOF lenses. Surgeons evaluate eye measurements, overall eye health, and visual priorities to determine whether this lens type will provide the best outcome.
In conclusion, EDOF lenses offer a modern approach to vision correction by providing a continuous range of focus, particularly between distance and intermediate vision. They are well suited for patients who frequently perform tasks at intermediate distances and want reduced dependence on glasses. Careful assessment by the surgeon ensures that the lens choice aligns with the patient’s eye health and lifestyle needs.
Toric Lenses for Astigmatism
Astigmatism occurs when the cornea has an irregular curvature, causing light to focus unevenly on the retina. This can lead to blurred or distorted vision at both near and far distances. Toric intraocular lenses are specifically designed to correct this type of refractive error during lens replacement surgery.
For patients with moderate to significant astigmatism, a toric lens can significantly improve visual clarity and reduce dependence on glasses. By compensating for the uneven curvature of the cornea, the lens helps focus light more accurately within the eye, supporting clearer and more stable vision across different viewing distances.
Accurate alignment of a toric lens is essential for achieving the desired result. Surgeons rely on detailed pre-operative corneal measurements to determine the correct lens power and axis of placement. Precise positioning ensures that the lens effectively neutralises astigmatism and delivers optimal visual outcomes after surgery.
Addressing Eye Health Conditions
Existing eye conditions play an important role in determining the most appropriate intraocular lens for lens replacement surgery. Conditions such as retinal disease, glaucoma, or significant dry eye can influence how well certain lens designs perform. In these situations, surgeons may recommend monofocal lenses, as they tend to provide stable vision with fewer optical side effects.
Before recommending a lens, surgeons carefully evaluate several aspects of eye health, including retinal function, intraocular pressure, and the condition of the cornea and ocular surface. These assessments help ensure that the chosen lens supports the eye’s overall health rather than introducing unnecessary visual challenges or complications.
By taking existing eye conditions into account, surgeons can tailor lens selection to each patient’s clinical situation. This careful balance between eye health and visual goals helps optimise both surgical safety and long-term visual outcomes.
Predicting Visual Outcomes
Advances in ophthalmic technology have made it possible to predict visual outcomes after lens surgery with impressive accuracy. Modern planning tools combine detailed biometric measurements with specialised software to estimate how the eye will function after the new intraocular lens is implanted. This process helps surgeons plan the procedure more precisely and align the surgical approach with the patient’s visual goals. By analysing multiple factors in advance, surgeons can also provide patients with realistic expectations about their potential results.
- Using Biometric Data for Precision: Measurements such as the length of the eye, corneal curvature, and astigmatism are entered into advanced calculation systems. These data points allow the software to determine the most suitable lens power and predict how light will focus inside the eye after surgery.
- Simulating Post-Surgery Vision: Predictive software can estimate how clearly a patient may see at different distances after lens implantation. This simulation helps surgeons explain the likely visual outcome and discuss whether glasses might still be required for certain tasks.
- Guiding Lens Selection: By analysing biometric data and visual priorities, surgeons can compare how different lens types may perform. This information supports the decision between options such as monofocal, multifocal, or extended depth-of-focus lenses.
- Managing Patient Expectations: Accurate predictions allow surgeons to explain the realistic benefits and limitations of surgery. When patients understand the expected results beforehand, they are more likely to feel satisfied with their final visual outcome.
In conclusion, predictive planning plays a key role in modern lens surgery. By combining biometric measurements with advanced software, surgeons can estimate post-operative vision with greater precision. This approach helps guide lens selection, improve surgical accuracy, and ensure that patients have clear and realistic expectations about their visual results.
Patient Consultation and Shared Decision-Making

Lens selection is a collaborative process between the surgeon and the patient. During the consultation, the surgeon explains the available lens options, their advantages, and any potential trade-offs associated with each design. This discussion helps patients understand how different lenses may affect their vision after surgery and what level of spectacle independence they can realistically expect.
A key part of this process involves understanding the patient’s lifestyle and visual priorities. Factors such as reading habits, computer use, night driving, and tolerance for possible visual phenomena like glare or halos are all considered. By discussing these elements openly, the surgeon can recommend a lens that aligns with both the patient’s daily activities and their expectations for visual performance.
Shared decision-making allows patients to take an active role in planning their treatment. When patients fully understand the options and feel involved in the decision, they are more confident about the surgery and better prepared for the visual outcomes that follow. This collaborative approach helps ensure that the final lens choice supports both medical safety and long-term satisfaction with vision.
Balancing Expectations and Realistic Outcomes
Even when the most suitable intraocular lens is selected, it is important for patients to have realistic expectations about the results of lens replacement surgery. While many people experience significant improvements in vision, some may still require reading glasses or occasional visual aids for certain tasks after the procedure. Understanding these possibilities helps patients approach surgery with a balanced perspective.
Surgeons carefully explain what outcomes are achievable based on your eye measurements, the overall health of your eyes, and the type of lens chosen. Factors such as astigmatism, retinal health, and lifestyle demands can influence how your vision performs after surgery. Discussing these elements in advance ensures that patients understand both the benefits and the limitations of the procedure.
Clear and honest communication is essential for achieving high patient satisfaction. When expectations are aligned with realistic surgical outcomes, patients are more likely to feel confident about their treatment and pleased with the improvements in their vision and quality of life.
Planning for Long-Term Vision
Choosing the right intraocular lens is not only about improving vision immediately after surgery but also about planning for long-term visual needs. Because the artificial lens implanted during lens replacement surgery is designed to remain in the eye permanently, surgeons carefully consider how the choice will support vision over many years.
Although the lens itself does not age, the eye continues to change over time. Factors such as natural ageing of the retina, changes in the vitreous, or the development of other eye conditions can influence visual performance in the future. Selecting a lens that provides stable and reliable vision helps ensure that patients maintain functional sight even as their eyes evolve.
Taking this long-term perspective allows surgeons to recommend lenses that balance current visual goals with future eye health. By planning ahead, patients are more likely to maintain visual independence, clarity, and comfort for many years after their lens replacement surgery.
The Role of Specialist Centres
Experienced centres such as the London Cataract Centre play an important role in guiding patients through the lens selection process. These specialist clinics provide comprehensive assessments that go beyond basic measurements, allowing surgeons to fully understand the unique characteristics of each patient’s eyes and visual needs.
By combining advanced biometric testing with detailed consultations, specialist centres can evaluate factors such as corneal shape, axial length, ocular health, and lifestyle requirements. This information helps surgeons recommend the most suitable intraocular lens from a wide range of available options, ensuring the choice is tailored to both medical and personal considerations.
Consulting a specialist centre also means benefiting from surgeons who have extensive experience with different lens technologies and surgical techniques. This expertise, together with careful planning and personalised guidance, increases the likelihood of achieving the visual clarity and independence that patients hope to gain from lens replacement surgery.
FAQs:
1. How do surgeons decide which lens is best for lens replacement surgery?
Surgeons choose the most suitable intraocular lens by analysing detailed eye measurements, the patient’s prescription, overall eye health, and lifestyle needs. Factors such as corneal shape, axial length, and astigmatism are considered alongside visual priorities like reading, driving, or computer use. This personalised evaluation helps determine the lens that will provide the best visual outcome.
2. What types of intraocular lenses are available for lens replacement surgery?
Several types of intraocular lenses are available, including monofocal, multifocal, extended depth-of-focus (EDOF), and toric lenses. Each type is designed to address different visual needs, such as clear distance vision, multiple focal ranges, or correction of astigmatism. The surgeon recommends the most appropriate option based on eye measurements and lifestyle requirements.
3. What is the difference between monofocal and multifocal lenses?
Monofocal lenses focus at a single distance, typically providing clear distance vision while requiring reading glasses for close tasks. Multifocal lenses create multiple focal points, allowing patients to see at both near and far distances. However, multifocal lenses may sometimes cause visual effects such as halos or glare around lights.
4. When are toric lenses recommended?
Toric lenses are recommended for patients with astigmatism, a condition caused by irregular corneal curvature. These specialised lenses are designed to correct the uneven shape of the cornea and improve visual clarity. Accurate measurements are required to ensure the lens is positioned correctly during surgery.
5. What are extended depth-of-focus (EDOF) lenses?
Extended depth-of-focus lenses provide a continuous range of vision, particularly between distance and intermediate ranges. They are often beneficial for people who spend a lot of time using computers or performing tasks at arm’s length. Compared with multifocal lenses, EDOF lenses may produce fewer night-time visual disturbances.
6. How do lifestyle factors influence lens selection?
Lifestyle plays an important role in determining the most suitable lens. For example, people who frequently drive at night may prefer lenses that minimise glare, while those who spend time reading or using digital devices may benefit from lenses that support near or intermediate vision. Surgeons consider daily activities when recommending a lens.
7. Do eye measurements affect which lens can be used?
Yes, detailed eye measurements are essential for selecting the correct intraocular lens. Tests such as biometry measure the length of the eye and corneal curvature, helping surgeons calculate the precise lens power required. These measurements ensure the artificial lens focuses light correctly after surgery.
8. Can existing eye conditions affect lens choice?
Yes, conditions such as glaucoma, retinal disease, or severe dry eye may influence which lens is recommended. In some cases, surgeons prefer monofocal lenses because they provide stable vision with fewer optical side effects. The overall health of the eye is carefully evaluated before making a final decision.
9. Will I still need glasses after lens replacement surgery?
Some patients may still need glasses after surgery, depending on the type of lens chosen and their visual needs. Monofocal lenses often require reading glasses for near tasks, while multifocal or EDOF lenses may reduce dependence on glasses. Your surgeon will explain what level of spectacle independence you can realistically expect.
10. Why is patient consultation important when choosing a lens?
Consultation allows the surgeon and patient to discuss visual goals, lifestyle habits, and expectations for surgery. This shared decision-making process helps ensure the selected lens aligns with both medical considerations and personal preferences. Clear communication also helps patients understand the benefits and limitations of each lens option.
Final Thoughts: Choosing the Most Suitable Lens for Your Vision
Selecting the right intraocular lens is a key part of achieving the best possible outcome from lens replacement surgery. Surgeons carefully evaluate detailed eye measurements, overall eye health, and individual visual priorities before recommending a lens. By considering factors such as prescription, corneal shape, astigmatism, and daily lifestyle needs, the lens choice can be tailored to provide clear, comfortable vision that supports everyday activities.
A personalised approach ensures that the chosen lens aligns with both medical findings and the patient’s expectations for vision after surgery. Through detailed consultation and careful planning, surgeons can help patients understand their options and make informed decisions about their treatment. If you’re looking for lens surgery in London, you can get in touch with us at London Cataract Centre.
References:
- Chen, J.L., Al‑Mohtaseb, Z.N. and Chen, A.J. (2024) Criteria for premium intraocular lens patient selection, Current Opinion in Ophthalmology. https://pubmed.ncbi.nlm.nih.gov/38920096/
- Zvorničanin, J. and Zvorničanin, E. (2018) Premium intraocular lenses: The past, present, and future, PMC Article. https://pmc.ncbi.nlm.nih.gov/articles/PMC6276729/
- Rao, S.K., Safran, S.G., Chang, D.F. and et al. (2025) International consensuses and guidelines on multifocal intraocular lenses, Asia‑Pacific Journal of Ophthalmology. https://www.sciencedirect.com/science/article/pii/S2162098925001410
- Salvá, L., García, S., García‑Delpech, S., Martínez‑Espert, A. and Ferrando, V. (2023) Optical performance of a segmented extended‑depth‑of‑focus intraocular lens under the influence of different values of spherical aberration generated by refractive surgery, Journal of Clinical Medicine https://www.mdpi.com/2077-0383/12/14/4758
- Badawy, M.M. (2024) Comparison between intraocular lenses TECNIS Eyhance IOL and AcrySof in cataract surgery outcomes, QJM: An International Journal of Medicine. https://academic.oup.com/qjmed/article/117/Supplement_2/hcae175.631/7904120