If you’re living with sickle cell disease and thinking about improving your vision, it’s completely natural to have questions. You may be wondering whether refractive lens exchange (RLE) is safe for you or if your condition increases the risks. It’s also common to feel unsure about how your health might affect the procedure. Having clear information can help you feel more confident about your options.
You might also be concerned about how sickle cell disease could affect your eyes and circulation during surgery. These concerns are valid, as the condition can influence blood flow and healing. It’s important to understand how these factors are taken into account when planning treatment. This helps ensure that your care is both safe and effective.
I want to reassure you that having sickle cell disease does not automatically rule out RLE surgery. What matters most is how well your condition is managed and your overall health. Your medical team will take a careful and personalised approach when assessing your suitability. This ensures that any potential risks are properly managed.
In this guide, you’ll learn everything you need to know before making a decision. It will explain how sickle cell disease can influence surgical planning and what risks need to be considered. You’ll also understand how ophthalmologists assess whether RLE is appropriate for you. By the end, you should feel better informed and more prepared to move forward.
What Is RLE Surgery?
Before looking at how sickle cell disease may affect your options, it’s helpful to understand what RLE surgery involves. This gives you a clearer idea of what to expect and how the procedure works. It also makes it easier for you to have informed discussions with your specialist. Having this foundation is important before considering any medical factors.
Refractive lens exchange is a procedure where your eye’s natural lens is removed and replaced with an artificial intraocular lens. It is very similar to cataract surgery in how it is performed. However, instead of treating a cloudy lens, it is carried out to correct refractive errors such as short-sightedness or long-sightedness. This means the focus is on improving your overall vision.
The aim of RLE is to reduce or even remove your reliance on glasses or contact lenses. It is particularly beneficial if you are over 40 or if laser eye surgery is not suitable for your eyes. Many people choose it for its long-term convenience and effectiveness. If you would like to explore further, you can learn more about RLE surgery in London.
Understanding Sickle Cell Disease
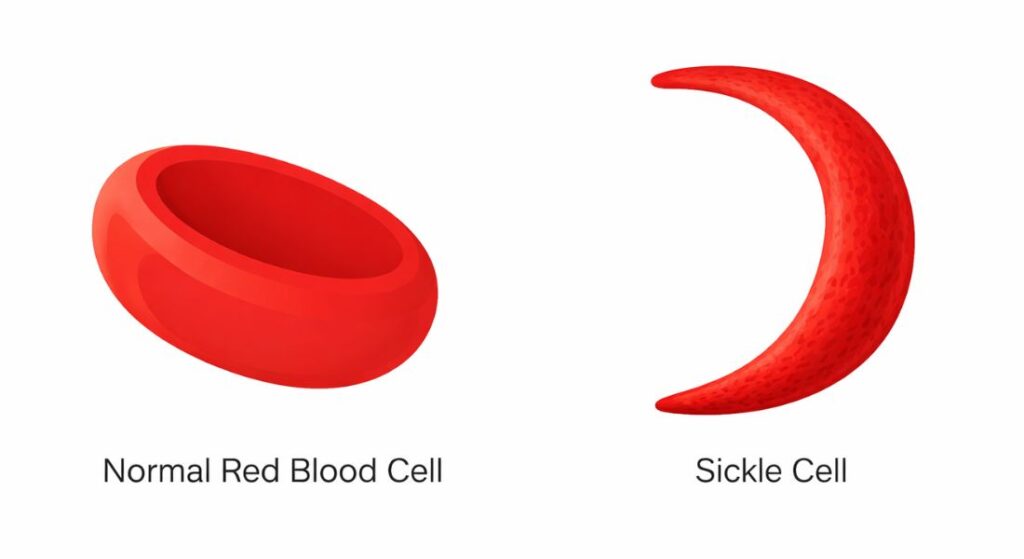
Sickle cell disease is a genetic blood disorder that affects the way your red blood cells behave. Instead of being round and flexible, the cells can become rigid and sickle-shaped. This change makes it harder for them to move smoothly through your blood vessels. As a result, it can affect how oxygen is delivered throughout your body.
Because these cells do not flow easily, they can sometimes block small blood vessels. This can reduce blood supply to certain areas and lead to complications over time. The effects can vary from person to person, depending on how severe the condition is. This is why careful monitoring and management are so important.
From an eye health perspective, this condition is particularly relevant because your retina depends on a healthy blood supply. Any disruption to circulation can affect how well your eyes function. It can also influence how your eyes respond to surgery and healing. This is why your eye specialist will consider your condition carefully when planning treatment.
How Sickle Cell Disease Affects the Eyes
Sickle cell disease can have a significant impact on eye health, particularly the retina, which relies on a steady supply of oxygen-rich blood. Changes in blood flow caused by the condition may lead to complications that affect vision over time. One of the main concerns is the development of sickle cell retinopathy, a condition that can progress if not properly monitored. Understanding these risks is essential when considering any form of eye surgery, including refractive lens exchange (RLE).
- Blocked Blood Vessels in the Retina: Reduced blood flow can cause small vessels in the retina to become blocked. This limits oxygen supply to retinal tissue, potentially leading to damage over time. Early detection is important to prevent progression and preserve vision.
- Abnormal Blood Vessel Growth: In response to poor circulation, the eye may form new, abnormal blood vessels. These vessels are often fragile and prone to complications. Their presence can increase the risk of further retinal issues if left untreated.
- Bleeding Within the Eye: Fragile blood vessels may rupture, causing bleeding inside the eye. This can lead to sudden changes in vision and may require prompt medical attention. Managing these risks is essential before considering any surgical procedure.
- Areas of Retinal Damage: Ongoing disruption to blood supply can result in permanent areas of retinal damage. This may affect visual clarity and, in severe cases, lead to vision loss. Careful monitoring helps identify and address these changes early.
In conclusion, while not everyone with sickle cell disease develops eye complications, the potential risks must be carefully evaluated. Conditions such as sickle cell retinopathy highlight the importance of thorough retinal assessment before surgery. A detailed examination allows your ophthalmologist to identify any underlying issues and plan appropriate care. This cautious approach helps ensure that any treatment decisions prioritise both safety and long-term visual health.
Does Sickle Cell Disease Affect Your Eligibility for RLE?
The answer is not a simple yes or no. It’s understandable to worry about how your condition might affect your options. Many factors need to be considered to determine whether RLE surgery is safe for you. This ensures your care is tailored to your individual needs.
Sickle cell disease does not automatically prevent you from having RLE surgery. Your suitability depends on factors such as the severity of your condition, whether you have any eye complications, and your overall health and stability. If your eyes are healthy and your condition is well managed, you may still be a suitable candidate. Careful assessment is key to making this determination.
However, if there are signs of retinal disease or other complications, your surgeon may recommend addressing those issues first. In some cases, alternative vision correction options may be suggested. This approach ensures that surgery is as safe and effective as possible for your eyes and overall health.
Circulation and Oxygen Levels: Why They Matter
One of the most important considerations for people with sickle cell disease is circulation. Your red blood cells may have difficulty moving smoothly through small vessels, which makes maintaining proper blood flow essential. During surgery, keeping oxygen levels stable and circulation adequate is critical. Poor circulation can increase the risk of complications, especially in delicate areas like the eyes.
Your surgical team will take careful steps to support your circulation and overall stability. This includes ensuring you are well-hydrated, monitoring oxygen levels closely, and minimising stress on your body. These measures are designed to protect your health during the procedure.
By taking these precautions, the risk of sickling episodes during or after surgery is significantly reduced. This careful planning helps make the procedure safer and supports smoother healing. Your medical team will personalise these strategies to suit your specific needs.
Anaesthesia Considerations
Refractive lens exchange (RLE) surgery is usually performed under local anaesthesia, often combined with mild sedation to keep you comfortable. For patients with sickle cell disease, anaesthesia requires special attention, as certain triggers can provoke sickling episodes. Factors like dehydration, low oxygen levels, or stress can increase these risks during surgery. By carefully managing these elements, your medical team can help ensure a safe and smooth procedure.
- Ensuring Proper Hydration: Maintaining adequate hydration is crucial for patients with sickle cell disease, as dehydration can increase the likelihood of red blood cells sickling. Your medical team will make sure you are well-hydrated before and during the procedure. This simple step helps reduce complications and supports safer anaesthesia.
- Monitoring Oxygen Levels: Oxygen levels are closely monitored throughout the surgery to prevent hypoxia, which can trigger sickling episodes. Continuous monitoring allows the team to respond immediately if oxygen levels drop. This proactive approach helps protect both the eyes and overall health during the procedure.
- Keeping the Procedure Smooth and Efficient: Minimising stress and ensuring the surgery is efficient are key priorities. A calm, controlled environment reduces physiological stress that could contribute to sickling. Efficient surgical techniques also shorten exposure to anaesthesia, further lowering risk.
- Individualised Anaesthesia Planning: Anaesthesia is tailored to your specific needs, taking into account your medical history and current health status. This personalised approach ensures that all potential triggers are addressed proactively. Close coordination between your ophthalmologist and anaesthetist maximises safety throughout the procedure.
In conclusion, anaesthesia for patients with sickle cell disease requires careful planning and monitoring. By focusing on hydration, oxygen levels, and a controlled surgical environment, the medical team minimises risks associated with sickling episodes. This thoughtful approach ensures that RLE surgery can be performed safely and comfortably. Proper preparation and vigilance are key to achieving the best possible outcome.
Retinal Risks and Surgical Planning
The retina is one of the most sensitive areas when it comes to sickle cell disease. Reduced blood flow can increase the risk of retinal complications, which makes careful assessment essential. This is why your ophthalmologist will take extra care when evaluating your eyes before surgery. Understanding the condition of your retina is a key part of planning a safe procedure.
Your ophthalmologist will perform a thorough retinal examination before recommending RLE. If any abnormalities are detected, they may need to be treated or stabilised before surgery. Addressing these issues first helps reduce the risk of complications and supports better long-term outcomes.
In some cases, you may be referred to a retinal specialist for further evaluation or treatment. This ensures that all aspects of your eye health are carefully managed. By taking these steps, your surgical team can plan a safer and more effective procedure tailored to your needs.
Infection and Healing
Another concern many patients have is whether sickle cell disease affects healing after surgery. While the condition mainly affects red blood cells, it can also influence how your body responds to stress and recovers. Understanding this helps you appreciate why careful planning and monitoring are important.
If your condition is stable and well-managed, healing is usually straightforward and comparable to patients without sickle cell disease. However, if complications are present, recovery may take longer or require closer supervision. Your medical team will monitor your progress to ensure any issues are addressed promptly.
I always emphasise the importance of following post-operative instructions carefully. This includes using prescribed medications, attending follow-up appointments, and taking steps to protect your eyes. Adhering to these guidelines plays a big role in supporting a smooth and successful recovery.
Pre-Surgical Assessment: What to Expect

If you have sickle cell disease, your pre-surgical assessment will be particularly thorough. This ensures that all aspects of your health are carefully reviewed before proceeding with RLE surgery. A detailed assessment helps your medical team plan the procedure safely and effectively. It also gives you reassurance that every factor is being considered.
Your assessment may include a comprehensive eye examination and retinal imaging to check for any complications. Your surgeon will also review your medical history and coordinate with your haematologist or GP. This collaboration ensures that your overall health is stable and optimised for surgery.
In my experience, this level of preparation is very reassuring for patients. It allows your care team to tailor the procedure specifically to your needs. By addressing potential risks in advance, the team can support a safer and smoother recovery.
When RLE Might Not Be Recommended
While refractive lens exchange (RLE) can be highly effective, it is not suitable for every patient at all times. Certain health conditions or complications may make surgery riskier, and proceeding without addressing these issues could compromise both safety and outcomes. Ophthalmologists carefully weigh these factors to determine the most appropriate timing or alternative options. The focus is always on protecting your health and ensuring the best possible visual results.
- Active Sickle Cell Complications: If you are experiencing an active sickle cell episode, surgery may be postponed. Active complications increase the risk of sickling during or after the procedure, which could lead to serious health issues. Waiting until your condition is stable helps reduce these risks and ensures safer surgery.
- Significant Retinal Disease: Advanced retinal problems, such as sickle cell retinopathy or other structural damage, may make RLE less safe or effective. Retinal stability is essential for good surgical outcomes, so any significant disease must be addressed first. Surgeons may recommend alternative treatments or delay surgery until the retina is optimally managed.
- Poor Overall Health or Instability: If your general health is unstable or there are uncontrolled medical issues, RLE may not be advisable. Surgery in these circumstances could increase complications and hinder recovery. Optimising overall health before proceeding ensures the safest and most successful outcome.
- Exploring Alternatives and Timing: When RLE is not recommended, your surgeon may suggest alternative vision correction methods or schedule surgery for a later date. This decision is made to prioritise safety without compromising long-term vision goals. Personalised guidance ensures that your eye care remains effective even if surgery is temporarily delayed.
In conclusion, RLE is not always the immediate solution for everyone, particularly for those with active sickle cell complications or significant retinal issues. Delaying surgery or considering alternatives is a proactive step to protect your health and optimise outcomes. By working closely with your ophthalmologist, you can make informed decisions that balance safety with your vision goals. Careful planning ensures that when surgery does proceed, it is performed under the safest possible conditions.
How Surgeons Minimise Risk
Modern eye surgery is highly advanced, and patient safety is always the top priority. Surgeons follow strict protocols to reduce risks and ensure the best possible outcomes. This careful approach is particularly important for patients with conditions like sickle cell disease, where circulation and oxygen levels need special attention.
To minimise risks, your surgical team will maintain a controlled and sterile environment throughout the procedure. They will monitor your oxygen levels and hydration closely to support healthy circulation. Gentle surgical techniques are used to reduce stress on your eyes, and post-operative care is tailored to your individual needs.
These precautions help manage the specific challenges associated with sickle cell disease. By taking these steps, your medical team can significantly reduce the risk of complications. This careful planning supports a safer procedure and a smoother recovery.
Alternatives to RLE Surgery
If RLE is not suitable for you at the moment, it’s important to know that there are other options available. You don’t have to feel limited, as several effective alternatives can help improve your vision. Understanding these choices allows you to make informed decisions about your eye care.
Common alternatives include glasses or contact lenses, which provide reliable vision correction without surgery. In some cases, other types of refractive procedures may be considered, depending on your eye health and overall suitability. Each option has its own benefits and considerations.
Your ophthalmologist will guide you through these choices based on your individual situation. They will assess your eyes, health, and lifestyle to recommend the safest and most effective solution. This personalised approach ensures you still have ways to achieve clear vision even if RLE isn’t the immediate option.
Long-Term Outlook
For patients with well-managed sickle cell disease and healthy eyes, the long-term outlook after RLE surgery is generally very positive. Many people achieve excellent vision and notice significant improvements in their daily life. This can make a real difference in independence and quality of life.
Visual outcomes are often comparable to those in individuals without the condition. Patients frequently experience reduced reliance on glasses or contact lenses. The key to success lies in thorough pre-surgical assessment and careful planning.
When the right precautions are taken, the benefits of surgery can be significant. Close monitoring, tailored care, and attention to circulation and retinal health all contribute to safe and effective results. With proper management, RLE can be a highly rewarding option for vision correction.
Emotional Considerations
Living with a chronic condition can make decisions about surgery feel more complex and overwhelming. You might feel anxious about potential risks or uncertain about whether you are a suitable candidate. These feelings are completely normal and understandable. Acknowledging them is an important step in making an informed decision.
I want to reassure you that your concerns are valid, but modern medicine has made it possible for many people with sickle cell disease to safely undergo procedures like RLE. Advances in surgical techniques and personalised care mean that risks can be carefully managed. This progress allows patients to achieve positive outcomes even with underlying health conditions.
Open communication with your care team can make a big difference in how confident you feel about moving forward. Sharing your questions and worries allows your surgeon to provide guidance tailored to your needs. Feeling supported and informed can help reduce anxiety and improve your overall experience.
FAQs:
1. Can I have RLE surgery if I have sickle cell disease?
Yes, many patients with well-managed sickle cell disease can safely undergo RLE. Your suitability depends on your overall health, circulation, and eye condition.
2. Does sickle cell disease automatically prevent me from having RLE?
No, having sickle cell disease does not automatically disqualify you. Your ophthalmologist will assess your retinal health, oxygen levels, and general stability before confirming eligibility.
3. How does sickle cell disease affect the eyes?
Sickle cell disease can impact retinal circulation, sometimes causing blocked vessels, abnormal blood vessel growth, bleeding, or areas of retinal damage. Careful monitoring helps manage these risks before surgery.
4. Why is circulation important during RLE surgery?
Proper circulation ensures oxygen-rich blood reaches your eyes. Poor blood flow can increase the risk of complications, so your surgical team takes precautions to maintain stable circulation during the procedure.
5. Are there special anaesthesia considerations for patients with sickle cell disease?
Yes. Anaesthesia is carefully managed to avoid triggers that can cause sickling, including dehydration, low oxygen levels, and stress. This ensures a safer and smoother procedure.
6. Does sickle cell disease affect healing after RLE surgery?
If your condition is stable, healing is usually comparable to patients without sickle cell disease. Close post-operative monitoring helps detect and address any issues early.
7. What tests are done before surgery for patients with sickle cell disease?
Pre-surgical assessment may include retinal imaging, eye exams, and coordination with your haematologist. These tests ensure your eyes and overall health are stable for surgery.
8. When might RLE surgery be delayed for sickle cell patients?
Surgery may be postponed if there are active sickle cell episodes, significant retinal disease, or instability in general health. Delaying ensures safety and better long-term outcomes.
9. Are there alternatives if RLE is not suitable?
Yes. Glasses, contact lenses, or other refractive procedures can provide clear vision until surgery becomes safer. Your ophthalmologist will help you choose the most appropriate option.
10. What is the long-term outlook for RLE in patients with sickle cell disease?
For those with well-managed disease and healthy eyes, long-term visual outcomes are typically excellent, with reduced reliance on glasses or contacts and stable, improved vision.
Final Thoughts: Navigating RLE Surgery with Confidence
Deciding on refractive lens exchange when you have sickle cell disease may feel daunting, but the key is understanding how your condition affects circulation, retinal health, and overall stability. With careful assessment, thorough pre-surgical planning, and personalised care, many patients with well-managed sickle cell disease safely undergo RLE and achieve excellent visual outcomes. Close coordination between your ophthalmologist, haematologist, and surgical team ensures that any potential risks are minimised and recovery is supported.
It’s important to stay informed, communicate openly with your care team, and follow all pre- and post-operative instructions. With proper management and precautions, you can achieve significant improvements in vision and quality of life. If you’re considering RLE surgery in London, you can get in touch with us at London Cataract Centre.
References:
- Hancox, J., Spalton, D. and Boyce, J. (2024) A survey of intraocular lens preferences of UK refractive surgeons, BMC Ophthalmology. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11378387
- Wallerstein, A., Gauvin, M., Trottier, P., Cohen, M., Lloyd, J., Racine, L., Albert, D., Ahmed, I.I.K. and Mimouni, M. (2023) Toric trifocal intraocular lens for refractive lens exchange: A multi-centre study, Journal of Refractive Surgery, 39(5), pp. 302–310. Available at: https://pubmed.ncbi.nlm.nih.gov/37162394/
- Cochener, B., Boutillier, G., Lamard, M. and Auberger-Zagnoli, C. (2018) A comparative evaluation of new-generation intraocular lenses for refractive lens exchange, Journal of Refractive Surgery. Available at: https://pubmed.ncbi.nlm.nih.gov/28396877/
- Zhang, F., Chen, X., Yu, A. and Wang, Q. (2024) Visual performance and patient satisfaction after trifocal intraocular lens implantation in presbyopic patients, Clinical Ophthalmology. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC11264366/
- Pedrotti, E., Carones, F., Aiello, F., Mastropasqua, R., Bruni, E. and Marchini, G. (2023) Visual outcomes and patient satisfaction after bilateral refractive lens exchange with a trifocal intraocular lens , Journal of Clinical Medicine. Available at: https://pubmed.ncbi.nlm.nih.gov/37052874/

