If you are considering refractive lens exchange, one of the most important questions you might not think to ask straight away is this: how will I see at night? Daytime vision improvements often take centre stage clear distance vision, freedom from reading glasses, and reduced dependence on varifocals. But real life does not only happen in bright light. Night driving, headlights, streetlights, and low-light contrast matter just as much.
Refractive lens exchange, also known as refractive lens exchange, involves replacing your natural lens with an artificial intraocular lens. The type of lens you choose plays a major role in how your night vision may feel afterwards. Monofocal lenses typically provide crisp distance clarity with minimal visual disturbances, while multifocal or extended depth-of-focus lenses can sometimes introduce halos or glare around lights at night.
It is important to understand that these visual phenomena are not complications in the traditional sense they are optical side effects of how certain premium lenses split or extend light to provide range of focus. Many patients adapt very well over time, as the brain learns to filter out unwanted visual signals. However, some people remain more aware of night-time glare, particularly in the early months after surgery.
Having a clear, honest discussion with your surgeon about your lifestyle especially if you drive frequently at night is crucial. When expectations are realistic and lens choice is aligned with your visual priorities, satisfaction rates are very high. Understanding potential night vision changes before surgery is one of the most powerful ways to ensure you feel confident and happy with your outcome afterwards.
What Is RLE and Why Night Vision Matters
Refractive lens exchange (RLE) is essentially the same procedure as cataract surgery, but performed before a cataract has significantly developed. Your natural lens is removed and replaced with an artificial intraocular lens (IOL) to correct refractive error and reduce dependence on glasses. It is a permanent change designed to provide long-term visual clarity.
The implanted lens does not age or become cloudy like a natural lens. However, unlike your natural lens, it does not adapt or change shape to adjust focus dynamically. Your youthful lens once had the ability to subtly shift and respond to lighting conditions. An artificial lens, by contrast, has a fixed optical design.
This is where night vision differences can arise. The way the IOL handles light particularly in low-light environments where your pupils are larger can influence glare, halos, and contrast sensitivity. If you are considering RLE surgery in London, the type of lens you choose will directly affect how you experience headlights, streetlights, and contrast after dark. Understanding this before surgery is key to long-term satisfaction.
First, Let’s Talk About Normal Night Vision
Before surgery, your natural lens plays a subtle but complex role in how light enters your eye. When it is healthy and clear, light passes through a single optical system and focuses smoothly onto the retina. In low-light conditions, your pupils enlarge to let in more light, and a clear lens helps maintain contrast and minimise distortion.
As we age, however, the natural lens gradually changes. Even before a cataract becomes obvious, microscopic lens changes can scatter incoming light. This scattering is what causes glare from headlights, halos around streetlights, and starburst patterns at night. Many patients already experience mild night-time visual disturbances without realising that early lens ageing is the cause.
This is why the effect of refractive lens exchange on night vision can vary. In some cases, replacing an ageing lens with a clear intraocular lens actually improves night clarity and reduces glare. In other situations particularly depending on the type of lens chosen new optical phenomena may be noticed. The outcome depends largely on lens design and how it distributes light in dim conditions.
The Role of the Pupil in the Dark
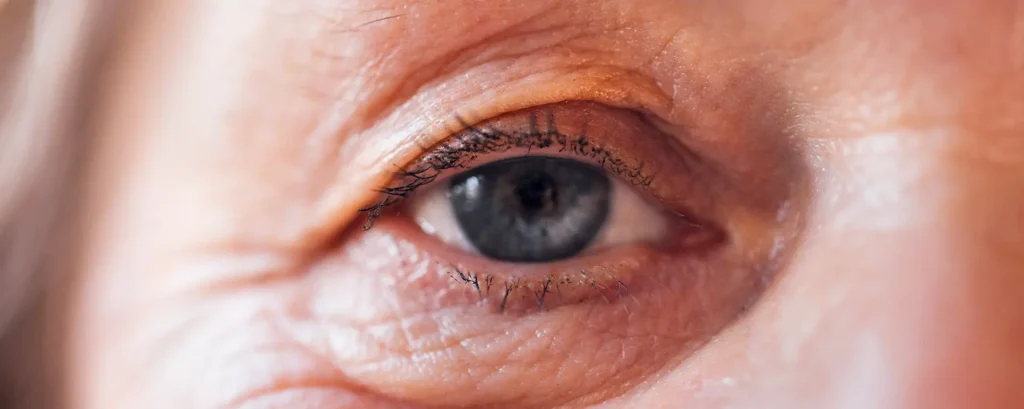
Vision can change noticeably in low-light environments, particularly after lens replacement surgery. At night, the pupil naturally dilates to allow more light into the eye. While this helps improve visibility in dim conditions, it also exposes a larger portion of the eye’s optical system. As a result, subtle optical characteristics of an intraocular lens may become more apparent.
- Pupil Dilation at Night: In darker settings, the pupil widens to maximise light entry. This physiological response improves night vision but changes how light interacts with the implanted lens. The larger aperture can influence visual perception.
- Exposure of the Optical System: When the pupil expands, more peripheral areas of the IOL are used for focusing light. Any minor imperfections, edge reflections, or lens design features may therefore become more noticeable. These effects are often minimal in daylight but clearer in dim lighting.
- Why Night Symptoms Are Discussed Separately: Visual quality in bright light does not always predict night-time performance. Symptoms such as glare, halos, or starbursts are more likely to appear when the pupil is dilated. For this reason, surgeons specifically address night vision expectations during consultations.
Understanding the role of the pupil in low-light conditions helps explain why some visual phenomena are more noticeable at night. These effects relate to normal optical principles rather than surgical failure. By discussing night-time expectations separately from general vision quality, patients can make informed and confident decisions about their lens choice.
Monofocal Lenses and Night Vision
If you choose a monofocal IOL, the lens is designed with a single focal point, usually set for clear distance vision. Optically, this is the simplest intraocular lens design. Light passes through one primary optical zone and focuses as a single image on the retina, without being split into multiple focal points.
Because there are no concentric rings, diffractive steps, or light-splitting elements, monofocal lenses tend to produce the lowest levels of glare and halos. For patients who drive frequently at night or are particularly sensitive to visual disturbances, this makes monofocal lenses the most predictable option in low-light conditions. Contrast sensitivity is generally strong, and headlights typically appear crisp rather than surrounded by rings.
The trade-off is range of focus. Since the lens is optimised for one distance, you will likely still need glasses for near tasks such as reading, phone use, or detailed work. For many people, however, the clarity and stability of night vision outweigh the need for reading glasses, making monofocal lenses a very reassuring choice.
Multifocal Lenses: Splitting Light for Multiple Distances
Multifocal intraocular lenses are designed to provide both distance and near vision by allowing you to focus at more than one range without glasses. They achieve this by splitting incoming light into multiple focal points, so that different portions of light are directed toward distance and near focus simultaneously. From an engineering perspective, it is an elegant and highly sophisticated solution.
However, there is a trade-off. Because the lens divides light into separate focal zones, the total light energy is redistributed rather than concentrated into a single point of focus. In bright daylight, this usually works extremely well and many patients enjoy a high level of spectacle independence.
In lower lighting conditions particularly at night when pupils enlarge this light-splitting design can sometimes create visual phenomena such as halos around headlights or glare from streetlights. These effects are not harmful, but they can be noticeable. Many patients adapt over time, yet it is important to understand this possibility before choosing a multifocal lens.
What Do Halos Actually Look Like?
Patients often describe halos as circular rings of light surrounding headlights, street lamps, or other bright point sources at night. They are usually symmetrical and consistent, appearing in both eyes in the same way. Some people notice a soft glow, while others see more defined rings radiating outward from the light.
For many individuals, halos are mild and most noticeable in very dark environments where contrast is high, such as night driving. Over time, the brain often adapts to these visual effects, making them less intrusive. This process of adaptation varies from person to person.
It is important to understand that halos are not harmful. They are optical phenomena created by the way certain intraocular lens designs distribute light, rather than a sign of damage or a complication with the surgery.
Glare and Starbursts
Visual phenomena such as glare and starbursts are sometimes discussed when considering multifocal intraocular lenses. These effects are related to how light interacts with the lens design, particularly in bright or low-light environments. While they can be noticeable in the early postoperative period, they are often temporary. Understanding why they occur helps set realistic and reassuring expectations.
- What Is Glare: Glare refers to increased sensitivity to bright light, such as oncoming headlights or strong sunlight. It may cause discomfort or a temporary reduction in contrast clarity. This is more noticeable when the visual system is still adapting after surgery.
- What Are Starbursts: Starbursts appear as radiating spikes or streaks extending from light sources, especially at night. They occur because multifocal lenses split light into different focal points. In the early months, the brain is still learning how to interpret these new light patterns.
- The Role of Neuroadaptation: The brain is remarkably adaptable, a process known as neuroadaptation. Over time, it learns to filter out unwanted visual artefacts and prioritise clear images. Most patients find that glare and starbursts become significantly less noticeable as this adaptation progresses.
Although glare and starbursts can initially feel concerning, they are a recognised part of the adjustment process with certain premium lenses. In most cases, symptoms improve as the brain adapts to the new optical system. Open discussion before surgery ensures you understand both the benefits and potential temporary effects, allowing you to make a confident and informed decision.
EDOF Lenses: A Middle Ground
Extended depth-of-focus (EDOF) lenses are designed to provide a continuous range of vision rather than distinct, separate focal points. Instead of sharply splitting light into distance and near zones, they stretch and elongate the focus to create a smoother transition between ranges. This approach allows many patients to see clearly at distance and intermediate without relying heavily on reading glasses.
Because of this optical design, EDOF lenses generally produce fewer halos than traditional multifocal lenses. Light is not divided into multiple strong focal points, which reduces the intensity of ring-like visual phenomena. However, some patients may still notice mild glare or subtle halos, particularly in very low-light conditions.
Night vision with EDOF lenses is often described as a middle ground. It is typically better than with traditional multifocals in terms of glare and halo intensity, but it may still feel slightly different compared to the crisp, single-focus clarity of a monofocal lens.
Why Does Light Splitting Cause Halos?
Let’s simplify this. When light enters a multifocal intraocular lens, part of it is directed toward distance focus and part toward near focus at the same time. The brain selects the image it needs, but the unused light does not simply disappear it is still present within the optical system.
At night, the pupil naturally becomes larger to allow more light in. In lower contrast conditions, more of the lens surface and its different focal zones are engaged simultaneously. This makes the interaction between the focal points more noticeable.
That overlap of light from different focal zones is what the brain interprets as rings, halos, or glare around bright sources. It is not a surgical error or a complication it is a predictable optical effect based on physics and lens design.
Contrast Sensitivity at Night
Another important factor to understand is contrast sensitivity. This refers to your ability to detect subtle differences between shades of grey, particularly in low-light environments. It plays a major role in how clearly you see at dusk, in fog, or when driving at night.
Multifocal lenses can slightly reduce contrast sensitivity compared to monofocal lenses because light is divided between multiple focal points rather than concentrated into one. In bright daylight conditions, this difference is rarely noticeable and most patients function completely normally.
In dim lighting, however, this small reduction in contrast can make objects appear slightly less sharp or defined. Road markings, pedestrians in dark clothing, or uneven surfaces may feel a little less crisp. For most people this effect is subtle, but it is an important part of setting realistic expectations before surgery.
Night Driving: What Should You Realistically Expect?
If night driving is an important part of your lifestyle for example, long-distance commutes or rural driving it is essential to discuss this with your surgeon before choosing a lens. Your lens choice can influence how you experience glare, halos, and contrast in low-light conditions.
With monofocal lenses, most patients report excellent clarity and minimal visual disturbances at night. EDOF lenses usually provide very good night vision as well, though mild halos or glare may occasionally be noticed. Multifocal lenses tend to produce more pronounced halos, but for many patients these are manageable once the brain adapts.
It is important to know that the majority of patients adapt well over time, experiencing minimal disruption in everyday night driving. A small minority, however, may continue to notice halos or glare more prominently, so setting realistic expectations is key to satisfaction after surgery.
How Common Are Halos After RLE?
Studies indicate that a noticeable number of patients with multifocal lenses experience halos in the first few months after surgery. These optical phenomena are most evident in low-light conditions, such as night driving or dimly lit rooms.
However, the proportion of patients who find halos truly bothersome over the long term is much smaller. Most people adapt as the brain gradually learns to filter out the unwanted light patterns, a process called neuroadaptation.
Managing expectations is key. If you are informed beforehand that halos are possible and understand why they occur, you are far more likely to accept them without concern. It is the element of surprise not the halos themselves that most often leads to dissatisfaction.
Do Halos Ever Go Away Completely?
For some patients, halos may disappear entirely over time, especially as the brain adapts to the new visual input. For others, the rings may never vanish completely but often fade into the background and become less noticeable.
This improvement happens through a process called neuroadaptation, where your visual cortex learns to prioritise important visual information and ignore repetitive or less relevant light patterns.
The timeline for this adjustment varies. For many, noticeable improvement occurs within weeks to a few months after surgery. Patience and realistic expectations are key to feeling comfortable with any lingering visual phenomena.
Are Certain People More Sensitive?
Yes, some individuals are more likely to notice night-time visual phenomena such as halos and glare. People who are highly detail-oriented or particularly sensitive to subtle visual imperfections may perceive these effects more readily than others.
Pupil size also plays a role. In low-light conditions, larger pupils allow more light to enter the eye, which can make halos more noticeable. Patients with naturally larger dark-adapted pupils may therefore experience these optical effects more prominently.
During preoperative assessment, your surgeon may measure pupil size and discuss how it could influence your lens choice. This information helps guide recommendations, aiming to balance visual range with comfort in night conditions.
Does RLE Improve Night Vision in Some Cases?
Refractive lens exchange (RLE) can sometimes enhance night vision, particularly in patients whose natural lens is developing early opacities. These subtle changes in the lens can scatter light, reducing clarity and creating glare or halos even before cataracts are fully formed. Replacing the natural lens with a high-quality monofocal IOL can restore sharpness and improve overall visual quality. In these cases, night vision may actually be better than it was pre-surgery.
- Impact of Early Lens Opacities: Even minor lens changes can scatter incoming light, affecting night-time clarity. Patients may notice glare, halos, or general haziness that reduces contrast sensitivity. Removing the lens addresses these subtle optical imperfections.
- Monofocal Lenses and Night Vision: Implanting a monofocal lens during RLE can deliver sharper, more consistent light focus across the retina. Many patients report improved clarity and reduced night-time visual disturbances compared to their preoperative vision.
- Not Always a Trade-Off: While premium lenses sometimes carry a risk of night-time phenomena, RLE with a monofocal lens can be an optical upgrade. Patients may gain improved overall vision, including night-time performance, rather than simply exchanging one limitation for another.
For individuals experiencing early lens-related vision issues, RLE can be more than corrective it can be transformative. Understanding how the procedure affects both day and night vision helps patients make an informed choice about their lens options and expected outcomes.
The Importance of Individualised Lens Choice
Choosing a lens is not about finding the “best” option in general; it’s about finding the best lens for your needs and lifestyle. Each lens type has its advantages and trade-offs, and your personal priorities should guide the decision.
Your tolerance for optical phenomena like halos or mild glare is important to consider. If being completely glasses-free is a top priority, you may be willing to accept some halos with a multifocal or EDOF lens. Conversely, if night driving or low-light vision is critical, a monofocal lens might be the safer choice.
Ultimately, there is no universal answer. A careful discussion with your surgeon about your lifestyle, visual goals, and expectations ensures the lens selected aligns with what matters most to you.
Can Halos Be Corrected After Surgery?
In rare cases where halos are persistent and significantly bothersome, lens exchange is an option. This involves replacing the original intraocular lens with a different type, but such procedures are uncommon and usually reserved for extreme cases.
Most patients adapt successfully over time through neuroadaptation, with halos becoming much less noticeable or fading into the background. The brain learns to prioritise relevant visual information, making the effect far less intrusive.
In some instances, mild residual refractive errors can amplify glare or halos. Performing a laser enhancement to fine-tune vision can improve visual sharpness and often reduces these symptoms, providing additional comfort for affected patients.
The First Few Months Are Not the Final Result
It’s important to remember that your early night vision after surgery does not represent the final outcome. During the first few weeks, your eyes are still healing and adjusting to the new lens.
Factors such as mild inflammation, fluctuations in the tear film, and ongoing neural adaptation all influence how you perceive light and contrast at night. These temporary changes can make halos or glare seem more noticeable initially.
Vision continues to refine over several weeks, and many visual disturbances gradually diminish as the eye and brain adapt. Patience during this period is key to accurately assessing your long-term night vision.
Honest Conversations Lead to Happy Outcomes

One of the most important predictors of satisfaction after RLE is thorough pre-operative counselling. Taking the time to discuss lens options, potential visual effects, and how each choice aligns with your lifestyle helps set realistic expectations and reduces anxiety about normal post-surgical phenomena.
For example, understanding that multifocal and EDOF lenses work by redistributing light clarifies why halos or mild glare may occur. When patients know the reason behind these effects, they are far less likely to be concerned or distressed by them. This knowledge empowers you to approach the recovery period with confidence rather than worry.
Additionally, honest conversations allow your surgeon to tailor recommendations to your priorities, whether that’s freedom from glasses, optimal night driving, or minimizing visual disturbances. When expectations match reality, satisfaction rates after surgery are extremely high, and most patients feel reassured about their visual outcomes.
Balancing Freedom and Optical Purity
Think of lens choice as a spectrum rather than a single “best” option. At one end, monofocallenses provide optical simplicity with minimal night phenomena, giving predictable clarity for distance vision but usually requiring glasses for near tasks.
At the other end, multifocal lenses offer the greatest freedom from spectacles, allowing both near and distance vision without additional correction. The trade-off is a higher likelihood of halos, glare, or mild reductions in contrast sensitivity, particularly in low-light conditions.
EDOF lenses sit between these extremes, providing a continuous range of vision with fewer optical side effects than multifocals. Your decision is ultimately about finding the right balance between visual freedom and optical purity, not achieving absolute perfection.
The Good News
The good news is that severe or disabling night vision problems after RLE are uncommon. Most patients experience only mild visual phenomena, such as halos or slight glare, particularly with multifocal lenses. These effects are usually manageable and often diminish over time as the brain undergoes neuroadaptation, learning to filter out less relevant visual information.
With appropriate counselling and realistic expectations, the majority of patients adjust successfully and remain highly satisfied with their vision. Even if minor halos persist, they rarely interfere with everyday activities like driving, reading, or using digital devices.
The key takeaway is that choosing knowingly understanding potential optical effects, comparing lens types, and considering your lifestyle priorities greatly increases the likelihood of a positive experience. Being informed helps you approach surgery with confidence, ensuring both peace of mind and long-term satisfaction with your visual outcomes.
FAQs:
1. How does RLE affect night vision?
Refractive lens exchange (RLE) can influence night-time vision because the artificial intraocular lens (IOL) interacts differently with light compared to your natural lens. Effects vary by lens type and pupil size in low-light conditions.
2. Can pupil size predict night vision issues after RLE?
Yes. Larger pupils at night expose more of the lens periphery, making halos, glare, or starbursts more noticeable. Surgeons often measure pupil size to guide lens choice for patients sensitive to night-time disturbances.
3. What causes halos and glare after RLE?
Halos and glare occur when light is split into multiple focal points (as with multifocal lenses) or interacts with the lens edge during pupil dilation at night. They are optical phenomena, not surgical complications.
4. Will halos or glare go away over time?
Most patients experience neuroadaptation, where the brain gradually filters out unwanted light patterns. Halos often diminish within weeks to months, though some may persist in a mild form.
5. Does RLE improve night vision in any cases?
Yes. In patients with early lens opacities, replacing the natural lens with a clear monofocal IOL can reduce glare, improve contrast, and enhance overall night vision compared to pre-surgery.
6. Are some people more sensitive to night-time visual phenomena?
Yes. People with larger pupils in low light or those highly detail-oriented may notice halos or glare more. Preoperative pupil assessment helps predict sensitivity and guide lens choice.
7. How does contrast sensitivity change after RLE?
Multifocal lenses can slightly reduce contrast sensitivity at night due to light splitting. Monofocal and EDOF lenses generally preserve contrast better, providing sharper perception in dim conditions.
8. What are starbursts and how do they differ from halos?
Starbursts appear as radiating spikes extending from light sources, while halos are circular rings. Starbursts are more noticeable at night and are related to multifocal lens design and pupil size.
9. Can halos or glare be corrected after surgery?
In rare, severe cases, lens exchange or laser enhancement can reduce residual visual disturbances. Most patients adapt successfully without additional procedures.
10. Why do multifocal lenses produce more halos than monofocal lenses?
Multifocal lenses split incoming light into different focal points for distance and near vision. At night, the overlap of these light zones becomes visible as halos or rings around bright lights. This is a normal optical effect, not a complication.
Final Thoughts: Choosing the Right Lens for Night Vision
Refractive lens exchange (RLE) can significantly improve your overall vision, but night-time visual experiences like halos, glare, or reduced contrast depend largely on your lens choice and individual eye characteristics. Monofocal lenses offer crisp distance vision with minimal optical disturbances, EDOF lenses provide a continuous range with mild night effects, and multifocal lenses deliver the greatest freedom from glasses but may cause more noticeable halos initially. Most patients adapt over time through neuroadaptation, and severe night vision problems are uncommon when expectations are realistic.
If you’re looking for RLE Surgery in London, you can get in touch with us at London Cataract Centre for personalised advice on lens selection and to discuss how your lifestyle and visual priorities influence your outcomes.
References:
- Ukai, Y. et al. (2021) Quantitative assessment of photic phenomena in the presbyopia‑correcting intraocular lens, https://pmc.ncbi.nlm.nih.gov/articles/PMC8635348/
- Khandelwal, S.S. et al. (2019) Effectiveness of multifocal and monofocal intraocular lenses for cataract surgery and lens replacement https://pubmed.ncbi.nlm.nih.gov/30627791/
- Trusiak, Z.H. et al. (2025) Enhanced Monovision Intraocular Lenses: Current Status and Future Perspectives https://www.mdpi.com/2227-9059/14/1/74
- Winther‑Nielsen, A., Corydon, L. and Olsen, T. (1993) Contrast sensitivity and glare in patients with a diffractive multifocal intraocular lens, Journal of Cataract and Refractive Surgery, https://pubmed.ncbi.nlm.nih.gov/8487170/
- Contrast Sensitivity and Glare Disability in Different IOL Types After Clear‑corneal Cataract Surgery (1998) Journal Français d’Ophtalmologie https://www.sciencedirect.com/science/article/abs/pii/S0181551225000117

