If you’ve been living with glaucoma and are considering refractive lens exchange (RLE) surgery, it’s natural to feel both curious and cautious. You want to improve your vision, but you’re also aware that glaucoma already affects your eyes. Understanding the risks, precautions, and potential benefits is key before making any decisions. I’m here to guide you through this step by step.
RLE, or refractive lens exchange, is similar to cataract surgery but performed before cataracts significantly develop. The procedure involves removing your natural lens and replacing it with an artificial intraocular lens (IOL), which can correct vision issues such as presbyopia or severe long-sightedness. For people with glaucoma, the decision is more nuanced because glaucoma affects the optic nerve and intraocular pressure (IOP), both of which are crucial for eye health.
Before considering RLE, you’ll need a thorough assessment to ensure your eyes can tolerate the surgery safely. Tests will include measuring your IOP, examining the optic nerve, and assessing the overall health of your retina. These steps help your surgeon identify any risks and plan the procedure in a way that protects your vision.
With careful planning, many patients with stable glaucoma can still undergo RLE safely. Lifestyle factors, ongoing monitoring, and adherence to follow-up care are equally important in maintaining long-term eye health. By understanding the process and taking the necessary precautions, you can make an informed decision about whether RLE is the right choice for you.
Understanding Glaucoma and Its Impact on Your Eyes
Glaucoma is often called the “silent thief of sight” because it usually progresses without noticeable symptoms until significant vision loss has occurred. The main issue in most cases is increased intraocular pressure (IOP), which can gradually damage the optic nerve. There are several types of glaucoma, including open-angle glaucoma, angle-closure glaucoma, and normal-tension glaucoma, each affecting your eyes in slightly different ways.
Why does this matter if you’re considering RLE surgery? The success of any eye procedure, including RLE, depends on a stable ocular environment. High IOP can make surgery more challenging and may increase the risk of complications during or after the procedure.
Pre-existing optic nerve damage is another important factor. It can influence how much your vision improves after surgery and how well your eyes tolerate the procedure. I always emphasise to my patients that knowing the health of your optic nerve and monitoring your IOP is essential it’s not optional when deciding whether RLE is right for you.
Why RLE Surgery Can Be Tricky with Glaucoma

When you have glaucoma, your eyes are already under extra strain. The natural lens sits behind your iris and helps regulate fluid flow inside your eye. Removing this lens during RLE surgery can temporarily spike intraocular pressure (IOP), especially in the first 24–48 hours after the procedure.
For patients with well-controlled glaucoma, these pressure changes are usually manageable. However, if your glaucoma is advanced or poorly controlled, there is a higher risk that surgery could worsen optic nerve damage. This doesn’t automatically rule out RLE it simply means extra precautions, careful planning, and close monitoring are essential.
The type of glaucoma you have also matters. Patients with angle-closure glaucoma may benefit from lens removal because it can open the angle and improve fluid drainage, while open-angle glaucoma is less likely to improve. In all cases, the goal is to protect your optic nerve and ensure the surgery does not worsen your existing condition.
Pre-Operative Assessment: What I Look for as Your Surgeon
Before even considering RLE surgery for a glaucoma patient, a thorough pre-operative assessment is essential. Each eye is unique, and glaucoma adds complexity that requires careful evaluation. Understanding the current state of your optic nerve, visual field, and eye pressure helps me make informed decisions about surgical safety. This detailed approach ensures that the procedure is tailored to your individual needs and minimises potential risks.
- Optic Nerve Evaluation: Using advanced imaging tools like optical coherence tomography (OCT), I assess the optic nerve for any existing damage. This evaluation helps predict how your eye might respond to surgery and identifies any vulnerabilities that could affect post-operative outcomes.
- Visual Field Testing: Glaucoma can cause blind spots or peripheral vision loss. Mapping these visual fields allows me to determine whether surgery could worsen vision in sensitive areas and helps set realistic expectations for visual improvement.
- Intraocular Pressure Measurements: Measuring IOP at different times of the day and with multiple techniques provides a complete picture of your eye pressure. Understanding these fluctuations is crucial, as elevated IOP can complicate both the surgery and the healing process.
- Medication Review: Many glaucoma medications influence eye pressure and healing. Reviewing your current prescriptions ensures that I can adjust treatment as needed before, during, and after surgery to reduce risks and support optimal recovery.
- Angle Assessment: Evaluating the drainage angle, especially in narrow-angle glaucoma patients, is vital. A shallow or blocked angle increases the risk of post-operative IOP spikes, so knowing this helps me plan precautions or consider alternative procedures if necessary.
In conclusion, pre-operative assessment for glaucoma patients is a multi-step process designed to protect vision and ensure safety. By evaluating the optic nerve, visual field, IOP, medications, and drainage angles, I can identify potential risk factors and determine whether RLE is a suitable option. This personalised approach maximises the chance of a safe procedure and successful visual outcome.
Potential Risks of RLE in Glaucoma Patients
RLE surgery is generally safe, but having glaucoma adds extra layers of complexity. One of the main concerns is post-operative spikes in intraocular pressure (IOP). While these pressure rises are usually temporary, they can pose a risk to the optic nerve in cases of severe or advanced glaucoma.
Even minor fluctuations in IOP can stress an optic nerve that is already compromised. You may also need adjustments to your glaucoma medications, such as eye drops, before and after surgery. Careful monitoring ensures that your IOP remains controlled throughout the procedure and recovery period.
Other potential risks include slower healing or complications related to the cornea, since glaucoma can sometimes reduce corneal endothelial cell count. Temporary visual fluctuations may also occur as your IOP stabilises, especially if your glaucoma is advanced. Discussing these risks upfront allows your surgeon to create a personalised plan that minimises complications and keeps your eyes safe.
When RLE Might Be Beneficial for Glaucoma
Interestingly, RLE surgery can sometimes provide benefits for certain glaucoma patients. For example, in angle-closure glaucoma, removing the natural lens can deepen the front chamber of your eye, widen the angle, and improve fluid drainage. This can help lower intraocular pressure and protect your optic nerve, which is especially important in preventing further vision loss over time.
In some situations, lens removal may also reduce your dependence on glaucoma medications. Fewer eye drops may be needed to maintain stable IOP, making daily management easier and more convenient. Your ophthalmologist will carefully assess whether this approach is appropriate for you and discuss any potential trade-offs.
RLE can also safely correct refractive errors, particularly if glasses or contact lenses are impractical or uncomfortable. However, it’s always a careful balance between improving vision and protecting your long-term eye health. I emphasise to my patients that RLE isn’t just about achieving clearer vision it’s about supporting your eyes and preserving optic nerve function while managing glaucoma effectively.
Choosing the Right Lens for Glaucoma Patients
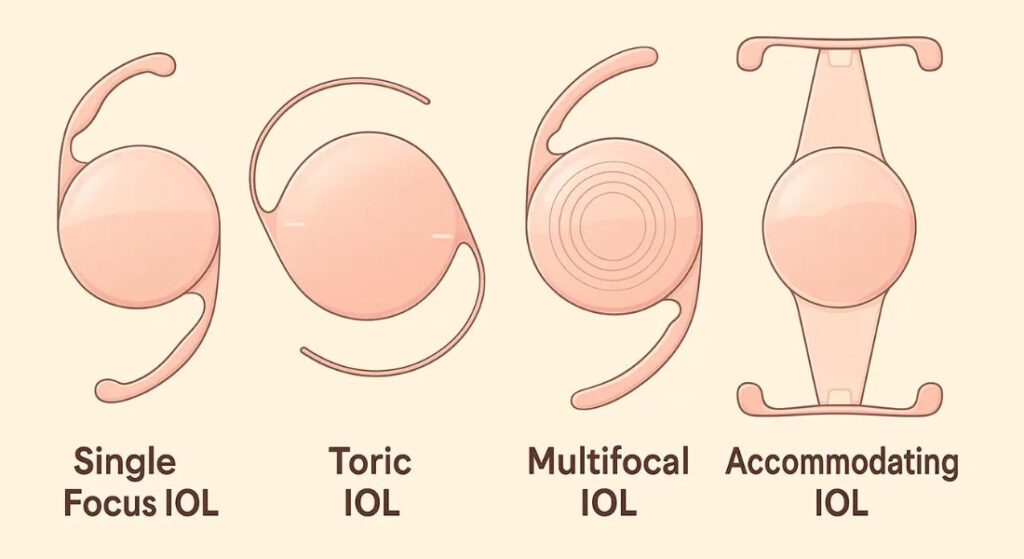
Selecting the correct intraocular lens (IOL) is a critical decision for glaucoma patients considering RLE surgery. Not all lenses are suitable, as certain designs can affect contrast and low-light vision areas already vulnerable due to optic nerve damage. Choosing the right lens involves balancing visual goals, glaucoma severity, and eye health to ensure both safety and optimal vision. This careful planning helps prevent complications and maximises post-operative satisfaction.
- Monofocal Lenses: These lenses provide clear vision at a single focal point, typically distance. They offer predictable outcomes and minimise the risk of reduced contrast sensitivity, making them a safer choice for glaucoma patients who may already have compromised optic nerves.
- Toric Lenses: Designed to correct astigmatism, toric lenses can improve clarity and reduce dependence on glasses. However, precise measurements are essential, as even small errors can affect visual outcomes and potentially complicate glaucoma management.
- Avoiding Multifocal Lenses in Advanced Glaucoma: Multifocal or extended depth-of-focus lenses split light to provide multiple focal points, which can reduce contrast and night vision. For patients with advanced glaucoma, these lenses can amplify existing visual challenges, so I generally advise against them in such cases.
- Personalised Lens Selection: Lens choice is not one-size-fits-all. I carefully discuss how optic nerve health, glaucoma severity, lifestyle, and visual needs influence the best lens option, ensuring that patients make informed decisions that prioritise both vision quality and safety.
In conclusion, choosing the right lens is a vital part of planning RLE surgery for glaucoma patients. By considering lens type, visual goals, and individual eye health, we can reduce risks and optimise outcomes. A thoughtful, personalised approach ensures that patients achieve the best balance between safety, comfort, and visual clarity.
Post-Operative Monitoring Is Essential
For glaucoma patients, follow-up care after RLE surgery is not optional it’s absolutely critical. Your eyes need careful monitoring to ensure that intraocular pressure (IOP) remains stable and that the optic nerve is not under stress. Early detection of any issues allows your surgeon to intervene before complications occur.
I usually schedule check-ups at several key intervals. On Day 1 after surgery, we check your IOP to catch any immediate spikes. During the first week, we assess your healing, visual clarity, and IOP trends. At around one month, a full examination is conducted, which may include imaging of the optic nerve if necessary.
Ongoing glaucoma monitoring continues long after your RLE, because while the surgery can improve vision, it does not cure glaucoma. If any pressure spikes or signs of optic nerve stress are detected, interventions can include temporary medications, laser therapy, or other treatments to prevent long-term damage. Regular follow-ups are essential to protect your vision and ensure the best possible outcome.
Lifestyle Considerations for Glaucoma Patients
While RLE surgery is an important step, your daily habits play a key role in protecting your vision, both during recovery and long-term. Maintaining healthy blood pressure is essential, as fluctuations can affect intraocular pressure (IOP) and potentially stress your optic nerve. Small adjustments to your routine can make a meaningful difference.
Moderate exercise can be beneficial, helping circulation and overall eye health, but it’s important to avoid heavy straining, especially immediately after surgery. Staying hydrated is also important, but rapid intake of large volumes of fluid can temporarily raise IOP, so pacing your fluids carefully is wise.
Adhering to your glaucoma medications and attending regular eye exams remain critical. Skipping drops or check-ups can jeopardise both your surgical outcome and long-term vision. These lifestyle adjustments may seem minor, but when glaucoma and RLE intersect, they play a significant role in supporting safe recovery and protecting your eyes for years to come.
When to Delay or Avoid RLE
In some cases, the safest approach is to delay or even avoid RLE surgery. This is especially important if you have advanced optic nerve damage, as fluctuations in intraocular pressure (IOP) during or after surgery could worsen your vision. Prioritising the long-term health of your eyes over immediate improvements is essential, and sometimes waiting until your glaucoma is more stable is the wisest choice.
Other factors may make surgery riskier. Poorly controlled IOP despite medications or previous laser treatments, severe corneal disease, or existing retinal problems can all increase the likelihood of complications. Your ophthalmologist will assess these conditions carefully and explain how they may impact both the procedure and recovery. This ensures that any decision about surgery is fully informed and tailored to your individual eye health.
Patient preference also plays an important role. You may feel more comfortable maintaining your current vision until your glaucoma is better managed or until your eyes are in a more stable condition. Being honest and open about these situations allows you and your surgeon to focus on protecting your long-term vision rather than rushing into surgery for short-term convenience. Thoughtful planning now often leads to safer outcomes and better results in the future.
Communicating Your Goals

One of the most important steps when planning RLE for glaucoma patients is having a clear discussion about your expectations. Understanding what matters most to you helps guide decisions about the procedure and lens choices. Are you primarily seeking freedom from glasses, or is maintaining stable vision the most important goal for you?
It’s also important to consider your willingness to commit to follow-up care. Regular appointments and potential adjustments in medication are often necessary to ensure both the success of your surgery and the long-term health of your eyes. Being prepared for this level of involvement is essential for a positive outcome.
Finally, think about how you weigh the benefits of clearer vision against potential glaucoma-related risks. Answering these questions honestly allows your ophthalmologist to create a personalised plan that aligns with both your vision goals and your eye health. Open communication ensures you feel confident and informed every step of the way.
Combining RLE with Glaucoma Procedures
In some cases, RLE surgery can be combined with glaucoma procedures to address both refractive needs and eye pressure management simultaneously. This approach requires careful planning to ensure safety and effectiveness, but it can offer significant benefits for patients with coexisting conditions. By coordinating treatments, we aim to improve vision while protecting the optic nerve and controlling intraocular pressure. These combined procedures are tailored to each patient’s unique eye health and glaucoma severity.
- Minimally Invasive Glaucoma Surgery (MIGS): MIGS procedures can be performed at the same time as lens removal to enhance fluid drainage and lower IOP. These surgeries are designed to be less invasive than traditional glaucoma surgery, reducing recovery time while still providing effective pressure control.
- Laser Trabeculoplasty: This laser treatment can be done before or after RLE to help manage eye pressure. By improving drainage through the trabecular meshwork, it reduces the risk of post-operative IOP spikes and helps maintain long-term glaucoma stability.
- Careful Planning for Dual Benefits: Combining RLE with glaucoma procedures requires precise pre-operative assessment and coordination. When done correctly, patients benefit from improved vision and better glaucoma management, minimising the need for additional surgeries in the future.
In conclusion, integrating RLE with glaucoma procedures can be a highly effective strategy for selected patients. With careful planning and personalised treatment, we can address both refractive needs and glaucoma control in a single surgical plan. This approach maximises safety, reduces overall recovery time, and provides comprehensive care for eyes affected by both conditions.
FAQs:
1. Can I have RLE surgery if I have glaucoma?
Yes, many patients with stable glaucoma can safely undergo RLE surgery. The key is that your intraocular pressure (IOP) and optic nerve health must be carefully assessed beforehand. Your surgeon will conduct a thorough evaluation and tailor the procedure to minimise any risk of optic nerve damage or pressure-related complications.
2. How does glaucoma affect RLE surgery risks?
Glaucoma makes the eyes more vulnerable during and after surgery. Post-operative spikes in IOP can stress the optic nerve, and pre-existing damage may limit the degree of visual improvement. Other risks include slower corneal healing and temporary visual fluctuations. Close monitoring and preventive strategies help reduce these risks.
3. What tests are needed before RLE if I have glaucoma?
Before surgery, a detailed assessment is performed. This typically includes optical coherence tomography (OCT) to check the optic nerve, visual field testing to map blind spots, multiple IOP measurements to assess fluctuations, angle assessment to evaluate fluid drainage, and a thorough review of glaucoma medications. These tests allow your surgeon to plan the safest approach.
4. Can RLE surgery benefit glaucoma patients?
In some cases, RLE can offer added benefits. For patients with angle-closure glaucoma, removing the natural lens can deepen the anterior chamber and improve fluid drainage, which may lower IOP and reduce dependence on eye drops. While the primary goal is vision correction, these secondary benefits can help protect the optic nerve over time.
5. Which type of lens is safest for glaucoma patients?
Monofocal lenses are usually recommended because they provide clear vision at a single distance and preserve contrast sensitivity, which is important for eyes already affected by glaucoma. Toric lenses may be used for astigmatism, but multifocal or extended-depth lenses are often avoided in advanced glaucoma as they can reduce contrast and night vision.
6. Is post-operative monitoring different for glaucoma patients?
Absolutely. After RLE, glaucoma patients require close follow-up to monitor IOP and optic nerve health. Checks usually occur on Day 1, the first week, one month, and at regular intervals thereafter. Early detection of IOP spikes or other complications allows timely intervention, which is critical for protecting long-term vision.
7. Can RLE be combined with glaucoma surgery?
Yes, in selected cases. Minimally Invasive Glaucoma Surgery (MIGS) or laser trabeculoplasty can be performed alongside RLE to improve fluid drainage and reduce IOP. Combining procedures can help patients achieve better vision and glaucoma control simultaneously, though it requires careful planning and assessment of the eye’s anatomy and disease severity.
8. When should RLE surgery be delayed or avoided for glaucoma patients?
Surgery may be postponed if glaucoma is advanced, IOP is poorly controlled, optic nerve damage is severe, or if other eye conditions are present. Prioritising optic nerve health over immediate vision correction ensures long-term safety. Your surgeon will only proceed once your glaucoma is stable and your eyes are in the best condition for surgery.
9. How do lifestyle factors affect RLE outcomes in glaucoma?
Lifestyle plays an important role in recovery and long-term eye health. Maintaining healthy blood pressure, adhering to glaucoma medications, pacing fluid intake, avoiding heavy straining, and doing moderate exercise all help maintain stable IOP. These steps reduce the risk of post-operative complications and support a smoother healing process.
10. hat are realistic expectations for glaucoma patients considering RLE?
RLE can provide significant improvement in refractive vision, reducing dependence on glasses or contact lenses. However, it does not cure glaucoma or prevent future optic nerve damage. Ongoing monitoring, medication adherence, and regular eye exams remain essential to protect your vision. The goal is safer, clearer vision while preserving long-term eye health.
Final Thoughts: RLE Surgery for Glaucoma Patients
RLE surgery can be a safe and effective option for many patients with stable glaucoma, but it requires careful planning, thorough pre-operative assessment, and ongoing post-operative monitoring. Protecting your optic nerve, managing intraocular pressure, and choosing the right lens are all essential steps to ensure both visual improvement and long-term eye health. Every patient’s situation is unique, so understanding your glaucoma type, the current state of your optic nerve, and how your eyes respond to pressure changes is crucial. Close collaboration with your ophthalmologist, adherence to medication, and regular check-ups allow for a tailored approach that balances safety with the best possible visual outcomes.
By working closely with your ophthalmologist and following recommended lifestyle and follow-up measures, you can achieve a successful outcome while minimising risks. If you’re looking for refractive lens exchange in London, you can get in touch with us at London Cataract Centre to discuss a personalised plan for your eyes.
References:
- Pasquali, A., Varano, L., Ungaro, N., Tagliavini, V., Mora, P., Goldoni, M. and Gandolfi, S., 2024. Does cataract extraction significantly affect intraocular pressure of glaucomatous/hypertensive eyes? Meta‑analysis of literature. Journal of Clinical Medicine https://www.mdpi.com/2077-0383/13/2/508/review_report
- Wang, S.Y., et al., 2020. Intraocular Pressure Changes after Cataract Surgery in Patients with and without Glaucoma: An Informatics‑Based Approach. Ophthalmology Glaucoma. https://pmc.ncbi.nlm.nih.gov/articles/PMC7529869/
- Tzu, J.H., Shah, C.T., Galor, A., Junk, A.K., Sastry, A. and Wellik, S.R., 2015. Refractive outcomes of combined cataract and glaucoma surgery. Journal of Glaucoma, https://pubmed.ncbi.nlm.nih.gov/24247998/
- Hayashi, K., 2001. Effect of cataract surgery on intraocular pressure control in glaucoma patients. Journal of Cataract and Refractive Surgery. https://www.sciencedirect.com/science/article/abs/pii/S0886335001010367
- Qureshi, I.A., 1997. Intraocular Pressure, Ocular Hypertension, and Glaucoma. Journal of Human Hypertension https://academic.oup.com/joh/article/39/3/211/7270525