If you’re living with osteoporosis and considering refractive lens exchange (RLE) surgery, it’s natural to wonder how your bone health might affect the procedure. You may have concerns about medications, healing, or whether systemic issues could influence your suitability. These are valid questions that deserve careful consideration.
Many patients worry about how osteoporosis treatments, such as bisphosphonates or calcium supplements, might interact with surgery. You may also wonder if your bone density could affect your recovery or the procedure itself. Discussing these details beforehand helps clarify any potential risks and ensures your plan is personalised.
The good news is that osteoporosis rarely prevents patients from undergoing RLE. The surgery primarily involves the eyes and does not place strain on bones, so most people with well-managed osteoporosis can proceed safely. Understanding your overall health allows for better planning and confidence.
By addressing both your bone health and eye health, we can ensure a safe and successful outcome. Careful pre-surgery evaluation and clear communication about medications or systemic conditions help reduce risks. With proper preparation, you can approach RLE with reassurance and peace of mind.
Why This Topic Matters
Your eyes don’t exist in isolation they are part of your overall health. Conditions like osteoporosis mainly affect your bones, but your general health, medications, and healing capacity can still influence surgical planning. Being aware of these connections helps ensure that your procedure is as safe and effective as possible.
Understanding how your systemic health interacts with RLE allows you to make informed decisions. You’ll know what to expect before, during, and after surgery, which can reduce anxiety. This knowledge also enables your care team to tailor the approach to your specific needs.
Being informed gives you confidence and helps minimise unnecessary risks. When you understand both your eye health and your overall condition, you can approach surgery with clarity and reassurance. Proper preparation is key to a smooth and successful outcome.
What Is RLE Surgery?
Before looking at osteoporosis-specific factors, it’s helpful to understand what refractive lens exchange (RLE) involves. Knowing the procedure basics makes it easier to see how your overall health, medications, or healing ability could influence surgical planning. Being informed helps you feel more confident and prepared.
RLE involves removing your natural lens and replacing it with an artificial intraocular lens. This new lens is designed to correct your vision and reduce dependence on glasses or contact lenses. The procedure is precise and tailored to your individual vision needs, offering clearer sight for distance, near, or both depending on the lens chosen.
RLE is very similar to cataract surgery, but the main difference is that it is done to improve vision rather than remove a cloudy lens. Understanding this distinction helps you set realistic expectations and plan appropriately. Knowing the basics also allows you to see how conditions like osteoporosis might factor into your overall surgical care.
Why People Consider RLE
You may be considering refractive lens exchange to reduce your reliance on glasses or contact lenses. Many people find the idea of clearer vision without constantly reaching for visual aids very appealing. It can make everyday activities like reading, driving, or using screens much easier.
Age-related vision changes, such as presbyopia, are another common reason to choose RLE. These changes can make near vision more difficult, requiring reading glasses or frequent adjustments. RLE can help correct these issues, improving both distance and near vision in a single procedure.
In some cases, laser eye surgery may not be suitable. Thin corneas, high prescriptions, or other eye conditions can make alternatives like RLE a safer and more effective option. Understanding why people choose RLE helps you consider whether it could be right for your vision needs.
Understanding Osteoporosis
Osteoporosis is a condition that causes your bones to become weak and more prone to fractures. This happens because bone density decreases, making the structure of your bones less stable. It can develop slowly over time, often without obvious symptoms until a fracture occurs.
The condition is most common in older adults, particularly postmenopausal women, but men can also be affected. Age, hormonal changes, and certain lifestyle factors can all contribute to its development. Being aware of your risk helps you take steps to protect your bone health.
Osteoporosis often requires medications to strengthen bones and reduce the risk of fractures. These treatments may include calcium and vitamin D supplements, bisphosphonates, or other therapies tailored to your needs. Managing the condition effectively supports both general health and surgical safety.
How Osteoporosis Affects the Body
Osteoporosis is a condition characterised by weakened bones, which can impact mobility, posture, and overall physical stability. Beyond the skeletal system, it may also affect how your body responds to surgery and healing. Medications used to manage osteoporosis can interact with other treatments, influencing recovery and surgical planning. Understanding these factors helps your healthcare team take a holistic approach, ensuring your eye procedure is both safe and effective.
- Impact on Mobility and Posture: Fragile bones can make movements more cautious and increase the risk of falls. Reduced mobility or altered posture may affect how you position yourself during surgery and recovery. Awareness of these challenges allows the surgical team to plan for additional support if needed.
- Systemic Health Considerations: Osteoporosis often coexists with other health conditions, such as arthritis or vitamin deficiencies. These factors can influence healing rates and response to anesthesia. Comprehensive assessment ensures your overall health is optimally managed before surgery.
- Medication Interactions: Treatments for osteoporosis, including bisphosphonates or hormone therapies, may interact with other medications used during surgery. Sharing your full medication list allows your doctor to avoid potential complications and tailor perioperative care accordingly.
- Bone Health and Recovery: Strong bone and tissue support contribute to smoother postoperative recovery. By considering your bone health in surgical planning, the team can reduce the risk of complications and promote quicker, safer healing.
In conclusion, osteoporosis affects more than just bones it can influence mobility, medication interactions, and overall surgical planning. By recognising these connections, your eye procedure can be approached with a focus on safety and holistic care. Understanding your systemic health allows your surgical team to customise treatment, supporting both comfort and recovery. Maintaining awareness of bone health ensures the best possible outcomes throughout your surgical journey.
Common Medications for Osteoporosis
Managing osteoporosis often involves a combination of medications and supplements to strengthen bones and reduce fracture risk. These treatments work in different ways, from slowing bone breakdown to supporting bone density. While most are compatible with RLE surgery, it’s important for your surgical team to know exactly what you are taking. This ensures any potential interactions or precautions are addressed in advance.
- Bisphosphonates: These medications reduce bone resorption, helping to maintain bone density and prevent fractures. They are generally safe for use around the time of eye surgery, though long-term use may require monitoring for certain systemic effects. Informing your doctor allows them to confirm there are no specific risks for your procedure.
- Denosumab: Denosumab is a monoclonal antibody that strengthens bones by targeting cells that break down bone tissue. It is usually compatible with surgery, but timing of doses may be considered to optimise recovery. Awareness of this medication helps your surgeon plan for any potential effects on healing.
- Hormone Therapy: Sometimes prescribed to postmenopausal women, hormone therapy can help maintain bone density. While generally safe for eye surgery, it’s important to discuss any hormone treatment as it may influence clotting or other systemic factors. This ensures safe perioperative care.
- Calcium and Vitamin D Supplements: These supplements support overall bone health and are typically safe to continue before and after RLE surgery. They help maintain bone strength and general wellness, without interfering with surgical outcomes. Maintaining regular supplementation contributes to overall recovery and stability.
In conclusion, osteoporosis medications each have unique mechanisms but are largely compatible with RLE surgery. Keeping your surgical team informed ensures that any potential interactions or timing considerations are addressed. This careful planning supports both your bone health and a smooth surgical experience. By understanding your treatments, you and your surgeon can work together to optimise safety and recovery.
How Osteoporosis Medications May Influence Surgery
While osteoporosis medications mainly target bone health, they can have indirect effects that are relevant for eye surgery. Understanding these potential interactions helps ensure your procedure is safe and smooth. Being aware of how your treatments may affect your eyes or healing is an important part of pre-surgery planning.
For example, bisphosphonates commonly prescribed to strengthen bones can occasionally contribute to inflammation or dry eyes. Although these effects are rare, they are worth noting when preparing for RLE. Addressing any minor issues beforehand helps reduce discomfort and supports better outcomes.
We always review your medications in detail before surgery. This ensures there are no conflicts with sedatives, antibiotics, or post-operative eye drops. Careful evaluation allows your surgical team to adjust the plan if needed, making the procedure safer and more comfortable.
Bone Health and Anaesthesia
Refractive lens exchange is usually performed under local anaesthesia with mild sedation. This type of anaesthesia targets the eye and surrounding area, rather than putting your whole body to sleep. It is minimally invasive and generally very safe for patients with osteoporosis.
Unlike general anaesthesia, local anaesthesia does not significantly impact bone health. Your bones are not exposed to stress or strain during the procedure, which reduces the risk of fractures or injury. This makes RLE a suitable option for most patients with osteoporosis.
However, it’s still important to ensure that your posture and positioning during surgery are comfortable and safe. Proper support helps prevent strain on your spine or joints, particularly if your bones are fragile. Taking these precautions contributes to a safer and more comfortable surgical experience.
Pre-Surgery Assessment
Before any procedure, I always carry out a thorough assessment to ensure your safety and readiness. This step allows us to identify any factors that could affect surgery or recovery and plan accordingly. Being well-prepared reduces risks and helps the procedure run smoothly.
For patients with osteoporosis, the assessment includes reviewing your bone health history, current medications, and any other systemic conditions. Understanding your overall health helps us anticipate potential challenges and tailor the surgical plan to your needs.
We also check vital signs such as blood pressure and cardiovascular stability, as well as any previous reactions to anaesthesia. This ensures that your body is well-prepared for both the procedure and recovery, giving you confidence and peace of mind.
Managing Fracture Risk
During surgery, special attention is given to positioning and support, particularly for patients with osteoporosis. Fragile bones can be more vulnerable to strain, so ensuring proper alignment is essential. This careful approach helps protect your skeletal health while you undergo the procedure.
We make sure you are comfortable on the surgical bed and avoid any movements or pressure that could increase fracture risk. Even small adjustments, such as extra padding or repositioning, can make a significant difference.
By taking these precautions, we can maintain both your safety and comfort throughout the surgery. Proper support allows you to focus on the procedure itself, knowing that your bone health is being protected.
Healing Considerations
Osteoporosis does not directly impact how your eyes heal after refractive lens exchange. The cornea and intraocular lens recovery process remain the same as in patients without bone conditions. This means your visual healing is generally unaffected by bone health alone.
However, systemic health, nutritional status, and any medications you take for osteoporosis can influence overall recovery. Adequate nutrition and well-managed health support your body’s ability to heal efficiently. Paying attention to these factors can make a noticeable difference in comfort and recovery speed.
Eye Surface Health
Maintaining a healthy tear film and ocular surface is important for all patients preparing for RLE. A stable and well-lubricated eye surface ensures accurate pre-surgical measurements, helps with lens placement, and contributes to a smoother surgical experience. It also supports faster and more comfortable healing after the procedure, which is vital for achieving the best possible vision outcomes.
In rare cases, some osteoporosis medications may contribute to mild dry eye. Although uncommon, even minor dryness can affect comfort during surgery and the accuracy of measurements needed for the intraocular lens. Addressing these issues ahead of time helps reduce any potential complications and improves overall results.
We always assess and treat any ocular surface problems prior to surgery. This may include artificial tears, lubricating gels, or other measures to stabilise the tear film. Ensuring your eyes are in optimal condition before RLE supports a safer procedure, a smoother recovery, and clearer, more reliable vision after surgery.
Sedation and Medication Review
Mild sedation is typically used during RLE to keep you calm and comfortable throughout the procedure. This type of sedation is carefully controlled and allows you to remain relaxed while the surgery is performed safely.
We always review your osteoporosis medications beforehand to check for any potential interactions or side effects. While most bone-strengthening treatments do not interfere with RLE, it’s important to confirm this to avoid complications.
This careful review helps ensure the procedure runs smoothly without affecting your overall health. By coordinating your medications and sedation plan, we can provide a safe, comfortable, and well-managed surgical experience.
Choosing the Right Lens
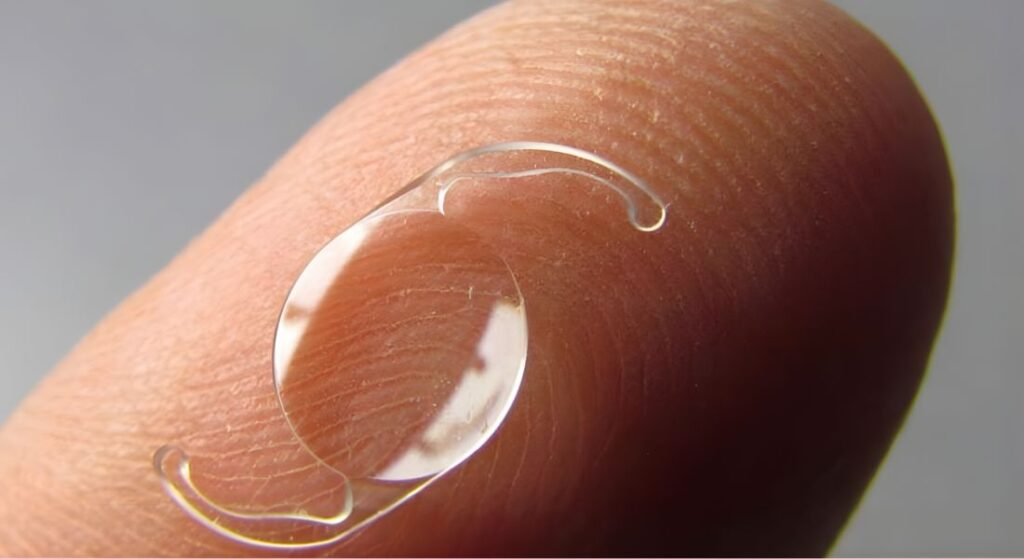
Choosing the right lens for RLE is tailored to your lifestyle, eye health, and vision goals. The type of lens you select can significantly influence how much you rely on glasses after surgery. Understanding the options helps you make a choice that fits your daily needs.
Monofocal lenses provide excellent distance vision but usually require reading glasses for near tasks. They are a reliable option for patients prioritising sharp distance vision and simplicity.
Multifocal or extended-depth-of-focus lenses can reduce your dependence on glasses for both near and distance vision. However, these options are assessed carefully in the context of your ocular health and any systemic conditions, such as osteoporosis, to ensure optimal outcomes. This personalised approach helps achieve the best balance between vision correction and overall safety.
Managing Expectations
I always emphasise the importance of having realistic expectations before undergoing RLE. While the procedure can dramatically improve vision and reduce your dependence on glasses or contact lenses, it is not a cure-all. Understanding what it can and cannot do helps you approach surgery with a clear perspective.
RLE does not treat osteoporosis or other systemic health conditions. Your bone health, medications, and overall wellness remain important for surgical planning and recovery, but they are separate from the visual outcomes of the procedure.
Focusing on achievable results ensures you can appreciate the benefits of RLE without disappointment. Clear communication and careful planning help you feel confident and prepared for the experience, both during and after surgery.
When Surgery Might Be Delayed
In some cases, surgery may need to be postponed if your osteoporosis medications or general health require optimisation. Ensuring that your body is in the best possible condition helps minimise any potential risks during the procedure.
Delaying surgery allows time to adjust medications, improve bone health, or address other systemic concerns. This preparation ensures your body is ready to handle both the procedure and recovery safely.
Taking the time to optimise your health before RLE improves both safety and visual outcomes. Proper planning provides peace of mind and supports a smoother, more comfortable surgical experience.
Timing Is Crucial
Proper timing is key to ensuring that both your eyes and your overall health are ready for surgery. Planning the procedure carefully allows your body to be in the best possible condition, which helps reduce stress and potential complications.
Rushing into surgery without optimising systemic health or reviewing medications can increase risks during the procedure. Taking the time to stabilise your health and address any concerns beforehand makes a significant difference.
Thorough preparation ensures a safer, smoother, and more comfortable surgical experience. By coordinating timing with your overall health, you give yourself the best chance for a successful outcome and a quick, uncomplicated recovery.
Lifestyle Factors That Help

Good general health plays an important role in ensuring the best outcomes from surgery. Supporting your bones and overall wellbeing helps your body recover efficiently and reduces the risk of complications. Simple lifestyle adjustments, alongside your prescribed treatments, can make a meaningful difference in both comfort and healing. Taking proactive steps before surgery sets the foundation for a smoother recovery process.
- Adequate Nutrition and Calcium Intake: Consuming a balanced diet rich in calcium and other essential nutrients supports bone strength. Proper nutrition also aids tissue repair and overall recovery after surgery. Ensuring you meet daily calcium requirements complements your osteoporosis treatment plan.
- Maintaining Hydration: Staying well hydrated supports all bodily functions, including circulation and healing. Adequate fluid intake also contributes to eye health, helping maintain a stable tear film before procedures like RLE. Hydration is a simple but effective step to optimise surgical outcomes.
- Following Your Prescribed Osteoporosis Medication Schedule: Consistently taking medications as directed helps maintain bone density and reduces fracture risk. Adhering to your schedule ensures your body remains in the best condition for surgery and recovery. Clear communication with your healthcare provider about medications prevents potential complications.
- Regular Physical Activity Within Your Abilities: Gentle exercise, tailored to your mobility and bone health, helps maintain strength, balance, and circulation. This not only supports bones but also aids overall wellness and resilience during recovery. Even light activity can contribute significantly to post-surgical outcomes.
In conclusion, lifestyle factors play a vital role in supporting both bone health and overall recovery from surgery. Adequate nutrition, hydration, adherence to medications, and safe physical activity all contribute to optimal results. Prioritising these habits helps your body heal efficiently and reduces the likelihood of complications. By combining healthy routines with medical guidance, you set yourself up for a safer, smoother surgical experience.
Post-Operative Care
After RLE, patients are typically prescribed anti-inflammatory and antibiotic eye drops. These drops help reduce inflammation, prevent infection, and support a smooth healing process. Following the instructions carefully is important for achieving the best results.
In most cases, these post-operative medications are fully compatible with osteoporosis treatments. You can usually continue your bone-strengthening medications without any issues.
We always review all prescriptions before surgery to ensure there are no potential interactions or side effects. This careful approach helps protect both your eyes and overall health while keeping your recovery as comfortable as possible.
Long-Term Eye Health
Even after a successful RLE procedure, ongoing eye check-ups remain essential. Regular monitoring ensures that your lens implants continue to function well and allows any potential issues to be detected early. This helps protect your long-term vision and maintain clear sight.
Your bone health does not interfere with the function of lens implants, so osteoporosis itself generally does not affect your visual outcomes. However, maintaining overall systemic wellbeing remains important for recovery and general health.
By combining regular eye care with attention to your general health, you can support both long-term vision and overall wellbeing. Routine follow-ups allow your eye care team to address any changes promptly, keeping your eyes in optimal condition.
Recovery After RLE
Most patients notice an improvement in their vision within just a few days after RLE. This rapid enhancement is one of the main benefits of the procedure, making everyday tasks like reading or driving much easier.
Full visual stabilisation may take several weeks, but osteoporosis does not interfere with the eye’s healing process. Your cornea and lens adapt in the same way as in patients without bone conditions.
We continue to monitor all patients closely during recovery to ensure everything progresses smoothly. Regular follow-ups help address any minor issues early, supporting a safe and comfortable healing process.
Emotional Considerations
Living with osteoporosis can already be stressful, especially if mobility is limited or you are concerned about fracture risk. These worries can affect day-to-day life and sometimes make decisions about medical procedures feel more daunting.
Adding eye surgery into the mix can increase anxiety further, even if the procedure itself is low risk. It’s natural to feel uncertain about outcomes, recovery, or how your health may affect the surgery.
I encourage patients to discuss their concerns openly. By addressing both visual and emotional needs, we can create a supportive environment that helps you feel reassured, informed, and confident throughout the process.
FAQs:
1. Can I have refractive lens exchange (RLE) if I have osteoporosis?
Yes. Osteoporosis does not directly affect the eye, and most patients with well-managed bone health can safely undergo RLE.
2. Do osteoporosis medications interfere with RLE surgery?
Most treatments, including bisphosphonates, calcium, vitamin D, and hormone therapy, are compatible with RLE. Your surgeon will review your full medication list to ensure safety.
3. Does osteoporosis increase the risk of complications during RLE?
Not usually. RLE is minimally invasive and does not strain bones. Extra precautions may be taken for posture and positioning if bones are fragile.
4. Can osteoporosis affect healing after RLE?
Osteoporosis itself generally does not impact eye healing. Overall health, nutrition, and systemic conditions can influence recovery speed and comfort.
5. Should I adjust my calcium or vitamin D intake before surgery?
No major adjustments are typically needed. Maintaining your usual supplements supports bone health and overall recovery.
6. Is local anaesthesia safe if I have osteoporosis?
Yes. RLE uses local anaesthesia with mild sedation, which does not place stress on bones and is generally very safe for patients with osteoporosis.
7. How do bisphosphonates affect eye surgery?
While rare, some bisphosphonates may cause mild eye surface irritation. Pre-surgery assessment ensures any issues are managed beforehand.
8. What precautions are taken during surgery for osteoporosis patients?
Special attention is given to positioning, support, and posture to minimise any risk of fractures or strain during the procedure.
9. Can osteoporosis affect lens selection for RLE?
Osteoporosis usually does not limit lens choice. Lens type is determined by visual needs, lifestyle, and eye health rather than bone health.
10. How can I optimise my health before RLE if I have osteoporosis?
Maintain your medications, ensure adequate nutrition and calcium intake, stay hydrated, engage in safe physical activity, and communicate any concerns with your surgeon.
Final Thoughts: Planning RLE with Osteoporosis in Mind
Having osteoporosis should not prevent you from considering refractive lens exchange, as the procedure is focused on the eyes and does not place stress on your bones. With a thorough pre-surgery assessment, careful review of medications, and attention to your overall health, RLE can be performed safely and effectively. Ensuring your condition is well-managed and maintaining good nutrition and lifestyle habits can further support a smooth experience and recovery. If you’re thinking about refractive lens exchange surgery, you can get in touch with us at London Cataract Centre.
References:
- Migliorini, F., Maffulli, N. and Eschweiler, J. (2021) Bisphosphonates and their clinical use in osteoporosis, Journal of Clinical Medicine, 10(9), p. 2027. Available at: https://www.mdpi.com/2077-0383/10/9/2027
- Pazianas, M., Clark, E.M., Eiken, P.A., Brixen, K. and Abrahamsen, B. (2013) Inflammatory eye reactions in patients treated with bisphosphonates and other osteoporosis medications: cohort analysis using a national prescription database, Journal of Bone and Mineral Research, 28(3), pp. 455–463. Available at: https://pubmed.ncbi.nlm.nih.gov/23044864/
- Clark, E.M. and Durup, D. (2015) Inflammatory eye reactions with bisphosphonates and other osteoporosis medications: what are the risks? Therapeutic Advances in Musculoskeletal Disease, 7(1), pp. 11–16. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC4314301/
- Alió, J.L., Grzybowski, A. and Romaniuk, D. (2014) Refractive lens exchange, Survey of Ophthalmology, 59(6), pp. 579–598. Available at: https://www.sciencedirect.com/science/article/abs/pii/S0039625714000873
- Etminan, M., Forooghian, F. and Maberley, D. (2012) Inflammatory ocular adverse events with the use of oral bisphosphonates: a retrospective cohort study, Canadian Medical Association Journal, 184(8), pp. E431–E434. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC3348220/

