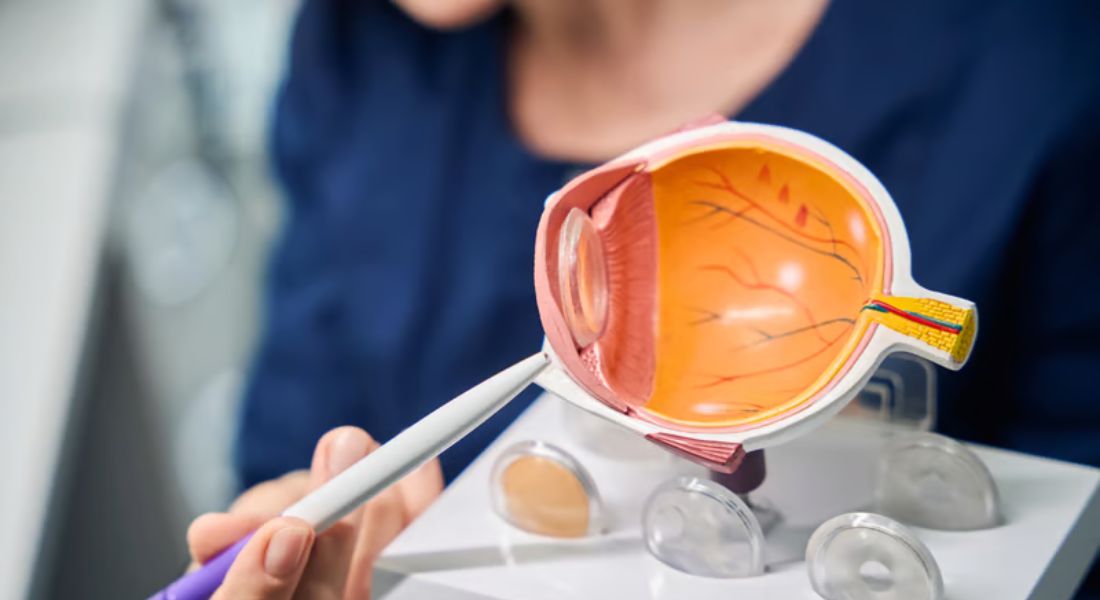
If you have macular degeneration and are considering refractive lens exchange (RLE), it’s natural to feel cautious. The condition affects the central part of your retina, which is vital for sharp, detailed vision. Knowing the potential benefits and limitations of RLE is essential before making any decisions.
RLE involves removing your natural lens and replacing it with an artificial intraocular lens (IOL). This procedure can correct vision issues such as presbyopia or hyperopia, reducing your dependence on glasses or contact lenses. However, for patients with retinal disease, additional considerations come into play that can affect both the safety and outcome of surgery.
A thorough evaluation of your retinal health is the first step. Your ophthalmologist will assess the extent of macular degeneration, check for signs of fluid, scarring, or atrophy, and determine how these factors might influence surgical results. Understanding the current condition of your retina helps set realistic expectations for what RLE can achieve.
With careful planning, RLE can still be a suitable option for some patients with macular degeneration. The key is a personalised approach that considers your retinal status, lens choice, and overall eye health. While the procedure can improve certain aspects of vision, it is important to recognise that it cannot reverse existing retinal damage, so clear communication with your surgeon is vital.
Understanding Macular Degeneration
Macular degeneration primarily affects the central part of your retina, called the macula, which is responsible for sharp, detailed vision. This is the area that allows you to read, recognise faces, and see fine details clearly. Any damage here can significantly impact daily activities, making careful evaluation essential before considering RLE surgery.
There are two main types of macular degeneration: dry (atrophic) and wet (neovascular). Dry AMD usually progresses slowly over time, which can make planning procedures like RLE more predictable. Wet AMD, on the other hand, can cause rapid changes in vision due to abnormal blood vessel growth and leakage, which may complicate surgical decisions.
Knowing which type you have is a critical first step in assessing your suitability for RLE. Your ophthalmologist will review your retinal scans, monitor for fluid or scarring, and help you understand how your specific condition may influence both the safety and outcomes of the procedure. This knowledge sets the foundation for realistic expectations and a personalised surgical plan.
Early versus Advanced AMD
The stage of your macular degeneration is a major factor when considering RLE surgery. In early AMD, your central vision is often still strong, and the retina retains much of its function. In these cases, RLE may offer meaningful improvements, such as reducing your dependence on glasses and enhancing overall clarity of vision.
Advanced AMD, however, presents more challenges. Damage to the macula may already have affected sharp vision, and RLE cannot reverse this retinal loss. While the procedure may still improve some aspects of vision, the overall benefits are often limited, and expectations need to be carefully managed.
Understanding the stage of your AMD helps you and your ophthalmologist make informed decisions about surgery. By aligning your expectations with your retinal health, you can plan for realistic outcomes while protecting the long-term function of your eyes. A personalised approach ensures safety and maximises the potential advantages of RLE.
How RLE Works for AMD Patients
It’s important to remember that RLE does not treat macular degeneration itself. The surgery is designed to replace your natural lens with an artificial intraocular lens (IOL) to correct refractive errors, such as long-sightedness, presbyopia, or other lens-related vision issues. This means that RLE addresses the lens, not the underlying retinal damage caused by AMD.
For patients with macular degeneration, RLE can still offer meaningful benefits. By correcting your refractive errors, the procedure can improve your overall visual clarity, particularly in the peripheral vision, and reduce your dependence on glasses or contact lenses. These improvements can enhance your day-to-day activities, even if central vision remains affected by AMD.
I always make sure my patients understand this distinction clearly. While RLE can enhance certain aspects of your vision and quality of life, it cannot restore vision that has already been lost due to retinal damage. Being realistic about what the surgery can achieve helps set expectations and ensures that your goals for vision improvement are achievable and safe.
Pre-Operative Retinal Assessment
A detailed retinal assessment is a crucial step before considering RLE surgery, especially for patients with diabetes or glaucoma. The retina’s health directly affects both surgical safety and potential visual outcomes. Early identification of retinal issues allows for timely treatment or adjustments in surgical planning, ensuring the best possible results. This assessment helps create a clear picture of eye health and informs personalised surgical decisions.
- Imaging with Optical Coherence Tomography (OCT): OCT provides a detailed, cross-sectional view of the retina, allowing me to detect subtle changes or damage to the macula. Understanding these details helps predict how your vision may respond to surgery and whether any interventions are needed beforehand.
- Fundus Photography: Capturing detailed images of the retina helps document current retinal health and detect areas of concern, such as microaneurysms or early diabetic changes. These images are invaluable for planning surgery and monitoring post-operative progress.
- Assessing Safety and Visual Outcomes: Retinal imaging helps determine if RLE surgery is safe and sets realistic expectations for visual improvement. Any detected abnormalities can be treated or stabilised before surgery, reducing risks and maximising recovery potential.
In conclusion, a comprehensive pre-operative retinal assessment is essential for patients considering RLE surgery. By using OCT and fundus photography, I can evaluate retinal health thoroughly, identify risks early, and tailor the surgical approach to each patient’s needs. This step ensures safer surgery and supports the best possible visual outcomes.
Setting Realistic Expectations
One of the most important parts of my consultations is discussing what RLE can realistically achieve for patients with macular degeneration. While many hope for perfect vision, it’s essential to understand that AMD limits the potential improvements. The procedure cannot reverse damage to the central retina, so your expectations need to be grounded in what is medically possible.
The primary goal of RLE in AMD patients is often to maximise your remaining vision. Correcting refractive errors can improve overall clarity, reduce dependence on glasses or contact lenses, and make day-to-day activities easier and more comfortable. These benefits may seem subtle compared to restoring vision completely, but they can significantly enhance quality of life.
I always emphasise the importance of patience and understanding the limits of surgery. By focusing on achievable outcomes such as sharper peripheral vision, reduced visual strain, and better overall visual comfort you can make an informed decision that aligns with your eye health and personal goals. Clear communication ensures that you feel confident and prepared for the procedure.
Importance of Visual Acuity Measurement
Measuring your visual acuity before RLE surgery is an essential step in planning the procedure. It gives a clear picture of how well your eyes are currently functioning and helps set realistic expectations for what the surgery can achieve. Knowing your baseline vision is particularly important for patients with macular degeneration, where central vision may already be compromised.
If your central vision is significantly affected, RLE may not dramatically improve how you see, even though the lens itself is replaced successfully. Understanding this limitation upfront helps you focus on achievable outcomes, such as sharper peripheral vision, reduced dependence on glasses, or improved overall visual comfort.
Visual acuity measurements also guide lens selection and surgical planning. Your ophthalmologist can use this information to choose the most suitable intraocular lens (IOL) and tailor the procedure to your individual eye health. Being informed about your starting point ensures a personalised approach and helps you make confident decisions about surgery.
Lens Selection Considerations
Selecting the right intraocular lens (IOL) is a critical step for patients with age-related macular degeneration (AMD) considering RLE surgery. The choice of lens can significantly affect contrast sensitivity, visual clarity, and overall satisfaction after surgery. Understanding how different lenses interact with retinal health helps ensure safer outcomes and optimal vision. Careful lens selection allows patients to achieve the best balance between functional vision and comfort.
- Monofocal Lenses: These lenses provide clear vision at a single distance, typically distance vision, and are generally well-tolerated by AMD patients. They offer predictable visual outcomes while minimising the risk of contrast sensitivity issues, which is important for eyes with retinal damage.
- Avoiding Multifocal Lenses: Multifocal lenses split light to provide multiple focal points, which can reduce contrast and night vision. For AMD patients, especially those with existing retinal damage, these lenses may amplify visual challenges and cause more strain or difficulty in low-light conditions.
- Personalised Lens Choice: Lens selection should consider the severity of retinal damage, visual goals, and lifestyle needs. I work closely with patients to ensure the lens chosen supports their daily activities and maximises visual comfort while minimising risks.
In conclusion, thoughtful lens selection is essential for AMD patients undergoing RLE surgery. Monofocal lenses often provide the safest and most predictable visual outcomes, while multifocal lenses may not be suitable in the presence of retinal damage. A personalised approach ensures patients achieve functional, comfortable vision while protecting their retinal health.
The Role of Contrast Sensitivity
Macular degeneration often reduces your contrast sensitivity, which is the ability to distinguish between subtle differences in light and dark. This can make everyday tasks, such as reading, recognising faces, or navigating in low-light conditions, more challenging. It’s an important factor to consider when planning RLE surgery.
Some types of intraocular lenses (IOLs) can further reduce contrast sensitivity, particularly certain multifocal or premium lenses. For patients with AMD, using these lenses may make it harder to see clearly in dim light or low-contrast situations. Selecting the right lens is therefore critical to preserving your remaining vision and maximising functional outcomes.
I always advise choosing lenses that maintain the highest possible contrast. This approach helps you make the most of your central vision and supports better overall visual performance after surgery. By tailoring lens selection to your retinal health, we can optimise clarity, comfort, and safety for daily activities.
Timing of Surgery
Timing is one of the most important factors when considering RLE for patients with macular degeneration. I always emphasise that surgery should ideally be performed when the condition is stable. When the retina is not actively changing, it allows for more predictable surgical planning and improves the likelihood of achieving a satisfactory visual outcome.
If macular degeneration is currently progressing, especially in cases of active wet AMD, it is usually better to prioritise retinal treatment first. Therapies such as anti-VEGF injections or other retinal interventions may be needed to stabilise the macula before any lens surgery is considered. Once the condition is under control, RLE can then be evaluated more safely.
Careful timing also allows your ophthalmologist to assess how much vision improvement is realistically possible. By ensuring the retina is stable and well monitored, we can reduce potential risks and give you the best chance of benefiting from RLE while protecting long-term retinal health.
Managing Expectations for Reading and Detail Work

Even after RLE, reading and other detailed tasks can remain challenging if the macula has been affected by degeneration. The macula is responsible for sharp, central vision, which is essential for activities like reading small print, recognising faces, or working on fine details. If this area has sustained damage, replacing the natural lens alone cannot fully restore that level of precision.
I always explain to patients that while RLE can improve overall clarity and reduce dependence on glasses, it does not repair retinal damage. Some patients notice better brightness or sharper peripheral vision after surgery, but central tasks may still require additional support. This is why it’s important to approach the procedure with realistic expectations about what improvements are possible.
In many cases, magnification tools or low-vision aids remain very helpful for daily activities. Simple devices such as handheld magnifiers, stronger reading lights, or digital magnification tools can make reading and detailed work much easier. Combining these aids with the visual improvements from RLE often provides the best overall outcome for patients living with macular degeneration.
Impact on Wet AMD Treatments
For patients receiving anti-VEGF injections or other treatments for wet AMD, RLE can still be considered in certain situations. However, it requires careful coordination with your retinal care plan. Wet age-related macular degeneration is typically managed with ongoing injections that control abnormal blood vessel growth, so surgery must be timed in a way that does not interrupt this treatment schedule.
In my experience, I work closely with retinal specialists to determine the safest timing for surgery. Often, RLE is scheduled between injection cycles, when the retina is stable and inflammation is minimal. This coordination helps ensure that the macular condition remains well managed while allowing the refractive benefits of lens replacement to be achieved.
The key goal is to make sure that RLE complements ongoing AMD treatment rather than complicating it. With good communication between your eye surgeon and retinal specialist, most patients can continue their injections without disruption while safely undergoing surgery.
Post-Operative Monitoring
Post-operative monitoring is particularly important for patients with macular degeneration. After RLE surgery, I usually schedule regular follow-up appointments to evaluate healing and ensure the retina remains stable. These visits often include detailed eye examinations and imaging tests such as OCT scans to closely monitor the macula.
Because RLE does not treat or stop macular degeneration, ongoing retinal surveillance is essential. Even if the surgery successfully improves refractive vision, the underlying retinal condition can still change over time. Early detection of any new macular changes allows timely treatment and helps protect the vision you still have.
I always remind patients that surgery is only one step in managing their eye health. Continued monitoring, adherence to treatment plans, and regular eye examinations play a crucial role in maintaining long-term visual stability.
Risks Specific to AMD Patients
Macular degeneration introduces a few additional risks that need to be carefully considered before RLE surgery. Because the retina is already affected, the eye can sometimes react more sensitively to the procedure. One possible complication is cystoid macular oedema, where fluid builds up in the central retina and temporarily affects vision. Although this condition is usually manageable with medication, it can delay the recovery process and require closer monitoring.
Another consideration is temporary visual fluctuation after surgery. Patients with AMD may notice that their vision takes longer to stabilise compared with those without retinal conditions. This happens because the macula is already compromised, so the eye needs more time to adapt after the lens has been replaced. In most cases, these changes settle gradually as healing progresses and the retina adjusts.
I always make sure to discuss these potential risks clearly during consultation. Having an open conversation helps patients understand what the recovery process may involve and prevents unrealistic expectations. When patients are well informed, they tend to feel more confident about the procedure and better prepared for the healing period.
Lifestyle Factors Affecting Outcomes
Your daily habits can play a meaningful role in both recovery after RLE surgery and the long-term progression of macular degeneration. Simple lifestyle choices often have a direct impact on how well your eyes heal and how stable your vision remains over time. I always encourage patients to think about their overall health, not just the surgery itself. Supporting your body properly gives your eyes the best possible environment for recovery.
Maintaining a balanced diet rich in antioxidants, vitamins, and essential nutrients is particularly helpful for retinal health. Foods containing vitamins C and E, zinc, lutein, and omega-3 fatty acids may support the macula and help slow the progression of AMD. Controlling blood pressure is equally important, as unstable blood pressure can affect circulation to the delicate structures of the eye. Good hydration and regular, moderate physical activity can also contribute to better overall eye health.
Avoiding smoking is one of the most significant lifestyle changes you can make if you have macular degeneration. Smoking is strongly linked with faster AMD progression and can also slow the healing process after surgery. By focusing on healthy habits and following medical advice, you can support both your surgical recovery and long-term retinal stability. These lifestyle choices work alongside surgical care to help protect and preserve your vision for the future.
Quality of Life Considerations
For many patients, the decision to undergo RLE surgery is not solely about achieving perfect vision. Instead, it is often about improving overall quality of life and making everyday activities easier and more comfortable. Even small improvements in visual clarity can significantly enhance independence and confidence. Understanding these benefits helps patients focus on realistic outcomes rather than perfection.
- Improved Visual Clarity: Even modest improvements in vision can make a noticeable difference in daily life. Tasks such as reading signs, recognising faces, or navigating unfamiliar environments can become easier and less stressful.
- Reduced Dependence on Glasses: One of the key motivations for RLE surgery is reducing reliance on glasses or contact lenses. While some patients may still need glasses for specific tasks, many experience greater freedom and convenience in their daily routines.
- Better Peripheral Awareness: Clearer vision can improve awareness of surroundings, which is particularly helpful for activities like walking outdoors, shopping, or driving. Enhanced peripheral vision can also contribute to a greater sense of safety and confidence.
- Greater Independence in Daily Activities: Improved vision can make everyday tasks such as cooking, reading, and using digital devices more comfortable. This increased independence often leads to better overall well-being and a more active lifestyle.
In conclusion, the goal of RLE surgery for many patients is to enhance quality of life rather than achieve flawless vision. Even moderate improvements can significantly impact daily comfort, independence, and confidence. By focusing on practical benefits and realistic expectations, patients can better appreciate the positive changes that surgery may bring to their everyday lives.
The Role of Low Vision Support
Low vision support can play an important role for patients with macular degeneration who undergo RLE surgery. While the procedure may improve overall clarity and reduce dependence on glasses, it cannot reverse damage that has already occurred in the macula. Because of this, additional visual support tools can help patients make the most of their remaining vision in everyday activities.
Many patients find that low vision aids significantly improve their ability to read, use digital devices, or perform detailed tasks. Tools such as handheld magnifiers, electronic readers, high-contrast displays, and specialised task lighting can make daily activities much easier and more comfortable. These technologies are designed to enhance contrast and enlarge text or images, helping compensate for the loss of central vision caused by macular degeneration.
I often encourage patients to explore these options with the help of a low vision specialist. Combining RLE surgery with the right visual aids can dramatically improve independence and quality of life. By using these supportive tools alongside regular eye care, patients can maximise functional vision and continue many of the activities they enjoy.
Communication with Your Surgeon

Open and honest communication with your surgeon is one of the most important parts of planning RLE surgery when you have macular degeneration. Every patient’s vision, lifestyle, and expectations are different, so it’s essential that your surgeon clearly understands what you hope to achieve. This conversation helps ensure that the surgical plan is tailored to your specific needs and retinal condition.
I always encourage patients to speak openly about their visual goals, daily challenges, and any concerns they may have about the procedure. For example, some people prioritise reading or using digital devices, while others focus more on improving distance vision for driving or outdoor activities. Understanding these priorities helps guide decisions about lens selection and overall treatment planning.
When expectations are discussed honestly from the beginning, patients tend to feel more confident and prepared. It also reduces the likelihood of disappointment after surgery because both the patient and surgeon share a clear understanding of the possible outcomes. This collaborative approach ultimately leads to better satisfaction and a smoother overall experience.
Combined Procedures
In certain situations, RLE surgery may be combined with other eye treatments to achieve the best possible visual outcome. This approach is usually considered when a patient has more than one eye condition that needs attention. By planning procedures together, surgeons can sometimes address multiple issues while reducing the overall number of surgical interventions.
For example, RLE may be coordinated with treatments such as retinal laser therapy or early cataract removal if these conditions are already affecting the eye. Carefully timing these procedures helps ensure that the retina remains stable while vision correction is performed. However, the decision to combine treatments always depends on the patient’s overall eye health and the stage of their retinal condition.
I always explain to patients that combined procedures require detailed planning and close collaboration between specialists. The goal is not simply to improve vision quickly, but to protect long-term eye health while achieving the safest outcome. Because every patient’s situation is different, the treatment plan is always highly individualised and carefully tailored.
When RLE Might Not Be Advisable
In certain situations, RLE surgery may be combined with other eye treatments to achieve the best possible visual outcome. This approach is usually considered when a patient has more than one eye condition that needs medical attention. By carefully coordinating procedures, surgeons can sometimes address multiple issues in a single treatment plan. This can also reduce the need for several separate surgeries over time.
For instance, RLE may be scheduled alongside treatments such as retinal laser therapy or early cataract removal if these conditions are already affecting the eye. Proper timing is extremely important because the retina needs to remain stable while vision correction is carried out. When the procedures are planned thoughtfully, it can support both visual improvement and retinal health. However, the decision to combine treatments always depends on the patient’s overall eye condition and the stage of their retinal disease.
I always explain to patients that combined procedures require detailed planning and close coordination between different eye specialists. The goal is not simply to improve vision quickly, but to protect the long-term health of the eye. Careful preparation helps reduce risks and ensures that each step of the treatment supports the next. Because every patient’s situation is unique, the final surgical plan is always personalised and thoughtfully tailored.
Choosing a Specialist Centre
Choosing the right specialist centre is a crucial step when considering RLE surgery, especially if you have macular degeneration. This type of case requires expertise not only in lens replacement surgery but also in understanding retinal diseases. An experienced team can carefully evaluate your eye health and design a treatment plan that prioritises both vision improvement and retinal safety.
I always recommend selecting a clinic where surgeons regularly manage patients with complex eye conditions. Centres with advanced diagnostic technology and strong collaboration between cataract and retinal specialists are better equipped to handle the unique challenges that macular degeneration presents. This level of expertise helps ensure that every stage of the process, from assessment to recovery, is managed with precision.
Specialist clinics such as the London Cataract Centre focus on providing personalised care for patients considering refractive lens exchange in London. Their experience with both RLE and retinal conditions allows them to create tailored treatment plans that support long-term eye health. Choosing a centre with this level of expertise can make a significant difference in both safety and overall visual outcomes.
FAQs:
1. Can you have RLE surgery if you have macular degeneration?
Yes, some patients with macular degeneration can still undergo RLE surgery, but eligibility depends on the stage and stability of the retinal condition. Your ophthalmologist will carefully assess the health of your macula using retinal imaging before recommending surgery. If the disease is mild or stable, RLE may help correct refractive errors and reduce dependence on glasses. However, the procedure cannot repair existing retinal damage, so expectations must remain realistic.
2. Does RLE surgery treat macular degeneration?
No, RLE does not treat or cure macular degeneration. The surgery replaces the natural lens with an artificial intraocular lens to correct refractive issues such as presbyopia or long-sightedness. While this can improve overall clarity of vision, it does not affect the retinal damage caused by AMD. Patients should view RLE as a way to optimise their remaining vision rather than a treatment for the disease itself.
3. What tests are needed before RLE if you have macular degeneration?
Before surgery, a detailed retinal evaluation is essential. Your ophthalmologist will typically perform optical coherence tomography (OCT) scans to assess the macula, along with fundus photography and visual acuity testing. These tests help identify fluid, scarring, or retinal thinning that could affect surgical outcomes. The results guide both surgical planning and realistic expectations about the potential benefits of RLE.
4. Can RLE improve vision for patients with AMD?
RLE can improve vision in certain ways for AMD patients, particularly by correcting refractive errors that affect overall clarity. Patients may experience sharper peripheral vision and less dependence on glasses. However, if the macula is significantly damaged, improvements in central vision may be limited. The main goal is often to maximise remaining vision rather than restore vision that has already been lost.
5. Which intraocular lens is best for patients with macular degeneration?
Monofocal lenses are usually the safest and most suitable choice for AMD patients. These lenses provide clear vision at one distance and preserve contrast sensitivity, which is important for eyes affected by retinal disease. Multifocal lenses are typically avoided because they split incoming light, which can reduce contrast and make visual tasks more difficult. A personalised lens selection process ensures the best balance between clarity and comfort.
6. Can RLE surgery worsen macular degeneration?
RLE surgery does not directly worsen macular degeneration, but careful monitoring is still required. Some patients may experience temporary retinal swelling after surgery, known as cystoid macular oedema, which can affect vision temporarily. This complication is usually treatable with medication. Regular follow-up appointments allow your surgeon to detect and manage any retinal changes early.
7. Can RLE be performed if you are receiving injections for wet AMD?
Yes, RLE can sometimes be performed in patients receiving anti-VEGF injections for wet AMD. However, the procedure must be carefully timed around the injection schedule. Surgeons often coordinate with retinal specialists to ensure the macula is stable before proceeding. This collaborative approach helps maintain retinal health while allowing the benefits of lens replacement surgery.
8. Will RLE help with reading if you have macular degeneration?
RLE may improve overall visual clarity, but reading small print can still be challenging if the macula is damaged. Since central vision is responsible for fine detail, retinal changes may limit reading ability even after successful surgery. Many patients continue using magnifiers, enhanced lighting, or digital visual aids to assist with detailed tasks. Combining RLE with low vision tools often provides the best results.
9. How important is post-operative monitoring for AMD patients?
Post-operative monitoring is extremely important for patients with macular degeneration. Follow-up appointments allow your surgeon to check healing progress and ensure the retina remains stable after surgery. OCT scans may be repeated to monitor the macula for any signs of swelling or disease progression. Regular retinal care remains essential because RLE does not stop AMD from progressing.
10. What are realistic expectations for RLE surgery in AMD patients?
Patients with macular degeneration should expect improvements mainly in overall visual clarity and reduced dependence on glasses. However, the surgery cannot restore vision that has already been lost due to macular damage. The goal is to maximise functional vision and improve daily comfort rather than achieve perfect eyesight. Clear communication with your surgeon ensures expectations align with the health of your retina.
Final Thoughts: Making an Informed Decision About RLE with Macular Degeneration
Living with macular degeneration does not automatically rule out the possibility of RLE surgery, but it does mean that the decision must be made with careful consideration. A detailed retinal assessment, realistic expectations, and thoughtful lens selection are all essential parts of ensuring that the procedure is both safe and beneficial. When the macula is stable and the treatment plan is tailored to your individual eye health, RLE can still offer meaningful improvements in overall visual clarity and daily comfort.
It’s important to remember that RLE is designed to correct refractive errors rather than treat macular degeneration itself. While the procedure may reduce dependence on glasses and improve certain aspects of vision, ongoing retinal care and monitoring remain crucial. Working closely with an experienced ophthalmologist ensures that every stage from assessment to recovery is carefully managed with your long-term eye health in mind. If you’re thinking about refractive lens exchange in London, you can get in touch with us at London Cataract Centre.
References:
- Nagyova, D., Tappeiner, C., Blaha, A., Goldblum, D. & Kyroudis, D. (2025). Visual Outcomes and Patient Satisfaction with Extended Monovision An Innovative Strategy to Achieve Spectacle Independence in Refractive Lens Exchange. Journal of Clinical Medicine. https://www.mdpi.com/2077-0383/14/16/5684
- Chang, J.S.M., Ng, J.C.M., Chan, V.K.C. & Law, A.K.P. (2014). Visual outcomes and patient satisfaction after refractive lens exchange with a single-piece diffractive multifocal intraocular lens. https://pubmed.ncbi.nlm.nih.gov/25505974/
- Grzybowski, A., Kanclerz, P. & Tuuminen, R. (2015) Refractive lens exchange in modern practice: when and when not to do it? Graefe’s Archive for Clinical and Experimental Ophthalmology https://pmc.ncbi.nlm.nih.gov/articles/PMC4655463/
- Fernández-Vega, L., Alfonso, J.F. & Baamonde, M.B. (2019) Incidence of intraoperative and early postoperative adverse events in a large cohort of consecutive refractive lens exchange procedures. American Journal of Ophthalmology https://www.sciencedirect.com/science/article/abs/pii/S0002939419304465
- Auffarth, G.U., Dick, H.B. & Schultz, T. (2024) Refractive lens exchange the evidence behind the practice. https://pmc.ncbi.nlm.nih.gov/articles/PMC11751179/