Ocular dominance is one of those invisible factors that can make or break lens replacement outcomes. Many patients assume their eyes contribute equally to vision, but the brain naturally prioritises input from one eye. Ignoring this can turn an otherwise technically perfect surgery into a source of frustration, with blurred near vision, headaches, or prolonged adaptation. Understanding dominance upfront is not optional it’s central to predictable results.
I see patients frequently underestimate its impact. Monovision strategies fail, multifocal lenses underperform, and neural adaptation takes longer when dominance is overlooked. It’s not about “better” or “stronger” eyes it’s about how the brain integrates information. Mapping dominance early gives you control over lens selection and sets expectations that align with your lifestyle and visual goals.
Dominance affects both short-term clarity and long-term satisfaction. The dominant eye usually drives distance vision, while the non-dominant eye adapts more easily to near tasks. Even minor misalignment or misassignment can compromise depth perception, reading comfort, and overall functional independence from spectacles. Proper testing transforms these potential pitfalls into predictable outcomes.
Modern assessment tools make this evaluation straightforward. Sensory tests, motor checks, and binocular vision assessments provide a clear picture of which eye should prioritise distance or near vision. Incorporating these results into surgical planning allows for tailored monovision, multifocal placement, or extended depth-of-focus strategies. Patients who engage with this process adapt faster and report higher satisfaction than those who skip it.
Why Ocular Dominance Matters
You may assume both eyes contribute equally, but the brain actually prioritises input from one eye over the other. This plays a critical role in lens selection, monovision planning, and overall satisfaction after surgery. Ignoring ocular dominance can compromise both functional outcomes and the adaptation process.
Many patients underestimate its importance. Without recognising which eye is dominant, monovision assignments can be reversed, multifocal lenses may not perform optimally, and neural adaptation can take longer than expected. Ocular dominance isn’t about “stronger” eyes it’s about how your brain processes visual information.
It affects both immediate and long-term results. The dominant eye typically drives distance vision, while the non-dominant eye adjusts more easily to near or intermediate correction. Accounting for dominance ensures that even technically perfect surgery translates into practical, everyday visual performance.
Types of Ocular Dominance
Ocular dominance isn’t a single trait it’s a combination of sensory and motor factors that shape how we perceive the world. Sensory dominance dictates which eye provides clearer, more reliable input to the brain, while motor dominance influences alignment and fixation. Most patients exhibit a mix of both, and recognising that blend is crucial for precise lens placement and visual comfort.
- Sensory dominance assessment: This identifies which eye contributes sharper, more accurate images to the brain. I rely on binocular tests to detect subtle differences in clarity and preference. Neglecting sensory dominance can cause strain or blur despite perfectly aligned lenses.
- Motor dominance evaluation: Motor dominance governs fixation and alignment during tasks requiring coordinated eye movement. Simple pointing exercises and tracking tests reveal which eye leads in motion. Ignoring this can result in discomfort or adaptation issues post-surgery.
- Practical testing methods: The “hole-in-the-card” test, combined with pointing tasks and binocular assessments, provides a comprehensive picture of dominance. Each method uncovers different aspects of how the brain prioritises visual input. Together, they guide lens placement decisions that feel natural to the patient.
- Implications for surgical outcomes: Correctly identifying dominance reduces headaches, eye strain, and blurred near vision. Even technically perfect lens implantation can fail if dominance isn’t considered. Early identification ensures post-operative comfort and higher patient satisfaction.
Understanding ocular dominance is more than a clinical formality it’s a roadmap for visual comfort and functional outcomes. Sensory and motor insights guide lens selection and placement, preventing subtle but persistent post-operative issues. When dominance is assessed and integrated into planning, surgery aligns with both anatomy and natural brain processing. The result is smoother adaptation, reduced strain, and a more satisfying visual experience.
Ocular Dominance and Monovision
You need to understand that monovision success depends heavily on ocular dominance. Assigning the dominant eye for distance vision and the non-dominant eye for near vision is essential for smooth neural adaptation. Reversing this setup often causes blurred vision, depth perception problems, and frustration.
I always trial monovision using contact lenses before surgery. This gives you a real sense of how your brain adapts to unequal focus between eyes. Trials are especially important for patients with weak or mixed dominance, where adaptation is less predictable and outcomes can vary.
Strong dominance generally leads to easier adaptation, while weak dominance may require more careful planning. In such cases, we discuss tailored lens powers or consider alternatives like extended depth-of-focus lenses. Personalising lens selection this way reduces post-operative challenges and improves satisfaction.
Multifocal Lenses and Dominance
You need to remember that ocular dominance remains crucial even when using multifocal lenses. The brain naturally prioritises input from the dominant eye, influencing how clearly you see at near, intermediate, and distance tasks. If this is ignored, uneven focus, visual disturbances, or longer adaptation periods can occur, leaving you frustrated despite technically successful surgery.
I carefully adjust lens power and positioning to match the dominant eye’s neural preference. This ensures your brain can integrate multiple focal points smoothly, reducing common issues such as halos, glare, or blur. Patients notice a clearer, more consistent experience when performing daily activities, from reading to driving in varying light conditions.
Dominance-informed multifocal strategies consistently deliver higher satisfaction than generic lens placement. By tailoring the lenses to your brain’s natural preference, adaptation is faster and functional recovery is smoother. This approach maximises the technology’s potential, making your vision feel natural rather than artificial, and ensures you enjoy the full benefits of surgery in everyday life.
Testing Protocols in Surgical Planning
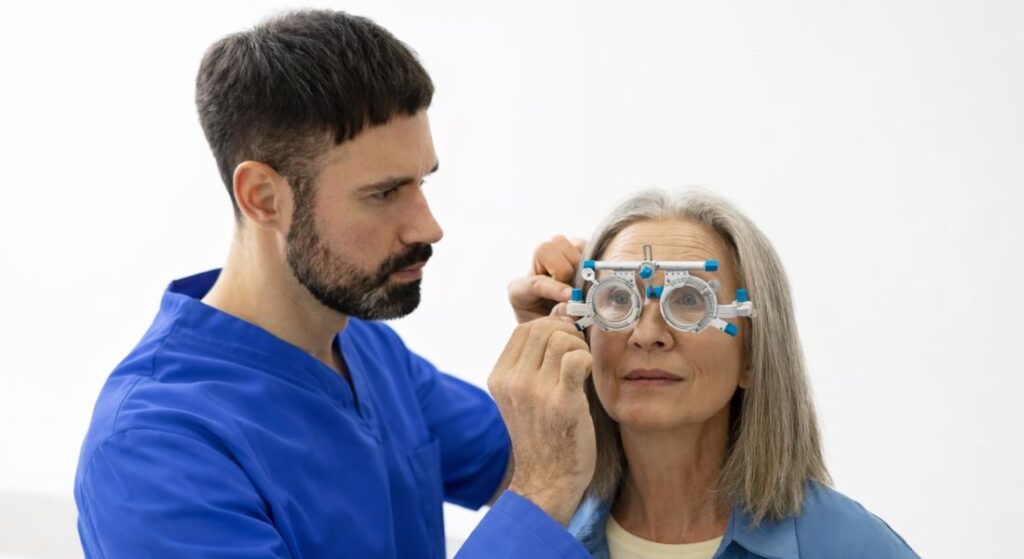
You need a thorough ocular dominance assessment before any lens replacement procedure. Sensory and motor evaluations, often supported by imaging or binocular vision analysis, provide a complete picture of which eye naturally leads. This information is critical for planning the procedure effectively.
The results directly influence key surgical decisions. They determine which eye should receive distance correction, whether monovision is appropriate, and if multifocal lenses require modification. Ignoring this step can lead to avoidable issues such as needing post-operative enhancements, relying on spectacles, or facing longer adaptation periods.
Following a structured testing protocol ensures your surgery is personalised from the outset. It minimises surprises and sets realistic expectations, giving you a smoother path to functional independence from reading glasses. Being meticulous at this stage is often what separates satisfactory outcomes from truly excellent ones.
Patient Education
Many patients underestimate how ocular dominance influences surgical outcomes. I dedicate time to explaining how the brain prioritises input, why certain lenses are chosen, and what adaptation timelines look like. This understanding isn’t just academic it shapes expectations, encourages compliance, and reduces anxiety before and after surgery.
- Explaining neural prioritisation: Patients gain insight into why one eye naturally leads in processing visual information. When they understand this, they are less likely to misinterpret temporary blur or adaptation difficulties as complications. Clarity here improves confidence and patience during recovery.
- Rationale behind lens selection: Walking patients through why a specific lens is chosen monofocal, multifocal, or extended depth-of-focus anchors decisions in their lifestyle needs. This transparency strengthens trust and reduces surprise or disappointment post-surgery. Patients can see the logic behind technical choices.
- Trial monovision sessions: Using contact lenses to simulate monovision allows patients to experience dominance effects firsthand. This practical trial reveals how one eye will focus at distance while the other handles near vision. Experiencing it in advance increases adaptability and reduces post-operative discomfort.
- Setting realistic expectations: Understanding the science behind the procedure prevents unrealistic assumptions about instant perfection. Patients who grasp adaptation timelines are more cooperative and less likely to panic over minor transitional visual changes. Education directly translates to higher satisfaction and smoother recovery.
Patient education transforms surgery from a passive experience into an informed partnership. By explaining dominance, lens choice, and adaptation, patients are better prepared mentally and practically. Trials and discussions reduce post-operative friction and build confidence. When patients truly understand the process, compliance improves, anxiety drops, and the final visual outcome is far more predictable.
Post-Operative Adaptation
You need to recognise that adaptation is a crucial phase, even when planning and surgery are flawless. Your brain requires time to integrate different focal lengths between eyes, especially with monovision or multifocal lenses. Patients who understand this process tend to be more patient and actively follow the exercises I recommend, which improves outcomes.
Neural adaptation strategies include alternating focus between near and distance tasks, adjusting reading distance, and optimising lighting conditions. These simple adjustments help your visual system recalibrate more efficiently.
It’s important to remember that adaptation is highly individual. Ocular dominance plays a major role in how quickly and comfortably your brain adjusts. Recognising this early helps you set realistic expectations and avoid frustration during the recovery period.
Lifestyle Considerations
You need to recognise that successful lens replacement is about more than anatomy—it has to fit your daily life. How you read, use screens, drive, or engage in hobbies directly affects which eye should be prioritised for distance or near vision. Ignoring these factors can result in technically successful surgery that doesn’t feel practical in everyday tasks.
I combine ocular dominance testing with lifestyle mapping to guide lens placement. This approach allows me to tailor the procedure so that your vision supports the activities you perform most frequently. By integrating these insights, the surgery becomes personalised rather than generic.
For example, a graphic designer may need precise intermediate vision for screen work, while a writer reading small print may prioritise near clarity. Aligning lens choice with both dominance and lifestyle ensures outcomes that are functional and practical, rather than chasing a theoretical “perfect” result. Patients consistently report higher satisfaction when their new vision fits seamlessly into daily life.
Common Mistakes Related to Dominance
Ocular dominance is subtle, and errors in recognising it is a frequent source of post-operative dissatisfaction. Many patients and even some clinicians assume both eyes contribute equally, which can misguide lens selection. Awareness of typical pitfalls allows for structured assessment and personalised planning, reducing the risk of avoidable complications and enhancing overall satisfaction.
- Assuming equal contribution from both eyes: Believing both eyes function identically often leads to incorrect monovision assignments. This mismatch can cause blurred vision, discomfort, or difficulty with depth perception. Accurate dominance mapping prevents these issues and aligns expectations with real visual behaviour.
- Skipping dominance testing: Pressure to streamline pre-op assessments or overreliance on technology can result in skipped tests. Omitting evaluation leaves lens placement decisions uninformed, increasing adaptation challenges post-surgery. Simple, reliable tests ensure decisions are evidence-based rather than assumed.
- Ignoring mixed or weak dominance: Some patients do not have a clear dominant eye, or dominance may vary by task. In these cases, staged trials or alternative lens strategies are essential. Overlooking this nuance can lead to ongoing visual strain and dissatisfaction.
- Overestimating patient adaptation: Not all individuals adjust naturally to monovision or multifocal setups. Assuming universal adaptability without guided exercises can result in persistent headaches, eye strain, or functional compromise. Structured adaptation plans improve tolerance and comfort.
Avoiding dominance-related mistakes is critical for smooth surgical outcomes. Thorough testing, personalised lens selection, and realistic adaptation planning transform potential pitfalls into predictable results. When these errors are actively addressed, patients experience fewer complications, greater comfort, and a higher likelihood of achieving the visual independence they sought. Consistency in these steps is what separates standard outcomes from optimised ones.
Long-Term Monitoring
You need to recognise that ocular dominance continues to matter well after surgery. Capsular shifts, subtle refractive changes, or issues with the ocular surface can influence how your eyes work together. Routine monitoring allows me to check that the dominant eye is still leading effectively and intervene before small problems affect daily vision.
Minor enhancements, such as laser touch-ups or temporary spectacles, can be guided by dominance to maximise effectiveness. Targeting adjustments this way preserves functional independence from reading glasses.
By combining careful long-term monitoring with proactive refinements, you maintain surgical gains and ensure satisfaction lasts. This approach keeps your vision stable, predictable, and aligned with your lifestyle for years to come.
Mixed or Crossed Dominance
You need to be aware that some patients have mixed or crossed dominance, where sensory and motor dominance do not align. These cases are more complex and demand careful planning and pre-operative assessment. Trial sessions with contact lenses are invaluable for determining which eye is best suited for distance or near correction.
Without this tailored approach, adaptation can take longer, and issues like headaches or persistent visual discomfort may arise. Patients with mixed dominance are particularly sensitive to incorrect assignments, making personalised planning essential.
Correctly identifying and accounting for mixed or crossed dominance ensures more predictable outcomes. By addressing these nuances early, you reduce frustration and maximise functional independence from reading glasses.
Psychological Impact
You need to recognise that understanding ocular dominance affects more than just vision it influences confidence and adaptation. Patients who know which eye is dominant and why a specific lens plan is chosen feel more in control and adjust more quickly. This knowledge reduces uncertainty and supports a smoother recovery.
Conversely, patients unaware of how dominance shapes outcomes often experience anxiety and frustration, even when the surgery itself is technically successful. Misunderstanding these factors can lower satisfaction and make normal adaptation feel like a problem.
Education and active engagement during planning are just as important as surgical skill. Taking the time to explain dominance, lens choices, and expected visual adaptation helps patients feel empowered and more likely to achieve lasting independence from reading glasses.
The Role of Technology
You need to appreciate that technology enhances every stage of dominance-informed surgical planning. AI-driven imaging, wavefront analysis, and binocular visual assessments provide objective confirmation of subjective dominance tests. This allows for precise lens selection and placement tailored to your eyes and how your brain processes visual input. Using these tools reduces guesswork and ensures the plan aligns closely with your lifestyle and visual priorities.
Post-operatively, technology continues to play a crucial role. Subtle misalignments, early neural adaptation issues, or minor refractive changes can be detected before they impact functional vision. Early detection allows timely adjustments, whether through laser enhancements, minor lens tweaks, or temporary corrective aids, improving recovery speed and overall satisfaction.
Integrating advanced diagnostic and monitoring tools with clinical expertise makes dominance-informed planning far more predictable. It ensures that surgery, lens performance, and neural adaptation work in harmony, delivering reliable vision that supports reading, screen use, driving, and other everyday tasks. This approach maximises the chances of sustained independence from reading glasses.
Financial and Procedural Implications
You need to understand that ignoring ocular dominance can have real financial and procedural consequences. Mistakes in eye assignment often lead to additional enhancements, extended recovery, or reliance on spectacles, increasing both cost and inconvenience. Proper testing upfront ensures the correct eye receives distance or near correction, minimising these risks.
Transparent discussion about these implications is essential. Patients who understand the value of pre-operative dominance assessment and trial sessions are more prepared for potential costs and adjustments. This clarity helps you make informed decisions rather than facing unexpected procedures later.
Planning around ocular dominance is not just a clinical step it’s an investment in long-term satisfaction. Taking the time to assess and integrate dominance properly maximises the likelihood of functional independence from reading glasses and reduces frustration over the years.
FAQs:
1. What is ocular dominance and why does it matter for lens surgery?
Ocular dominance refers to the brain’s preference for visual input from one eye. It guides lens placement, monovision planning, and adaptation, directly affecting post-operative comfort and satisfaction.
2. How is ocular dominance tested before surgery?
Tests include sensory assessments, motor evaluations, and binocular vision checks. Simple methods like the “hole-in-the-card” test, combined with pointing and tracking exercises, give a reliable picture of dominance.
3. How does dominance affect monovision outcomes?
Assigning the dominant eye for distance and the non-dominant eye for near tasks is essential. Reversing this can cause blurred vision, headaches, and poor adaptation.
4. Does ocular dominance influence multifocal lens performance?
Yes. The brain prioritises input from the dominant eye, impacting near, intermediate, and distance clarity. Tailored lens placement based on dominance improves neural adaptation and reduces glare or halos.
5. What about patients with weak or mixed dominance?
They may require trial monovision with contact lenses or customised lens powers. Careful planning ensures smoother adaptation and higher satisfaction.
6. How does lifestyle factor into dominance-based planning?
Reading habits, screen use, hobbies, and driving determine which eye should prioritise distance or near vision. Aligning lens selection with daily activities ensures practical, functional outcomes.
7. Can dominance change over time or after surgery?
Minor shifts in capsular position, refraction, or ocular surface can influence dominance. Routine monitoring helps maintain functional independence from reading glasses.
8. What are the risks of ignoring ocular dominance?
Skipping dominance testing or assuming both eyes contribute equally can lead to incorrect lens assignments, prolonged adaptation, visual strain, or the need for post-operative enhancements.
9. How does patient education improve outcomes?
Explaining dominance, lens choice, and adaptation timelines empowers patients. Understanding the process reduces anxiety, ensures compliance, and improves functional independence.
10. Does technology help with dominance-informed planning?
Advanced imaging, wavefront analysis, and binocular assessments enhance accuracy. Technology supports precise lens placement, detects early adaptation issues, and allows timely refinements for optimal results.
Final Thoughts: Why Ocular Dominance Matters for Lasting Visual Success
Understanding ocular dominance isn’t a technical extra it’s central to achieving predictable, comfortable outcomes from lens replacement. Mapping which eye your brain prioritises, tailoring monovision or multifocal placement accordingly, and combining this with lifestyle considerations transforms surgery from a standard procedure into a personalised solution. Patients who skip these steps often face longer adaptation, visual strain, or disappointment despite technically successful surgery.
Long-term satisfaction depends on more than the operation itself. Structured testing, trial monovision sessions, education, and careful follow-up ensure neural adaptation proceeds smoothly and functional independence is maintained. Technology aids precision, but patient engagement and realistic expectations remain critical. If you’re thinking about Lens Surgery in London, you can get in touch with us at London Cataract Centre. Engage early, plan meticulously, and maximise your chances of lasting, comfortable vision.
References:
- Handa, T., Mukuno, K., Uozato, H., Niida, T., Shoji, N., Minei, R., Nitta, M. and Shimizu, K. (2004) Ocular dominance and patient satisfaction after monovision induced by intraocular lens implantation. Journal of Cataract & Refractive Surgery https://pubmed.ncbi.nlm.nih.gov/15093637/
- Zheleznyak, L., Alarcon, A., Dieter, K.C., Tadin, D. and Yoon, G. (2015) The role of sensory ocular dominance on through‑focus visual performance in monovision presbyopia corrections. https://pmc.ncbi.nlm.nih.gov/articles/PMC4461890/
- Schwartz, R. and Yatziv, Y. (2015) The effect of cataract surgery on ocular dominance. Clinical Ophthalmology https://pmc.ncbi.nlm.nih.gov/articles/PMC4686333/
- Fawcett, S.L., Gonçalves, R. and Hurwitz, J.A. (2005) Effects of ocular dominance on binocular summation after monocular reading adds. Journal of Cataract & Refractive Surgery https://www.sciencedirect.com/science/article/abs/pii/S0886335005001677
- Kim, S.J., Park, C.Y. and Lim, D.J. (2026) Factors Affecting Postoperative Satisfaction After Presbyopia‑Correcting Intraocular Lens Surgery. Journal of Clinical Medicine, https://www.mdpi.com/2077-0383/15/1/336

