For patients with macular degeneration, lens replacement surgery requires careful planning because the macula the central portion of the retina is essential for sharp, detailed vision. Any damage to this area can affect how much benefit you gain from surgery, making a thorough retinal assessment a crucial first step. Understanding the health of your macula helps set realistic expectations for visual improvement.
Lens replacement, also called refractive lens exchange or cataract surgery, involves removing your natural lens and implanting a clear artificial intraocular lens (IOL). This procedure can correct cataracts, presbyopia, or other refractive errors. However, the presence of macular degeneration adds complexity, as the surgery cannot reverse retinal damage or restore vision lost from the disease. The aim is to improve clarity and comfort while safeguarding the remaining central vision.
Several factors influence surgical outcomes, including the type and stage of macular degeneration, the overall health of your eye, and the specific lens chosen. Early or stable cases often benefit most, whereas advanced degeneration may limit the potential gains. Discussing your visual goals and understanding the realistic results is essential for planning the procedure.
A personalised approach ensures both safety and effectiveness. Your ophthalmologist will carefully evaluate your retina, discuss lens options, and tailor the surgery to your eye’s specific needs. With proper assessment, planning, and follow-up care, many patients with macular degeneration can safely undergo lens replacement and achieve meaningful improvements in vision and quality of life.
Understanding Macular Degeneration
Macular degeneration affects the macula, the central part of the retina responsible for sharp, detailed vision. This area allows you to read, recognise faces, and see fine details clearly, which makes understanding your retinal health essential before considering lens surgery.
There are two main types: dry (atrophic) and wet (neovascular). Dry AMD progresses slowly and often allows for more predictable surgical outcomes, whereas wet AMD can cause rapid changes in central vision, requiring careful monitoring and treatment coordination before surgery. Identifying the type is a critical first step in planning lens replacement.
The stage of the disease also influences potential benefits. Early-stage AMD may permit meaningful improvements in vision after surgery, while advanced disease can limit the gains. Knowing both the type and severity helps set realistic expectations and allows your surgeon to tailor the procedure for the safest and most effective outcome.
How Lens Replacement Works
Lens replacement surgery works by removing your natural lens and implanting a clear artificial intraocular lens (IOL). This procedure can correct refractive errors, reduce glare, and restore sharper vision, depending on the overall health of the eye. Modern techniques are minimally invasive, using tiny incisions that often heal without stitches, allowing for a faster recovery and improved visual comfort.
For patients with macular degeneration, it’s important to understand that the surgery cannot reverse damage to the retina. The procedure focuses on improving the clarity of the visual pathway so the remaining healthy retinal tissue can function as effectively as possible. Clearer optics can make the most of your central vision and may enhance the perception of colour and contrast, even if some retinal cells are compromised.
By optimising what the retina can see, lens replacement helps maximise visual potential and comfort. While it doesn’t cure macular degeneration, it can make everyday tasks like reading, recognising faces, and navigating your environment easier. Combined with careful retinal monitoring and management, lens replacement can significantly improve quality of life for patients with stable or early-stage macular degeneration.
Retinal Evaluation Before Surgery
A thorough retinal assessment is a critical step before recommending lens replacement surgery, especially for patients with conditions such as age-related macular degeneration (AMD). The retina’s health directly impacts both the safety of surgery and the potential visual outcomes. By performing detailed imaging and evaluations, the surgeon can make informed decisions about whether surgery is appropriate and which type of lens will provide the best results. This careful planning helps ensure optimal outcomes while minimising risks.
- Optical Coherence Tomography (OCT): OCT provides high-resolution, cross-sectional images of the retina, allowing detailed examination of the macula and optic nerve. This imaging helps detect subtle changes in retinal structure that could affect surgical safety or visual results.
- Fundus Photography: Fundus photographs capture detailed images of the retina, documenting its current state. These images allow the surgeon to track changes over time and plan the procedure based on the health of the macula and surrounding tissues.
- Other Imaging Techniques: Additional tests may be used to assess retinal thickness, blood flow, or other structural features. Combining multiple imaging methods provides a comprehensive view of retinal health, helping identify any risks or complications before surgery.
- Guiding Lens Selection and Surgical Planning: Understanding the condition of the retina is essential for selecting the most appropriate intraocular lens (IOL). For AMD patients, this evaluation ensures that the chosen lens supports the best possible vision without compromising retinal health.
In conclusion, retinal evaluation is a vital part of pre-operative planning for lens replacement surgery. Through OCT, fundus photography, and other imaging techniques, the surgeon can assess retinal health, guide lens selection, and determine the safety and likely outcomes of the procedure. Careful assessment ensures personalised surgical planning and maximises the chances of achieving optimal vision for patients with AMD or other retinal conditions.
Setting Realistic Expectations
Setting realistic expectations is a crucial part of preparing for lens replacement surgery, particularly for patients with macular degeneration. While the procedure can improve overall clarity, reduce glare, and correct refractive errors, it cannot restore vision that has already been lost due to retinal damage. Understanding this distinction early helps patients approach surgery with a clear and informed mindset.
I always emphasise that the primary goal is to maximise the potential of remaining healthy retinal tissue. Lens replacement can reduce dependence on glasses, improve peripheral vision, and enhance visual comfort, even if perfect central vision is no longer achievable. These improvements can make everyday tasks like reading, recognising faces, and navigating your environment easier and less tiring.
Having a thorough discussion about realistic outcomes helps patients set appropriate expectations and feel more confident about the procedure. When patients understand both the benefits and the limitations, they are more likely to appreciate the improvements in daily visual function and feel satisfied with their results, even if certain central vision challenges remain.
Lens Options for AMD Patients
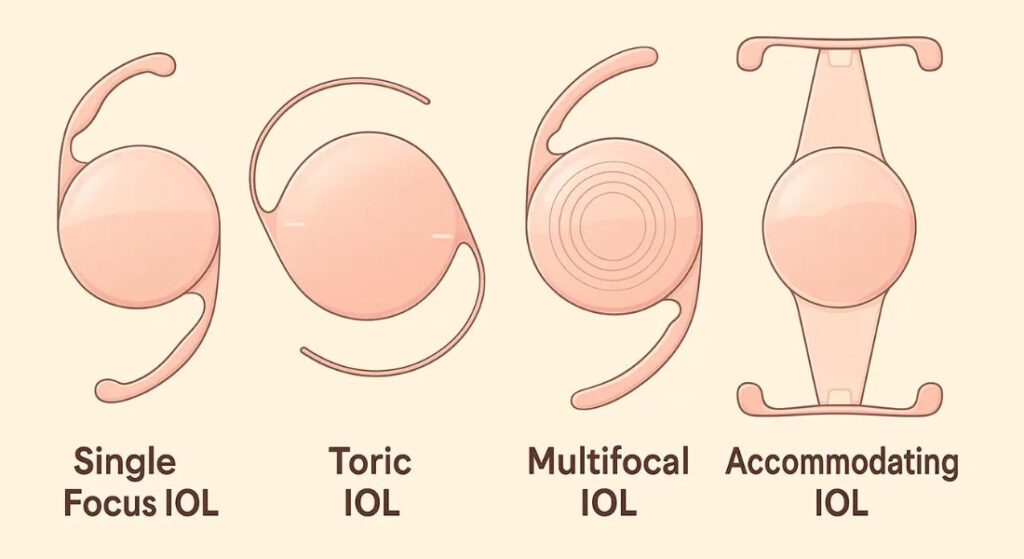
Not all intraocular lenses (IOLs) are suitable for patients with macular degeneration. Multifocal lenses, while popular for reducing dependence on glasses, can decrease contrast sensitivity, which may be problematic when the macula is already compromised. This could make reading or recognising fine details more difficult for patients with retinal damage.
For many AMD patients, monofocal lenses are the preferred option. These lenses provide clear and predictable distance vision, reduce visual strain, and preserve contrast, making them safer and more effective for individuals with central retinal impairment.
The choice of lens is always personalised. I take into account your visual goals, lifestyle needs, and the health of your retina to recommend the lens that maximises functional vision while minimising potential complications.
Impact on Daily Activities
Lens replacement can significantly improve overall vision, but patients with macular degeneration may still need magnification aids or specialised tools for reading, detailed work, or hobbies that require fine vision. I make a point of discussing how the surgery can enhance everyday activities while being honest about the limitations that may persist due to retinal damage.
Even modest gains in clarity, contrast, and visual sharpness can make a meaningful difference. Tasks such as watching television, recognising faces, navigating unfamiliar environments, and performing household chores often become easier, safer, and less tiring. Improved peripheral vision and reduced glare can also contribute to greater comfort and independence in daily life.
Understanding both the benefits and the ongoing challenges allows patients to approach lens replacement with realistic expectations. This perspective helps them make the most of the visual improvements, plan for any additional aids or strategies they may need, and maintain confidence in managing their vision over the long term.
Timing the Surgery
The timing of lens replacement surgery is a crucial factor in achieving the best outcomes, particularly for patients with age-related macular degeneration (AMD). Performing surgery when the retina is stable reduces potential risks and increases the likelihood of improved vision. If the macular degeneration is actively progressing, it is usually safer to stabilise the retinal condition before proceeding with surgery. Thoughtful scheduling helps balance safety with the potential benefits of the procedure.
- Surgery During Disease Stability: Lens replacement is safest when retinal disease is stable. Stable retinal health reduces the risk of complications and ensures that the visual improvements from surgery are not compromised by ongoing degeneration.
- Avoiding Surgery During Active Progression: If AMD or other retinal conditions are actively worsening, surgery may be postponed. Intervening during active disease could increase the risk of poor outcomes or complicate post-operative recovery.
- Optimising Visual Benefit: Timing surgery correctly maximises the likelihood that the patient will experience meaningful improvements in vision. Stable retinal health allows the new lens to function effectively without interference from ongoing retinal changes.
- Coordinating with Retinal Treatments: In some cases, ongoing retinal therapy such as injections or laser treatment may need to be considered before surgery. Aligning lens replacement with retinal management ensures both treatments support long-term visual outcomes.
In conclusion, careful timing of lens replacement surgery is essential for patients with retinal conditions such as AMD. Performing the procedure during periods of stability minimises risks and maximises the visual benefits. Coordinating surgery with retinal treatment plans allows for safer, more effective outcomes and better long-term vision management.
Managing Expectations for Reading and Detail Work

Even with successful lens replacement, patients with macular degeneration may continue to experience limitations in central vision. This means that reading small print, performing detailed crafts, or carrying out precision tasks can remain challenging if the macula is affected. Being aware of these potential limitations before surgery helps patients form realistic expectations and plan accordingly.
I always discuss practical strategies to maximise the use of remaining vision. Enhanced lighting, high-quality magnifiers, electronic reading aids, and other specialised low vision tools can make everyday activities such as reading, writing, or hobbies much more manageable and comfortable.
By combining the improvements achieved through lens replacement with these adaptive strategies, patients can make the most of their visual potential. This integrated approach not only supports independence and confidence but also reduces frustration, helping patients maintain an active and fulfilling lifestyle despite ongoing central vision challenges.
Combining Surgery with Retinal Care
Patients with wet AMD often receive ongoing treatments such as anti-VEGF injections to manage fluid and prevent further retinal damage. Lens replacement surgery can still be performed safely in these patients, but careful planning and timing are essential to avoid interfering with their existing treatment schedule.
Collaboration between the retinal specialist and the lens surgeon is crucial. By coordinating appointments and monitoring the eye closely, we ensure that the retina remains stable while surgery is carried out, minimising risks and optimising visual outcomes.
This joint approach allows patients to benefit from lens replacement without compromising ongoing retinal therapy. It also provides peace of mind, knowing that both the lens and the retina are being managed together to achieve the safest and most effective results.
Monitoring After Surgery
Post-operative follow-up is a critical part of care after lens replacement surgery. Regular eye examinations allow the surgeon to monitor healing, detect any changes in the retina early, and ensure that visual recovery is progressing as expected. These visits also provide an opportunity to address any concerns or symptoms promptly.
Even after successful lens replacement, macular degeneration can continue to progress. Monitoring the retina closely helps identify new changes or complications at an early stage, allowing timely intervention to protect remaining vision.
Consistent follow-up not only safeguards the health of the eye but also helps patients maintain the best possible visual function. By combining surgical care with ongoing retinal monitoring, we can maximise quality of life and long-term outcomes for patients with macular degeneration.
Risks Specific to AMD Patients
Patients with age-related macular degeneration (AMD) face unique considerations when undergoing lens replacement surgery. The condition itself can increase the risk of certain post-operative complications, making careful planning and monitoring essential. Understanding these risks helps patients make informed decisions and prepares them to manage any issues that may arise during recovery. Open discussion with the surgeon ensures realistic expectations and better overall outcomes.
- Cystoid Macular Oedema (CMO): One of the most common post-operative risks in AMD patients is cystoid macular oedema, a swelling of the central retina that can temporarily reduce vision. Early detection and treatment with anti-inflammatory drops or other interventions often resolve the issue and restore visual clarity.
- Potential for Slower Visual Recovery: Due to underlying retinal damage, AMD patients may experience slower improvement in vision compared with those without retinal conditions. Recovery timelines should be discussed in advance to set realistic expectations.
- Increased Sensitivity to Surgical Stress: The macula in AMD patients may be more vulnerable to inflammation or trauma during surgery. Surgeons take additional precautions to minimise stress on the retina and reduce the risk of complications.
- Importance of Monitoring and Early Intervention: Close post-operative follow-up is crucial for detecting and managing any complications quickly. Prompt treatment of issues such as swelling or inflammation can prevent long-term vision problems and improve surgical outcomes.
In conclusion, AMD patients face specific risks during lens replacement surgery, including cystoid macular oedema and slower visual recovery. By discussing these risks openly and implementing careful monitoring, surgeons can minimise complications and ensure patients are well-prepared. Understanding the potential challenges allows patients to approach surgery with confidence and realistic expectations, ultimately supporting better outcomes.
Lifestyle Factors and Outcomes
Maintaining a healthy lifestyle plays an important role in supporting both retinal health and recovery after lens replacement surgery. Diets rich in antioxidants, leafy greens, and omega-3 fatty acids can help protect retinal cells, while staying active and managing blood pressure contributes to overall eye health.
Avoiding smoking is particularly critical, as tobacco use accelerates the progression of macular degeneration and can negatively affect healing after surgery. Staying hydrated and managing chronic conditions such as diabetes also supports optimal visual outcomes.
These lifestyle measures work alongside surgical intervention, helping patients maximise the benefits of lens replacement. By combining healthy habits with careful post-operative care, patients can protect their vision, enhance recovery, and maintain the improvements achieved through surgery over the long term.
Low Vision Support
Even after successful lens replacement, some patients continue to experience challenges with detailed vision due to macular degeneration. Low vision aids such as handheld magnifiers, electronic readers, or specialised lighting can help maximise the use of remaining vision for reading, hobbies, or daily tasks.
Incorporating these tools alongside surgical intervention allows patients to maintain independence and perform tasks that might otherwise be difficult. For many, even small enhancements in clarity and contrast can make a meaningful difference in everyday life.
By combining lens replacement with tailored low vision support, patients can significantly improve their quality of life. This integrated approach ensures that surgical benefits are fully leveraged while addressing ongoing visual limitations in a practical and empowering way.
Communication with Your Surgeon

Clear and open communication with your surgeon is essential for achieving the best possible outcomes in lens replacement surgery. Discussing your vision goals, daily challenges, and personal expectations helps the surgical team understand what matters most to you.
This dialogue allows the surgeon to personalise the procedure, select the most suitable lens, and design a post-operative plan tailored to your retinal health and lifestyle needs. It ensures that every aspect of care aligns with your visual priorities.
By sharing your concerns and objectives, you help maximise the benefits of surgery while setting realistic expectations. This collaborative approach fosters confidence, improves satisfaction, and supports the safest and most effective visual outcome despite the limitations imposed by macular degeneration.
When Lens Replacement Might Not Be Advisable
In cases of advanced macular degeneration where central vision is severely impaired, lens replacement may offer only limited visual improvement. Patients in this situation might find that the risks and recovery associated with surgery outweigh the potential benefits.
Non-surgical approaches, ongoing monitoring, and low vision aids can often provide safer and more practical ways to maintain independence and quality of life. These strategies help patients manage daily activities without the added stress of surgery.
Every decision regarding lens replacement must be personalised. By carefully weighing the potential for visual improvement against surgical risks and the natural progression of the disease, patients and surgeons can choose the approach that best supports long-term eye health and functional vision.
Choosing a Specialist Centre
Experience and specialised expertise are especially important when considering lens replacement for patients with macular degeneration. This procedure requires not only technical skill in performing lens surgery but also a thorough understanding of retinal disease and how it can influence visual outcomes. Surgeons must evaluate the stage of macular degeneration, the health of the macula, and the patient’s overall eye condition to plan a safe and effective procedure.
Specialist centres, such as the London Cataract Centre, provide personalised care tailored to each patient’s unique retinal health and vision goals. Their teams often work closely with retinal specialists, coordinating pre-operative assessments, lens selection, and post-operative monitoring to ensure that surgery complements ongoing retinal care and maximises visual potential.
By consulting an experienced centre, patients gain confidence that every step from detailed evaluation to recovery is carefully managed. This collaborative, expert approach helps patients achieve the best possible outcomes, reduces risks, and ensures that long-term retinal health remains a central focus throughout the lens replacement process.
FAQs:
1. Can I have lens replacement surgery if I have macular degeneration?
Yes, patients with stable or early-stage macular degeneration can often safely undergo lens replacement. The surgery can improve clarity and comfort, but it cannot reverse retinal damage.
2. Will lens replacement improve my central vision lost to macular degeneration?
Lens replacement cannot restore vision already lost from macular degeneration. Its goal is to maximise the potential of remaining healthy retinal tissue and enhance overall visual quality.
3. What pre-operative assessments are needed for AMD patients?
A thorough retinal evaluation, including Optical Coherence Tomography (OCT) and fundus photography, is essential. These tests assess the macula’s health and guide lens choice and surgical planning.
4. Which types of intraocular lenses (IOLs) are suitable for AMD patients?
Monofocal lenses are generally preferred because they preserve contrast and reduce visual strain. Multifocal lenses may decrease contrast sensitivity and are often unsuitable for eyes with macular damage.
5. How does the stage of macular degeneration affect surgery outcomes?
Early or stable AMD often allows meaningful visual improvement, while advanced disease may limit gains. Discussing realistic expectations with your surgeon is crucial for planning.
6. Can lens replacement be combined with ongoing retinal treatments?
Yes, with careful timing and coordination. For patients receiving anti-VEGF injections or other therapy, surgery can be scheduled to avoid interfering with ongoing treatment.
7. What risks are specific to AMD patients undergoing lens replacement?
Risks include cystoid macular oedema, slower visual recovery, and increased sensitivity to surgical stress. Close post-operative monitoring helps detect and manage complications early.
8. How will lens replacement affect daily activities?
Even with macular degeneration, improved clarity and contrast can make tasks like reading, recognising faces, and navigating environments easier. Low vision aids may still be helpful for detailed work.
9. When might lens replacement not be advisable for AMD?
In advanced cases with severe central vision loss, the surgery may offer limited benefit. Non-surgical options, ongoing monitoring, and low vision support might be more practical.
10. Why is choosing a specialist centre important?
Expertise in both lens surgery and retinal disease ensures personalised care, safe planning, and coordinated post-operative monitoring. This maximises visual potential and long-term retinal health.
Final Thoughts: Lens Replacement for Patients with Macular Degeneration
Lens replacement surgery can offer meaningful improvements in clarity, contrast, and overall visual comfort for patients with stable or early-stage macular degeneration. While the procedure cannot restore vision lost from retinal damage, careful pre-operative assessment, personalised lens selection, and coordination with ongoing retinal care allow patients to maximise the potential of their remaining healthy retinal tissue. Post-operative monitoring, realistic expectations, and the use of low vision aids further support daily activities and quality of life.
If you’re considering Lens Surgery in London, you can get in touch with us at London Cataract Centre. Consulting an experienced surgeon ensures a tailored approach that balances safety, retinal health, and optimal visual outcomes.
References:
- Mehta, H. (2021) ‘Management of cataract in patients with age‑related macular degeneration https://pmc.ncbi.nlm.nih.gov/articles/PMC8228734/
- Seo, J.H. and Lee, Y., 2024. Causal associations of glaucoma and age‑related macular degeneration with cataract: a bidirectional two‑sample Mendelian randomisation study https://www.mdpi.com/2073-4425/15/4/413
- Forooghian, F., Agrón, E., Clemons, T.E., Ferris, F.L. and Chew, E.Y., 2009. Visual acuity outcomes after cataract surgery in patients with age‑related macular degeneration: Age‑Related Eye Disease Study Report https://pubmed.ncbi.nlm.nih.gov/19700198/
- Hovanesian, J.A., et al., 2017. Optimizing cataract surgery in patients with age‑related macular degeneration. Survey of Ophthalmology, https://www.sciencedirect.com/science/article/abs/pii/S0039625716301424
- Tufail, A., 2008. Age‑related macular degeneration: diagnosis and management. British Medical Bulletin, https://academic.oup.com/bmb/article-abstract/85/1/127/292600

