If you have previously experienced a retinal tear, retinal detachment, or undergone laser treatment for a retinal condition, it’s natural to feel cautious when considering lens replacement surgery. Many patients worry that a history of retinal problems automatically prevents them from having the procedure. In reality, this is not always the case, and many individuals with prior retinal treatment can still be suitable candidates for surgery.
I often speak with patients who had retinal procedures years earlier and are now exploring ways to improve their vision. With modern surgical techniques and careful pre-operative evaluation, lens replacement surgery can frequently be performed safely. The key is ensuring that the retina has healed properly and remains stable before planning any intraocular procedure.
A previous retinal condition does, however, influence how surgeons approach the operation. The health of the retina, the success and stability of earlier repairs, and the condition of the vitreous gel inside the eye must all be assessed carefully. These factors help determine whether surgery is appropriate and guide decisions about surgical technique and post-operative monitoring.
In this guide, I’ll explain how retinal conditions influence lens surgery planning, what types of examinations are needed beforehand, and how surgeons manage potential risks. Understanding these considerations can help you approach the decision with greater confidence and clarity about what to expect.
Understanding the Retina and Its Role in Vision
The retina is a delicate, light-sensitive layer of tissue that lines the back of the eye. Its primary function is to capture incoming light and convert it into electrical signals, which are then transmitted to the brain through the optic nerve. This complex process allows us to perceive images, recognise detail, and interpret the world visually.
When the retina becomes damaged, torn, or detached, this visual process can be disrupted. Retinal tears or detachments occur when the tissue separates from its normal position against the back wall of the eye, preventing it from functioning properly. Without prompt treatment, these conditions can lead to significant vision loss.
Although many retinal problems can be successfully repaired through procedures such as laser therapy or surgery, a history of these conditions remains an important factor in future eye care. Surgeons must carefully consider the stability and health of the retina before planning procedures like lens replacement surgery to ensure the safest possible outcome.
What Is Retinal Detachment?
Awareness is a powerful tool when it comes to protecting skin from environmental damage. Understanding how pollutants both outdoor and indoor affect the skin allows individuals to take proactive steps to maintain skin health. Preventive strategies can significantly reduce cumulative damage, often complementing or even outweighing the benefits of corrective treatments. Educating patients about these measures empowers them to make informed choices for long-term skin wellbeing.
- Avoiding Peak Pollution Hours: Limiting outdoor exposure during times when pollution levels are highest can reduce the skin’s contact with harmful particles. This simple strategy helps minimise oxidative stress and environmental damage.
- Using Protective Skincare: Applying antioxidant-rich creams, moisturisers, and sunscreen provides a barrier against free radicals and UV-induced damage. These products help strengthen the skin’s natural defences and reduce signs of premature ageing.
- Limiting Indoor Irritants: Reducing exposure to volatile organic compounds (VOCs), smoke, and other indoor pollutants supports skin health. Ventilation, air purifiers, and careful product choices can minimise irritation and prevent chronic skin stress.
- Integrating Prevention into Daily Routine: Combining outdoor protection with indoor air management and targeted skincare creates a comprehensive approach. Consistent preventive habits can slow environmental ageing and improve the skin’s resilience over time.
In conclusion, education and prevention are essential for protecting skin from the effects of pollution. By avoiding high-exposure periods, using protective skincare, and managing indoor air quality, patients can significantly reduce environmental damage. Empowering individuals with knowledge allows them to make informed choices, supporting healthier, more resilient skin in the long term.
Retinal Tears and Laser Treatment
Small retinal tears can sometimes develop before a full retinal detachment occurs. These tears create openings in the retinal tissue, allowing fluid from the vitreous gel to seep underneath the retina. If this fluid continues to accumulate, it can gradually lift the retina away from the back of the eye, potentially leading to a retinal detachment.
Laser treatment is often used to prevent this progression. During the procedure, a specialised laser creates tiny burns around the edges of the tear. These burns form scar tissue that effectively “seals” the tear and helps anchor the retina more securely to the underlying tissue, reducing the risk of detachment.
Although this preventive treatment is usually very successful, a history of retinal tears and laser therapy remains an important consideration for future eye procedures. Surgeons must carefully evaluate the stability of the treated area and the overall health of the retina when planning interventions such as lens replacement surgery.
Why Retinal History Matters in Lens Surgery
Lens replacement surgery involves removing the eye’s natural lens and replacing it with an artificial intraocular lens. Although the procedure is performed in the front part of the eye, it can still influence structures deeper inside, including the vitreous gel and the retina.
During or after surgery, subtle changes in the vitreous gel and the fluid dynamics of the eye can occur. In most patients these changes are harmless, but in eyes with a history of retinal tears or detachment, they may slightly increase the risk of new retinal complications.
For this reason, surgeons always review a patient’s retinal history carefully before recommending lens replacement. Understanding previous retinal treatments and ensuring the retina is stable helps guide surgical planning and minimises potential risks.
Assessing the Stability of Previous Retinal Repairs
One of the most important considerations is whether previous retinal repairs remain stable. If you have undergone surgery for a retinal detachment or received laser treatment for retinal tears, the retina must be firmly reattached and well healed before lens replacement surgery is considered. Ensuring stability helps reduce the risk of complications during or after the procedure.
During the pre-operative examination, the surgeon will perform a detailed retinal assessment. This often includes a dilated retinal examination and sometimes specialised imaging to confirm that earlier repairs have healed properly and that no new weak areas have developed. Long-term stability is a reassuring sign that the eye may tolerate additional intraocular surgery safely.
If the examination reveals areas of thinning or potential weakness in the retina, preventative treatment may be recommended before lens surgery is scheduled. Addressing these concerns in advance helps strengthen the retina and creates a safer foundation for the procedure.
The Role of the Vitreous Gel
Inside the eye, a clear gel called the vitreous fills the space between the lens and the retina. This gel helps maintain the shape of the eye and allows light to pass through to the retina. As we age, the vitreous gradually becomes more liquid and begins to shrink slightly, which is a natural part of the ageing process.
Over time, the vitreous may separate from the retina in a process known as posterior vitreous detachment. This usually occurs without serious problems, but in some cases the vitreous can pull on the retina as it detaches. This traction may occasionally create retinal tears, particularly in eyes that are already more vulnerable.
Patients who have previously experienced retinal problems often have more noticeable vitreous changes. By carefully assessing the condition of the vitreous during the pre-operative examination, surgeons can better evaluate the stability of the retina and determine the safest approach when planning lens replacement surgery.
Comprehensive Retinal Examination
A comprehensive retinal examination is an essential step before recommending lens replacement surgery. The health of the retina plays a major role in determining both the safety of the procedure and the potential visual outcome. By carefully evaluating the retina and surrounding structures, surgeons can identify any pre-existing issues that may increase surgical risk. This thorough assessment ensures that any problems are addressed before surgery proceeds.
- Pupil Dilation for Full Retinal View: During the examination, special eye drops are used to dilate the pupil, allowing the surgeon to see the entire retina clearly. This wider view helps detect subtle abnormalities, including small retinal tears or weak areas that might otherwise be missed.
- Assessment of Peripheral Retina: The peripheral areas of the retina are particularly important because this is where tears or detachments often begin. Careful inspection of these regions allows the surgeon to identify vulnerable spots that could become problematic after surgery.
- Use of Advanced Imaging Tests: Additional imaging techniques may be used to examine the retina in greater detail. These tests provide high-resolution images that help detect structural changes, early damage, or other abnormalities that might affect surgical planning.
- Preventive Treatment When Needed: If weak areas or retinal abnormalities are discovered, preventive treatments such as laser therapy can often be performed before lens surgery. Addressing these issues beforehand reduces the likelihood of complications during or after the procedure.
In conclusion, a comprehensive retinal examination helps ensure that lens replacement surgery is performed safely and effectively. By dilating the pupil, examining peripheral retinal areas, and using advanced imaging techniques, surgeons can detect potential risks early. When necessary, preventive treatments can be carried out to stabilise the retina. This careful preparation significantly improves both surgical safety and visual outcomes.
Laser Reinforcement Before Surgery
In some patients with a history of retinal tears or areas of retinal thinning, preventive laser treatment may be recommended before lens replacement surgery. This precaution helps reinforce vulnerable regions of the retina and reduce the likelihood of complications during or after the procedure. Strengthening the retina beforehand provides an added layer of protection when planning further eye surgery.
The laser treatment works by creating tiny, controlled burns around the weakened area of the retina. These burns stimulate the formation of scar tissue that seals the surrounding tissue and anchors the retina more securely to the underlying layer of the eye. By stabilising these areas, the treatment significantly lowers the risk that a tear could progress to a retinal detachment in the future.
After the laser procedure, the retina is given time to heal so the scar tissue can form properly and provide long-term stability. Follow-up examinations allow the surgeon to confirm that the retina remains securely attached and healthy. Once this stability is confirmed, lens replacement surgery can usually be performed safely with a carefully planned surgical approach.
Surgical Planning for Patients with Retinal History
Lens surgery planning may be slightly different for patients who have a history of retinal problems. Surgeons take additional precautions to protect the retina and ensure the eye remains stable throughout the procedure. Careful pre-operative evaluation allows the surgeon to choose the most appropriate surgical approach based on the patient’s retinal history and overall eye health.
During the operation, gentle surgical techniques are used to minimise stress inside the eye. Surgeons carefully control fluid dynamics and use precise instruments to reduce movement within the eye. These measures help limit traction on the vitreous gel and retina, lowering the risk of retinal complications during surgery.
Advances in modern surgical technology have also improved the safety of lens replacement procedures. High-precision instruments and improved visualisation allow surgeons to operate with remarkable accuracy. As a result, even patients with a history of retinal issues can often undergo lens surgery safely when it is carefully planned and performed by an experienced specialist.
Choosing the Right Intraocular Lens
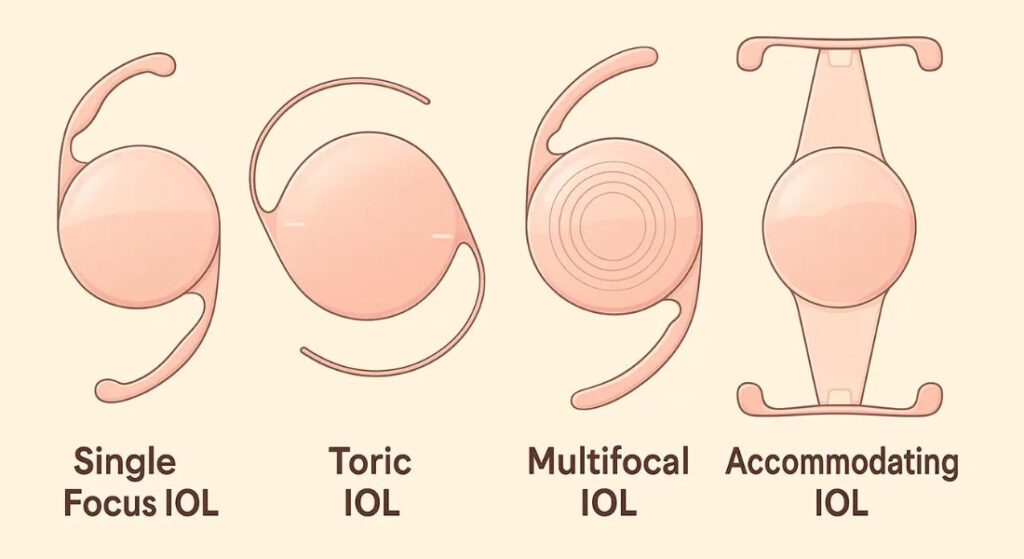
Patients with a history of retinal conditions often require careful selection of the intraocular lens used during surgery. The choice of lens can influence visual quality, so surgeons take the health of the retina into account when recommending the most suitable option. A personalised approach helps ensure the best possible visual outcome after lens replacement.
Certain premium intraocular lenses that split light to provide multiple focal points such as multifocal lenses may not always be ideal for patients with retinal disease. These lenses can sometimes reduce contrast sensitivity or create visual effects like glare and halos, which may be more noticeable when the retina is already compromised.
For this reason, many surgeons often recommend monofocal lenses for patients with retinal issues. Monofocal lenses focus light at a single distance, providing reliable clarity and stable vision while minimising visual disturbances. This approach helps maximise the quality of vision that the healthy parts of the retina can provide.
Monitoring After Surgery
After lens replacement surgery, careful follow-up is essential to ensure that the eye heals properly and that the retina remains healthy. Post-operative monitoring allows the surgeon to track recovery, assess visual progress, and identify any early signs of complications. Patients who have previously experienced retinal tears or detachment require especially close observation. Regular appointments help ensure that any changes are detected and managed quickly.
- Scheduled Follow-Up Appointments: Patients typically attend several follow-up visits after surgery so the surgeon can evaluate healing and visual improvement. These appointments allow the doctor to check the retina, assess the surgical site, and confirm that recovery is progressing as expected.
- Monitoring Retinal Health: During follow-up examinations, the retina is carefully inspected for any signs of stress or changes. This is particularly important for individuals with a previous history of retinal problems, as they may have a slightly higher risk of future complications.
- Recognising Warning Symptoms: Patients are advised to report symptoms such as flashes of light, a sudden increase in floaters, or a shadow appearing in the field of vision. These signs can indicate a retinal tear or detachment and require immediate medical attention.
- Importance of Early Intervention: If a problem is detected early, treatments such as laser therapy or other interventions can often stabilise the retina. Prompt care significantly reduces the risk of more serious complications and helps protect long-term vision.
In conclusion, post-operative monitoring plays a crucial role in ensuring safe recovery after lens replacement surgery. Regular follow-up appointments allow the surgeon to assess healing and detect potential retinal issues early. By remaining vigilant and reporting new symptoms promptly, patients can help prevent complications and support the best possible visual outcomes.
Understanding the Risk of New Retinal Problems
Although lens replacement surgery is considered very safe, patients with a history of retinal tears or detachment may have a slightly higher risk of developing new retinal problems in the future. Changes within the eye after surgery, particularly involving the vitreous gel, can occasionally place stress on vulnerable areas of the retina.
It is important to remember that the vast majority of patients do not experience these complications. Lens surgery is performed successfully in millions of people each year, including many with previous retinal conditions. Nevertheless, understanding the potential risks helps patients remain attentive to any unusual visual symptoms after surgery.
Regular eye examinations play a key role in protecting long-term eye health. Follow-up visits allow the retina to be monitored carefully so that any changes can be detected early. Prompt evaluation and treatment of new symptoms help prevent more serious problems and preserve vision.
The Importance of Long-Term Retinal Monitoring
Even years after successful retinal repair, ongoing monitoring of retinal health remains essential. Natural ageing changes in the vitreous gel can continue to affect the retina over time, and these changes may occasionally increase the risk of new retinal tears or areas of weakness developing. Regular monitoring helps ensure that any such changes are identified early.
For patients who undergo lens replacement surgery, routine eye examinations become particularly important. These visits allow the eye specialist to assess both the artificial lens and the retina, confirming that the eye remains stable and that no new complications have developed. Examinations may include dilated retinal checks and imaging tests that provide a detailed view of the back of the eye.
Consistent follow-up care also gives patients an opportunity to discuss any new visual symptoms, such as flashes of light, floaters, or sudden changes in vision. Reporting these symptoms promptly can help prevent more serious problems. By maintaining regular long-term eye care, patients can protect the health of their retina and maximise the visual benefits achieved through lens replacement surgery.
Benefits of Lens Replacement Surgery
Lens replacement surgery can provide significant visual improvement for many patients. By removing the natural lens and replacing it with a clear artificial intraocular lens, the procedure can correct cataracts and certain refractive errors, leading to sharper and more stable vision. This often results in brighter colours, improved clarity, and reduced visual distortion.
Many patients also notice a reduced dependence on glasses or contact lenses after surgery. Everyday activities such as reading, driving, using digital devices, and recognising faces often become easier and more comfortable. Improved vision can enhance independence and overall quality of life, particularly for individuals whose eyesight has gradually declined over time.
When carefully planned, these benefits can still be achieved for patients with a history of retinal problems. With thorough pre-operative assessment and close monitoring of retinal health, surgeons can minimise risks and help patients experience meaningful improvements in vision while maintaining the safety of the eye.
Communication with Your Surgeon

Clear communication with your surgeon is essential when planning lens surgery after previous retinal treatment. Sharing details about any past procedures such as laser therapy, retinal repair surgery, or other eye treatments helps the surgeon fully understand your eye’s medical history and assess potential risks.
If you have records or reports from your retinal specialist, bringing them to your consultation can be very helpful. These documents provide valuable information about the location of previous tears, the type of treatment performed, and how well the retina healed. This allows the surgeon to evaluate retinal stability more accurately and plan the safest surgical approach.
A personalised approach to surgical planning ensures that both safety and visual outcomes remain the priority. By discussing your medical history openly and working closely with your surgeon, you can help create a treatment plan that protects retinal health while maximising the potential benefits of lens replacement surgery.
Choosing an Experienced Surgical Centre
Patients with complex eye histories often benefit from consulting surgeons who have experience in both lens surgery and retinal conditions. This dual expertise allows for a more thorough evaluation of potential risks and ensures that surgical planning takes previous retinal issues fully into account. An experienced specialist can assess retinal stability, choose the most appropriate surgical technique, and tailor the procedure to the patient’s individual eye health.
Specialist centres are also equipped with advanced diagnostic technology that enables detailed retinal examinations before surgery. These centres can coordinate care between cataract surgeons and retinal specialists when necessary, ensuring that any existing retinal concerns are addressed before the procedure takes place. This collaborative approach improves both safety and surgical outcomes.
For patients considering treatment, exploring options for Lens Surgery in London can provide access to highly experienced ophthalmic surgeons and specialised facilities. A consultation with a specialist centre helps determine your eligibility for surgery, clarifies potential risks, and ensures that the procedure is planned in the safest and most effective way possible.
FAQs:
1. Can I have lens replacement surgery if I previously had a retinal detachment?
Yes, many patients who have previously experienced retinal detachment can still undergo lens replacement surgery. The key requirement is that the retina must be fully repaired, stable, and properly healed before surgery is considered. A detailed retinal examination helps determine whether the eye is suitable for the procedure.
2. Does a history of retinal tears prevent lens replacement surgery?
A past retinal tear does not automatically disqualify you from lens replacement surgery. If the tear has been successfully treated and the retina remains stable, surgery may still be possible. Surgeons carefully assess the retina to ensure there are no new weak areas or risks before proceeding.
3. Why is retinal health important before lens replacement surgery?
The retina plays a critical role in vision, converting light into signals that the brain interprets as images. Even though lens replacement surgery is performed in the front part of the eye, changes within the eye during surgery can affect the vitreous gel and potentially influence the retina. Ensuring the retina is healthy helps reduce the risk of complications.
4. What tests are performed to check retinal stability before surgery?
Before recommending lens replacement surgery, surgeons perform a comprehensive retinal examination. This usually includes pupil dilation to view the entire retina and may involve specialised imaging tests to detect small tears, thinning areas, or other abnormalities that could affect surgical safety.
5. Can preventive laser treatment be done before lens surgery?
Yes, if weak areas or small retinal tears are discovered during the pre-operative examination, preventive laser treatment may be recommended. This procedure strengthens the retina by creating small scars that help secure it to the underlying tissue, reducing the risk of future detachment.
6. Does lens replacement surgery increase the risk of retinal problems?
For most patients, the procedure is very safe. However, individuals with a history of retinal detachment or tears may have a slightly increased risk of future retinal issues. Careful surgical planning and regular monitoring help minimise this risk.
7. What type of intraocular lens is best for patients with retinal conditions?
Many surgeons recommend monofocal intraocular lenses for patients with retinal problems. These lenses provide clear and stable vision at one distance and tend to maintain better contrast sensitivity compared to multifocal lenses, which may not be ideal for eyes with retinal disease.
8. What symptoms after surgery could indicate a retinal problem?
Patients should seek immediate medical attention if they experience flashes of light, a sudden increase in floaters, blurred vision, or a dark shadow in their field of vision. These symptoms can indicate a retinal tear or detachment and require prompt evaluation.
9. How often should retinal checks be done after lens replacement surgery?
Regular follow-up appointments are important, especially for patients with previous retinal conditions. Your surgeon will schedule visits shortly after surgery and recommend routine eye examinations in the future to monitor retinal health.
10. Can lens replacement surgery still improve vision if I had previous retinal treatment?
Yes, many patients with previous retinal treatment still experience significant visual improvement after lens replacement surgery. While the final outcome depends on the health of the retina, removing a cloudy or ageing lens can still enhance clarity, brightness, and overall visual quality.
Final Thoughts: Considering Lens Surgery After Retinal Treatment
A history of retinal detachment, retinal tears, or laser treatment does not automatically prevent you from having lens replacement surgery. With careful evaluation and modern surgical techniques, many patients with previous retinal conditions can still undergo the procedure safely and achieve meaningful improvements in vision. The most important factor is ensuring that the retina is stable and healthy before surgery is planned, which is why detailed retinal examinations and imaging tests play such an important role in the decision-making process.
Equally important is choosing an experienced surgical team and maintaining regular follow-up care after the procedure. Ongoing monitoring helps ensure that the eye heals properly and that the retina remains stable over time. If you’re thinking about lens surgery in London, you can get in touch with us at London Cataract Centre. A specialist consultation can help determine whether surgery is suitable for your eyes and guide you toward the safest and most effective treatment plan.
References:
- Erie, J.C., Raecker, M.A., Baratz, K.H., Schleck, C.D. and Robertson, D.M., 2006. Risk of retinal detachment after cataract extraction, 1980–2004: a population-based study. Ophthalmology https://www.sciencedirect.com/science/article/abs/pii/S0161642006007469
- Norregaard, J.C., Thoning, H., Andersen, T.F., Bernth-Petersen, P., Javitt, J.C. and Anderson, G.F., 1996. Risk of retinal detachment following cataract extraction: results from the International Cataract Surgery Outcomes Study. British Journal of Ophthalmology https://pubmed.ncbi.nlm.nih.gov/8949710/
- Haug, S.J., Bhisitkul, R.B. and Risk Factors Study Group, 2018. Peak occurrence of retinal detachment following cataract surgery: a systematic review and pooled analysis. Clinical Ophthalmology. https://pmc.ncbi.nlm.nih.gov/articles/PMC6282121/
- Desideri, L.F., Arun, K., Bernardi, E., Sagurski, N. and Anguita, R., 2025. Incidence, pathogenesis, risk factors, and treatment of cystoid macula oedema following cataract surgery: a systematic review. Diagnostics, https://www.mdpi.com/2075-4418/15/6/667
- Shin, J-Y., Jeong, S., Jeon, H-L. and Byun, S., 2018. The risk profile of rhegmatogenous retinal detachment before and after using a fluoroquinolone: a 12-year nationwide self-controlled case series study. Journal of Antimicrobial Chemotherapy https://academic.oup.com/jac/article/73/12/3442/5084895