When patients first consider refractive lens exchange (RLE), the question I hear most often is: “Is it safe?” It’s a completely reasonable concern. Your eyes are precious, and the idea of surgery can feel intimidating. Naturally, you want to understand the risks before making any decision.
Refractive lens exchange is generally very safe, particularly when performed by an experienced surgeon in a well-equipped centre. Modern techniques and advanced intraocular lenses have made the procedure highly predictable. Complications are rare, and the vast majority of patients recover smoothly with excellent visual outcomes.
Like any surgical procedure, RLE does carry some potential risks. These may include infection, inflammation, retinal complications or temporary visual disturbances such as glare or halos. While these events are uncommon, understanding them is important for setting realistic expectations.
Knowing how risks are managed and what safeguards are in place can help you make an informed choice. Careful pre-operative assessment, precise surgical planning and expert follow-up all contribute to safety. By being aware of the process, you can approach RLE with confidence and clarity.
Introduction: Why Safety Matters in RLE
Safety is at the heart of every decision I make with patients considering refractive lens exchange. Unlike changing your glasses, surgery is permanent and irreversible, so understanding the process is essential. Being informed about both the potential benefits and the possible risks helps you decide whether RLE is the right choice for your eyes.
In this guide, we’ll explore the procedure itself, explaining how it works and what to expect during and after surgery. We will also look at potential complications, even though they are uncommon, so you can approach the decision with realistic expectations.
Finally, we will discuss the safeguards and modern techniques that protect your eyes throughout the process. From precise measurements to advanced surgical technology, every step is designed to maximise safety. Understanding these measures can give you confidence as you consider whether RLE is the right option for you.
What RLE Is and How It Works
Refractive lens exchange (RLE) is essentially the same procedure used in modern cataract surgery, but performed before a cataract develops. During RLE, your natural lens is carefully removed and replaced with a clear artificial intraocular lens. This lens is precisely calculated to correct common vision problems such as long-sightedness, short-sightedness, presbyopia, and even astigmatism. The surgery is quick, minimally invasive, and usually performed under local anaesthetic, allowing most patients to remain comfortable throughout.
One of the key benefits of RLE is that it provides a permanent correction. Unlike glasses or contact lenses, which can only adjust vision externally, the artificial lens remains inside your eye for life. It also removes the risk of future cataracts because the ageing natural lens is no longer present. This long-term stability can give patients peace of mind, knowing that their vision is unlikely to deteriorate due to lens-related changes in the future.
Because RLE is a well-established procedure, the techniques have become highly refined over the years. Surgeons use advanced diagnostic technology, detailed eye measurements, and careful planning to ensure precise lens placement and alignment. Modern equipment allows for highly predictable outcomes and minimal complications. Understanding how the procedure works, and why it is considered safe, can help you feel more confident when deciding whether RLE is the right option for your eyes.
How Safe Is RLE in General?
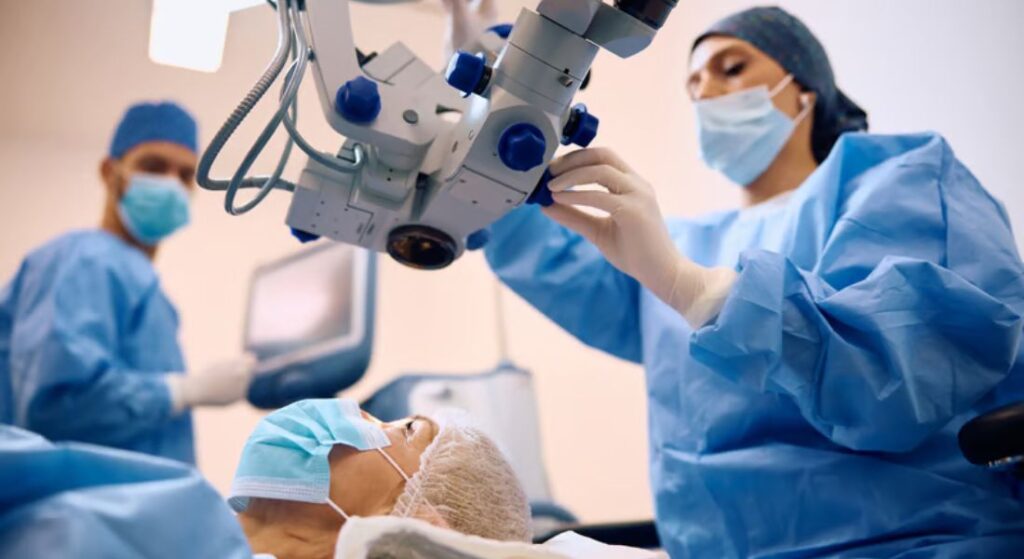
Refractive lens exchange (RLE) is considered very safe when performed by experienced surgeons. The procedure is based on the same techniques used in modern cataract surgery, which is one of the most common and safest operations performed worldwide. This long track record of success gives reassurance about both safety and predictability.
With today’s advanced diagnostic and surgical technology, the likelihood of serious complications is extremely low. Careful measurements, precise lens selection, and meticulous surgical technique all contribute to excellent outcomes. Most patients notice an improvement in vision almost immediately, often within the first few days after surgery.
While no surgical procedure is entirely without risk, the combination of refined techniques and skilled surgeons makes RLE a reliable option for long-term vision correction. Patients can usually expect a smooth recovery and a significant reduction in dependence on glasses or contact lenses.
The Importance of Surgeon Experience
When it comes to refractive lens exchange (RLE), not all surgeons have the same level of expertise, and experience can significantly impact outcomes. Choosing a surgeon who regularly performs advanced lens procedures is crucial for achieving safe and reliable results. Experienced surgeons are more familiar with the nuances of lens selection, placement, and patient-specific considerations, which can make a real difference in visual outcomes.
- Precision in Lens Placement: Accurate alignment of the intraocular lens is critical for optimal vision, especially with toric or multifocal lenses. Experienced surgeons have refined techniques that ensure the lens sits in the correct position, reducing the risk of visual disturbances. This precision directly affects how well the eye focuses at different distances.
- Careful Handling of Ocular Tissue: The eye is delicate, and every surgical step requires careful attention. Surgeons with extensive experience are adept at minimizing trauma to the cornea and surrounding tissues. This helps reduce complications, speeds up recovery, and supports long-term eye health.
- Familiarity with Potential Complications: Every surgical procedure carries some level of risk, and RLE is no exception. Experienced surgeons anticipate potential challenges and are prepared to manage them effectively. Their knowledge of both common and rare complications increases the likelihood of a smooth surgical experience.
Choosing a highly skilled and experienced surgeon is one of the most important factors in achieving excellent results with RLE. Beyond the technology and lenses themselves, surgical expertise ensures safety, precision, and a higher likelihood of meeting visual expectations. Patients can feel confident knowing that their care is in capable hands, supported by both skill and experience.
Pre-Operative Screening: Your First Line of Defence
Safety begins long before you enter the operating theatre. Thorough pre-operative screening is the first step in ensuring a successful outcome. During this stage, your cornea, retina, intraocular pressure, and overall eye health are carefully evaluated. These assessments help identify any potential issues that could affect surgery or recovery.
By understanding the specific characteristics of your eyes, the surgeon can anticipate challenges and select the most appropriate intraocular lens. Detailed measurements and imaging allow precise planning of lens power, alignment, and placement. This preparation is essential to minimise risk and maximise the likelihood of excellent visual outcomes.
Pre-operative screening also gives you the opportunity to ask questions and discuss your expectations. Knowing that every precaution has been taken provides reassurance and confidence before the procedure. It is the foundation for safe, effective, and personalised RLE surgery.
Choosing the Right Intraocular Lens
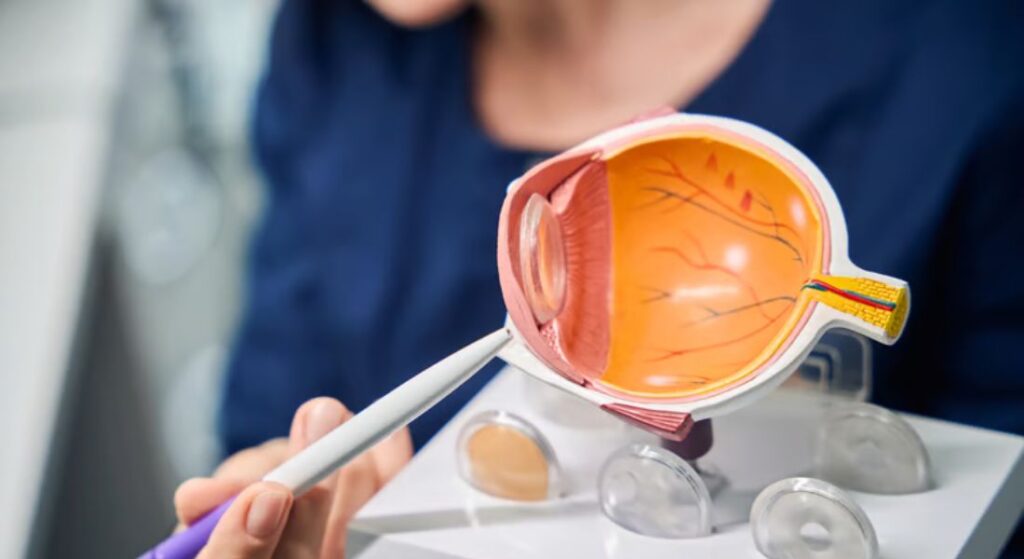
Selecting the right intraocular lens is about more than just achieving good vision it also plays a key role in safety and long-term satisfaction. Monofocal lenses are simple and predictable, offering excellent distance clarity with minimal adaptation required. Toric lenses are designed to correct astigmatism, but they need precise alignment to work effectively, making careful planning essential.
Multifocal and extended depth of focus (EDOF) lenses can provide a broader range of focus, allowing better vision for near, intermediate, and distance tasks. However, these designs may require a period of adaptation as your brain learns to process multiple focal points. Some patients notice mild visual phenomena such as halos or glare initially, which usually settle over time.
Choosing a lens that suits both your eyes and your lifestyle is crucial. The right lens reduces the risk of post-operative issues and ensures that your vision meets your daily needs. By carefully considering your priorities with your surgeon, you can achieve the best balance between clarity, comfort, and long-term safety.
Common Minor Side Effects
Even in very safe procedures like RLE, minor side effects can sometimes occur as part of the normal healing process. These are usually temporary and not a cause for concern. Common examples include mild dryness, light sensitivity, a gritty or scratchy feeling in the eye, or occasional fluctuations in vision. Some patients may notice slight blurriness or tearing during the first few days after surgery.
Most of these symptoms gradually improve within days or a few weeks as the eye settles and adapts to the new lens. Simple measures, such as using lubricating eye drops, protecting the eyes from bright sunlight, and following your post-operative care instructions, can help manage these effects effectively. Regular follow-up appointments also allow your surgeon to monitor recovery and address any concerns promptly.
Being aware of these minor side effects beforehand helps set realistic expectations for your recovery. While they can be mildly uncomfortable at first, the vast majority of patients find they are short-lived and do not interfere with the overall improvement in vision. Understanding this can provide reassurance and confidence as you recover.
Serious but Rare Complications
While refractive lens exchange (RLE) is generally very safe, it’s important to be aware of potential complications, even if they are uncommon. Understanding these risks helps patients recognise warning signs early and seek timely treatment. Most serious issues are rare and manageable when addressed promptly, allowing most patients to enjoy excellent long-term outcomes.
- Infection (Endophthalmitis): Infection inside the eye is extremely uncommon after RLE but can occur. Prompt treatment with antibiotics is usually effective, and early intervention is critical to prevent permanent vision loss. Surgeons take strict precautions to minimise this risk during and after surgery.
- Retinal Detachment: Retinal detachment is a rare complication, with slightly higher risk for patients with high myopia. If it occurs, it can be successfully managed with surgical repair. Regular post-operative monitoring helps detect any early signs so treatment can be initiated promptly.
- Posterior Capsule Opacification (PCO): Sometimes the thin membrane behind the lens can become cloudy months or years after surgery, causing blurred vision. This condition, known as posterior capsule opacification, is treatable with a simple and quick laser procedure, restoring clarity without the need for further surgery.
- Lens Dislocation or Rotation: Displacement or rotation of the implanted lens is rare, particularly for toric lenses designed to correct astigmatism. When it does occur, it can be corrected through a minor surgical adjustment. Proper surgical technique and lens selection help minimise this risk.
- Inflammation or Swelling: Temporary inflammation or swelling inside the eye is common in the early recovery phase. Anti-inflammatory eye drops usually manage this effectively, and symptoms typically resolve without lasting effects.
Being aware of these rare complications allows patients to act quickly if anything unusual occurs. Most people undergo RLE without any significant issues, and early recognition ensures that any problems are treated successfully, supporting safe and lasting visual improvement.
Lens Rotation and Toric Lenses
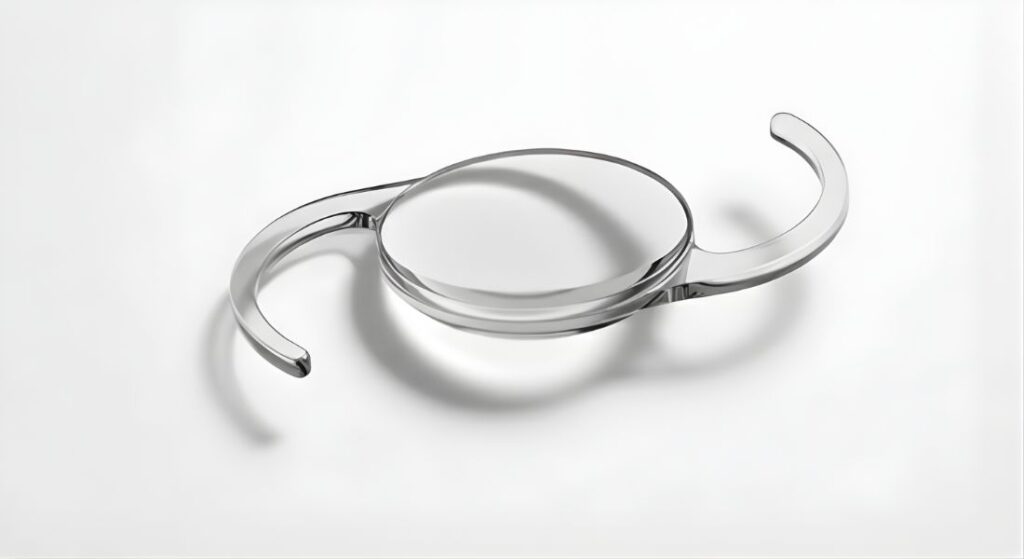
Toric lenses are specially designed to correct astigmatism, but their effectiveness depends on precise alignment within the eye. Even a small rotation can reduce the visual correction, making careful placement during surgery essential. Fortunately, modern lens designs and advanced surgical techniques have greatly minimised this risk, making lens rotation uncommon.
If a lens does rotate enough to affect vision, a minor repositioning procedure can usually restore optimal alignment. These adjustments are typically quick and safe, ensuring the lens continues to provide the intended correction.
The key to avoiding rotation issues lies in careful pre-operative planning, accurate measurements, and close post-operative monitoring. By taking these steps, surgeons can maximise the stability of toric lenses and help patients achieve the best possible vision.
Modern Surgical Safeguards
Advances in technology have dramatically improved the safety of refractive lens exchange. Micro-incision surgery, for example, allows the lens to be removed through a tiny opening, which reduces trauma to the eye and lowers the risk of infection. These smaller incisions also help speed up healing and recovery.
Modern phacoemulsification systems gently break up and remove the natural lens, minimising stress on the surrounding eye structures. Digital imaging and planning tools guide precise lens placement, ensuring the artificial lens is positioned accurately for optimal visual outcomes.
Strict sterile protocols and careful surgical technique further reduce the risk of infection or complications. Together, these safeguards create a highly controlled and safe environment for your eyes, giving patients confidence in both the procedure and the results.
Who May Be at Higher Risk?
While RLE is generally safe, certain patients may face slightly higher risks due to underlying eye or health conditions. Identifying these factors early allows your surgeon to adjust the surgical plan or recommend alternative approaches. Careful assessment ensures that each patient receives personalised advice tailored to their individual risk profile.
- Very High Myopia or Extreme Prescriptions: Patients with very strong prescriptions, especially high myopia, may have a slightly increased risk of retinal complications. Extra monitoring and careful surgical planning help manage these risks effectively. Specialised techniques may also be used to ensure the best possible outcomes.
- Pre-Existing Retinal Disease: Conditions such as diabetic retinopathy or macular degeneration can make eye surgery more complex. Awareness of these conditions allows the surgeon to tailor the procedure and follow-up care to protect vision. Early detection helps minimise potential complications.
- Previous Eye Surgeries or Trauma: A history of eye surgery or trauma can affect the eye’s structure, making lens placement more challenging. Surgeons take these factors into account to reduce risk and ensure precise outcomes. Pre-operative imaging and planning are crucial in these cases.
- Certain Autoimmune Conditions: Some autoimmune disorders can affect healing and increase the likelihood of inflammation after surgery. Identifying these conditions beforehand allows for appropriate pre- and post-operative management. This may include medication adjustments or closer monitoring during recovery.
By carefully evaluating these higher-risk factors, surgeons can optimise safety and visual outcomes for each patient. Early identification helps ensure that any additional precautions are taken, providing reassurance and personalised care throughout the RLE process.
Preparing for Surgery: What You Can Do
You can play an important role in making your surgery as safe and successful as possible. Following your surgeon’s pre-operative instructions carefully is essential. This includes disclosing all medications, medical conditions, and allergies, as well as avoiding activities that could irritate your eyes, such as rubbing them.
Preparing your home and daily routine for the first few days after surgery can also make recovery smoother. Simple steps like arranging for someone to drive you home, keeping prescribed eye drops nearby, and avoiding strenuous activity help minimise risk.
Attending all follow-up appointments and promptly reporting any unusual symptoms is equally important. Early detection of any issues allows timely intervention, which supports a safe recovery and the best possible visual outcome. By taking these steps, you become an active partner in ensuring your eyes heal safely and effectively.
What Happens During Surgery
Refractive lens exchange is a relatively quick procedure, usually taking around 15–20 minutes per eye. You remain awake throughout, with anaesthetic drops used to ensure comfort, so general anaesthesia is not required. This allows for a safe, controlled procedure while you stay relaxed and responsive.
During the surgery, your natural lens is carefully removed and replaced with a clear artificial lens through a tiny incision. The lens is folded for insertion and then positioned precisely, which is especially important when using toric or multifocal designs to ensure optimal vision correction.
Precision is key at every step, from lens alignment to placement. Most patients notice improved clarity within the first few days, and vision continues to settle and stabilise over the following weeks. The combination of advanced technique and careful planning makes the procedure both safe and highly effective.
Recovery: The First Few Days
Immediately after refractive lens exchange, your vision may feel slightly hazy or fluctuate from moment to moment. This is completely normal as your eye begins to adjust to the new artificial lens. Some patients also notice mild redness, light sensitivity, a gritty feeling, or occasional blurriness, all of which are common early post-operative symptoms. These effects are usually temporary and part of the normal healing process.
Most patients begin to enjoy noticeably clearer distance vision within the first few days. Colours may appear brighter because the ageing natural lens has been replaced with a clear artificial lens. Following your surgeon’s post-operative instructions, including using prescribed eye drops and avoiding rubbing or putting pressure on the eyes, helps support smooth recovery and reduces the risk of complications.
It’s important to remember that every eye heals at its own pace. While minor fluctuations in vision or slight discomfort are normal at first, clarity typically continues to improve steadily over the first week and beyond. Regular follow-up visits allow your surgeon to monitor progress and ensure your eyes are healing as expected, giving you confidence in the recovery process.
Neural Adaptation: How Your Brain Adjusts
Your brain has spent decades processing images through your natural lens, so it becomes highly accustomed to the way your eyes focus light. When a new artificial lens is introduced during RLE, your visual system needs time to adapt to this different optical setup. This adaptation occurs primarily in the visual cortex, which interprets the images sent from your eyes.
The process is particularly important for multifocal or extended depth of focus (EDOF) lenses. These lenses create multiple focal points, allowing you to see clearly at different distances, but your brain must learn to process these signals effectively. During this period, it’s common to notice halos, glare, or subtle differences in contrast, especially in low-light conditions.
Adaptation usually takes several weeks, and most patients find that these visual effects fade gradually as the brain becomes accustomed to the new lens. Patience during this stage is key, as the combination of eye healing and neural adjustment contributes to the final quality of vision. By understanding this process, you can approach recovery with realistic expectations and confidence.
Night Vision Considerations
Night driving or low-light conditions can sometimes reveal subtle visual effects after RLE. With monofocal lenses, night vision tends to remain very natural, with minimal issues such as glare or halos. These lenses provide clear, sharp vision at the chosen focal distance without introducing complex optical effects.
Multifocal lenses, on the other hand, may produce halos or starbursts around lights, especially in the early weeks after surgery. These effects are usually temporary and tend to diminish as your brain adapts to the new lens. Extended depth of focus (EDOF) lenses generally offer a middle ground, improving intermediate and distance vision while producing fewer night-time visual phenomena than multifocals.
Discussing your night vision needs before surgery is essential. If you frequently drive at night or work in low-light conditions, your lens choice can be tailored to balance daytime clarity, near vision, and night-time performance. Careful planning helps ensure your vision meets your lifestyle requirements safely and comfortably.
Long-Term Safety and Stability
Once your natural lens is replaced during RLE, cataracts can no longer develop, providing a permanent solution to age-related lens changes. The artificial lens is stable, does not age, and maintains its clarity for decades. This long-term stability is one of the key advantages of the procedure, giving patients lasting visual improvement and peace of mind.
Long-term complications are uncommon, but in rare cases, a mild posterior capsule haze may develop years after surgery. This can slightly affect vision, but it is easily and safely treated with a quick laser procedure known as YAG capsulotomy.
Overall, the combination of a permanent lens, refined surgical technique, and effective follow-up care makes RLE a highly reliable procedure. Most patients enjoy stable, clear vision for many years with minimal ongoing maintenance.
Comparing RLE Safety with Other Procedures
When considering vision correction options, it’s important to understand how refractive lens exchange (RLE) compares with alternatives like laser surgery. Each procedure has its own benefits and limitations, and the choice depends on your eye health, prescription, and long-term goals. RLE offers a highly predictable and durable solution, particularly for patients with presbyopia or higher levels of astigmatism.
- Predictable and Long-Lasting Results: RLE provides stable, long-term vision correction because it replaces the eye’s natural lens with an artificial one. Unlike laser procedures, which reshape the cornea, the lens implant remains unchanged over time. This predictability is especially valuable for patients seeking permanent solutions.
- Addresses Future Vision Changes: Laser vision correction cannot prevent age-related changes such as presbyopia or cataracts. As the natural lens continues to age, patients may still require glasses or additional procedures in the future. RLE, by contrast, removes the natural lens, addressing both current refractive errors and the risk of cataract development.
- Reduces Dependence on Glasses: With a properly selected intraocular lens, RLE can reduce or eliminate the need for glasses across multiple distances. Many patients enjoy freedom from reading glasses or multifocal lenses. This convenience is a key advantage over procedures that only correct distance vision temporarily.
- Avoids Future Cataract Surgery: Because RLE replaces the natural lens early, patients typically do not need cataract surgery later in life. This dual benefit vision correction now and cataract prevention makes RLE a unique and long-term solution for suitable candidates.
Overall, RLE offers a highly safe and durable alternative to laser vision correction for many patients. Its long-term predictability, ability to address presbyopia and cataracts, and potential to reduce reliance on glasses make it a compelling choice for those seeking comprehensive vision improvement.
Balancing Risk and Benefit
No surgical procedure is completely risk-free, and it’s important to acknowledge that before deciding on RLE. Like any operation, there are potential complications, although serious issues are rare when the surgery is performed by experienced surgeons in a well-equipped centre. Understanding these risks helps set realistic expectations.
The benefits of RLE are significant. Patients often gain clear, stable vision across distance and sometimes intermediate ranges, experience reduced dependence on glasses, and, importantly, eliminate the future risk of cataracts. These advantages can have a major positive impact on daily life and long-term eye health.
By weighing both the potential risks and the likely benefits, you can make a confident and informed decision. A thorough discussion with your surgeon ensures that you understand what the procedure can realistically achieve, helping you choose the option that best fits your lifestyle and visual needs.
FAQs:
1. How safe is refractive lens exchange (RLE)?
RLE is considered very safe, especially when performed by an experienced surgeon using modern techniques. Complications are rare, and most patients enjoy smooth recovery and excellent long-term vision.
2. What are the common minor side effects after RLE?
Temporary symptoms such as mild dryness, light sensitivity, gritty or scratchy feeling, occasional blurriness, or fluctuating vision can occur. These usually resolve within days to weeks as the eye heals.
3. What serious but rare complications should I be aware of?
Although uncommon, complications can include infection (endophthalmitis), retinal detachment, posterior capsule opacification (PCO), lens dislocation or rotation, and temporary inflammation or swelling. Most are treatable if detected early.
4. How important is the surgeon’s experience for RLE safety?
Extremely important. Experienced surgeons ensure precise lens placement, minimise trauma to eye tissues, and are better equipped to anticipate and manage potential complications, improving both safety and visual outcomes.
5. What role does pre-operative screening play in RLE safety?
Screening assesses cornea, retina, intraocular pressure, and overall eye health to identify risks. Detailed measurements and imaging allow precise lens selection and placement, maximising safety and visual accuracy.
6. Can I prevent lens rotation with a toric lens?
Modern surgical techniques and careful pre-operative planning greatly reduce the risk of lens rotation. If rotation occurs, a minor repositioning procedure can restore optimal alignment and visual correction.
7. How does RLE affect night vision?
Night vision outcomes depend on lens type. Monofocal lenses usually preserve natural night vision, multifocal lenses may cause temporary halos or glare, and EDOF lenses provide a balance with fewer visual disturbances.
8. Is RLE a permanent solution?
Yes. The artificial lens does not age, cataracts cannot develop, and vision remains stable for decades. Rare issues like posterior capsule opacification can be easily treated with a simple laser procedure.
9. How does RLE compare to laser vision correction?
RLE provides predictable, long-term results and addresses presbyopia and cataract risk. Laser procedures reshape the cornea and cannot prevent age-related lens changes, so patients may still need glasses or surgery later.
10. How can I ensure a safe recovery after RLE?
Follow all pre- and post-operative instructions carefully, attend follow-up appointments, report any unusual symptoms promptly, avoid rubbing your eyes, and use prescribed eye drops. Proper preparation and adherence to care instructions support a smooth recovery.
Final Thoughts: Ensuring Safety with RLE Surgery
Refractive lens exchange is a highly safe and effective procedure when performed by experienced surgeons using modern techniques. While no surgery is entirely without risk, serious complications are rare, and most patients enjoy smooth recovery, clear vision, and long-term stability. Careful pre-operative screening, precise lens selection, and advanced surgical safeguards all contribute to minimising risks and maximising visual outcomes.
Understanding potential minor side effects, rare complications, and the importance of neural adaptation helps set realistic expectations and supports a confident recovery. By choosing the right surgeon and following post-operative guidance, you can achieve excellent long-term vision with minimal disruption to your daily life. If you’re thinking about refractive lens exchange in London, you can get in touch with us at London Cataract Centre.
References:
- Alió, J.L., Pinero, D.P. and Plaza‑Puche, A.B., 2024. Refractive Lens Exchange: A Review. Clinical Ophthalmology, https://pubmed.ncbi.nlm.nih.gov/39146574/
- Hannan, S.J. et al., 2023. Immediate Sequential Bilateral Surgery in Refractive Lens Exchange Patients: Clinical Outcomes and Adverse Events. Ophthalmology, https://www.sciencedirect.com/science/article/pii/S0161642023002798
- Park, C.Y., 2026. Factors affecting postoperative satisfaction after presbyopia‑correcting intraocular lens implantation. Journal of Clinical Medicine https://www.mdpi.com/2077-0383/15/1/336
- Dołowiec‑Kwapisz, A., Piotrowska, H. and Misiuk‑Hojło, M., 2022. Evaluation of visual and patient‑reported outcomes after bilateral implantation with a non‑diffractive extended depth of focus intraocular lens. Journal of Clinical Medicine, https://pmc.ncbi.nlm.nih.gov/articles/PMC9456700/
- Mohamed, T.A., Soliman, W., El Sebaity, D.M. & Fathalla, A.M. (2017) Refractive lens exchange combined with primary posterior vitrectorhexis in highly myopic patients. https://pubmed.ncbi.nlm.nih.gov/28512581/

