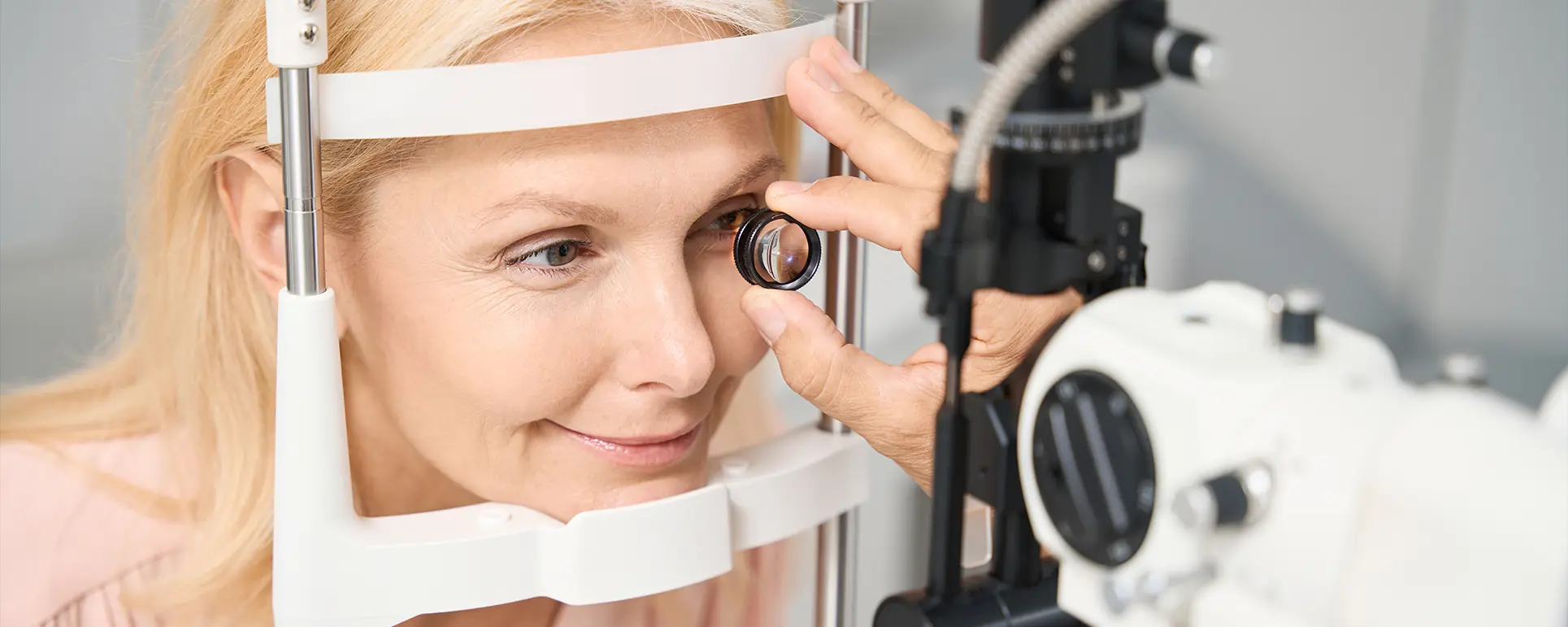
If you’ve had cataract surgery and received a toric intraocular lens (IOL), you probably expected clearer vision almost immediately. So if your eyesight still feels blurry, distorted or not quite right, it’s natural to feel worried or confused. One possible explanation although rare is that the IOL has rotated slightly from its intended position.
Toric lenses are designed to correct astigmatism, but they work properly only when they stay aligned at the exact angle your surgeon placed them. If that angle shifts, even by a few degrees, it can affect the clarity of your vision. The good news is that most cases of toric IOL rotation are easy to diagnose and straightforward to fix. In this guide, I want to walk you through why rotation happens, what symptoms you might notice, how surgeons confirm it and what the repositioning procedure involves.
Whether your surgery was recent or you’re preparing for a future procedure, understanding IOL rotation can give you peace of mind and help you recognise when to seek advice.
What Is a Toric IOL and Why Alignment Matters
A toric IOL is a specialised lens designed to correct astigmatism during cataract surgery. Astigmatism occurs when the cornea has an irregular curve, causing light to scatter rather than focus clearly. A toric lens has built-in power at a specific axis that neutralises this irregularity.
Toric IOLs are an effective solution for patients with astigmatism who want clearer vision without relying solely on glasses. Understanding how these lenses work and why precise alignment is critical can help you appreciate the importance of surgical accuracy and postoperative care for the best visual outcomes.
Why alignment is crucial:
- Toric IOLs must sit at a precise angle
- Even small rotations reduce the effect
- Misalignment can bring back astigmatism
- Correct positioning gives sharper vision
Because of this, surgeons carefully measure, mark and align the lens during your procedure. If it rotates, the astigmatism correction changes.
Why Does an IOL Rotate?

While most IOLs stay perfectly in place, rotation can happen for a few reasons.
1. The Shape of the Capsular Bag – After cataract surgery, your new lens sits inside the natural capsule that held your original lens. In some people, this capsule is slightly larger or looser, which can allow the IOL to rotate before it settles.
2. Residual Fluid in the Eye – During surgery, your surgeon uses liquids to clean, fill and flush the eye. If a small amount of fluid remains behind the lens, it may allow it to glide slightly until it settles.
3. High Astigmatism or Stronger Toric Power – The higher the astigmatism correction, the more sensitive the lens is to rotation. A stronger toric IOL needs to remain perfectly aligned.
4. Delay in Capsular Contraction – Over the weeks following surgery, the capsule naturally shrinks around the lens, holding it tightly in place. If this happens slowly, there is a longer window for rotation.
5. Eye Trauma or Excessive Rubbing – Significant pressure on the eye in the early healing phase can shift the IOL.
6. Rare Surgical or Anatomical Factors – These include unusually smooth capsules, weak zonules or very elastic capsular bags, although these are uncommon.
How Common Is IOL Rotation After Cataract Surgery?
Rotation of a toric intraocular lens (IOL), which is designed to correct astigmatism, is relatively uncommon. Most toric lenses remain stable within the first few days after surgery and typically do not move afterward.
Small rotations, usually less than 5 degrees, can occur in a minority of patients. These minor shifts generally do not affect vision and rarely require intervention. Significant rotations over 10 degrees are much less common.
Repositioning is needed in only about 1–2% of cases. When it does occur, rotation usually happens within the first week after surgery, when the lens is still settling into place.
Overall, modern surgical techniques and lens designs make toric IOL rotation a rare complication, and most patients enjoy stable, predictable vision following cataract surgery.
How Does Rotation Affect Your Vision?
While rotation of a toric IOL doesn’t harm the eye itself, it can significantly affect visual clarity. The lens is specifically aligned to correct astigmatism, so even small shifts can alter how light is focused on the retina.
Common symptoms of rotation include blurry vision, distorted or ghosted images, and the return of astigmatism. Patients may also notice difficulty reading, seeing fine details, or increased glare and halos, particularly in low-light conditions.
Some people describe the sensation that one eye “isn’t right” or that their vision is worse than it was immediately after surgery. The severity of these symptoms usually correlates with the degree of lens rotation the more the lens rotates, the more noticeable the visual changes.
If you experience these issues, your ophthalmologist can assess the lens position and determine whether a simple repositioning procedure is needed to restore optimal vision.
How Many Degrees of Rotation Matter?
Even small rotations of a toric intraocular lens (IOL) can have a noticeable impact on your vision. These lenses are specifically designed to correct astigmatism, and their effectiveness depends on precise alignment with the natural curvature of your cornea. Because every degree of rotation alters how light is focused onto the retina, even minor shifts can reduce the lens’s corrective power, affecting clarity and sharpness. Understanding how rotation affects vision helps patients appreciate why careful placement and follow-up are so important after surgery.
- A 5° rotation from the intended axis can reduce the effectiveness of astigmatism correction by approximately 15%.
- A 10° rotation results in roughly a 30% loss of the intended correction, which may noticeably affect vision.
- A 20° rotation can eliminate most or all of the corrective benefit, leaving residual astigmatism uncorrected.
- At 30° or more, the lens may actually reverse the intended effect, worsening vision rather than improving it.
This highlights why precise alignment and careful monitoring of toric lenses are essential for achieving the best possible visual outcomes.
How Surgeons Diagnose IOL Rotation
If you’re noticing symptoms, your surgeon can check whether the IOL has rotated.
1. Vision Assessment – They’ll measure your visual sharpness and compare it with expected results.
2. Astigmatism Measurement – If astigmatism has returned or worsened, rotation is a possible cause.
3. Slit Lamp Examination – A special microscope allows your surgeon to see the tiny axis marks on the IOL. These marks show the exact angle of the lens.
4. Imaging or Topography – If needed, additional scans help confirm alignment and measure any change in corneal shape.
5. Review of Surgical Axis Measurements – Your surgeon compares the current angle with the angle used during surgery. If they don’t match, rotation is confirmed.
When Should You Contact Your Surgeon?
After toric IOL surgery, most patients experience improved vision, but it’s important to monitor any changes closely. Knowing when to contact your surgeon can help address issues like lens rotation early, ensuring your astigmatism correction remains effective and your vision stays sharp.
You should get in touch if you notice:
- Blurred or reduced vision after initial improvement
- Ghosting or double images
- A sudden return of astigmatism
- Uneven clarity between the two eyes
- Vision that changes positionally
- A “tilted” or “shifted” feeling
It’s better to contact your surgeon early, even if you’re unsure. Rotation is easier to fix the sooner it’s detected.
How Surgeons Fix a Rotated IOL
The repositioning procedure is typically quick and highly successful.
Here’s what to expect.
1. A Simple, Short Procedure – Repositioning is usually done under local anaesthesia. You won’t feel pain, but you may feel light pressure.
2. The Surgeon Re-enters the Eye – A tiny incision is made, often using the same location as your original surgery.
3. The Lens Is Rotated Back into Position – Using delicate instruments, your surgeon gently rotates the IOL to the correct axis. This often takes just a few minutes.
4. Fluid Is Removed to Prevent Re-Rotation – Your surgeon removes any residual fluid behind the lens so it stays stable.
5. The Capsule Is Allowed to Grip the Lens Again – Over the next few days to weeks, the capsule contracts naturally and holds the lens firmly in place.
6. Recovery Is Usually Fast – Vision often improves immediately or within a few days. Most people return to normal activities quickly.
Is Re-Rotation Possible?
While toric IOLs are designed to remain stable, there is a small chance they may rotate after surgery. Understanding the possibility of re-rotation and how it’s managed can help set realistic expectations and ease any concerns about long-term outcomes.
If rotation occurs, surgeons have several strategies to correct it, from repositioning the lens to using stabilising devices or, in rare cases, exchanging the IOL. Most patients experience excellent stability, but knowing the options provides reassurance and clarity.
If this happens, your surgeon may:
- Repeat repositioning
- Use a capsular tension ring to stabilise the lens
- Consider exchanging the IOL for another model
These situations are rare and handled on a case-by-case basis.
How You Can Reduce the Risk of Rotation
There are simple ways to support stable healing.
1. Avoid Rubbing Your Eye – Pressure on the eye can shift the lens in the early days.
2. Follow Your Drops Schedule Carefully – This reduces inflammation and supports healing.
3. Avoid Heavy Lifting or Impact Exercise Early On – Your surgeon will advise how long to wait depending on your procedure.
4. Sleep with Your Protective Shield – Especially during the first week.
5. Attend All Follow-Up Appointments – Your surgeon can catch and treat rotation early.
Does Rotation Happen Only with Toric IOLs?
Rotation of intraocular lenses (IOLs) is primarily a concern with toric lenses rather than standard lenses. While it is true that all types of IOLs have the potential to move slightly after implantation, in most cases, standard monofocal or multifocal lenses do not cause noticeable vision changes if they rotate. This is because these lenses do not correct astigmatism, so a minor shift in their orientation does not impact the way light focuses on the retina or the overall clarity of vision.
Toric IOLs, on the other hand, are specifically designed to correct astigmatism, which means that the exact alignment of the lens is critical to achieving optimal vision. Even a small degree of rotation can reduce the lens’s effectiveness and lead to blurry, distorted, or ghosted vision. Because of this sensitivity, surgeons pay special attention during implantation to ensure toric lenses are placed at the correct axis, and patients are carefully monitored in the early postoperative period to detect any rotation.
In short, while rotation can theoretically occur with any type of IOL, it is the toric lenses where this issue is clinically significant. The precise alignment of toric IOLs is essential for them to perform their corrective function, making rotation a unique concern for patients who have received these specialized lenses.
What If Rotation Isn’t the Cause of Blurry Vision?
Blurry or distorted vision after cataract surgery isn’t always caused by lens rotation. There are several other potential reasons your vision may not feel perfectly sharp. Dry eye can make vision hazy, while residual refractive error may leave small amounts of nearsightedness, farsightedness, or astigmatism. Inflammation inside the eye or swelling of the retina, known as cystoid macular edema (CME), can also reduce clarity.
Posterior capsular opacification, sometimes called an “after-cataract,” may develop months after surgery and cause cloudiness. Additionally, natural floaters or other healing changes in the eye can temporarily affect vision. Your surgeon will carefully evaluate all these possibilities and rule out lens rotation as part of a thorough assessment to determine the cause of your blurry vision.
Blurry or distorted vision after cataract surgery can come from several other causes, including:
- Dry eye
- Residual refractive error
- Inflammation
- Swelling of the retina (CME)
- Posterior capsular opacification (“after-cataract”)
- Floaters
- Healing changes
Your surgeon will rule out rotation among other possibilities.
Will Glasses Fix IOL Rotation?
In cases of very mild toric IOL rotation, glasses can sometimes help improve vision temporarily. They may compensate for small residual refractive errors and make everyday tasks easier while your eye is settling.
However, if the lens has rotated significantly, glasses alone cannot restore full clarity. The toric correction built into the IOL is designed to work at a precise alignment, and large misalignments render this correction ineffective.
In these situations, the only reliable way to regain optimal vision is lens repositioning. This minor procedure realigns the IOL to its intended orientation, correcting astigmatism and restoring visual quality.
It’s important to consult your ophthalmologist promptly if you notice blurry vision, ghosting, or other visual disturbances after toric IOL surgery. Early assessment ensures timely intervention and the best possible outcome.
How Long After Surgery Can an IOL Rotate?
Most lens rotations occur shortly after surgery, while the eye is still healing and the lens is settling into place. The majority of rotations happen within the first 24 hours, as the lens adjusts inside the capsular bag. Additional small shifts can occur during the first week as swelling decreases and the eye stabilises. Very rarely, minor rotation may occur within the first month after surgery. Rotations months or years later are extremely uncommon because, by that time, the capsular bag has fully contracted around the lens, holding it securely in place.
FAQs:
1. What is a toric IOL, and why does alignment matter?
A toric intraocular lens is a specialized lens implanted during cataract surgery to correct astigmatism. Its design includes power along a specific axis to neutralize irregular corneal curvature. Alignment is crucial because even a small rotation can reduce the effectiveness of the astigmatism correction. Misalignment can cause blurry or distorted vision, and proper positioning ensures the lens delivers the intended clarity and sharpness.
2. How common is IOL rotation after surgery?
Toric IOL rotation is relatively uncommon. Most lenses remain stable after surgery, and small rotations of less than five degrees occur in a minority of patients. Significant rotations, which are noticeable or require intervention, are rare. Fewer than one to two percent of patients need surgical repositioning, and most rotations happen within the first week following the procedure.
3. What causes a toric IOL to rotate?
Rotation can occur for several reasons. The shape and size of the capsular bag may allow the lens to move before it fully settles. Residual fluid left behind the lens during surgery can let it glide slightly. Lenses designed to correct high levels of astigmatism are more sensitive to rotation. Delayed capsular contraction can also provide a longer window for movement. Additionally, trauma or rubbing of the eye during the early healing phase can shift the lens, and rare anatomical variations, such as weak zonules or unusually elastic capsules, may contribute.
4. How does IOL rotation affect vision?
When a toric IOL rotates, it does not damage the eye, but it can reduce visual clarity. Patients often notice blurry vision, ghosting, or distortion. Astigmatism may return, making it difficult to see fine details or read clearly. Some individuals experience glare, halos, or an unusual feeling that one eye “isn’t right.” The greater the rotation, the more noticeable these visual changes become.
5. How many degrees of rotation are significant?
Even small rotations can impact vision. A rotation of five degrees can cause roughly 15 percent loss of the intended astigmatism correction. A ten-degree rotation may result in about 30 percent loss, while a twenty-degree shift can negate the full correction. If the lens rotates thirty degrees or more, it may even reverse the intended effect of the toric correction.
6. How do surgeons diagnose IOL rotation?
To confirm rotation, surgeons first assess visual acuity and compare it to expected outcomes. They measure astigmatism to see if it has returned or worsened. A slit lamp examination allows the surgeon to view the tiny axis marks on the lens and determine its current orientation. Additional imaging or corneal topography may be used if needed. Finally, the surgical axis recorded during the procedure is compared with the lens’s present alignment to verify rotation.
7. When should I contact my surgeon?
Patients should contact their surgeon if vision becomes blurred after initial improvement, if ghosting or double images appear, or if astigmatism suddenly returns. Uneven clarity between the eyes, vision that changes depending on eye position, or a “tilted” visual feeling are also signs that require consultation. Early communication is important because rotation is easier to fix when detected promptly.
8. How is a rotated IOL fixed?
The repositioning procedure is typically quick and performed under local anaesthesia. The surgeon makes a tiny incision, often at the original surgical site, and gently rotates the lens back into the correct position using precise instruments. Any residual fluid behind the lens is removed to prevent further rotation. Over the next few days to weeks, the capsular bag naturally contracts and holds the lens firmly. Most patients notice immediate improvement or recovery within a few days.
9. Can IOL rotation happen again?
Re-rotation is uncommon but possible, particularly if the capsular bag is very loose or the lens corrects high astigmatism. In these cases, surgeons may repeat repositioning, use a capsular tension ring for stabilization, or consider exchanging the lens for a different model. Such situations are rare and are managed on an individual basis.
10. Are there ways to reduce the risk of rotation?
Patients can minimise the risk by avoiding rubbing the eye, following the prescribed eye drop regimen, and refraining from heavy lifting or impact exercise in the early healing phase. Wearing a protective eye shield while sleeping, especially during the first week, helps prevent accidental pressure. Attending all scheduled follow-up appointments allows the surgeon to detect and address rotation early, ensuring the best visual outcomes.
Final Thought: IOL Rotation and Replacement
Toric IOL rotation after cataract surgery is uncommon but can affect visual clarity if it occurs. Understanding the causes, recognising the symptoms, and seeking timely medical advice can make the difference between prolonged blurred vision and a simple, effective correction. Modern repositioning procedures are generally quick, safe, and highly successful, allowing most patients to regain optimal vision within days.
If you’re considering IOL replacement surgery in London, you can reach out to us at Eye Clinic London to discuss whether this treatment is the right choice for your vision goals.
References:
1. Singh, A. et al. (2020) ‘Rotational stability of toric intraocular lenses’, Journal of Cataract & Refractive Surgery. https://pmc.ncbi.nlm.nih.gov/articles/PMC8737107/
2. Rastogi, A. et al. (2018) ‘Comparative evaluation of rotational stability and visual outcomes after toric IOL implantation’, Clinical Ophthalmology. https://pmc.ncbi.nlm.nih.gov/articles/PMC5859597/
3. Hu, E.H. (2023) ‘Repositioning Rates of Toric IOLs Implanted in Cataract Surgery’, Clinical Ophthalmology. https://pmc.ncbi.nlm.nih.gov/articles/PMC10752012/
4. Ichikawa, K. et al. (2025) ‘Study on Factors Affecting Toric Intraocular Lens Rotation’, Journal of Clinical Medicine. https://www.mdpi.com/2077-0383/14/18/6599
5. Park, R.B. (2024) ‘Astigmatism Management in Modern Cataract Surgery’, Vision. https://www.mdpi.com/2411-5150/8/1/9