Refractive Lens Exchange (RLE) surgery has become a popular option for people looking to reduce dependence on glasses or contact lenses, especially for those with age-related vision changes. It involves replacing the eye’s natural lens with an artificial intraocular lens, similar to cataract surgery, to correct vision. While generally safe for many patients, underlying conditions like thyroid eye disease (TED) can complicate both the procedure and recovery.
Thyroid eye disease is an autoimmune condition that affects the tissues around the eyes, not just the thyroid gland itself. Patients with TED may experience bulging eyes, swelling, and in some cases, double vision. These structural changes can alter the eye’s anatomy and tear film, making any intraocular procedure potentially more challenging. Understanding these factors is crucial for safe surgical planning.
For those considering RLE surgery, the presence of TED raises important questions about timing, risk, and expected outcomes. Surgeons must carefully evaluate the severity of the eye changes, the stability of thyroid function, and any ongoing inflammation. This ensures the procedure does not worsen symptoms or lead to complications such as increased dry eye, corneal exposure, or limited eye movement.
In this guide, we’ll explore how thyroid eye disease can influence RLE surgery, what preoperative assessments are necessary, and the strategies used to minimise risks. By understanding the interaction between TED and RLE, patients can make informed decisions and set realistic expectations for vision improvement and overall eye health.
Understanding Thyroid Eye Disease
If you’ve been diagnosed with thyroid eye disease (TED), you know it affects more than just your thyroid. TED can cause changes in the tissues around your eyes, sometimes leading to bulging, double vision, or dry eyes. These changes don’t just affect appearance they can also influence how safe and effective certain eye surgeries, like Refractive Lens Exchange (RLE), may be.
RLE surgery involves replacing your natural lens with an artificial one to correct vision, similar to cataract surgery. While generally safe, the structural changes caused by TED can make the procedure more complex. Swelling, inflammation, or abnormal eye movement may increase the risk of complications or affect recovery, so careful evaluation is essential before surgery.
Understanding the relationship between TED and RLE helps patients make informed decisions. By assessing the stability of the thyroid condition, the severity of eye changes, and overall eye health, surgeons can plan the safest approach. With proper precautions, many patients with TED can still benefit from improved vision through RLE.
What Is RLE Surgery?
Refractive Lens Exchange (RLE) is a surgical procedure where your eye’s natural lens is replaced with an artificial intraocular lens to correct vision. Unlike cataract surgery, which is performed when the lens has become cloudy, RLE is usually done proactively to improve vision and reduce dependence on glasses or contact lenses.
RLE is especially useful for people who are long-sighted (hyperopic) or experiencing age-related difficulty focusing on near objects. The artificial lens can be customised to correct near, distance, or even both types of vision, depending on your lifestyle and visual needs.
While RLE is generally safe, it is still major eye surgery and requires careful evaluation. Factors like the shape of your eye, overall eye health, and any underlying conditions including thyroid eye disease must be considered to ensure the best results and minimise complications.
How TED Can Affect Eye Structure
Thyroid Eye Disease (TED) can significantly impact the tissues and muscles surrounding the eyes. Inflammation caused by TED can change the shape of the eye or increase orbital pressure, leading to discomfort or vision changes. Understanding these structural effects is crucial for anyone considering Refractive Lens Exchange (RLE) surgery. Being aware of these factors helps in planning a safer procedure with better visual outcomes.
- Inflammation of Eye Muscles: TED can inflame the extraocular muscles, which control eye movement. This can lead to limited eye mobility and may complicate precise surgical measurements required for RLE.
- Altered Eye Shape: Swelling and tissue changes can subtly change the shape of the eyeball. These alterations may affect the accuracy of lens placement and refractive results after surgery.
- Increased Orbital Pressure: Fluid buildup or tissue expansion can raise pressure inside the orbit. High orbital pressure may contribute to discomfort and increase the risk of complications during or after RLE.
- Impact on Surgical Planning: Structural changes due to TED require careful assessment before surgery. Surgeons may need to adjust the surgical approach or timing to ensure optimal safety and vision correction outcomes.
In summary, TED can cause a range of structural changes that directly influence eye health and surgical planning. From muscle inflammation to altered eye shape, each factor must be carefully evaluated. Patients considering RLE surgery should discuss these considerations with their ophthalmologist to ensure a safe and effective procedure. Understanding the potential impact of TED on eye structure helps set realistic expectations for post-surgery results.
Assessing Orbital Changes
One of the main concerns with thyroid eye disease (TED) is proptosis, where the eyes are pushed forward due to swelling of the tissues around them. This forward movement can make surgery more challenging because there is less protective tissue around the eye, increasing the risk of exposure or injury during the procedure.
Surgeons will carefully assess the degree of proptosis before recommending Refractive Lens Exchange (RLE). This evaluation often involves detailed imaging and measurements of the orbit to understand how much the eye has shifted and how the surrounding muscles and tissues are affected.
Understanding these orbital changes is essential for planning a safe surgical approach. By assessing the structure and positioning of the eyes, your surgeon can tailor the procedure to reduce risks and optimise visual outcomes, even in the presence of TED.
Dry Eye Considerations
Many people with thyroid eye disease (TED) experience dry eye because your eyelids may not close fully or your tear production may be reduced. This can leave the surface of your eyes exposed, leading to irritation and discomfort in your daily life. You may also notice symptoms such as a gritty sensation, redness, or sensitivity to light. These signs can gradually worsen if the condition is not properly managed.
Dry eyes can make your recovery after surgery more difficult and may increase the risk of infection. When your eyes are not adequately lubricated, healing can be slower and less comfortable for you. You might also experience fluctuating vision or ongoing irritation during the recovery period. This is why careful attention to eye health is essential before proceeding with treatment.
Managing dry eye beforehand is critical to improving your outcomes with refractive lens exchange (RLE). You may be advised to use lubricating eye drops, follow a treatment plan, or make lifestyle adjustments to support better eye moisture. Taking these steps helps create a healthier surface for surgery and promotes smoother healing. By addressing dryness early, you can improve both your comfort and the overall success of the procedure.
Eye Movement and Double Vision
Thyroid eye disease (TED) can sometimes affect the muscles that control your eye movement, which may lead to double vision. This happens when the eyes do not move in perfect alignment, causing you to see two images instead of one. You might notice this more when looking in certain directions or when you are tired. These symptoms can interfere with your daily activities and visual comfort.
While refractive lens exchange (RLE) can improve your vision, it will not correct problems related to eye muscle function. This means that any double vision caused by TED may still remain after the procedure. It is important for you to understand this limitation before deciding on surgery. Your surgeon will carefully assess your condition to determine whether RLE is suitable for you.
For the best outcome, your condition should be stable before going ahead with surgery. Surgeons usually recommend waiting until your TED is inactive, as active disease can increase the risk of worsening double vision. Taking time to stabilise your eye health helps reduce complications and supports better results. This approach ensures that your treatment plan is both safe and effective for your needs.
Timing of Surgery
The timing of refractive lens exchange (RLE) in patients with thyroid eye disease (TED) is very important for achieving safe and effective results. Your eyes need time to stabilise before any surgical procedure is considered. This means the inflammation should have reduced and your eye position should remain consistent. When these factors are stable, the risk of complications is generally lower.
If you proceed with surgery while your condition is still active, it can lead to unpredictable outcomes. Changes in eye shape or position during the active phase may affect your vision after the procedure. You might also experience discomfort or a need for further corrective treatment. This is why careful planning and timing are essential for your overall satisfaction.
Waiting until your TED is stable allows your surgeon to assess your eyes more accurately and plan the procedure effectively. It also helps ensure that your visual results are more predictable and long-lasting. Taking a measured approach can improve both your safety and comfort throughout the process. By allowing the condition to settle, you give yourself the best chance of a successful outcome.
Pre-Operative Assessment
Before considering refractive lens exchange (RLE), you will undergo a thorough pre-operative eye assessment. This is an important step to understand the current health and structure of your eyes. Your surgeon will take the time to review your symptoms and any effects caused by thyroid eye disease (TED). This careful evaluation helps ensure that the procedure is planned safely and appropriately for you.
As part of the assessment, you may have specialised imaging to evaluate the orbit and surrounding eye structures. Your eye pressure will also be measured, along with a detailed assessment of your tear film. These tests provide valuable information about how your eyes are functioning and whether there are any underlying concerns. Each step is designed to give a complete picture of your eye health.
The results of these tests help your surgeon decide whether you are a suitable candidate for RLE. If any issues are identified, they may need to be managed before moving forward with surgery. This process ensures that risks are minimised and outcomes are improved. By completing a thorough assessment, you can feel more confident about the safety and success of your treatment.
Understanding the Risks
Like any surgical procedure, refractive lens exchange (RLE) carries potential risks that you should be aware of. When you have thyroid eye disease (TED), some of these risks may be slightly higher or require extra consideration. You may experience issues such as delayed healing or increased sensitivity after the procedure. Being aware of these possibilities helps you prepare for the recovery process.
In patients with TED, there can also be changes in eyelid position or ongoing problems related to dry eye. These factors can affect both your comfort and your visual results after surgery. You might notice irritation, uneven tear distribution, or fluctuations in vision during healing. Your surgeon will discuss these concerns with you and explain how they can be managed effectively.
Understanding these risks in advance allows you to make a well-informed decision about your treatment. It also gives you the opportunity to ask questions and address any concerns you may have. Taking the time to consider both the benefits and potential complications is an important part of the process. This approach ensures that you feel confident and prepared before moving forward with surgery.
Managing Expectations
Having realistic expectations is very important when considering refractive lens exchange (RLE). While the procedure can significantly reduce your dependence on glasses, it does not address all eye-related concerns. You should understand what the surgery can and cannot achieve before making a decision. This helps you approach the treatment with a clear and balanced perspective.
RLE will not correct issues caused by thyroid eye disease (TED), such as double vision or orbital swelling. These conditions are related to changes in the eye muscles and surrounding tissues rather than the lens itself. You may still need additional treatments or management for these symptoms. Being aware of these limitations helps prevent disappointment after surgery.
Discussing your expected outcomes with your surgeon ensures you have a clear understanding of the results. They will explain what improvements you can realistically expect based on your specific condition. This open conversation allows you to ask questions and address any concerns in advance. With the right expectations, you are more likely to feel satisfied with your overall outcome.
Lens Selection
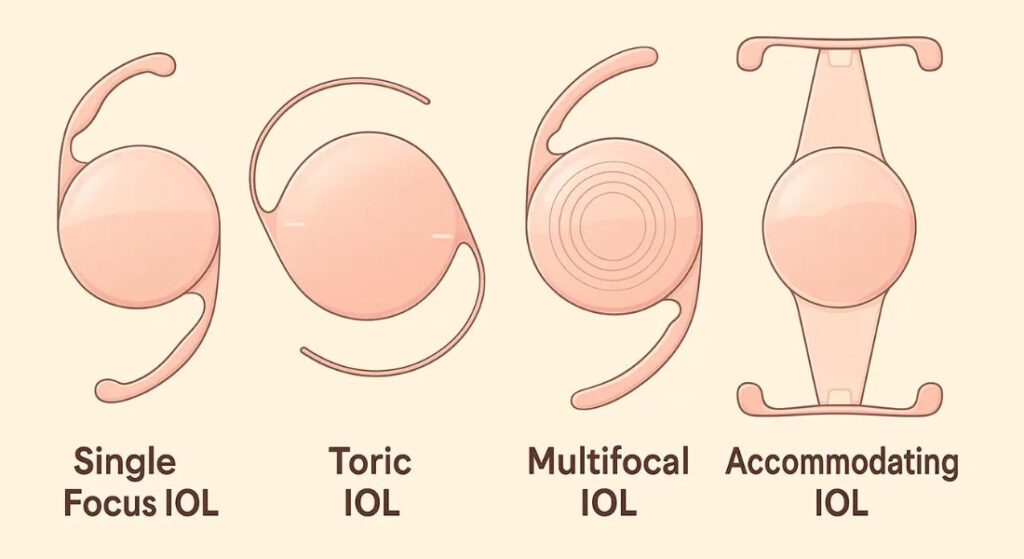
Choosing the right intraocular lens during RLE is an important decision, especially for patients with thyroid eye disease (TED). The condition can affect eye alignment, tear film stability, and overall visual quality, all of which influence lens performance. Because of these factors, lens selection must be carefully tailored to each individual. Your surgeon will evaluate your eye health and anatomy to recommend the most suitable option.
- Multifocal Lenses: Multifocal lenses are designed to provide clear vision at multiple distances, reducing dependence on glasses. However, in TED patients, issues like dry eye or visual fluctuations can affect how well these lenses perform. Your surgeon may recommend caution if there are concerns about visual quality or stability.
- Toric Lenses: Toric lenses are used to correct astigmatism and can significantly improve visual clarity. In patients with TED, the shape of the eye and cornea must be stable for accurate correction. If there are irregularities, your surgeon will assess whether a toric lens will deliver consistent results.
- Monofocal Lenses: Monofocal lenses provide clear vision at a single distance, typically for either near or far vision. They are often considered the safest and most predictable option for TED patients. This is because they are less affected by issues like dry eye or minor alignment problems.
- Individualised Assessment: Every TED case is different, so lens choice must be personalised. Your surgeon will consider factors such as eye surface health, orbital changes, and visual expectations. This ensures that the selected lens offers both safety and optimal visual outcomes.
Lens selection in RLE for patients with thyroid eye disease requires a thoughtful and customised approach. While advanced lenses like multifocal or toric options can offer benefits, they may not always be suitable depending on eye stability and anatomy. In many cases, simpler lenses provide more reliable results and fewer visual disturbances. Discussing your options thoroughly with your surgeon helps ensure the best possible outcome for your vision and comfort.
Post-Operative Care
After refractive lens exchange (RLE), your post-operative care focuses on managing inflammation, preventing infection, and supporting proper healing. You will usually be given eye drops and specific instructions to follow during your recovery. It is important that you use these treatments as directed to protect your eyes. Taking care during this period helps promote a smoother and more comfortable healing process.
If you have thyroid eye disease (TED), your care may involve additional monitoring. Your surgeon may check for any changes in eyelid position or how your eyes move after the procedure. You might also be advised to report any new symptoms, such as increased discomfort or double vision. This close observation helps ensure that any concerns are addressed early.
Regular follow-up appointments are essential to achieving the best possible results. During these visits, your surgeon will assess your healing and make any necessary adjustments to your treatment plan. Attending all scheduled appointments helps reduce risks and supports long-term success. By staying consistent with your care, you can improve both your comfort and visual outcome.
Dry Eye Management Post-Surgery
Dry eye management does not stop after your refractive lens exchange (RLE) surgery. You may continue to experience dryness as your eyes heal, especially if you have thyroid eye disease (TED). It is important to follow your surgeon’s advice to keep your eyes well lubricated. Ongoing care helps maintain comfort and protect the surface of your eyes.
You may need to use lubricating eye drops regularly to support tear balance and reduce irritation. In addition, simple lifestyle adjustments, such as staying hydrated and limiting screen time, can make a noticeable difference. In some cases, further treatments or procedures may be recommended to improve tear production. These steps are tailored to your individual needs and symptoms.
Proper dry eye care plays a key role in your overall recovery and visual outcome. It helps reduce discomfort, supports healing, and lowers the risk of complications. By staying consistent with your treatment plan, you can improve both short-term comfort and long-term eye health. This approach ensures the best possible results following your surgery.
Visual Recovery Timeline
Your vision after refractive lens exchange (RLE) may take several weeks to fully stabilise. In the early stages, you might notice fluctuations as your eyes adjust to the new lens. It is normal for clarity to improve gradually rather than immediately. During this time, following your surgeon’s advice is important for a smooth recovery.
If you have thyroid eye disease (TED), certain changes such as fluctuating eyelid position can temporarily affect how clearly you see. These variations may cause brief periods of blurred or inconsistent vision. You might find that your vision changes throughout the day or in different lighting conditions. These effects are usually temporary but should be monitored closely.
Patience is key during your recovery, as your eyes need time to heal and adapt. Sticking to your post-operative instructions, including using prescribed eye drops, can support better results. Attending follow-up appointments also helps ensure your progress is on track. With proper care and time, your vision is likely to become more stable and comfortable.
Long-Term Considerations
Refractive lens exchange (RLE) is a permanent solution for correcting your refractive error, meaning the treated lens does not need to be replaced. This can significantly reduce your reliance on glasses or contact lenses in the long term. However, it is important to understand that thyroid eye disease (TED) is a separate condition that may still change over time. Your overall eye health will depend on how TED progresses.
Even after successful surgery, TED can continue to affect the surrounding eye structures, such as the muscles and eyelids. You may notice changes in comfort, appearance, or vision if the condition evolves. These changes are not related to the lens implant itself but still require attention. Being aware of this helps you stay prepared for any future developments.
Regular follow-up care remains essential, even years after your procedure. Your eye specialist will monitor your condition and address any new symptoms as early as possible. Ongoing check-ups help maintain your eye health and support long-term visual stability. By staying consistent with your care, you can manage TED effectively alongside your surgical results.
Combining RLE with Other Treatments
Sometimes, if you have thyroid eye disease (TED), you may require additional treatments alongside refractive lens exchange (RLE). These can include procedures such as orbital decompression or eyelid surgery, depending on your specific condition. In some cases, these treatments are carried out before RLE to improve eye stability. In others, they may be recommended after surgery to refine both function and appearance.
Each treatment addresses different aspects of TED, such as pressure within the orbit or changes in eyelid position. While RLE focuses on improving your vision, these additional procedures aim to enhance comfort and eye alignment. You may find that a combined approach provides more balanced and effective results. Your care plan will be tailored to suit your individual needs and the stage of your condition.
Coordinating the timing of these procedures is essential for achieving the best outcome. Your surgeon will carefully plan the sequence to ensure your eyes are stable and ready for each step. This approach helps reduce complications and supports better healing throughout the process. By managing treatments together, you can optimise both your visual results and overall appearance.
Psychological Impact
Living with thyroid eye disease (TED) can take a significant emotional toll, affecting both self-confidence and overall well-being. Changes in appearance, vision issues, and ongoing discomfort often contribute to stress and anxiety. When considering surgery like RLE, these feelings can intensify due to uncertainty about outcomes. Addressing the psychological aspect is essential to ensure a more balanced and confident approach to treatment.
- Emotional Stress and Anxiety: TED can lead to ongoing emotional strain due to visible eye changes and fluctuating vision. This may cause self-consciousness or about daily interactions and quality of life. Recognising these feelings is the first step toward managing them effectively.
- Fear of Surgery: The idea of undergoing eye surgery can naturally create fear and hesitation. Concerns about safety, recovery, and results may feel overwhelming without proper guidance. Open discussions with your surgeon can help clarify doubts and reduce anxiety.
- Importance of Communication: Talking openly about your concerns allows your surgeon to better understand your expectations and worries. This communication helps build trust and ensures you feel supported throughout the process. It also enables more personalised guidance tailored to your emotional and physical needs.
- Mental Readiness: Being mentally prepared for surgery is just as important as being physically fit. A positive and informed mindset can improve your overall experience and recovery. Taking time to feel confident in your decision leads to better satisfaction with the outcome.
The psychological impact of thyroid eye disease and the prospect of surgery should not be overlooked. Emotional well-being plays a crucial role in how patients perceive and recover from treatment. By addressing fears, seeking clear information, and maintaining open communication with your surgeon, you can approach RLE with greater confidence. A balanced mindset ultimately contributes to a smoother journey and more reassuring surgical experience.
Patient Stories and Experiences

Hearing from other people with thyroid eye disease (TED) who have undergone refractive lens exchange (RLE) can be reassuring. Their experiences often give you a clearer idea of what to expect before, during, and after surgery. You may find comfort in learning how others have managed similar concerns. These real-life insights can help you feel more confident in your decision-making.
Many patients report an improved quality of life after RLE, particularly with reduced dependence on glasses or contact lenses. However, they often highlight the importance of properly managing dry eye symptoms throughout the process. Waiting until the disease is stable is also commonly emphasised as a key factor in achieving good results. These shared experiences show how preparation and timing can influence your outcome.
Listening to patient stories can help you set realistic expectations for your own journey. You gain a better understanding of both the benefits and the limitations of the procedure. This allows you to approach treatment with a balanced and informed perspective. By learning from others, you can feel more prepared and satisfied with your overall experience.
FAQs:
1. What is Refractive Lens Exchange (RLE)?
Refractive Lens Exchange (RLE) is a surgical procedure where the eye’s natural lens is replaced with an artificial intraocular lens to improve vision and reduce dependence on glasses or contact lenses.
2. Is RLE surgery safe for people with thyroid eye disease (TED)?
RLE can be safe for patients with thyroid eye disease, but only when the condition is stable. A thorough assessment is required to minimise risks and ensure the best outcomes.
3. How does thyroid eye disease affect eligibility for RLE?
TED can alter eye structure, cause inflammation, and affect tear production. These changes may influence whether you are a suitable candidate and how the surgery is planned.
4. Should I wait until my thyroid eye disease is stable before surgery?
Yes, surgeons usually recommend waiting until TED is inactive or stable. Performing surgery during the active phase can lead to unpredictable results and higher complication risks.
5. Can RLE correct double vision caused by TED?
No, RLE does not correct double vision caused by muscle or alignment issues. Additional treatments may be needed to address this symptom.
6. Does thyroid eye disease increase the risk of dry eye after RLE?
Yes, TED often causes dry eye, which can worsen after surgery. Proper management before and after the procedure is essential for comfort and healing.
7. What pre-operative tests are needed before RLE in TED patients?
Pre-operative assessment may include eye imaging, tear film evaluation, eye pressure measurement, and orbital analysis to ensure safe surgical planning.
8. Which type of intraocular lens is best for TED patients?
Monofocal lenses are often considered the safest option due to their predictability. Multifocal or toric lenses may be used in some cases, depending on eye stability and surface health.
9. What are the risks of RLE in patients with thyroid eye disease?
Risks may include dry eye worsening, delayed healing, fluctuating vision, and potential changes in eyelid position or eye alignment.
10. Can RLE be combined with other treatments for TED?
Yes, RLE may be combined with procedures like orbital decompression or eyelid surgery. The timing and sequence of treatments are carefully planned for optimal results.
Final Thought: Making an Informed Decision About RLE with TED
Refractive Lens Exchange can be a highly effective way to improve vision, but when combined with thyroid eye disease, it requires a more careful and personalised approach. From assessing eye structure and managing dry eye to choosing the right timing and lens type, every step plays a vital role in achieving safe and satisfying results. The key is ensuring that your condition is stable and that all potential risks are thoroughly evaluated before proceeding.
With expert guidance, detailed pre-operative assessments, and realistic expectations, many patients with TED can still benefit from improved vision and a better quality of life. Open communication with your surgeon and a commitment to ongoing eye care will help you navigate the process with confidence. If you’re considering RLE surgery in London, you can get in touch with us at London Cataract Centre.
References:
- Wróbel-Dudzińska, D., et al. (2024) The Effect of Dry Eye Disease Treatment Prior to Cataract Surgery on Refractive Error Reduction, Journal of Clinical Medicine, 15(4), 1640. Available at: https://www.mdpi.com/2077-0383/15/4/1640
- Caldwell, A.S., Patnaik, J.L., Ackerman, M., Christopher, K.L., Lynch, A.M. and Singh, J.K. (2021) Risk of refractive prediction error after cataract surgery in patients with thyroid eye disease, Clinical Ophthalmology, 15, pp. 4431–4438. Available at: https://pubmed.ncbi.nlm.nih.gov/34795474/
- Chiew, Y. and Poh, K.W. (2025) When postoperative inflammation isn’t benign: Thyroid eye disease following cataract surgery, Cureus, 17(10), e95196. Available at: https://pmc.ncbi.nlm.nih.gov/articles/PMC12638460/
- Al-Mujaini, A., Wali, U. and Bhandari, S. (2011) Medical management of thyroid eye disease, Saudi Journal of Ophthalmology, 25(1), pp. 3–13. Available at: https://www.sciencedirect.com/science/article/pii/S1319453410000998
- Hsu, H.-J., Hsu, C.-K., Chen, T.-S. and Hsu, C.-H. (2016) Thyroid eye disease, QJM: An International Journal of Medicine, 109(1), pp. 67–68. Available at: https://academic.oup.com/qjmed/article-abstract/109/1/67/1869890