If you have been referred for cataract surgery through the NHS, you may quickly notice that waiting times vary widely depending on where you live. In some regions of the UK, patients may receive surgery within a few months, while in other areas the wait can be considerably longer. These differences can be surprising and sometimes frustrating for patients who are eager to restore their vision.
Many people assume that because the NHS is a national healthcare system, waiting times should be consistent across the country. However, healthcare services are organised regionally, and each area manages its own resources, surgical capacity, and patient demand. As a result, access to cataract surgery can differ significantly from one location to another.
Several factors contribute to these regional variations. Local demand for cataract treatment, the number of available ophthalmic surgeons, operating theatre capacity, and funding allocation all influence how quickly patients can receive surgery. Areas with larger populations or older demographics may experience higher demand, which can naturally lead to longer waiting lists.
In this guide, I will explain the main reasons behind these regional differences in NHS cataract surgery waiting times. Understanding the pressures facing the healthcare system, as well as how regional services operate, can help patients better understand why waiting periods vary and what options may be available.
Understanding Cataracts and Their Impact
Cataracts develop when the natural lens inside the eye gradually becomes cloudy. This clouding affects how light passes through the eye, leading to symptoms such as blurred vision, glare from bright lights, faded colours, and difficulty seeing clearly. As the cataract progresses, everyday activities like reading, driving, or recognising faces may become increasingly challenging.
Cataracts are extremely common, particularly with ageing. While early stages may cause only mild visual disturbance, many patients eventually require surgery once the condition begins to interfere with daily life and independence. Because the condition develops gradually and affects a large portion of the population, the number of people needing treatment continues to grow.
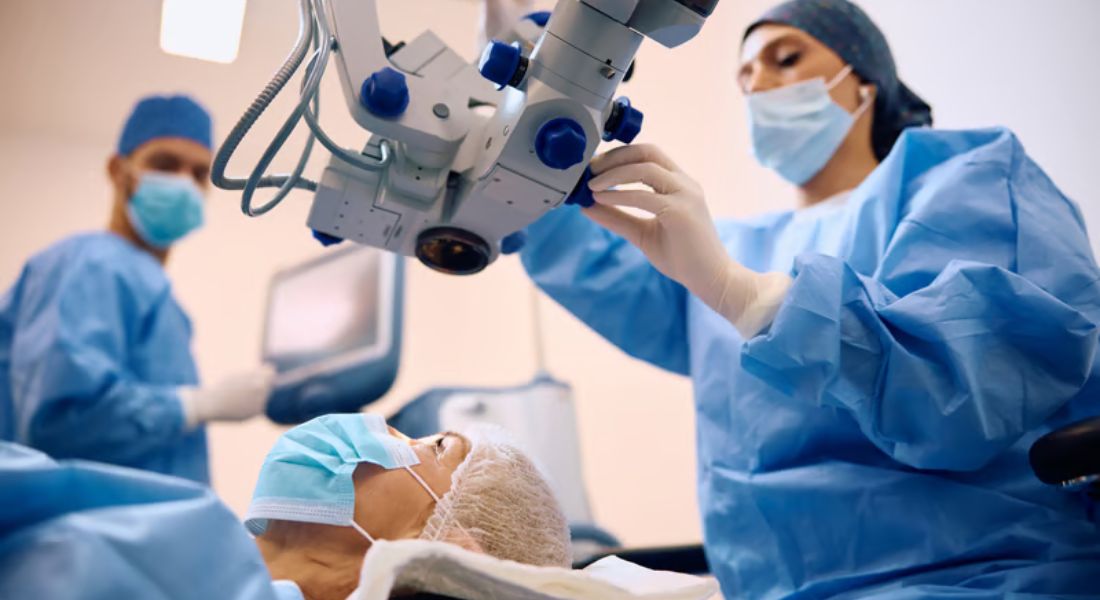
Cataract surgery involves removing the cloudy natural lens and replacing it with a clear artificial intraocular lens. The procedure is highly effective and is one of the most frequently performed operations within the NHS. Due to the high demand for treatment, managing access to cataract surgery has become an important challenge for healthcare providers.
Why Waiting Times Are Different Across the UK
Although the NHS is a national healthcare system, many services are organised and managed at a regional level. Local healthcare organisations are responsible for planning services, allocating resources, and managing patient demand within their areas. Because of this structure, the way cataract surgery is delivered can vary between different parts of the UK.
Each region faces its own challenges, including differences in population size, patient demand, staffing levels, and available funding. Areas with larger or older populations may have more patients requiring cataract surgery, while some regions may have fewer ophthalmic surgeons or limited operating theatre availability. These factors can naturally lead to variations in waiting times.
In some locations, hospitals may have greater surgical capacity and more specialised staff, allowing patients to receive treatment more quickly. In others, workforce shortages or higher demand can create longer waiting lists. As a result, waiting times often reflect a combination of local healthcare pressures rather than a single underlying cause.
The Role of Integrated Care Boards
In England, healthcare services are organised and funded through regional bodies known as Integrated Care Boards (ICBs). These organisations are responsible for planning how NHS resources are distributed across their local populations. Their decisions influence the availability of hospital services, community care, and specialist treatments. Because of this structure, access to procedures such as cataract surgery can vary depending on how each region prioritises its healthcare resources.
- Planning and Funding Local NHS Services: Integrated Care Boards oversee the planning and funding of healthcare services within their designated areas. They evaluate the health needs of the local population and determine how resources should be distributed across hospitals, clinics, and community healthcare providers.
- Allocation of Resources Across Services: ICBs must decide how to balance funding between different medical services, including emergency care, chronic disease management, and elective procedures such as cataract surgery. These decisions directly influence how much surgical capacity is available in local hospitals.
- Impact on Cataract Surgery Capacity: If an ICB faces limited resources or prioritises other urgent healthcare demands, the number of available cataract surgery appointments may decrease. When surgical capacity is reduced, waiting lists can grow longer, affecting how quickly patients receive treatment.
- Regional Variation in Waiting Times: Because each ICB manages resources independently, waiting times for procedures may differ between regions. Some areas may have shorter queues due to higher surgical capacity, while others may experience delays if demand exceeds available resources.
In conclusion, Integrated Care Boards play a central role in determining how healthcare services are delivered across England. Their decisions regarding funding and resource allocation influence the availability of procedures such as cataract surgery. While this decentralised approach allows services to be tailored to local needs, it can also lead to variations in waiting times between different regions.
Demand Pressures from an Ageing Population
One of the main reasons cataract surgery waiting times vary across the UK is the growing demand for treatment. Cataracts are strongly linked to ageing, and as the population gets older, the number of people requiring surgery continues to rise. This increasing demand places significant pressure on ophthalmology services within the healthcare system.
Certain regions have a higher proportion of older residents, which naturally leads to more patients needing cataract surgery. Hospitals and eye departments in these areas often face greater workloads, as they must manage a larger number of referrals from GPs and optometrists. As a result, waiting lists can grow more quickly in regions with older populations.
When the number of patients requiring treatment exceeds the available surgical capacity, delays become difficult to avoid. Even a relatively small gap between demand and the number of operations that can be performed each week can gradually extend waiting times, leading to longer periods before patients receive surgery.
Workforce Availability in Ophthalmology
The availability of trained ophthalmologists and specialised surgical staff is another major factor influencing cataract surgery waiting times. Cataract procedures require a highly skilled team, including experienced surgeons, theatre nurses, and ophthalmic technicians who work together to deliver safe and effective treatment. Without sufficient staff, hospitals cannot schedule as many operations.
Some regions face shortages of ophthalmology specialists, particularly in rural or less densely populated areas. Recruiting and retaining highly trained eye surgeons can be challenging in certain locations, which may limit the number of surgical sessions that hospitals are able to offer each week.
When staffing levels are restricted, the number of cataract procedures that can be performed naturally decreases. This can lead to longer waiting lists and slower patient throughput. As a result, variations in workforce availability play a significant role in the regional differences seen in NHS cataract surgery waiting times.
Operating Theatre Capacity
Operating theatre capacity plays a significant role in determining how quickly patients can access cataract surgery. The procedure requires specialised equipment, trained staff, and dedicated theatre space to be performed safely and efficiently. Hospitals must allocate their operating theatres among many different surgical specialties, which can create competition for available time. As a result, the number of cataract procedures that can be performed often depends on how theatre resources are managed within a hospital.
- Need for Specialised Equipment and Facilities: Cataract surgery requires microscopes, phacoemulsification machines, and other specialised ophthalmic equipment. These tools must be available in properly prepared operating theatres to ensure safe and precise surgical procedures.
- Competition for Theatre Time: Hospitals typically share operating theatres among several departments, including orthopaedics, general surgery, and cardiology. Because each specialty requires theatre access, ophthalmology departments may receive a limited number of surgical sessions each week.
- Impact on Surgical Throughput: When theatre availability is restricted, the number of cataract procedures that can be scheduled is also limited. This can lead to longer waiting lists, particularly in hospitals experiencing high patient demand.
- Dedicated Cataract Surgery Units: Some hospitals have introduced specialised cataract surgery theatres designed for high efficiency. These units streamline patient flow and allow surgeons to perform a greater number of procedures in a single day, helping to reduce waiting times.
In conclusion, operating theatre capacity is a key factor influencing how quickly cataract surgery can be delivered. Limited theatre availability can restrict the number of procedures performed, contributing to longer waiting lists. However, hospitals that establish dedicated cataract surgery units can significantly increase efficiency. These specialised facilities often help reduce delays and improve access to treatment.
Commissioning Decisions and Local Policies

Local commissioning decisions also play an important role in determining access to cataract surgery. In some regions, healthcare commissioners previously introduced strict referral thresholds that determined when patients could be placed on surgical waiting lists. These thresholds often required patients to reach a certain level of visual impairment before they qualified for treatment.
The purpose of these policies was to manage demand and ensure that limited surgical capacity was directed toward patients with the greatest clinical need. However, they sometimes resulted in variations between regions, with patients in some areas gaining access to surgery more quickly than others depending on local referral rules.
Although national guidance now encourages more consistent and equitable access to cataract surgery across the NHS, some local differences in referral pathways and approval processes can still exist. These variations may influence how quickly patients progress from diagnosis to being placed on a waiting list and eventually receiving surgery.
The Impact of COVID-19 on Waiting Lists
The COVID-19 pandemic had a significant impact on elective healthcare services across the NHS, including cataract surgery. During the height of the pandemic, many hospitals were forced to postpone routine procedures so that staff, equipment, and operating theatres could be redirected toward emergency and critical care services. This meant that thousands of planned cataract operations were delayed.
Operating theatres were often repurposed to support intensive care units or to treat patients with severe COVID-19 infections. At the same time, hospitals needed to reduce patient traffic within clinical settings to limit the spread of the virus. As a result, many non-urgent procedures, including cataract surgery, were temporarily suspended or significantly reduced.
Although most ophthalmology services have now resumed normal activity, the backlog created during that period continues to influence waiting times in some regions. Areas that experienced greater disruption during the pandemic may still be managing longer waiting lists as healthcare providers work to catch up on delayed treatments.
Differences Between Urban and Rural Areas
Geography can significantly influence how easily patients access cataract surgery. The availability of hospitals, ophthalmology specialists, and medical infrastructure often differs between urban and rural locations. These variations can affect both the speed of diagnosis and the timing of surgical treatment. As a result, patients living in different areas may experience different waiting times for the same procedure.
- Greater Hospital Capacity in Urban Areas: Cities typically have larger hospitals with more operating theatres and specialised ophthalmology departments. This increased capacity often allows urban centres to perform a higher number of cataract surgeries each year.
- Higher Number of Specialists: Urban regions generally attract more ophthalmologists and trained surgical staff. Having a larger pool of specialists can help hospitals schedule more procedures and manage patient demand more effectively.
- Limited Resources in Rural Locations: Rural hospitals may have fewer ophthalmology services and limited access to specialised equipment. As a result, surgical appointments may be less frequent, which can extend waiting times for patients living in these areas.
- Travel Requirements for Treatment: In some cases, patients from rural communities must travel to larger regional hospitals for cataract surgery. This additional distance can make scheduling and attending appointments more challenging for some individuals.
In conclusion, geographic location can play an important role in access to cataract surgery. Urban areas often benefit from larger hospitals and more specialists, which can increase surgical capacity. Rural areas may face resource limitations that affect how quickly procedures can be performed. These differences can contribute to variations in waiting times, even within the same healthcare system.
Referral Pathways and GP Access

The journey toward cataract surgery usually begins when an optometrist or GP identifies the presence of cataracts and refers the patient to an ophthalmologist for further assessment. This initial referral step plays an important role in determining how quickly a patient enters the surgical pathway.
In some regions, community optometry services have expanded their role in cataract assessment. Optometrists may carry out detailed examinations, confirm the diagnosis, and refer patients directly to hospital eye services. This streamlined approach can reduce delays in diagnosis and help patients move more efficiently through the system.
Where referral pathways are well organised and integrated between primary care and hospital services, patients may progress to surgery more quickly. In other areas, however, more complex or slower referral systems can create additional waiting periods before patients are assessed by a specialist and placed on the surgical list.
Private Sector Partnerships
To help reduce waiting times, the NHS sometimes works in partnership with independent healthcare providers to increase the number of cataract procedures that can be performed. These collaborations allow patients to receive surgery in facilities outside traditional NHS hospitals while the treatment is still funded by the NHS.
By using additional surgical centres and experienced ophthalmic teams, these partnerships can expand overall capacity and help address growing demand for cataract surgery. In areas where independent providers are actively involved, hospitals may be able to perform more procedures each week and gradually reduce waiting lists.
However, the extent to which these partnerships are used varies between regions. Local commissioning decisions, available healthcare infrastructure, and the presence of suitable independent clinics all influence whether such collaborations are implemented. As a result, some areas benefit from increased surgical capacity while others rely primarily on NHS hospital resources.
Technological Advances in Cataract Surgery
Modern surgical techniques have made cataract surgery faster, safer, and more efficient than in the past. Advances in surgical instruments, imaging technology, and surgeon training now allow experienced ophthalmologists to perform a large number of procedures with a high level of precision and safety. These improvements have helped increase the overall capacity for cataract treatment.
Some hospitals have introduced high-volume cataract surgery programmes designed to maximise efficiency. These programmes often use standardised surgical pathways, specialised cataract theatres, and dedicated teams that focus specifically on cataract procedures. By streamlining the process, hospitals can perform more operations within a single day.
Regions that adopt these high-efficiency surgical models may be able to reduce waiting times more quickly. In contrast, areas that continue to rely on more traditional scheduling systems may treat fewer patients per session, which can contribute to longer waiting lists over time.
Patient Factors and Clinical Prioritisation
Not all patients are placed on waiting lists in exactly the same position. Clinical prioritisation plays an important role in determining how quickly cataract surgery is offered. Ophthalmologists assess the severity of vision loss, the impact on daily activities, and any safety concerns before deciding how urgently treatment is needed.
Patients whose vision has deteriorated significantly, or who face increased risks because of poor eyesight such as difficulty driving, working, or maintaining independence may be prioritised for earlier surgery. In some cases, individuals who rely heavily on good vision for safety or employment may also be considered more urgent.
While this prioritisation system ensures that patients with the greatest clinical need receive treatment first, it can also influence overall waiting times. Those with less severe symptoms may need to wait longer while more urgent cases are addressed, contributing to the variation in waiting periods across the healthcare system.
The Importance of Follow-Up Care
Cataract surgery does not conclude once the operation is complete. Follow-up care is an essential part of the treatment process, allowing ophthalmologists to monitor healing, ensure the eye is recovering correctly, and confirm that vision is improving as expected. These appointments also provide an opportunity to detect and manage any complications early, such as inflammation, infection, or changes in eye pressure, which can affect long-term outcomes.
Hospitals must carefully allocate clinic appointments, medical staff, and resources not only for performing surgery but also for providing thorough post-operative care. Most patients require multiple follow-up visits in the weeks and months after surgery to monitor recovery, adjust eye drops, and verify that the artificial lens is functioning optimally. These visits are critical to achieving the best possible visual results and maintaining eye health.
Balancing surgical volume with post-operative follow-up is an important aspect of managing ophthalmology resources. Departments must ensure that patients receive adequate attention after surgery while still maintaining the capacity to treat new cases. This careful planning helps protect patient safety and satisfaction but can also influence overall waiting times for cataract procedures in different regions.
What Patients Can Do While Waiting
Waiting for cataract surgery can be challenging, especially when vision is noticeably impaired. While waiting times vary depending on hospital resources and regional factors, there are practical steps patients can take to manage symptoms and maintain safety. Proactive measures can help preserve independence, reduce frustration, and ensure any changes in vision are addressed promptly.
- Regular Eye Examinations: Continuing routine check-ups with an optometrist or ophthalmologist helps track the progression of the cataract. These visits ensure that any rapid changes in vision are detected early, allowing for timely intervention if necessary.
- Updating Glasses Prescriptions: Sometimes, updating your glasses or contact lens prescription can temporarily improve clarity and visual comfort. While this doesn’t stop the cataract from progressing, it can make reading, driving, and other daily activities easier.
- Optimising Home Environment: Simple adjustments such as improving lighting, reducing glare, and using magnification tools can make a significant difference in daily life. These changes help patients perform tasks more safely and comfortably while waiting for surgery.
- Reporting Rapid Vision Changes: If vision deteriorates suddenly or symptoms such as double vision, flashes of light, or increased blurriness occur, contacting an optometrist or GP promptly may allow the referral to be reviewed. Early attention can ensure urgent cases are prioritised appropriately.
In conclusion, patients awaiting cataract surgery can take proactive steps to manage their vision and daily life. Regular eye check-ups, updated prescriptions, environmental adjustments, and prompt reporting of rapid changes all contribute to maintaining safety and comfort. These measures help patients cope effectively while waiting for surgical treatment.
Considering Alternative Options

When NHS waiting times are long, some patients choose to explore private treatment as an alternative. Private cataract surgery often provides faster access to procedures, shorter waiting periods, and more flexible scheduling. Costs vary depending on the clinic, surgeon, and the type of intraocular lens selected, but many patients find the reduced wait and personalised care worthwhile.
Specialist centres, such as the London Cataract Centre, offer tailored consultations and treatment options for both cataract and lens surgery. These centres combine advanced surgical techniques with personalised care, taking into account each patient’s eye health, lifestyle needs, and visual goals. Experienced surgeons can guide patients through lens selection, discuss recovery expectations, and provide a clear plan for follow-up care.
Exploring both NHS and private pathways allows patients to make fully informed decisions about their care. By understanding differences in waiting times, costs, surgical options, and service models, patients can choose the approach that best meets their individual needs, balancing safety, convenience, and long-term visual outcomes.
The Future of Cataract Services in the NHS
Reducing cataract waiting times remains a key priority for the NHS. Ongoing investment in surgical capacity, workforce development, and modern operating facilities is designed to increase the number of procedures that can be safely performed each year. These measures aim to improve access to cataract surgery and ensure that more patients receive timely treatment.
Integrated Care Boards are also working to streamline referral pathways, standardise assessment processes, and reduce regional variation in waiting times. By improving coordination between primary care, community optometry services, and hospital eye departments, patients can move more efficiently from diagnosis to surgery.
As healthcare systems continue to adapt to the challenges of an ageing population and rising demand for cataract treatment, gradual improvements in waiting times are expected in many areas. Combined with technological advances and better resource planning, these initiatives offer hope for more equitable and timely access to cataract surgery across the UK.
FAQs:
1. Why do NHS cataract surgery waiting times vary across the UK?
Waiting times differ because healthcare services are managed regionally. Factors such as local demand, funding allocation, surgeon availability, operating theatre capacity, and population demographics all influence how quickly patients can access surgery.
2. How does population age affect cataract surgery waiting times?
Regions with higher proportions of older residents often see more referrals for cataract surgery. Increased demand can lead to longer waiting lists, especially if surgical capacity or workforce resources are limited.
3. What role do Integrated Care Boards play in cataract surgery access?
ICBs in England plan and fund healthcare services in their regions. Their decisions on resource allocation, surgical capacity, and service prioritisation can directly influence how quickly patients can receive cataract surgery.
4. How does workforce availability impact waiting times?
Cataract surgery requires skilled ophthalmologists, theatre nurses, and technicians. Shortages of trained staff reduce the number of procedures that can be performed, contributing to longer waiting lists in some regions.
5. Can hospital operating theatre capacity affect cataract surgery scheduling?
Yes. Limited theatre availability, competition among surgical specialties, and insufficient specialised equipment can restrict the number of cataract procedures, increasing waiting times. Dedicated cataract units often help reduce these delays.
6. Did COVID-19 affect NHS cataract waiting times?
Absolutely. Many elective procedures, including cataract surgery, were postponed during the pandemic. Backlogs created by these delays continue to influence waiting times in some areas.
7. Are there differences in waiting times between urban and rural areas?
Yes. Urban areas usually have larger hospitals, more ophthalmologists, and higher surgical capacity, often resulting in shorter waits. Rural areas may face limited resources and longer travel distances, which can extend waiting periods.
8. Can patients access private cataract surgery to reduce waiting times?
Yes. Private treatment offers faster access, flexible scheduling, and shorter waiting periods. Many patients choose private surgery when NHS waiting lists are long, though costs vary depending on lens type and clinic.
9. How do referral pathways influence how quickly I can get surgery?
The speed of referral from GPs or optometrists affects when you are added to a surgical waiting list. Regions with streamlined referral systems can process patients faster, while complex or slower pathways may increase waiting times.
10. What can I do while waiting for NHS cataract surgery?
Patients can manage symptoms through regular eye exams, updating glasses prescriptions, optimising lighting and home environments, and reporting sudden changes in vision. These measures help maintain safety and comfort while waiting for treatment.
Final Thoughts: Understanding NHS Cataract Waiting Times
NHS cataract surgery waiting times can vary widely across the UK due to differences in regional resources, workforce availability, population demographics, and local commissioning decisions. Factors such as operating theatre capacity, referral pathways, and even the impact of COVID-19 have all contributed to the variation patients may experience. Understanding these influences can help manage expectations and highlight why some areas may provide faster access to surgery than others.
While waiting for surgery, patients can take practical steps to maintain visual comfort and safety, including regular eye check-ups, updating prescriptions, and optimising home environments. For those seeking faster access or personalised care, exploring private options is also possible. If you’re looking to enhance your vision or need personalised guidance, our specialist team at the London Cataract Centre is here to help. Consulting with experienced specialists ensures that your cataract treatment is planned safely, efficiently, and tailored to your individual needs.
References:
- Dmuchowska, D. A., Pieklarz, B., Konopinska, J., Mariak, Z. and Obuchowska, I. (2021) Impact of Three Waves of the COVID‑19 Pandemic on the Rate of Elective Cataract Surgeries at a Tertiary Referral Center: A Polish Perspective. International Journal of Environmental Research and Public Health https://www.mdpi.com/1660-4601/18/16/8608
- Salisbury, C., Johnson, L., Purdy, S., Valderas, J. M., and Montgomery, A. A. (2011) Epidemiology and impact of multimorbidity in primary care: a retrospective cohort study. British Journal of General Practice https://www.sciencedirect.com/science/article/abs/pii/S0140673623020731
- Schein, O. D., Katz, J., Bass, E. B., Tielsch, J. M., Lubomski, L. H., Amirhamzeh, M., Feldman, M., Colton, T. and Petty, B. G. (1999) The Relative Impact of Visual Impairment and Cardiovascular Disease on Health‑Related Quality of Life in Older People. Archives of Ophthalmology, https://pmc.ncbi.nlm.nih.gov/articles/PMC1955650/
- Chapman, J., Horne, R., Petrie, K. and Richards, T. (2002) Pooled cataract waiting lists: views of hospital consultants, general practitioners and patients. Journal of the Royal Society of Medicine, https://pubmed.ncbi.nlm.nih.gov/12461145/
- Bullen, H. (2025) Determinants of quality in the independent and public hospital sector: implications for NHS elective care delivery. International Journal for Quality in Health Care, https://academic.oup.com/intqhc/article/37/1/mzaf019/8052777