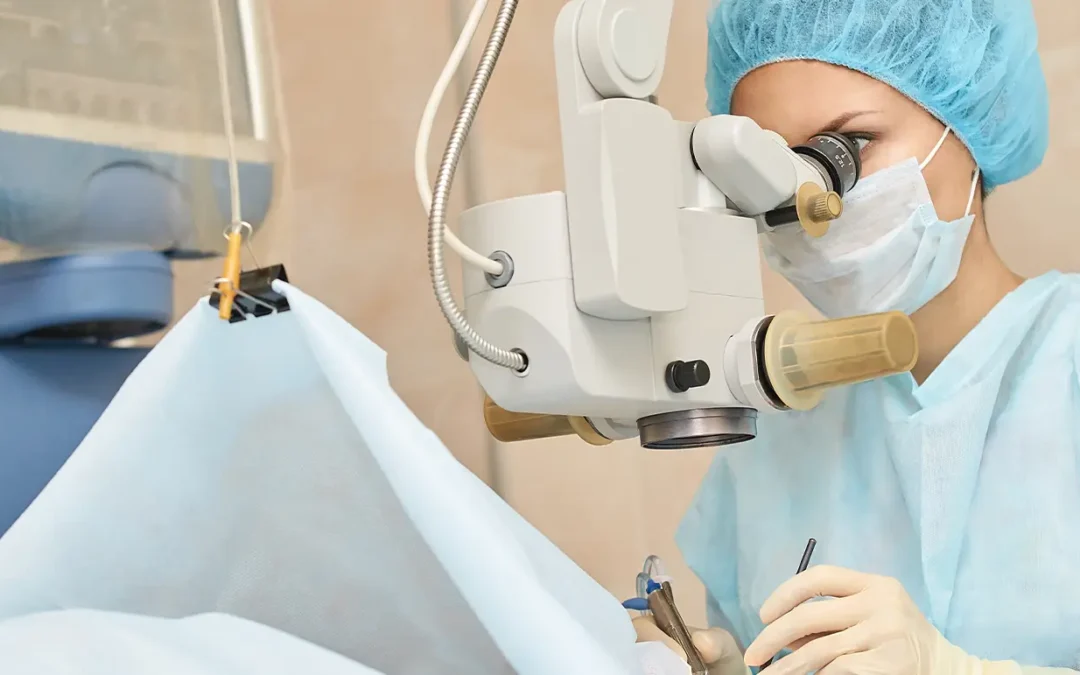
Most people think of cataract surgery as a straightforward fix remove the cloudy lens, insert a clear one, and restore vision. For many, that’s absolutely true. But for patients with severe corneal disease, lens replacement alone isn’t enough.
In these complex cases, the problem isn’t just inside the eye it’s also at the surface. The cornea, the transparent front window of your eye, can become so scarred, opaque, or damaged that light can’t pass through clearly, even if the lens behind it is perfect.
That’s where artificial corneas (keratoprostheses) come in. When used alongside or after cataract surgery, they can help restore vision for people once thought untreatable. In this article, we’ll explore when this approach is needed, how the surgeries are coordinated, and what new materials are making these combined treatments more successful than ever.
Understanding Cataract Surgery and Its Limits
Cataract surgery replaces your eye’s natural, clouded lens with an artificial intraocular lens (IOL). It’s one of the safest and most common operations in the world.
But even with a perfect lens, your vision depends on the clarity of your cornea. The cornea focuses incoming light onto your retina. If it’s scarred or damaged, your vision may remain cloudy even after cataract surgery.
In simple terms: the best lens in the world won’t help if the window it’s sitting behind is fogged over. That’s why patients with both cataracts and corneal damage may need more than standard surgery a combined approach that restores clarity to both the lens and the cornea for truly sharp, lasting vision.
When Cataract Surgery Alone Isn’t Enough
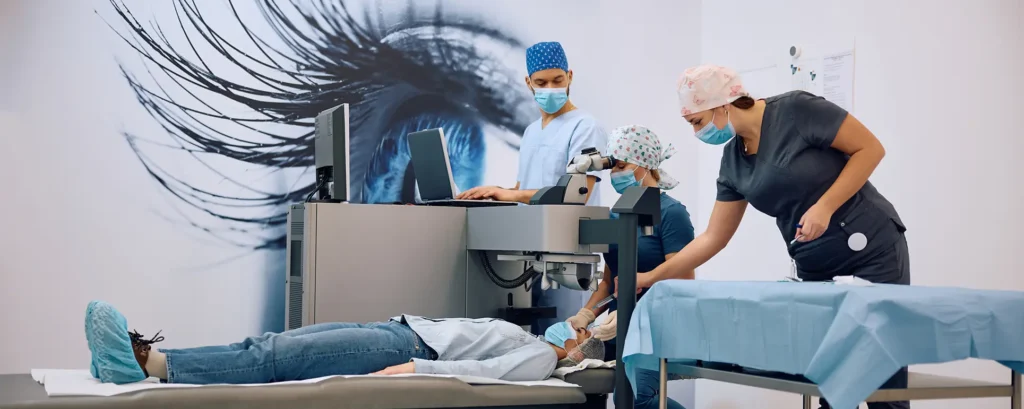
Cataract surgery restores the lens but doesn’t address problems with the cornea itself. Patients with severe corneal scarring from injury, infection, or prior surgery may still experience vision impairment even after cataract removal.
Other conditions, such as corneal dystrophies like Fuchs’ endothelial dystrophy, chemical burns, or autoimmune-related damage, can also block or distort light entering the eye. In these cases, the cornea remains a limiting factor for clear vision.
Severe keratoconus or failed corneal transplants may require additional interventions to restore sight. When the cornea prevents light from passing efficiently, treatments like corneal transplants or specialized keratoplasty become necessary alongside or after cataract surgery.
Introducing the Artificial Cornea (Keratoprosthesis)
An artificial cornea, or keratoprosthesis (KPro), is a synthetic device that replaces the damaged natural cornea. It allows light to reach the retina when traditional corneal transplants have failed or are not viable.
Unlike donor corneal tissue, which can be rejected or become cloudy again, an artificial cornea is made from biocompatible materials such as PMMA (polymethyl methacrylate) and hydrogel polymers designed to integrate with eye tissue.
Think of it as a permanent window implant that stays clear and stable for years, even in eyes that have experienced multiple failed grafts.
When Artificial Corneas Are Used with Cataract Surgery
In certain complex eye conditions, both cataracts and severe corneal damage can significantly impair vision. In such cases, artificial corneas, or keratoprostheses, may be used alongside cataract surgery to maximise visual outcomes. Depending on the patient’s condition, surgeons may choose either a staged approach or a combined procedure, each tailored to safely restore both corneal clarity and lens focusing ability.
There are two main situations when both surgeries come into play:
1. Sequential Approach
In the sequential approach, cataract surgery is performed first, allowing the eye to heal before a keratoprosthesis (artificial cornea) is implanted. This method is suitable when the cornea is partially clear or when cataract removal may improve visibility, helping the surgeon reassess corneal damage and evaluate retinal health before proceeding with the KPro.
2. Combined Procedure (Triple Surgery)
The combined procedure, often called triple surgery, involves cataract extraction, IOL implantation, and keratoprosthesis placement in a single operation. This is typically reserved for patients with long-standing blindness due to both corneal opacity and cataract, particularly after multiple failed corneal transplants, offering a more comprehensive and efficient visual restoration.
The advantage? It restores both the clarity of the cornea and the focusing power of the lens in one coordinated step.
How the Procedures Are Coordinated

Combining cataract surgery with artificial cornea implantation demands careful coordination and precise planning. The surgical team must synchronise each step, ensuring seamless transitions between procedures while maintaining patient safety and optimising outcomes.
Pre-Surgery Assessment: Before surgery, detailed imaging helps guide the procedure. Ultrasound biometry determines the correct lens power, OCT scans evaluate the retina and optic nerve, and corneal topography maps the corneal surface. These steps are especially crucial when visibility through a scarred cornea is limited.
During Surgery: During the operation, the cloudy lens is removed and replaced with a synthetic IOL. The damaged cornea is partially or fully excised, and the artificial cornea is implanted, often supported with donor tissue to ensure stability and proper positioning.
After Surgery: After surgery, careful post-operative monitoring is essential to prevent infection, inflammation, or pressure-related complications. Lifelong use of antibiotic and anti-inflammatory eye drops is typically required to maintain eye health and protect the new cornea.
Types of Artificial Corneas Used Today
Today, several types of keratoprostheses are used, each designed to address specific eye conditions. These artificial corneas vary in material, design, and suitability, allowing surgeons to choose the most effective option for restoring vision in complex cases.
1. Boston Keratoprosthesis (Boston KPro): The most widely used artificial cornea globally, the Boston KPro has a central clear optic surrounded by a supporting donor corneal ring. It’s typically used in patients with multiple failed corneal grafts or severe scarring.
2. Osteo-Odonto-Keratoprosthesis (OOKP): This highly specialised procedure uses a small piece of tooth and jawbone from the patient to anchor the optical cylinder. It’s reserved for the most severe cases such as chemical burns or Stevens-Johnson syndrome where other options won’t survive.
3. AlphaCor: A flexible hydrogel-based keratoprosthesis made entirely from synthetic material, eliminating the need for donor tissue. It’s biocompatible and reduces the risk of immune rejection.
4. CorNeat KPro (Next-Generation Design): A newer entrant, the CorNeat KPro uses nano-fibres that encourage tissue integration, allowing the eye’s natural cells to grow into the implant. It represents the future of long-lasting artificial corneal restoration.
Why Material Science Matters
Material science plays a crucial role in the success of modern corneal implants. Early artificial corneas often faced complications such as poor integration, infection, and clouding, limiting their effectiveness. Advances in biomaterials have largely overcome these issues.
Today’s keratoprostheses are designed to be biocompatible, reducing the risk of rejection. They are also flexible yet strong, carefully engineered to match the natural curvature of the cornea for better vision outcomes.
Transparency and stability are essential for consistent light transmission, ensuring clear vision. Researchers are now exploring materials like titanium mesh, collagen scaffolds, and nanocomposite hydrogels to further enhance durability, comfort, and long-term performance.
Who Is a Candidate for Combined Surgery?
Combined cataract and artificial cornea surgery may be recommended for patients who have both a cataract and corneal opacity that significantly limits vision. Addressing both issues at once can maximise the chance of meaningful visual improvement.
Candidates often include those who have experienced multiple failed corneal grafts or cannot undergo another donor transplant due to severe eye surface disease. High-risk conditions, such as autoimmune disorders or limbal stem cell deficiency, may also make combined surgery the preferred option.
Before recommending the procedure, your ophthalmologist will carefully assess the potential for visual recovery. Not every patient benefits, particularly if the retina or optic nerve has existing damage, so a thorough evaluation is essential to ensure the best outcome.
Benefits of Combining Cataract Surgery and Artificial Cornea Implantation
Combining cataract surgery with artificial cornea implantation offers patients a unique opportunity for comprehensive visual restoration. By addressing both lens clouding and corneal opacity in a single procedure, this approach not only enhances clarity of vision but also streamlines recovery and improves long-term outcomes. For carefully selected candidates, it can provide a meaningful, lasting improvement in sight and quality of life.
Comprehensive restoration: This approach provides comprehensive visual rehabilitation by addressing both corneal opacity and lens clouding at the same time. Patients benefit from clearer vision and a healthier ocular surface.
Single recovery phase: Since both procedures are done together, healing occurs simultaneously. This reduces the overall downtime compared with sequential surgeries, allowing patients to return to daily activities sooner.
Improved vision potential: Light transmission and visual focus are optimised, giving patients the potential for significantly improved clarity and quality of vision compared with treating only one issue.
Better long-term stability: Modern synthetic corneas offer better long-term structural stability, reducing the risk of complications and ensuring the eye remains healthy and functional over time.
For suitable candidates, this approach can offer a genuine second chance at functional sight.
Risks and Challenges
As with any complex eye surgery, combined cataract and artificial cornea procedures carry certain risks. These include infection, inflammation, and raised eye pressure, all of which require careful monitoring during recovery.
Rare but serious complications can also occur, such as device extrusion, retinal detachment, or macular oedema. Awareness and early detection of these issues are key to preventing long-term damage.
Careful patient selection and lifelong follow-up play a crucial role in minimising complications. Opting for an experienced surgical centre with advanced facilities, such as the London Cataract Centre, greatly improves both safety and visual outcomes.
Recovery and Aftercare
Recovery from combined cataract and keratoprosthesis surgery is more gradual than with standard cataract procedures. Patients must follow a strict regimen to support healing and protect the implant.
Daily eye drops, including antibiotics and steroids, help prevent infection and control inflammation. Special bandage contact lenses are often used to shield the keratoprosthesis and promote corneal stability.
Regular follow-up appointments are essential, especially during the first year, to monitor the eye’s progress. Vision typically improves slowly over weeks to months as swelling decreases and the eye adapts to the implant.
What Patients Can Expect Long-Term
With modern materials and careful maintenance, artificial corneas can last many years. Most patients experience:
- Clearer, sharper vision.
- Improved ability to recognise faces and navigate independently.
- Reduced sensitivity to glare once healing is complete.
However, lifelong care is essential skipping medication or follow-ups can jeopardise results.
The Role of Innovation in 2026 and Beyond
Innovation is rapidly transforming corneal surgery, with research pushing the boundaries of what’s possible. Emerging technologies aim to make complex cases more manageable and improve overall patient outcomes.
One exciting development is 3D-printed corneas using collagen bio-inks. These lab-grown tissues could provide custom-fit solutions for patients who cannot receive donor corneas, reducing dependence on traditional transplants.
Smart implants are also on the horizon, designed to release medication gradually. This approach can control inflammation and infection automatically, reducing the need for frequent eye drops and improving recovery.
Artificial-intelligence-guided surgery promises higher precision and safer procedures. By combining advanced imaging, predictive analytics, and robotic assistance, surgeons can tackle previously untreatable cases, offering renewed hope for patients with severe corneal and lens conditions.
Frequently Asked Questions (FAQs):
1. Can cataract surgery and artificial cornea implantation really be done together?
Yes, in select cases, both procedures can be performed in the same surgical session. This combined approach often called “triple surgery” is typically reserved for patients who have both a cataract and severe corneal opacity that prevents light from reaching the retina. It’s a complex operation requiring a skilled surgical team, but when successful, it can restore vision in eyes that were previously untreatable. The key lies in careful planning, as surgeons must assess the retina, choose the right lens power, and ensure that the corneal replacement will remain stable long term.
2. How do doctors decide whether to perform cataract surgery first or combine it with an artificial cornea?
The decision depends on the degree of corneal damage. If the cornea is only mildly cloudy, cataract surgery alone may be performed first, allowing doctors to assess how much vision improves. If the cornea is severely scarred or opaque, combining cataract removal with artificial cornea implantation makes more sense, as the lens replacement alone would not restore clarity. The ophthalmologist’s evaluation of your corneal health, retinal condition, and previous surgical history guides the final recommendation.
3. What materials are artificial corneas made from?
Modern artificial corneas are crafted from biocompatible materials such as PMMA (polymethyl methacrylate), titanium, and advanced hydrogel polymers. These substances are transparent, durable, and designed to integrate with surrounding eye tissues. Some newer designs, like the CorNeat KPro, even use nano-fibre scaffolds that encourage natural cell growth into the implant, enhancing stability and longevity. These innovations reduce the risk of immune rejection and make artificial corneas more reliable than earlier versions.
4. How long does recovery take after combined cataract and keratoprosthesis surgery?
Recovery varies by patient but generally extends over several months. Vision often begins to improve within weeks, but complete healing can take up to six months as swelling reduces and the eye adapts to the new corneal device. Regular post-operative check-ups are crucial during this time to monitor for infection, inflammation, or increased intraocular pressure. Most patients continue using antibiotic and anti-inflammatory drops indefinitely to maintain eye health and protect the implant.
5. Are there any long-term risks with artificial corneas?
While outcomes are often excellent, there are potential long-term risks such as glaucoma, infection, device extrusion, or inflammation. The eye’s natural tear film and immune response can change after surgery, requiring constant care. However, with proper management, many patients maintain clear and functional vision for years. Choosing a highly experienced surgical centre and adhering to lifelong follow-up care dramatically lowers the risk of complications.
6. How successful are artificial corneas in restoring vision?
Success rates have improved significantly in the last decade, thanks to better materials and surgical techniques. Most patients experience a substantial increase in clarity and visual function, particularly those who were previously blind due to corneal opacity and cataracts. While perfect 20/20 vision may not always be achievable, many regain enough sight to recognise faces, read large print, and navigate independently. Long-term outcomes depend on the health of the retina and optic nerve as well as post-surgical care.
7. Who is not a good candidate for this combined procedure?
Patients whose vision loss is primarily due to retinal or optic nerve damage may not benefit from artificial cornea implantation, as these parts of the eye cannot be replaced. Likewise, those with uncontrolled glaucoma, active eye infections, or poor overall health may be unsuitable. Your ophthalmologist will conduct detailed imaging and tests to determine whether the potential benefits outweigh the surgical risks.
8. What’s the difference between a donor cornea transplant and an artificial cornea?
A donor corneal transplant uses human tissue from an eye bank to replace the damaged cornea. While effective, it carries risks of rejection and clouding over time, especially after multiple surgeries. In contrast, an artificial cornea is made from synthetic materials designed to resist rejection and remain permanently clear. This makes it particularly useful for patients who have had several failed grafts or are not suitable candidates for donor tissue due to immune issues or limited availability.
9. How do artificial corneas improve upon older designs?
Earlier keratoprostheses often faced issues with poor integration, chronic inflammation, and infection. Newer models like the Boston KPro Type II and CorNeat KPro use advanced surface coatings, hydrogels, and nanocomposite materials that bond more effectively with the eye’s natural tissues. These improvements have extended the lifespan of the implants and reduced the frequency of complications. The result is clearer, more stable vision that lasts longer and requires fewer follow-up surgeries.
10. What future developments can patients look forward to?
Research in 2026 and beyond is moving toward bioengineered and “smart” corneas. Scientists are experimenting with 3D-printed collagen structures, self-healing polymers, and implants that release medication automatically to prevent infection. Artificial intelligence is also being integrated into surgical planning to improve accuracy and outcomes. These innovations could make artificial corneas safer, more accessible, and suitable for a wider range of patients turning once-experimental procedures into standard vision-restoring options.
Final Thoughts: When Vision Restoration Goes Beyond the Lens
The combination of cataract surgery and artificial cornea implantation represents one of the most advanced frontiers in modern ophthalmology. For patients who once faced irreversible vision loss due to both lens and corneal damage, this dual approach now offers genuine hope. By addressing the clarity of both the cornea and the lens simultaneously, it restores the eye’s full optical pathway something traditional surgery alone can’t achieve.
With rapid progress in biomaterials, 3D printing, and AI-assisted surgery, artificial corneas are becoming safer, more adaptable, and longer lasting than ever before. What was once considered experimental is now becoming a reliable path to restored sight and independence.
If you’re looking to enhance your vision or need personalised guidance, our specialist team at the London Cataract Centre is here to help.
References:
1. Ahmad, S., Fares, U. and Dua, H.S., 2021. Artificial cornea and future corneal replacement technology. British Journal of Ophthalmology, 105(10), pp.1352–1358.
Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8440302/
2. Greiner, M.A. and Mannis, M.J., 2020. Recent innovations in keratoprosthesis and artificial cornea design. Current Opinion in Ophthalmology, 31(4), pp.271–278.
Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7332611/
3. Harissi-Dagher, M. and Dohlman, C.H., 2022. The Boston Keratoprosthesis: outcomes, complications, and future directions. Survey of Ophthalmology, 67(1), pp.1–20.
Available at: https://pubmed.ncbi.nlm.nih.gov/34895759/
4. Leong, C., Tan, D.T.H. and Mehta, J.S., 2021. Corneal tissue engineering and regenerative medicine: current progress and future outlook. MDPI – Biomolecules, 11(2), p.248.
Available at: https://www.mdpi.com/2218-273X/11/2/248
5. Holland, E. J., Pandit, S. V., Sánchez-Abella, J., Haiek, A., Loinaz, M., Dupin, N., Gonzalez, S., Larra, M., Bidaguren, P., Lagali, N. S., Moloney, G. M. and Ritter, T., 2021. Artificial Cornea: Past, Current, and Future Directions. Cornea, 40(1), pp.1–15.
Available at: https://pubmed.ncbi.nlm.nih.gov/34869489/